* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Spinal Cord and the Peripheral Nervous System
Neural coding wikipedia , lookup
Node of Ranvier wikipedia , lookup
Nonsynaptic plasticity wikipedia , lookup
Axon guidance wikipedia , lookup
Patch clamp wikipedia , lookup
Neural engineering wikipedia , lookup
Neurotransmitter wikipedia , lookup
Resting potential wikipedia , lookup
Optogenetics wikipedia , lookup
Caridoid escape reaction wikipedia , lookup
Embodied language processing wikipedia , lookup
Biological neuron model wikipedia , lookup
Clinical neurochemistry wikipedia , lookup
Neuroregeneration wikipedia , lookup
Proprioception wikipedia , lookup
Evoked potential wikipedia , lookup
Development of the nervous system wikipedia , lookup
Chemical synapse wikipedia , lookup
Microneurography wikipedia , lookup
Feature detection (nervous system) wikipedia , lookup
Single-unit recording wikipedia , lookup
Synaptic gating wikipedia , lookup
Premovement neuronal activity wikipedia , lookup
Central pattern generator wikipedia , lookup
Electrophysiology wikipedia , lookup
End-plate potential wikipedia , lookup
Molecular neuroscience wikipedia , lookup
Synaptogenesis wikipedia , lookup
Circumventricular organs wikipedia , lookup
Nervous system network models wikipedia , lookup
Channelrhodopsin wikipedia , lookup
Neuroanatomy wikipedia , lookup
Neuromuscular junction wikipedia , lookup
Neuropsychopharmacology wikipedia , lookup
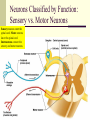
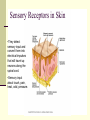
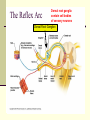
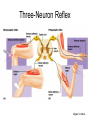
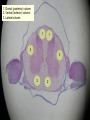
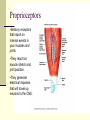
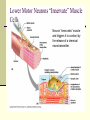
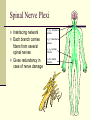
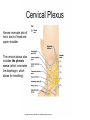
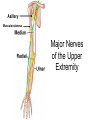
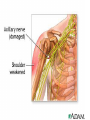
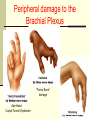
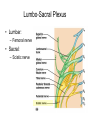
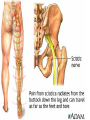
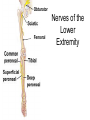
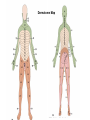
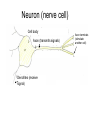
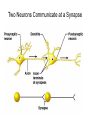
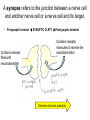
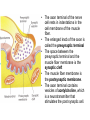
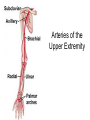
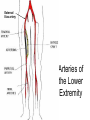
Peripheral Nerves and Arteries • CNS = Central Nervous System (Brain and spinal cord) • PNS = Peripheral Nervous System (nerves to appendages) • Neurons are grouped functionally according to the direction the nerve impulse travels relative to the CNS. • Sensoroy Neurons (afferent neurons) transmit impulses toward the CNS. They originate in the PNS and terminate in the CNS. • Motor Neurons (efferent neurons) transmit impulses from the CNS to effector organs (muscles and glands). They originate in the CNS and terminate in the PNS. • Interneurons (association neurons) connect sensory neurons to motor neurons within the spinal cord and brain. They originate and terminate in the CNS, and form complex neuronal pathways. They make up 99.98% of the neurons in the body, reflecting the vast amount of information processed in the CNS. Sensory Input and Motor Output Sensory (afferent) neurons are those that pick up sensory signals from receptors in the fingers, toes, etc Bundles of the same kind of sensory neurons travel together as NERVES, and go from the PNS to the CNS Motor (efferent) neurons originate in the brain, and the signals are carried away from the CNS and go to the muscles and glands. Information IN Sensory or “afferent” neurons carry information into the CNS from receptors located throughout the body. Information OUT Motor or “efferent neurons” carry electrical impulses away from the CNS to innervate “effector organs,” like muscles and glands. Neurons Classified by Function: Sensory vs. Motor Neurons Sensory neurons enter the spinal cord. Motor neurons leave the spinal cord. Interneurons connect the sensory and motor neurons. Figure 12.11 Sensory Receptors in Skin •They detect sensory input and convert them into electrical impulses that will travel up neurons along the spinal cord. •Sensory input about touch, pain, heat, cold, pressure. The Reflex Arc Dorsal root ganglia contain cell bodies of sensory neurons Dorsal Root Ganglion Simple Reflex Arc In the spinal cord, these three neurons together (sensory, lower motor, and interneuron) form the SIMPLE REFLEX ARC. They process information without the brain. So if you touch a hot stove, the sensory input comes into the spinal cord, the association neurons send the information to the lower motor