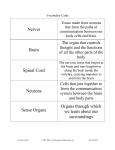
* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Membrane potential moves toward the K equilibrium
Optogenetics wikipedia , lookup
Microneurography wikipedia , lookup
Feature detection (nervous system) wikipedia , lookup
Axon guidance wikipedia , lookup
Nonsynaptic plasticity wikipedia , lookup
Neural engineering wikipedia , lookup
Development of the nervous system wikipedia , lookup
Signal transduction wikipedia , lookup
Synaptic gating wikipedia , lookup
Patch clamp wikipedia , lookup
Neurotransmitter wikipedia , lookup
Spike-and-wave wikipedia , lookup
Circumventricular organs wikipedia , lookup
Clinical neurochemistry wikipedia , lookup
Neuromuscular junction wikipedia , lookup
Biological neuron model wikipedia , lookup
Single-unit recording wikipedia , lookup
Neuroregeneration wikipedia , lookup
Action potential wikipedia , lookup
Nervous system network models wikipedia , lookup
Channelrhodopsin wikipedia , lookup
Chemical synapse wikipedia , lookup
Node of Ranvier wikipedia , lookup
Neuroanatomy wikipedia , lookup
Membrane potential wikipedia , lookup
Synaptogenesis wikipedia , lookup
Electrophysiology wikipedia , lookup
Resting potential wikipedia , lookup
End-plate potential wikipedia , lookup
Neuropsychopharmacology wikipedia , lookup
NEUROSCIENCE 1 – 07/01/2005 (page 1 of 2) The Nervous System Disorders Look for asymmetry – good indicator that something is wrong Common neurological disorders arise from non-neurological events (eg CVA) The cause of “intrinsic” disorders is not known. Disorders arise from either: (a) neuronal degeneration (b) neuronal dysfunction Disorders can show either: and/or (a) loss of function (b) abnormal function Psychiatric disorders involve altered behaviour when no pathological cause can be found. Neurology and Psychiatry may overlap considerably. Major Causes (a) Trauma >>eg skull fracture, spinal injury (b) Cerebrovascular Accident (CVA) >>eg stroke - blocked/bleeding artery (c) Infection eg meningitis ** (d) Neoplasia (tumour) eg glioma: gen. of new tissue–little cranial space (e) Metabolic disorders eg diabetic neuropathy ^^ (f) Genetic disorders eg Down’s syndrome. (g) Environmental factors eg heavy metal encephalopathy toxins (pb). (h) Immunological factors eg multiple sclerosis. >>(a) and (b) most common ** infection via meninges (membranes covering brain) viral – non fatal, bacterial – fatal huge influx of WBC and inflammation. ^^ degeneration of the peripheral nerves. Epilepsy: Abnormal Synchronous firing of neurones (EEG). Parkinsons Disease: Loss of dopaminergic (specific group of) receptors in midbrain. Bell’s Palsy: Denervation of facial muscles (Left supplies Left, Right supplies Right). Re-enervation is possible if infection treated. Divisions Division Consisting of Function Central Nervous System (CNS) Brain & Spinal Cord “Housekeeping” functions processing sensory and motor information and maintaining internal environment. Also supports higher functions of percpetion, cognition, emotion and personality CRANIAL NERVES CONNECTED DIRECTLY TO BRAIN i.e. not via spinal cord Peripheral Nervous System (PNS) Peripheral Nerves & Ganglia Provides sensory and motor innervation to the body Autonomic Nervous System (ANS) Parts of CNS & PNS Controls visceral (organ) function and homeostasis Each division has local control of function, but some larger systems have several communicating structures that are apart from one another eg the motor system The cerebral hemispheres of the brain have contralateral control of the body (ie left hemisphere controls right side of body. Thus there is lateralisation and localisation of the NS. Some higher functions only exist in one hemisphere - unilateral (eg language in left hemisphere only). PNS – cutting of an axon leads to sprouting from the cut end in order to re-establish a connection – i.e. it can regenerate, although this is not always successful as the connections can get mixed up with those of other neurons. CNS – No axon regeneration is possible. This is most probably due to the environment that the cell is in. Neurons Neurons are the functional cell units of the nervous system. The generate and conduct electrical impulses releasing chemicals at synpases. They are supported by neuroglia which outnumber neurons by 9:1 Synpase Cell Body Axon Impulse Direction Axons of neurones of the PNS can regenerate after injury although recovery may be compromised by non-specific target innervation Axons of the CNS do not regenerate Diagnostic Techniques (a) History Taking (i) Presenting complaint (ii) Other illnesses (iii) Social situation (iv) Patient