* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download neuroplasticity 2016
Apical dendrite wikipedia , lookup
State-dependent memory wikipedia , lookup
Neural engineering wikipedia , lookup
Neural coding wikipedia , lookup
Central pattern generator wikipedia , lookup
Single-unit recording wikipedia , lookup
End-plate potential wikipedia , lookup
Caridoid escape reaction wikipedia , lookup
Endocannabinoid system wikipedia , lookup
Neuroeconomics wikipedia , lookup
Metastability in the brain wikipedia , lookup
Long-term potentiation wikipedia , lookup
Biological neuron model wikipedia , lookup
Aging brain wikipedia , lookup
Optogenetics wikipedia , lookup
Long-term depression wikipedia , lookup
Eyeblink conditioning wikipedia , lookup
Neuromuscular junction wikipedia , lookup
Clinical neurochemistry wikipedia , lookup
De novo protein synthesis theory of memory formation wikipedia , lookup
Channelrhodopsin wikipedia , lookup
Holonomic brain theory wikipedia , lookup
Axon guidance wikipedia , lookup
Premovement neuronal activity wikipedia , lookup
Environmental enrichment wikipedia , lookup
Development of the nervous system wikipedia , lookup
Neuroplasticity wikipedia , lookup
Molecular neuroscience wikipedia , lookup
Nonsynaptic plasticity wikipedia , lookup
Neuroregeneration wikipedia , lookup
Nervous system network models wikipedia , lookup
Neurotransmitter wikipedia , lookup
Activity-dependent plasticity wikipedia , lookup
Feature detection (nervous system) wikipedia , lookup
Neuropsychopharmacology wikipedia , lookup
Neuroanatomy wikipedia , lookup
Synaptic gating wikipedia , lookup
Synaptogenesis wikipedia , lookup
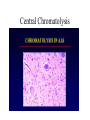
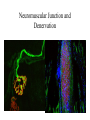
Neuroplasticity • Lundy-Ekman, Chapter 4 • Dr. Donald Allen Outcomes • Describe habituation and its role in therapy. • Explain what is happening during long-term potentiation. • Describe the anatomical and metabolic features of injury to the nervous system. • Describe the anatomical changes that can occur during the recovery from injury. • Describe the effects of forced use on recovery from an injury. Plasticity • What makes something plastic? – – Neuroplasticity • Any change in the nervous system that is not periodic – Duration of more than a few seconds – Combination of both flexibility and stability Types of Neuroplasticity • Habituation • Learning and Memory • Recovery from Injury Habituation • Considered by some to be the simplest form of learning • Decreased response to a repeated innocuous stimulus • Involves changes in neurotransmitter release (strength of synaptic connections) • Reversible – Stop repeating the stimulus – Change the stimulus – Sensitizing stimulus http://www.people.virginia.edu/~jyl8b/Percep/infant.html How could you use habituation? • Use of techniques and exercises to decrease the neural response to a stimulus Learning and Memory • More long-lasting, persistent • Also involves changes in strength of synaptic connections • 3 Main types of learning and memory Motor Memory • AKA: Procedural memory • Learning a task – Riding a bike Verbal Memory • Declarative memory • Items that can be spoken or written • Repetition? Emotional Memory • Not well understood • Memory for associations of emotions with specific places, people, etc. Neurological mechanisms of Learning and Memory • Neuroimaging techniques – Initial stages of motor learning • Large and diffuse areas of the brain involved – With repetition • Decrease in number of brain regions which are active – Task learned • Only small, distinct regions of the brain show activity during performance of a task Long-Term Memory • Long-term memory requires the synthesis of new proteins and growth of new synaptic connections – In animal studies, giving protein synthesis inhibitors blocks the formation of new memories Long-term Potentiation • Proposed mechanism to explain long-term memory • Occurs in hippocampus (part of temporal lobe) • Hippocampus is important for processing verbal memory – Bilateral damage to hippocampus results in an inability to form new verbal memories Studies on LTP • Repetitive stimulation will increase the responses to the stimulus • Started with animal studies – slices of hippocampus – Treatment • Single stimulus – measure response • Repeated stimuli • Single stimulus – measure response – now much larger response • http://users.rcn.com/jkimball.ma.ultranet/BiologyP ages/L/LTP.html Requirements for LTP • Cooperativity • Associativity • Specificity Cooperativity • There must be multiple excitatory inputs into the hippocampal neuron that will exhibit LTP • The multiple inputs have an additive effect • The individual inputs do not have to be strong. Even weak inputs can show potentiation is they occur in association with strong inputs Associativity • Both the presynaptic fibers