* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Copy of PNS philadelphia
Single-unit recording wikipedia , lookup
Metastability in the brain wikipedia , lookup
Axon guidance wikipedia , lookup
Brain–computer interface wikipedia , lookup
Perception of infrasound wikipedia , lookup
Biological neuron model wikipedia , lookup
Endocannabinoid system wikipedia , lookup
Haemodynamic response wikipedia , lookup
Proprioception wikipedia , lookup
Central pattern generator wikipedia , lookup
Optogenetics wikipedia , lookup
Neuroregeneration wikipedia , lookup
Feature detection (nervous system) wikipedia , lookup
Development of the nervous system wikipedia , lookup
Caridoid escape reaction wikipedia , lookup
Basal ganglia wikipedia , lookup
Premovement neuronal activity wikipedia , lookup
End-plate potential wikipedia , lookup
Anatomy of the cerebellum wikipedia , lookup
Clinical neurochemistry wikipedia , lookup
Nervous system network models wikipedia , lookup
Neurotransmitter wikipedia , lookup
Synaptic gating wikipedia , lookup
Molecular neuroscience wikipedia , lookup
Chemical synapse wikipedia , lookup
Neuromuscular junction wikipedia , lookup
Neuropsychopharmacology wikipedia , lookup
Stimulus (physiology) wikipedia , lookup
Neuroanatomy wikipedia , lookup
Synaptogenesis wikipedia , lookup
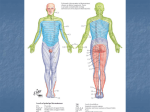
Peripheral Nervous System 2 3 Sensory Afferent Dorsal root Peripheral nervous system (PNS) Motor Efferent Dorsal root ganglia where cell body of sensory neuron is located Somatic Motor Ventral root Autonomic Motor interneuron Skeletal muscle smooth muscles, cardiac muscles, and glands 4 Efferent division of PNS is divided: somatic NS & autonomic NS. 1-Somatic neurons innervate skeletal muscles, 2-Autonomic neurons innervate smooth & cardiac muscle, glands, and GIT (Enteric NS ). 5 6 Somatic Division 1. Innervates skeletal muscles: Conscious of its activity. 2. Only one motor neuron to effector (no gangalia) 3. NT: only Ach 4. Only stimulatory/excitatory signals 5. Fast-conducting, thick (9-13 um), myelinated axons (A fibers). 6. Severing neurons causes muscle paralysis 7 Autonomic Division 1-Innervates glands, smooth, & cardiac muscles. Usually unaware of its actions. 2-Two motor neurons control effector (ganglion). 3-NT: Ach, norepinephrine & epinephrine. 4-Stimulatory & inhibitory signals. 5-Slow-conducting: preganglionic thin (3 um) (B fibers); , lightly myelinated axons; postganglionic very thin (1 um), unmyelinated axons (C fibers). 6- Denervation causes muscle hypersensitivity of effector. A phenomena called (Denervation hypersensitivity) Neurons & Nervous Systems 8 Neurons & Nervous Systems 9 Neurons & Nervous Systems 10 11 The autonomic nervous system( ANS( )or Visceral nervous system) ANS is the part of the peripheral nervous system that acts as a control system, maintaining homeostasis in the body. These activities are generally performed without conscious control or sensation. The ANS affects heart rate, digestion, respiration rate, salivation, perspiration, diameter of the pupils, urination, and sexual arousal . ANS main components are parasympathetic nervous system and sympathetic nervous system Autonomic system 12 The sympathetic and parasympathetic systems are similar in the following aspects: a. Both function automatically and usually in an involuntary manner. b. Both innervate all internal organs. Visceral organs (organs within body cavity). c. Breathing rate and blood pressure are regulated by reflex actions to maintain homeostasis. d. Both utilize two neurons and one ganglion for each impulse. 1) The first neuron has a cell body within the CNS: it is called preganglionic neuron and it sends a preganglionic fiber. 2) The second neuron has a cell body within the ganglion it is called postganglionic neuron and it sends a postganglionic fiber. 13 14 preganglionic Autonomic neuron effector neuron Preganglionic Postganglionic Autonomic Axon will neuron has a Axon will neuron in cell body synapse synapse with Autonomic within cell within Ganglion is Autonomic target tissue called Nuclei in postganglio the gray nic neuron matter of brain or spinal cord. Autonomic Nerve Pathway Two-neuron chain Sympathetic Division 1. Sympathetic preganglionic fibers are cholinergic; postganglionic fibers are adrenergic (NT: norepinephrine ) 2. Sympathetic division activates body to fight or flight through adrenergic effects. 3. Too much stimulation cause aging 4. To defend or flee, muscles need a supply of glucose and oxygen; the sympathetic system accelerates heartbeat, and dilates bronchi. 