observation. (b) Neurological Exam (i) Level of consciousness (ii) Speech (iii) Mental State & Cognitive Function (iv) Cranial nerve function # (v) Motor function (vi) Sensory function # critical gives idea of brain function (c) Neurophysiology /Electrophysiology (i) Electroencephalography (EEG) (ii) Electromyography (EMG) & Nerve Conduction Study (d) Imaging (i) Computerised Tomography (CT) – hard tissues (ii) Magnetic Resonance Imaging (MRI) – soft tissues ^^ (iii) Angiography of cerebral vasculature ^^ Consider: Size of pt. does it fit? + Metal implants? e.g. pacemaker. Psychiatric Disorders – Alter behaviour or mood – No demonstrable pathology – Neurology and Psychology may overlap considerably NEUROSCIENCE 2 (page 1 of 2) Cells of the Nervous System Neuronal Structure All neurons are essentially the same in structure. The diversity of types of neuron arises from the difference in the number and shape of their processes (a) Cell body (Soma) (i) Metabolic centre of the cell (ii) Large nucleus (iii) Abundant rough endoplasmic reticulum (iv) Well developed Golgi apparatus(Hi levels of trafficking) (v) Numerous mitochondria (vi) Numerous lysosomes (vii) Highly organised metabolically active cell (b) Dendrites (i) Receives incoming information (ii) Branch away from cell body (iii) Greatly increase surface area of neuron (iv) Dendritic spines receive majority of synapses (c) Axon (i) Conducts impulse away from cell body (ii) Emerges as the Axon Hillock (iii) Myelinated or unmyelinated (iv) Nodes of Ranvier (d) Terminals (i) Close to target the axon forms terminal branches (ii) Specialised structures called synpatic terminals (iii) Boutons (end of terminal) or varicosities along terminal SEE Mosby Crash Course p11 INTRACELLULAR TRANSPORT – functional polarization 1. Anterograde transport. - transport of materials needed for neurotransmission and survival away from cell body. a) fast anterograde - synaptic vesicles, transmitters, mitochondria 400mm/day uses microtubular network and requires oxidative metabolism. uses specific molecular motors. b) slow anterograde - bulk cytoplasmic flow of soluble constituents - 2. Retrograde transport. a) - fast retrograde – return of organelles. transport of substances from extracellular space. trophic growth factors, neurotropic viruses. uses different molecular motors. Neuronal Sub-Types Morphological Sub-Types (a) Pseudounipolar neuron Two fused processes which are both axonal DRG neurones give rise to no dendrites and receive no synapses. (b) Bipolar neuron Two axonal processes arising from the cell body (c) Golgi Type I Multipolar neuron Cells that extend long distances Pyramidal cells of Cerebral Cortex (purkinje) (d) Golgi Type II Multipolar neuron Cells that have relatively short axons Functional Sub-Types (a) Sensory neuron Conducts impulses from sensory receptors to the spinal cord and brain. Usually pseudounipolar with one process dividing into twowith one travelling to the CNS and one to a sensory receptor. (b) Motor neuron (c) Interneuron Conduct impulses from the brain and spinal cord to effectors such as muscles or glands. Usually multipolar with large cell body. Responsible for the modification, coordination, integration, facilitation and inhibition between sensory input and motor output. The cell bodies and processes remain within the CNS. Can be large multipolar or small local bipolar. Neuronal Organisation Neurons of the CNS are grouped according to their function (a) Nucleus Unencapsulated cell bodies within CNS (func.similar) eg Brain Stem (b) Laminae Layers of similar neurons eg Cerbral Cortex, Cerebellum (c) Ganglion Groups of cell bodies in the PNS eg Dorsal Root Ganglia (d) Fibre Tracts Bundles of axons in the CNS eg Corpus Callosum (white matter) (e) Nerves Bundles of axons outside CNS. Often mixed sensory/motor. Synaptic Organisation Terminal portions of axons form synapses with other neurons which release chemical transmitters to relay the impulse. Neurons receive multiple inputs which are integrated at the postsynaptic neuron. The types of synapse are: (a) Axodendritic (usually excitory effect) (b) Axosomatic (usually inhibitory effect) (c) Axo-axonic (either to the hillock or terminal and usually modulatory) Neuroglia Support cells of the CNS which perform varying functions. They are in close contact with neurons and are essential for correct functioning. 