neurons, the muscle contracts, and you take your hand off the stove before your brain even knows it. This is an example of a withdrawal reflex. Simple reflex behavior involves three neurons, and no brain involvement. Reflexes are automatic events. They involve both motor and sensory neurons, they are rapid, involuntary, and they involve multiple synapses. KNEE-JERK REFLEX is also an example of a threeneuron reflex. Spinal Cord Reflexes Stretch Reflex (knee-jerk; patellar reflex) Muscle contracts in response to a sudden stretch force (with a reflex hammer). After a severe spinal cord injury, all spinal reflexes are lost below the level of the injury for 2 weeks. Then the patellar reflex returns but it is often exaggerated (hyper-reflexic), indicating damage is still present. Withdrawal Reflex The body part is quickly removed from a painful stimulus. Sensory neurons carry the information to the spinal cord, and the muscles remove the limb immediately, before the brain receives the pain information. Three-Neuron Reflex Figure 12.18a, b Withdrawal Reflex When you touch a hot object, the sensory neuron sends the impulse to the spinal cord where it synapses on an interneuron. The interneuron synapses on a motor neuron The motor neuron tells your muscles to contract to remove your hand. While you are taking your hand off the hot object, a branch of the sensory neuron travels to the brain to report the sense of pain. However, your hand has already been withdrawn because of the reflex command from the spinal cord. Sensory Information goes to brain All sensory information goes to the brain for interpretation. To get there, the axons have to travel up the spinal cord. Sensory axons travel in the white matter of the spinal cord to get to the brain. White Matter White matter of the spinal cord forms conduction pathways called NERVE TRACTS. The white matter in each half of the spinal cord is organized into three columns: Dorsal (posterior) column Ventral (anterior) column Lateral column Each column has ascending tracts, which consist of axons conducting impulses toward the brain and descending tracts, which consist of axons conducting impulses away from the brain. Sensory Tracts are grouped into columns Some tracts in the spinal cord are for neurons transmitting sensory information about light touch, pain, and temperature. They travel to the thalamus in the dorsal column. Some tracts in the spinal cord are for neurons transmitting sensory information about vibration. They travel to the thalamus in the lateral column. Some tracts in the spinal cord are for neurons transmitting sensory information about balance. They travel to the cerebellum in the ventral column. 1. Dorsal (posterior) column 2. Ventral (anterior) column 3. Lateral column 1 1 3 3 2 2 Sensory Tracts Therefore, when sensory information enters the spinal cord, the signal goes to the brain via a TRACT. A tract is a collection of axons inside the central nervous system. Sensory axons from neurons transmitting the sense of touch, temperature, pain, or vibration send a branch to the thalamus portion of the brain. SENSORY TOUCH SPINAL NERVE POSTERIOR ROOT TRACT (in the dorsal column) THALAMUS Sensory Tracts Sensory axons from neurons called proprioceptors transmit the sense of balance and will travel to the cerebellum. PROPRIOCEPTORS SPINAL NERVE POSTERIOR ROOT TRACT (in the ventral column) CEREBELLUM Tracts to the Brain These tracts have various names, depending on what types of neurons are traveling within them. For example, within the dorsal tract is a specific region called the SPINOTHALAMIC TRACT which transmits pain and temperature. Within the ventral tract is a specific region called the SPINOCEREBELLAR tract which transmits signals of balance and position to the cerebellum. There are many other tracts as well. Some tracts send sensory information to the brain, and some tracts send motor commands from the brain to the muscles. PROPRIOCEPTION NEURONS These are sensors within the muscles that measure the amount of force and movement (they are sensory). Proprioception neurons travel up the spinocerebellar tract. The brain can then interpret whether you are off balance, then send a command to the muscles to contract and straighten yourself up so you don’t fall. Note that this sense of balance is NOT the same as the sense of balance from equilibrium in the ears. Proprioception neurons are located within the muscles. During a physical exam, a doctor will test the patient’s proprioception ability by telling them to close their eyes and place their finger on their nose. This may indicate a lesion in the