5. To divert energy from less necessary digestive functions, the sympathetic system inhibits digestion. 16 6. Preganglionic neurons of sympathetic division originate in thoracic & lumbar regions (T1-L2) (thoracolumbar division). 7. Preganglionic fibers are short. 17 8. Most terminate in sympathetic ganglia that lies parallel the spinal cord, that is, 18 preganglionic fibers synapse with ganglia located in two sympathetic chains close to the spinal cord (double rows called paravertebral ganglia). Some ascend/descend within sympathetic trunk to synapse with another paravertebral ganglion. Others pass through the ganglion and emerge from the sympathetic chain without synapsing. 9.Synapses in Paravertebral (sympathetic chain) Ganglion: 19 Postganglionic axons enter the ventral ramus of the joining spinal nerves via communicating branches called gray rami communicantes . The ganglia are distinguished as cervical, thoracic, lumbar, and sacral The ganglia are distinguished as cervical, thoracic, 20 lumbar, and sacral Preganglionic fiber serving head, neck, and thorax emerge from21 spinal cord segments T1-T6 and ascend the sympathetic chain to synapse with postganglionic neurons within cervical ganglia (inferior, middle, and superior) - Superior cervical ganglion: Stimulates dilator muscles of irises Inhibits nasal and salivary glands Stimulates copious sweating Stimulates arrector pili muscle to contract Causes blood vessel vasodilation Provides branches to carotid body (oxygen sensor) and larynx & pharynx. 22 23 Middle cervical ganglia - innervates heart and skin Inferior cervical ganglia innervates heart, aorta, dilates bronchioles, constrict esophageal sphincter 24 25 10-Synapses in Prevertebral (Collateral) Ganglion: Preganglionic fibers of T5-L2 synapse in prevertebral ganglia. Fibers enter and leave without synapsing and form several nerves collectively called splanchnic nerves (greater, lesser, and lumbar). 26 Greater splanchnic nerve Celiac ganglion - innervates 1-stomach (decrease muscle activity/constricts pyloric sphincter), 2-adrenal medulla (secretes epinephrine/norepinephrine), 3-liver (epinephrine stimulates liver to release glucose), 4-kidney (vasoconstriction, decrease urine output), 5-intestine (decrease smooth muscle activity). 27 Lesser splanchnic nerve Superior mesenteric (via celiac) ganglion innervates small intestine 28 •Lumbar splanchnic nerve Inferior mesenteric ganglion innervates large intestine 29 - Lumbar splanchnic nerve Hypogastric ganglion innervates bladder and urethra (causes relaxation of smooth muscle of bladder wall and constricts urethral sphincter/inhibits voiding), genitalia (causes ejaculation in males and vaginal contractions in females) 30 Adrenal gland: Located above each kiddney Upon stimulation by Sympathetic system: 31 A- Cortex: releases steriod hormones B- medulla: releases adrenaline (epinephrine) 85% and norepinephrine 15% they differ slightly from each other and termed catacholamines Sympathetic system and Adrenal gland together are called Sympathoadrenal system Stimulation of the adrenal medulla releases adrenaline (epinephrine) into the bloodstream which will act on adrenoceptors, producing a widespread increase in sympathetic activity. Parasympathetic Division 32 1. Pre- & postganglionic parasympathetic fibers are cholinergic (secrete Ach) 2. The neurotransmitter released is acetylcholine. 3. Parasympathetic exerts antagonistic actions via cholinergic effects (house keeping). 4. It promotes internal responses resulting in a relaxed state. 5. The parasympathetic system causes the eye pupil to constrict, promotes digestion, and retards heartbeat. 1. (Craniosacral division): Preganglionic neurons originate in brain stem (CN III, VII, IX, X) III oculomotor 3 VII facial, 7 IX, glossopharyngeal; 9 X, vagus;10 and 2-4 sacral region of spinal cord. 33 7. Preganglionic fibers are long. They synapse in ganglia that contains the postganglionic neurons which are found in terminal ganglia: are located close to the target organ intramural ganglia: located within the wall of the target organ 7. Postganglionic fibers are short. E.g fibers that innervate the digestive tube, are located inside its walls. 8. Cutaneous effectors such as arrector pili, sweat glands, and blood vessels do not get Parasympathetic innervations. 34 10. The vagus (X) nerve synapses in terminal ganglia located in so many regions of the body (heart, lungs, esophagus, stomach, liver, small intestine, and upper half of the large intestine). 11. Parasympathetic outflow from the sacral levels of the spinal cord innervates the lower half of the large intestine, rectum, urinary, and reproductive systems. 