1 ) Astroglia (Astrocytes) Astroglia are the most numerous of the neuroglia in the CNS and are closely associated with blood vessels, ventricles, neuronal soma, synapses and nodes of Ranvier Functions: 2) Oligodendroglia Myelinating cells of the CNS which are found in rows in axon tracts. They have small spherical nuclei with few processes. Functions: 3) Microglia (a) Scaffold for other cell types (b) Forms blood-brain barrier and brain-CSF barrier (c) K+ buffering (d) Removal and degradation of neurotransmitters (GABA) (e) Divides in response to injury (scar tissue formation) (a) Elaboration and maintenance of neuronal myelin (b) Forms up to 40 myelin nodes for up to 50 neurons (c) Very susceptible to nutritional state, toxins and infections (d) Involved in myelin disease states (eg multiple sclerosis) Derived from blood monocytes which invade to CNS during fetal development. Relatively small cells with highly branched processes. They turn into large phagocytosing cells during tissue damage. Functions: 4) Other Glial Cells (a) Resident macrophages of the CNS (b) Antigen Presenting capability (c) Role in tissue modelling Ependymal Cells: Form the simple cuboidal lining of the ventricles and central canal of the cord. They are ciliated at the luminal surface and have gap junctions NO TIGHT JUNCTIONS. Schwann Cells Envelop the axons of motor and sensory neurons. Produce myelin for cells of the PNS. They also have the same functions as the astrocytes and promote repair. Satellite Cells Perform the functions of astrocytes in the grey matter of the CNS. NEUROSCIENCE 3 (page 1 of 3) The Resting Potential Diffusion – movement of molecules from one location to another solely as a result of their random thermal motion Diffusion – movement of molecules from a region of higher concentration to a region of lower concentration Diffusion equilibrium – uniform concentration and no further net movement Flux – number of molecules (mols) crossing a surface per unit time (mols / s) Electrical concepts Electrical forces: another way to move molecules Opposite charges attract and like charges repel Force increases with the quantity of charge Membrane Potentials: key concepts >>>>> Ions, not electrons Potential (emf – electro-motive force): electrical force between ions that repels like charges and attracts opposite charges. Units: mV Current: movement of ions due to the influence of potential. Units: Amps Resistance of a material: a measure of how hard it is for current to flow through it. Units: Ohms Lipids: High Resistance, low permeability to ions Salt solution (ICF and ECF): Low Resistance, easy for ions to move Resting membrane potential - e.m.f. (voltage) between the inside and outside of a cell: •The zero reference point is outside the cell. •The inside of the cell is negative compared to the ref. •All cells have a membrane potential •In excitable cells (neurons and muscle cells) it is particularly important to cell function Understanding the ionic basis of the resting membrane potential Membrane separates charge. This can happen because both: 1. The membrane is selectively permeable. Lets some ions through, but not others. 2. The concentration of at least one permeant ion is different on the two sides of the membrane Permeability of a membrane to an ion: number indicating how easy it is for the ion to cross the membrane. Different for each cell !!! >> It is the flux of the ion through the membrane per unit of concentration gradient. >> Permeability depends on the type and number of specific ion channels in the membrane. Generation of a membrane potential due to diffusion through a selectively permeable membrane: Case 1. Membrane impermeable to all ions. No separation of charge. Membrane potential = 0 V Cell 1 NaCL @ 0.15 mM Cell 2 KCl @ 0.15 mM Case 2. Membrane permeable to K+ only (through K+ selective channels) . K+ diffuses down its conc gradient. Compartment 1 gains + and compartment 2 loses + causing separation of charge across the membrane. Cell 1 NaCL @ 0.15 mM More K+ diffuses and the voltage across the membrane increases (= membrane potential). As + charge increases in compartment 1, it increasingly repels entry of K + . Finally fluxes are equal, no net diffusion. Flux of K+ down its conc gradient (from 2 to 1) is equal to the flux of K+ down the electrical gradient (from 1to 2). Note that K+ conc in compartment 1 is still LESS than in compartment 2. Only a miniscule number of ions cross; the change in concentration is very, very small Cell 2 KCl @ 0.15 mM Case 3. Membrane permeable to Na+ only (through Na+ selective channels) . Na+ diffuses down its conc gradient. Compartment 2 gains + and compartment loses + causing separation of charge across the membrane. Note: the direction of charge movement is different than in previous case for a membrane permeable to K + Cell 1 NaCL @ 0.15 mM Cell 2 KCl @ 0.15 mM Finally fluxes are equal, no net diffusion. Note: compared