cerebellum. Who else may ask you to do this test? Alcohol disrupts the cerebellum. Proprioceptors •Sensory receptors that report on internal events in your muscles and joints. •They report on muscle stretch and joint position. •They generate electrical impulses that will travel up neurons to the CNS. Proprioception Disorders Damage to proprioceptors can occur from consuming excess vitamin B6 (pyridoxine). Patients cannot tell where their body parts are unless they look at them. They have difficulty with all motor tasks including walking, eating, dressing, etc. They must use their vision to watch each body part to make it move in the right direction. Motor command come from the brain All motor commands (the command to move a skeletal muscle) originate in the brain. The cell body of these neurons (motor neurons) are in the brain. Their axons travel down the spinal cord. Motor neurons travel in the grey matter of the spinal cord. There are always two motor neurons involved in making skeletal muscles contract: an upper motor neuron (UMN) and a lower motor neuron (LMN). Upper and Lower Motor Neurons The motor neuron whose cell body is in the brain is called an upper motor neuron. It relays the signal to the motor neuron whose cell body is in the spinal cord, called the lower motor neuron. The lower motor neuron leaves the spinal cord and synapses on a muscle, causing contraction. Lower Motor Neurons “Innervate” Muscle Cells Neuron “innervates” muscle and triggers it to contract by the release of a chemical neurotransmitter. Upper and Lower Motor Neuron Diseases Some diseases only effect the UMN, and some only effect the LMN. Lower motor neuron disorders: Multiple Sclerosis Polio Upper motor neuron disorder: Cerebral palsy Upper and Lower motor neuron disease ALS Autonomic Neuropathy Autonomic neuropathy is damage to autonomic nerves. The autonomic nerves are those that supply involuntary body functions, including heart rate, blood pressure, perspiration and digestion. A common symptom in autonomic neuropathy is dizziness. Muscle twitches and lack of sensation are NOT symptoms, since they are not supplied by autonomic nerves. Peripheral Nervous System Peripheral nerves are those that are outside of the spinal cord. We will now discuss those nerves that supply the arms and legs. As these nerves first exit the spinal cord, they are called spinal nerves. They travel in groups; each group of spinal nerves is called a plexus. Spinal Nerve Plexi Interlacing network Each branch carries fibers from several spinal nerves Gives redundancy in case of nerve damage C1-C4- Cervical plexus C5-T1- Brachial plexus L1-L4- Lumbar Plexus L4-S4- Sacral Plexus Cervical Plexus Nerves innervate skin of neck, back of head and upper shoulder. The cervical plexus also includes the phrenic nerve (which innervates the diaphragm, which allows for breathing) Brachial Plexus Brachial Plexus Brachial Plexus Damage to Brachial Plexus Klumpke’s paralysis (brachial plexus damaged during birth) Acquired Brachial Plexus injuries Crutch paralysis (total upper extremity paralysis) Claw Hand / Ape hand (ulnar nerve damage) Hand of benediction (median nerve damage) Wrist Drop or “Waiter’s Hand” (radial nerve damage) Axillary Musculocutaneus Major Nerves of the Upper Extremity Axillary Nerve Deltoid Teres minor Musculocutaneus Nerve Supplies anterior muscles of the arm Biceps brachii Brachialis Coracobrachialis Median Nerve Supplies no muscles of the arm Supplies anterior forearm (except flexor carpi ulnaris) Damage can cause Carpal Tunnel Syndrome Hand of benediction Ape Hand Ulnar Nerve Supplies flexor carpi ulnaris “Funny Bone” Damage can cause claw hand Radial Nerve Supplies muscles on the posterior arm and forearm Triceps brachii Extensor carpi radialis Extensor digitorum communis Damage can cause wrist drop Peripheral damage to the Brachial Plexus “Funny Bone” damage Ape Hand Carpal Tunnel Syndrome Lumbo-Sacral Plexus • Lumbar: – Femoral nerve • Sacral: – Sciatic nerve Obturator Femoral Nerves of the Lower Extremity Obturator Nerve Supplies adductor muscles Femoral Nerve Anterior Thigh Quadriceps femoris Sciatic Nerve Supplies back of thigh Biceps femoris Semimembranosis Semitendonosis Then it branches into the common peroneal and tibial nerves to supply the leg and foot. The common peroneal branches into the superficial and deep peroneal. Tibial Nerve Posterior leg and foot Gastrocnemius Soleus Tibialis Posterior Common Peroneal Nerve Superficial branch Lateral side of leg Supplies peroneal muscles (lateral leg) Peroneus longus, brevis, and tertius Deep branch Supplies anterior leg muscles