12. The parasympathetic fibers within III oculomotor 3 ,VII facial, 7 and IX, glossopharyngeal; synapses in ganglia located in the head. 35 pterygopalatine ganglia Parasympathetic (Craniosacral Division) 36 Cranial Outflow Oculomotor nerve (III) - Preganglionic fibers from oculomotor nuclei in the midbrain synapses in the ciliary ganglion (in eye), postganglionic fiber innervates smooth muscle of eye Pupil constriction and lens movement to cause focusing Facial nerve (VII) - Preganglionic fibers from lacrimal nuclei in the pons synapses in the pterygopalatine ganglia, postganglionic fiber innervates lacrimal glands of eye Lubrication of eye and tear formation - Preganglonic fibers from superior salivatory nuclei in the pons synapses in the submandibular ganglia, postganglionic fibers innervate submandibular and sublingual salivary glands Production of saliva and secretion of salivary enzymes 37 Glossopharyngeal nerve (IX) - Preganglionic fibers from the inferior salivary nuclei in the medulla synapses in the otic ganglia, postganglionic fibers innervate the parotid salivary gland. Vagus nerve (X) - Preganglionic fibers from the dorsal motor nuclei of the medulla synapses in terminal ganglia located within the walls of the target organ Intramural ganglia ....effects: 1. Heart -decreases heart rate and constricts coronary veins 2. Lung - constricts bronchioles 3. Gall bladder - expel bile 4. Stomach - stimulates secretion of enzymes 5. Intestines - increase motility (peristalsis) and relaxes sphincters 38 39 Sacral Outflow Preganglionic fibers from lateral gray matter of spinal cord in segments S2-S4 synapse in ganglia within walls of the target organ - Intramural ganglia....effects: 1. Distal large intestines - relaxes sphincters 2. Bladder - contraction of smooth muscle of bladder wall; relaxes urethral sphincter promotes voiding 3. Genitalia - causes penile and clitoral erection 40 41 Response to Adrenergic Stimulation 42 Adrenergic effects (epinephrine from adrenal gland) and norepinephrine ) of sympathetic nerves include both excitatory and inhibitory effects. Stimulation of the heart, vasoconstriction in the viscera and skin, and glycogenolysis in the liver. (is the break down of glycogen to glucose-1-phosphate and glucose) . The smooth muscles of bronchoils and some blood vessels are inhibited from contraction resulting in bronchodilation, vasodilation. Adrenergic receptor classes are α and β. Some organs have only α or β receptors; other organs (heart) have both types of receptors. There are two subtypes of alpha receptors )α 1 and α 2) and two subtypes of beta receptors )β 1 and β 2). These subtypes can be selectively stimulated or blocked by therapeutic drugs. Examples: Heart (ß1), muscle of iris (α1), smooth muscle of blood vessels (α1) are stimulated to contract, smooth muscle of bronchioles (ß2) dilates. 43 Adrenergic Receptors o α1 Excitatory; e.g., arteriolar constriction o α2 Inhibitory; e.g., GI smooth muscle o β1 Excitatory; e.g., increased rate and force of cardiac contraction o β2 Inhibitory; e.g., arteriolar & bronchiolar (dilation) Response to cholinergic stimulation Acetylcholine is the preganglionic neurotransmitter for both divisions of the ANS, as well as the postganglionic neurotransmitter of parasympathetic neurons . Nerves that release acetylcholine are said to be cholinergic . In the parasympathetic system, ganglionic neurons use acetylcholine as a neurotransmitter, to stimulate muscarinic receptors. Ach binding to muscarinic receptors located in cardiac muscle hyperpolarization Inhibitory signals slow heart rate Ach binding to muscarinic receptors located in smooth muscle and glands depolarization excitatory signals contraction 45 46 Autonomic agonists and antagonists Agonist Binds with a neurotransmitter’s receptor and elicits an effect that mimics that of the neurotransmitter. Antagonist Binds with a neurotransmitter’s receptor and blocks the neurotransmitter’s response. Autonomic agonists and antagonists Atropine oBlocks the effect of acetylcholine at muscarinic receptors but does not affect nicotinic receptors oSuppresses salivary and bronchial secretions before surgery, to reduce the risk of a patient inhaling these secretions into the lungs Autonomic agonists and antagonists Salbutamol oSelectively activates β 2 adrenergic receptors at low doses oDilate the bronchioles in the treatment of asthma without undesirably stimulating the heart Other autonomic neurotransmitters • Certain postganglionic fibers do not produce their effect through Acetylcholine or norepinephrine, hence they are termed nonadrenergic, noncholinergic fibers . • Proposed NT of these fibers include, vasoactive intestinal peptide (VIP), and Nitric oxide (NO). • NO causes vasodilation of cerebral arteries. It promotes relaxation of smooth muscles. 