to the previous case for a membrane permeable to K + the sign of the membrane potential is opposite to previous case even though the conc’s are the same as in the previous case The key difference is the selectivity of the membrane Electrochemical equilibrium for an ion is reached when its concentration gradient is balanced by the electrical gradient across the membrane. It is the electrical potential (voltage across the membrane) that prevents diffusion down the ion’s concentration gradient. Composition of the Main Fluid Compartments _______________________________________________ in plasma*** in muscle (mmol/l) (mmol/l) ______________________________________________ Na+ 150 10 K+ 5 150 2+ Ca 2 10-4 * Na and Cl most abundant in PLASMA. ClOrganic phosphates1Protein17- 110 5 1 5 130 2 * K and Organo-P most abundant in MUSCLE. pH 7.4 7.1 ---------------------------------------------------------------------osmolarity 285 mosm/l 285 mosmol/l Na+ and K+ are most important ions for the resting potential of neurons Nernst Equation: relates the size of the equilibrium potential of an ion to the size of its concentration gradient EX+ = (RT/ZF) ln (Co /Ci) R = gas constant, T = Temp. o Kelvin, Z = charge on ion (-1 for Cl-, +2 for Ca+2), F = Faraday’s number, 96,500 coulombs of charge per mol of ion with single charge, and ln means log to base e Substituting the constants and body temperature, and converting from ln to log gives: EX+ = (61/Z) log10 (Co /Ci) Nernst Equation: relates the size of the equilibrium potential of an ion to the size of its concentration gradient EX+ = 61 log10 (Co /Ci) >>> >>> The equilibrium potential for Na using the concentrations above is +72 mV The equilibrium potential for K using the concentrations above is – 90 mV. To check sign of equilibrium potential: What sign does the inside need to keep the concentration gradient as is? Real membrane potential for typical neuron is –70 mV. Not equal to the equilibrium potential of Na+, +72 mV Not equal the equilibrium potential of K+, -90 mV Real membrane potential is –70 mV, closer to K+ equilibrium potential because membrane is more permeable to K+ than to Na+. K+ diffuses down its conc gradient through permanently open K+ channels, so inside becomes negative. However, the membrane is slightly permeable to Na+, so some Na+ diffuses in down its conc gradient and cancel out the effect of an equivalent number of K + diffusing out. K+, Na+ and Cl- all contribute to the real membrane potential. The size of each ions contribution is proportional to how permeable the membrane is to the ion. Goldman Equation describes the resting membrane potential. Vm = (RT/F) x [ ln PK (Ko) + P Na (Nao) + PCl (Cl-i) ] / [ PK (Ki) + P Na (Nai) + PCl (Cl-o) ] Changes in membrane potential. Two types: Graded potentials and Action potentials Changes in membrane potential: some definitions Depolarisation (from -70 to 0 mV). Overshoot (from 0 to +60 mV). Repolarization (from 0/+60 to -70 mV). Hyperpolarization (from -70 to -90 mV). Resting potential (-70mV). Graded potentials: change in membrane potential in response to stimulation. Properties of graded potentials. Can be depolarizing or hyperpolarizing. A stronger stimulus produces a larger graded potential. Graded potentials get smaller the farther they travel (Decremental spread): >> Charge ‘leaks out’ of membrane! DO NOT LEARN THIS !!!!! NEUROSCIENCE 4 (page 1 of 3) The Action Potential The Ionic Basis of the Action Potential Key concepts •Permeability depends on channel state (open or closed) •When Pion increases the ion crosses the membrane down its electrochemical gradient. •This moves the membrane potential toward the equilibrium potential for that ion. ***Changes in membrane potential during the Action Potential are NOT due to ion pumps***** Action potential: amplitude: up to 100 mV change. Size depends on neuron type duration: a few ms (1ms = 0.001 s). Depends on neuron type (1-100 ms). Equilibrium potential for Na 1) Resting potential Equilibrium potential for K Five parts 1) Resting membrane potential. PK >> PNa, therefore membrane potential nearer equilibrium potential for K than that for Na Voltage-gated Na channels and Voltage-gated K channels Na Channel activation gate closed Na Channel inactivation gate open K channel closed 2) The stimulus depolarizes the membrane potential (moves it in the + direction). This part of the action potential is also called the “foot”. Its shape is exaggerated in the diagram. 