and the postsynaptic cell must be activated together – An action potential in the presynaptic axon must produce an action potential in the postsynaptic neurons – I.e. The synapse must be effective Specificity • Only synapses that are associated with an action potential in the postsynaptic neuron will be potentiated. Effects of LTP • Involves – Increases in synaptic activity – Increased effectiveness of neuron firing Role of non-neuronal cells in LTP • Astrocytes – Change shape rapidly in response to stimulation – Increase in astrocyte-neuron contacts in rats raised in challenging environment compared to standard conditions Mechanism of LTP • Conversion of ‘silent synapses’ into active synapses • Postsynaptic membrane is remodeled to form new dendritic spines and synapses Recovery from Injury • What we see depends on what parts of the neuron are injured – Cell body – Axon Injury to cell body • If severe, will kill the cell – In general, dead neurons are not replaced – However, changes in the remaining neurons can promote recovery after the injury Injury to Axon • Will cause degenerative changes, but will not necessarily kill the neuron • If axon severed, the two ends will seal • We now have a proximal section of the axon, which is attached to the cell body, and a distal section, which continues to the presynaptic terminal Distal section of axon • This section is separated from the cell body and will degenerate – Wallerian degeneration • Glial cells will clean up the degenerating neurons. In the peripheral nervous system, what kind of glial cells will these be? • The postsynaptic cell will show some degenerative changes (it has lost inputs) – Trans-synaptic degeneration – Some may die. It depends on the importance of the lost inputs Proximal section of axon • Still attached to soma, so has the potential to survive depending on what happens to the neuron – Central chromatolysis – dissolution of Nissl substance in the cell body – Cell body may die Central Chromatolysis Recovery After an Injury • Recovery is affected by age at time of injury – Recovery decreases with age – Children can have an entire cerebral hemisphere removed and show little permanent deficits Regrowth of Axons after Injury • Sprouting (page 72, Fig 4-4) – Collateral sprouting • Denervated target is reinnervated by branches of intact axons – Regenerative sprouting • Target and axon both damaged • Target dies • Injured axon sends out collaterals to new targets Functional Regeneration • More prevalent in peripheral nervous system • Schwann cells make growth factors that contribute to recovery of peripheral axons – NGF- Nerve growth factor • Recovery is better with a crush injury compared to a cutting injury • Growth is slow: 1 mm/day = 1 inch/month CNS regeneration • Little or no functional regeneration – No Schwann cells producing NGF – Oligodendrocytes inhibit growth of neurons – Incomplete cleanup of cellular debris by microglia Potential problems during regeneration • Sprouting may innervate inappropriate targets – Motor neurons may innervate different muscles • May produce unintentional movements • Synkinesis • These movements are usually short-lived, and the individual relearns muscle control – Can also see confusion of sensory modalities Changes in synapses after injury • Local edema and recovery of synaptic effectiveness • Denervation hypersensitivity • Synaptic hypereffectiveness • Unmasking of silent synapses Effects of edema • Local edema can occur after an injury • The edema can put pressure on axons or cell bodies • Some synapses may become inactive • Return of synaptic effectiveness – As the edema resolves, the effectiveness of the synapses can return • What does this mean for therapists? – Immediately after an injury, there can be a loss of function – Permanent or Temporary? – As edema resolves, the patient may exhibit a return of function Denervation hypersensitivity • Occurs when there is damage to presynaptic terminals • The postsynaptic cells lose all or some of their synaptic inputs • Neurons like to maintain a moderate level of stimulation. Denervation removes this stimulation. • Postsynpatic neurons (and muscles) respond by producing more receptors – These new receptors will respond to neurotransmitters that are released by adjacent axons Neuromuscular Junction and Denervation Synaptic hypereffectiveness • Sometimes only some of the axon branches of a neuron are damaged • The presynaptic cell body still makes the usual amount of neurotransmitter, but now the neurotransmitter is distributed to less presynaptic terminals • Therefore, each terminal receives more neurotransmitter, and more neurotransmitter is released at each synapse Unmasking of silent synapses • Disinhibition of silent synapses • Many synapses in the central nervous system appear to be non-functional (silent) • An injury