50 • ORGANS WITH DUAL INNERVATION. • Most organs receive DUAL INNERVATION • ORGANS WITHOUT DUAL INNERVATION • some organs receive only sympathetic innervations. • Adrenal medulla, arrector pili muscle, sweat glands, and most blood vessels. • Regulation in these cases is achieved by increasing or decreasing the tone (firing rate) of sympathetic fibers. 52 Control of autonomic system by higher brain centers Visceral functions are largely regulated by autonomic reflexes. Sensory input is transmitted to brain centers that integrate this information and respond by modifying the activity of preganglionic autonomic neuron 53 54 The medulla oblongata is the area that directly controls the activity of the autonomic system. Medulla is regulated by higher brain areas, these include the hypothalamus cerebellum, and cerebrum. located in medulla are centers for the control of the cardiovascular, pulmonary, reproductive ,urinary and digestive systems. Mush of the sensory input of these centers travels in the afferent fibers of the vagus nerve. Since medulla oblongata controls the activity of the autonomic motor fibers a reflex takes place. The hypothalamus is influenced by input from the limbic system (group of forebrain nuclei and fiber tracts that form a ring around brain stem) The limbic system is involved in basic emotional drive. These interconnections provide an autonomic component to some of the visceral responses that accompany emotions. limbic system hypothalamus medulla 55 56 Medulla is also regulated by higher brain areas, which are the cerebellum, and cerebrum Nerve impulses from cerebellum to Medulla affect motion sickness, Nausea, sweating, and CV changes. Frontal and temporal lobes of cerebral cortex are involved in personality. 57 غير مطلوب ولكن للعلم فقطBrain-computer interface Amyotrophic lateral sclerosis (ALS, also called Lou Gehrig’s Disease) is a neurological disease characterized by the degeneration of the motor neurons that control voluntary movements. The disease begins with muscle weakening and lack of coordination and eventually destroys the neurons that control speech, breathing, and swallowing; in the end, the disease can lead to paralysis. At that point, patients require assistance from machines to be able to breathe and to communicate. Several special technologies have been developed to allow “locked-in” patients to communicate with the rest of the world. One technology, for example, allows patients to type out sentences by twitching their cheek. These sentences can then be read aloud by a computer. A relatively new line of research for helping paralyzed patients, including those with ALS, to communicate and retain a degree of self-sufficiency is called brain-computer interface (BCI) technology and is illustrated in Figure 15. This technology sounds like something out of science fiction: it allows paralyzed patients to control a computer using only their thoughts. There are several forms of BCI. 58 Figure 15: With brain-computer interface technology, neural signals from a paralyzed patient are collected, decoded, and then fed to a tool, such as a computer, a wheelchair, or a robotic arm. 59 Some forms use EEG recordings from electrodes taped onto the skull. These recordings contain information from large populations of neurons that can be decoded by a computer. Other forms of BCI require the implantation of an array of electrodes smaller than a postage stamp in the arm and hand area of the motor cortex. This form of BCI, while more invasive, is very powerful as each electrode can record actual action potentials from one or more neurons. These signals are then sent to a computer, which has been trained to decode the signal and feed it to a tool—such as a cursor on a computer screen. This means that a patient with ALS can use e-mail, read the Internet, and communicate with others by thinking of moving his or her hand or arm (even though the paralyzed patient cannot make that bodily movement). Recent advances have allowed a paralyzed locked-in patient who suffered a stroke 15 years ago to control a robotic arm and even to feed herself coffee using BCI technology. Despite the amazing advancements in BCI technology, it also has limitations. The technology can require many hours of training and long periods of intense concentration for the patient; it can also require brain surgery to implant the devices. 60