3) Upstroke phase. PNa increases because the Voltage-gated Na channels open quickly. The upstroke starts when the membrane potential reaches the threshold potential. Na ions enter the cell down their electrochemical gradient. PK also increases as the Voltage-gated K channels start to open, but this is slower. K ions leave the cell down their electrochemical gradient, but fewer than Na ions entering. Net effect: Membrane potential moves toward the Na equilibrium potential (more Na IN than K OUT!!) Voltage-gated Na channels and Voltage-gated K channels Na Channel activation gate open Na Channel inactivation gate open K channel closed 4) Repolarization phase. PNa decreases because the Voltage-gated Na channels inactivate. Na entry stops. PK increases as the Voltage-gated K channels remain open. K ions leave the cell down their electrochemical gradient. Net effect: Membrane potential moves toward the K equilibrium potential During Repolarization (early) Voltage-gated Na channels and Voltage-gated K channels Na Channel activation gate open Na Channel inactivation gate closed - ↓ Perm. to Na K channel open Absolute refractory period: Voltage-gated Na channel cannot open (inactivation gate reders it insensitive to Voltage!!!) Stimulus, even if stronger than usual, does not trigger an Action Potential Repolarization (late) Voltage-gated Na channels and Voltage-gated K channels Na Channel activation gate closed Na Channel inactivation gate closed K channel open Absolute refractory period: Voltage-gated Na channel cannot open 5) After-hyperpolarization phase. PK is greater than at rest because the Voltage-gated K channels are still open. K ions continue leaving the cell down their electrochemical gradient. Membrane potential moves closer to the K equilibrium potential until the Voltage-gated K channels close. Then the membrane potential returns to the resting potential. Voltage-gated Na channels and Voltage-gated K channels Na Channel activation gate closed Na Channel inactivation gate open K channel open Relative refractory period: a stronger than normal stimulus is needed to open the Voltage-gated Na channel Na channels in resting state, but K channels are open !!!!!! DOES NOT OCCUR IN ALL CELLS !!!!!! Summary of time-course of changes in Permeability to Na and to K during the Action potential: Na equilibrium potential +30 30 Permeability Membrane potential Membrane potential (mV) 20 10 PNa PK 0 -70 0 2 4 K equilibrium potential Time (ms) Regenerative Relationship between PNa and Membrane Potential •Threshold: change in membrane potential required to open voltage-gated Na channels. •All-or-Nothing” nature: once threshold has been reached a full size action potential is produced. •Refractory state: unresponsive to stimulus Initially depolarization is caused by an event outside the cell (stimulus such as transmitter binding to receptor, etc). If less than threshold, graded potential returns to Resting potential. Once threshold is reached the cycle continues. Positive feedback behaviour. Depolarisation causes Opening of Voltage-gated Na channels causes increase in Na Permeability causes Increase Na entry into cell causes depolarisation causes…etc,etc Self-regenerating process or All-or-Nothing Response: once threshold is reached a full sized action potential is produced The cycle continues until the Voltage-gated Na channels inactivate which means they close and become Voltage- insensitive. The membrane remains in a refractory (unresponsive) state until the Voltage-gated Na channels recover from inactivation and become Voltage-sensitive again. Propagation of the Action Potential: Local current flow depolarizes new adjacent region toward threshold Direction of propagation of action potential Remainder of axon at resting potential New active area at peak of action potential Old active region returning to resting potential New adjacent area at resting potential Ion movements during the action potential •Na ions enter the cell, and K ions leave the cell. •BUT only a very small number of ions cross the membrane and change the membrane potential. •The concentration change is extremely small, less than 0.1% **Ion pumps are NOT directly involved in the ion movements during the Action Potential** >> e.g. Na/K pump: Between action potentials Na/K pump returns ions that moved durin AP Action potential travels quickly Velocity range in mammals axons: Large diameter, myelinated axons 120 m/s Small diameter, non-myelinated axons 1 m/s Axon diameter and myelination affect conduction velocity Conduction velocity •Increases with axon diameter because of the electrical properties (less resistance to current flow inside the large diameter axon, etc) •Is higher in myelinated than non-myelinated axons of the same diameter because of electrical properties (action potentials only occur at