to pathways in the brain can unmask these synapses and they can become functional What chemicals are important for these changes in synapses? • • • • • • NMDA receptors Ca++ ions Neurotrophins (growth factors) Substance P Nitric oxide Changes in subtypes of sodium ion channels Functional Reorganization of the Cerebral Cortex • When we look at somatosensory and motor areas of the cortex, we find that specific parts of the body can be mapped onto the surface of the cerebral cortex. • Determined by: – Studies like Broca’s and Wernicke’s – Recording which areas of the cortex show electrical activity after sensory stimulation or active muscle contraction • Further studies using MRI have confirmed the electrical studies • Large areas of cortex represent the hands and face (high number of sensory receptors and need for controlled movements) • For somatosensation, there are actually several different maps that are parallel to each other • General map for humans, but there will be differences between individuals Changes in the Somatotopic map of the cerebral cortex • If we use a particular part of our body more, the area of cortex corresponding to the area will increase in size (Elbert et al., 1995) • If a region of the body is lost, the area of cortex corresponding to the region will decrease in size. – In people with upper extremity amputations, much of the region of the cortex that use to correspond to the U/E becomes reorganized. The area can then provide a presentation of the face. • This reorganization occurs through the unmasking of silent synapses • Similar brain reorganization is thought to occur in people who are blind or deaf – People who are congenitally deaf often have enhanced peripheral vision to moving objects – People who are blind use visual areas of cortex when reading Braille writing Complications of Reorganization • May see referred sensations after an amputation – Stimuli that are applied to one area of the body are felt to occur in a different part of the body – A touch to the chin may be felt as if it were applied to a missing fifth finger • Functional reorganization may also be a factor in some chronic pain syndromes, where pain persists after the injury heals. Factors that can influence neuroplasticity • Neuronal activity – Overstimulation of somatosensory pathways causes the increased release of inhibitory neurotransmitters – If there is understimulation of sensory pathways, the cortex can become more sensitive to weak stimuli • Reduced activity can promote axonal growth to increase stimulation Factors that can influence neuroplasticity – Growth Factors • Brain-derived neurotrophic factor (BDNF) – Supports survival of sensory neurons, basal forebrain cholinergic neurons, and mesencephalic dopaminergic neurons – May be of use in local treatment of neurodegenerative disorders (Parkinson’s Disease) – May be of use in protecting motor neurons in patients with motor neuropathies and ALS Growth Factors Continued • Nerve Growth Factor – NGF • May have a role in treating – Alzheimer’s Disease – protects cholinergic neurons in primates – Diabetic neuropathy – Chemotherapy-induced neuropathies • May promote neuroplasticity Overview of Neuroplasticity • Defines how the nervous system responds to: – Injuries – Changes in neuronal activity How does neuroplasticity affect the treatment of patients with CNS injuries • Forced-activity • Excito-toxicity Forced Activity • Patient has an injury to the central nervous system. The studies in humans have mostly involved patients with strokes • Patient is made to use the affected body part • Studies have been done with people and animals Kozlowski et al., 1996 • Lesion to sensorimotor cortex – Forced use of limb immediately after lesion • Lesion increased in size: Excitotoxicity • Long-term behavioral deficits – Poor limb placement – Decreased response to sensory stimulation – Defective use of limb for postural support Nudo et al., 1996 • Also in animals – Small lesion in cortex associated with hand movements • See loss of function from lesion site • Also loss of function in adjacent, undamaged cerebral cortex – Initiated movement 5 days after lesion • Prevented loss of function in area adjacent to lesion • In some animals, neural reorganization: hand representation extended into regions which previously represented shoulder and elbow Human Studies • Most done by one research group and its students • Stroke patients – Restrain unaffected upper extremity – Practice tasks with affected extremity • Chronic stroke: > 1 year of dysfunction • Results: See motor improvements Why could constraint therapy work? • Learned helplessness Excitotoxicity • Too Much Of A Good Thing – – – – – Ischemia or TBI Release and Spread of Glutamate NMDA receptors – Ca++ influx Too much Ca++ can kill neurons Extension of region of neuron death