Injury causes “Foot Drop” Dermatomes You don’t need to memorize the dermatome map; just know that a dermatome is the area of skin innervated by a cutaneous branch of a spinal nerve at a particular level. Dermatome Map Action Potentials Cell membranes have gates embedded in them that allow only certain ions to go through. These are called ion channels. K+ channels are open most of the time, but Na+ channels are closed unless a nerve stimulates them. Na+ K+ K+ Na+ Na+ K+ K+ K+ K+ Therefore, K+ can go back and forth from the cell, but Na+ is blocked from entering the cell. The outside of most cell membranes is positively charged compared to the inside of the cell membrane. How does this happen? Na+ There are many potassium ions (K+) on the inside of the cell because the cell membrane is more permeable to K+ then to other ions. Na+ Na+ Cell membranes contain K+ channels which are often open to allow K+ to flow into the cell and accumulate. Na+ Na+ Na+ Na+ Na+ K+ K+ K+ K+ K+ Proteins - K+ However, that creates an area of high concentration of potassium on the inside of the cell, and all molecules tend to diffuse from an area of high concentration to an area of low concentration. Na+ Na+ That means that potassium will then flow out of cell until it is equally concentrated on both Na+ sides of the membrane. Na+ Na+ Na+ Na+ K+ K+ K+ K+ K+ Proteins - - Na+ K+ K+ K+ K+ K+ 56 There are also a lot of sodium ions (Na+) on the outside of the cell. The cell membrane contains Na+ channels, but they are often closed, so this so they tend to stay on the outside of the cell. ClSince there are now so many Na+ + Na + and K ions on the outside of the cell, and only a few negatively charged ions, such as Chloride Na+ (Cl-), the overall charge of the outside of the cell membrane is positive. Na+ Na+ Na+ Cl Na+ Na+ K+ K+ K+ K+ K+ Proteins - - The inside of the cell is negative because there are a lot of proteins inside of a cell, and proteins are + Na usually negatively charged. The negative charge is greater than ClK+ the positive charges of the Cl remaining K+ K+ K+ K+ K+ 57 MEMBRANE POTENTIALS • The charge difference on the outside and inside of the cell membrane is called the resting membrane potential. • Resting membrane potential is calculated at the point at which potassium has reached equilibrium. • The resting membrane potential is usually positive, since sodium ions are also present when potassium is at its equilibrium. • The resting membrane potential will be changed if the membrane permeability to one or more ions is selectively altered. When a muscle cell or nerve cell is stimulated, Na+ channels in the cell membrane quickly open, and the sodium rushes into the cell. ClCl- That causes the inside of the cell membrane to become positively charged. The ions left on the outside are Cl- which have a negative charge, so the outside of the cell membrane now has an Cloverall negative charge. Cl- ClCl- Cl- Na+ K+ K+ + K K+ K+ Na+ + + Na + Na + Na Na Proteins - + Na - + Na K+ Cl- K+ K+ K+ K+ 59 MEMBRANE POTENTIALS • When the outside of a cell membrane goes from a positive charge to a negative charge, this change is called depolarization. It only lasts for a short time because the Na+ channels quickly close, the sodium leaves the cell, and the outside of the membrane becomes positively charged again. • The change back to resting potential is called repolarization. • The rapid depolarization and repolarization of the cell membrane is called an action potential. ACTION POTENTIAL • The action potential begins when the charge reaches a certain threshold. • An action potential is like an electrical current being conducted from cell to cell. • That makes the outside of the cell next to it to also go from positive to negative and back again. • The action potential then continues from cell to cell. When it reaches its target organ, such as a muscle, the muscle will contract. • In a muscle fiber, an action potential results in muscle contraction. Neuron (nerve cell) Cell body Axon (transmits signals) Dendrites (receive signal) Axon terminals (stimulate another cell) Two Neurons Communicate at a Synapse A synapse refers to the junction between a nerve cell and another nerve cell or a nerve cell and its target. • Presynaptic terminal SYNAPTIC CLEFT Postsynaptic terminal Contains vesicles filled with neurotransmitter Contains receptor molecules to receive the neurotransmitter Direction of action potential Motor neurons • Skeletal muscle fibers do not contract unless they are stimulated by motor neurons. • Motor neurons are nerve cells along which action potentials travel to skeletal