nodes of Ranvier, etc). >Conduction velocity is reduced by factors that: • Reduce axon diameter (regrowth after injury) or • Reduce myelination. Conduction may be blocked due to extensive localized loss of myelin. Multiple sclerosis and diphtheria are examples of demyelinating diseases. • Conduction velocity is also reduced by cold, anoxia, compression and drugs (some anaesthetics). NEUROSCIENCE 5 (page 1 of 3) Neurotransmitters Neurotransmitters: • Provide enormous diversity in the variety transmitters (~ 200) and the genes that encode their receptors (~ 300). • Amino acids (e.g. glutamate and gamma amino butyric acid [GABA]), amines (e.g. noradrenaline and dopamine) and neuropeptides (e.g. opioid peptides). • May mediate rapid (µs- ms) or slower effects (ms-s). • Vary in abundance from mM to nM CNS tissue concentrations Neurones receive multiple transmitter influences which are integrated to produce diverse functional responses Neurotransmitter Synthesis Neurotransmitter Release ElectroMechanical Transduction 200µs REQUIREMENTS: 1) Biosynthesis: Glutamate GABA ; Glutamic Acid Decarboxylase (GAD) 2) Followed by packageing in Synaptic Vesicles (near Synaptic Cleft) (a) Action Potential -> Membrane Depolarisation reaches nerve terminal opening Ca2+ channels. (b) Ca2+ ions enter terminal and activates neurotransmitter vesicles (c) Vesicles dock on the presynaptic membrane (d) Vesicles fuse to membrane and form pore (e) Transmitter is released by exocytosis (f) Vesicle is recycled back into the membrane (g) Vesicle is filled with more neurotransmitter • Ca2+ • Transmitter containing vesicles to be docked on the presynaptic membrane • Vesicular release of neurotransmitter (T) FILLING Protein complex formation between vesicle, T T membrane and cytoplasmic proteins to enable ENDOCYTOSIS T vesicle proteins both vesicle docking and a rapid response to Ca2+ entry leading to membrane fusion and exocytosis. • ATP • Vesicle recycling Synaptic Transmission T T T DOCKING T T T MEMBRANE FUSION & EXOCYT OSIS Presynaptic membrane proteins (a) Quanta Hypothesis – quanta ~ 4-10 thousand molecules of NT (b) Synaptic Vesiccles – Small Clear-Cored (ACh) 200µs Large Dense-Cored (Neuropeptides+Proteins) 50ms RELEASE OCCURS IN RESPONSE TO INCREASED [Ca2+] = 200µM Fast/Slow Systems Fast (milliseconds) acting neurotransmitter systems are Ligand-Gated Ion Channels. They act in a space of milliseconds and use amino acids as the neurotransmitter including: (a) GABA (γ-amino butyric acid) CNS (b) Glutamate (Glu) CNS (c) Aspartate (Asp) CNS (d) Acetylcholine (Ach) NMJ Slow acting systems (seconds/minutes) are G-Protein Linked Receptors. They act in seconds or minutes and use monamines or neuropeptides as neurotransmitters including (in CNS and PNS): (a) Acetylchloine (ACh) – muscarinic receptors (b) Dopamine (DA) (c) Noradrenaline (NA) (d) 5-hydroxytryptamine (5-HT) (e) Neuropeptides – enkaphalin (endogenous opiate) T TT Inhibition/ Excitation Neurotransmitters can have either an inhibitory or an excitatory effect on the postsynaptic membrane. Inhibition -Inhibitory Post Synaptic Potential (IPSP)occurs when the membrane potential is moved away from the threshold potential by the neurotransmitter (usually by increasing permeability to Cl- ions). Excitation Excitatory Post Synaptic Potential (EPSP) occurs when the membrane potential is moved towards the threshold value (usually by increasing sodium and potassium permeability). Diffuse/Precise A diffuse system is one in which the impulse is spread to numerous postsynaptic neurones (eg some NA, DA systems) whereas a precise system is one where the impulse is spread to few specific neurones. Modulatory systems affect the cortex, brain stem and spinal cord and affect arousal, mood, motivation and sleeping. Receptors GLUTAMATE RECEPTORS Na + Ca 2+ Na + AMPA RECEPTORS NMDA RECEPTORS alpha amino-3-hydroxy-5-methyl4-is oxaz ole propionic acid N-methy l-D aspartate Majority of FAST excitatory synapses Rapid onset, offset and desensitisation Slow component of excitatory transmission Serve as coincidence detectors which underlie learning mechanisms • An excitatory CNS synapse is mediated by GLUTAMATE. • Recylcing of GLUTAMATE by Excitatory Amino Acid Transporter (EAAT) in Glial Cell or Pre Synaptic Nerve terminal. Abnormal cell firing leads to seizures associated with excess GLUTAMATE in the synapse Pentameric organisation of the GABA receptor and pharmacologically important binding domains GABA steroids barbiturates ß benzodiazepines alpha • ethanol SEE TUTORIAL SHEET FOR DIAGRAM OF GABA SYNAPSE. Zn convulsants Drugs facilitating GABA transmission are: antiepileptic anxiolytic