muscle fibers. Axons of these neurons enter muscles and send out branches to several muscle fibers. • Each branch forms a junction with the muscle fiber called a neuromuscular If one neuron sends a signal, only its muscle fibers (the motor unit) contract. This allows for strength variations in lifting a chair vs. an eraser. For full strength, all the motor units contract. For half strength, half of the motor units contract. Motor unit at a neuromuscular junction • The axon terminal of the nerve cell rests in indentations in the cell membrane of the muscle fiber. • The enlarged knob of the axon is called the presynaptic terminal • The space between the presynaptic terminal and the muscle fiber membrane is the synaptic cleft • The muscle fiber membrane is the postsynaptic membrane. • The axon terminal contains vesicles of acetylcholine, which is a neurotransmitter that stimulates the post synaptic cell. • An action potential causes the release of Ach (acetylcholine; the neurotransmitter at the neuromuscular junction) into the synaptic cleft. • Ach binds to receptor sites on the muscle fiber (muscle cell) membrane. This opens up the Na+ channels so that sodium rushes into the cell. • When Na+ brings its positive charge to the inside of the cell, it causes the outside of the cell to become negative (depolarization). Then the Na+ channels close, the Na+ exit the cell, taking their positive charges with them, and the membrane repolarizes. This event is called an action potential, which travels along the length of the muscle fiber and causes it to contract. • The Ach that was released is rapidly broken down by an enzyme, Ach-ase (acetylcholinesterase). This ensures that the action potential will result in only one contraction of each muscle fiber. Acetylcholine Antagonists • Some INSECTICIDES inhibit acetylcholinesterase, so Ach accumulates in the synaptic cleft and acts as a constant stimulus to the muscle fiber. The insects die because their respiratory muscles contract and cannot relax. • Other poisons, such as CURARE, the poison used by South American Indians in poison arrows, bind to the Ach receptors on the muscle cell membrane and prevent Ach from working. That prevents muscle contraction, resulting in flaccid paralysis. Myasthenia gravis • Myasthenia gravis is an autoimmune disorder in which antibodies attack and destroy some acetylcholine receptors. • Acetylcholine is therefore less likely to stimulate muscle contraction, resulting in muscle weakness and fatigue. • Symptoms usually begin in the eyelid and facial muscles, and manifests as drooping muscles on half or both sides of the face, drooping eyelids, and slurred speech. • Neostigmine is an anti-cholinesterase drug which reduces the symptoms by inhibiting Ach-ase activity, preventing the breakdown of Ach. Consequently, Ach levels in the synapse remain elevated, so Ach is available to bind to those few functional Ach receptors that are left. Arteries of the Upper Extremity Arteries of the Upper Extremity Subclavian artery is so named because it goes under the clavicle. The subclavian artery changes names when it enters the axilla. It is now called the axillary artery. The axillary artery supplies triceps brachii The arm area is referred to as the brachium. The axillary artery changes names when it leaves the axilla and enters the arm. It is now called the brachial artery (in the arm) The brachial artery supplies all the arm muscles (biceps brachii, coracobrachialis, brachialis). At the elbow, the brachial artery divides into the radial and ulnar arteries to supply the forearm. External Iliac artery Arteries of the Lower Extremity Arteries of the Lower Extremity The abdominal aorta branches into the external iliac arteries. When the external iliac artery leaves the abdomen at the groin, it enters the thigh and is now called the femoral artery. Femoral artery supplies muscles of thigh (including adductor muscles) The femoral artery changes names and becomes the popliteal artery when it reaches the knee. The popliteal artery changes names to tibial artery in leg. The tibial artery supplies the leg muscles. Peripheral Vascular Disease (PVD) Refers to the obstruction of large arteries, frequently in the lower extremity. Usually caused from atherosclerosis (fatty plaques). Symptoms Claudication: pain, weakness, numbness, or cramping in muscles due to decreased blood flow Sores, wounds, or ulcers that heal slowly or not at all Change in color (blueness or paleness) or temperature (coolness) when compared to the other limb Diminished hair and nail growth on affected limb and digits (shiny, hairless skin)