sedative muscle relaxant Drug Treatment Drugs acting on GABA receptor to increase affinity for GABA cause: (a) Sedation, Sleep (b) Anticonvulsant (c) Reduced voluntary muscle tone Drugs acting to block sodium channels are used as antiepileptics since they stop rapid firing of neurones eg Phenytoin and Carbamazepine. Increased GABAergic action also helps prevent seizures. Dopaminergic drugs such as L-DOPA which can pass through the blood-brain barrier are used to treat Parkinson’s which is due to loss of dopaminergic cells Tiagabine INCREASES transmitter availability by blucking GABA transporters (stays in synapse for longer as it is not taken up and recycled). Vigabatrin INHIBITS inactivation of neurotransmitter (GABA transaminase). Benzodiazapines and Barbiturates increases activation of receptors (GABAA Receptor) Epilepsy: Refers to a disorder of brain function characterized by the periodic and unpredictable occurrence of seizures. A seizure is the transient alteration of behaviour due to the disordered, synchronous, and rhythmic firing of populations of brain neurones. The pharmacological agents in current clinical use for inhibition of seizures are referred to as anticonvulsant or antiepileptic drugs. Seizures are thought to arise from the cerebral cortex and they can be classified into partial seizures, those beginning focally at a cortical site, and generalized seizures, those that involve both hemispheres widely from the outset. The behavioural manifestations of a seizure are determined by the functions normally served by the cortical site at which the seizure arises. Thus, for example, a seizure involving the motor cortex is associated with clonic jerking of the body part controlled by this region of the cortex. A simple partial seizure is associated with preservation of consciousness, whilst a complex partial seizure is associated with impairment of consciousness. Examples of generalized seizures include absence, myoclonic and tonic-clonic seizures. Neurotransmitters in epilepsy: Epilepsy is a neurological disorder associated with abnormal neurotransmitter function in the brain. A decrease in GABA-mediated inhibition or an increase in glutamate-mediated excitation in the brain may result in seizure activity. Indeed, both glutamate and GABA are thought to play key roles in the brain mechanisms causing epilepsy in man. Pharmacological evidence for a role of neurotransmitters in epilepsy · Impairment of GABA-mediated inhibition causes seizures in animals e.g. impairment of synthesis, release (tetanus toxin) or postsynaptic action (bicuculline, picrotoxin). · Enhancement of GABA-mediated inhibition leads to seizure suppression e.g. central (i.c.v.) administration of GABA or inhibition of the GABA metabolizing enzyme GABA-T (vigabatrin). · Many clinically useful anticonvulsant drugs are known to act, at least in part, by potentiating central GABA-mediated inhibition e.g. benzodiazepines, phenobarbital (see Section 3). · Central (i.c.v.; focal) administration of glutamate or glutamate receptor agonists causes seizurelike activity in animals. · Glutamate receptor antagonists are anticonvulsant in experimental models of epilepsy. · Some therapeutically effective anticonvulsant drugs act partly by blocking glutamate-mediated excitation in the brain e.g. phenobarbital. Biochemical evidence for a role of neurotransmitters in epilepsy · Cobalt-induced seizures in rodents are associated with glutamate release and with GABA concentration, GAD activity and GABA uptake (probably reflecting GABA neurone loss) at the seizure focus. · Audiogenic seizures in mice (DBA/2 mice) are associated with glutamate receptor binding in the brain and with GABA release from depolarized brain slices. NEUROSCIENCE 6 (page 1 of 4) The Central Nervous System Divisions: The CNS is divided into the following major divisions: (a) Spinal Cord – controls reflex sensori-motor functions and autonomic function (b) Brainstem (medulla, pons, midbrain) – controls vital functions (eg breathing) (c) Cerebellum – controls co-ordination of movement (d) Diencephalon (thalamus, hypothalamus) – interfaces CNS, ANS, endocrine (e) Cerebral hemispheres (cortex, ganglia) – all functions Define the functions of the dorsal and ventral horns of the spinal cord and how the dorsal and ventral roots and spinal nerves relate to them: Ventral horn contains cell bodies of somatic motor neurons and motor nuclei (carries motor signals out to body); exits spinal cord to form the ventral root, then combines with the dorsal root to form the spinal nerve Dorsal horn contains autonomic and somatic sensory nuclei (receives sensory information from the Body) Define the 3 components of the brainstem and state the main functions of the brainstem: Midbrain, Pons, Medulla oblongata; the brainstem is a netlike region of interspersed grey and white matter; medulla contains sensory and motor neurons, many nuclei – affiliates with 5/12 cranial nerves, the cardiovascular centre and part of the respiratory centre; Pons is a bridge that connects the cerebellum by transverse neurons and are also part of the sensory and motor tracts, it is also involved in the respiratory centre; Midbrain contains tracts and nuclei, contains neurons for muscle activity, input from proprioceptors Define the functions of the 2 main structures of the diencephalons: Thalamus – relay between lower structures and cerebral cortex Hypothalamus – control of homeostasis, interface between CNS, ANS and endocrine system State the functions of the basal ganglia and cerebellum: Cerebellum - coordinates movement (CANNOT INITIATE IT) Basal ganglia – controls movement (TOGETHER THEY :regulate posture and balance) Lateral aspect of left cerebral hemisphere - Cortical lobes: Explain the structure and functions of the meninges: Cranial meninges protect and cover the brain and are continuous with spinal meninges >> Dura mater – tough membrane attached to bone or forming partitions (dural folds) with venous sinuses in their margins >> Arachnoid membrane – thin membrane attached to the underside of the dura >> Pia mater – delicate membrane closely adherent to the surface of brain and spinal cord Explain the relationship between the spinal segments, spinal nerves and vertebrae and state at what level a lumbar puncture can be performed safely: Spinal Cord The spinal cord has various spinal and vertebral levels with nerves arising from each. There are 31 pairs of spinal nerves: (a) Cervical (C1 – C8) 08 C1-7 above; C8 below 7 (b) Thoracic (T1 – T12) 12 below corr. Vert. 12 (c) Lumbar (L1 – L5) 05 below corr. Vert. 5 (d) Sacral (S1 – S5) 05 below corr. Vert. 5 (e) Coccygeal Nerve 01 between vertebrae 2 Nerves 31 Vertebrae 29 Lumbar puncture between L3/L4 or L4/L5 NOT L2 OR ABOVE Spinal nerves leave the intervertebral foramen between the named vertebrae the immediately superior vertebrae Identify the components of the ventricular system and relate them to the divisions of the CNS: >> Lateral ventricle relates to the cerebral hemisphere (1 in each hemisphere) >> 3rd ventricle relates to the diencephalon (in the middle of the diecephalon) >> Aqueduct relates to the midbrain >> 4th ventricle relates to the pons and medulla at the front and the cerebellum at the rear >> Central Canal goes through the centre of the sinal cord for almost the entire length. Define herniation as applied to the brain and explain its clinical significance: Herniation is displacement of brain tissue by either a tumour or bleed; a space-occupying lesion may cause herniation of brain tissue from one compartment to another Explain the composition, circulation and functions of CSF The CSF: Contains fewer cells, less protein, less K+ and Ca+ and higher Mg+ and Cl- than blood; A colourless liquid that protects the brain and spinal cord from chemical and physical injury; Carries oxygen, glucose and other necessities from the blood to the neurons and Neuroglia; Circulates through the subarachnoid space, around the brain and spinal cord, and through the ventricles within the brain and spinal cord; It is produced in the choroids plexuses, networks of capillaries in the walls of the ventricles that filter and secrete into the blood plasma; Ependymal cells cover these capillaries and their tight junctions form the blood-CSF barrier Volume is 80-150ml, Flow Rate is 500ml/day Define hydrocephalus, its pathology and outline how it may be treated: Hydrocephalus is caused by elevated CSF pressure; can arise when drainage of the CSF from the ventricles is compromised; o 2 types – communicating (all ventricles affected) and non-communicating (not all affected) Signs and symptoms; child – increased head circumference, irritability, loss of upward gaze; adult – headache, drowsy and blackouts Treated by: draining excess CSF, or by inserting a shunt from the lateral ventricle to the vena cave or abdominal cavity Define meningitis and its pathology, distinguishing between viral and bacterial aetiology: Meningitis is the infection of the pia mater and subarachnoid space; symptoms are headache, fever, tiredness and irritability; confusion, drowsiness, neck stiffness; rash in 75% Bacterial meningitis – CSF is TURBID, Hi WBC count (neutrophils), glucose level is low Viral meningitis – CSF is normal, any increase in WBC is predominantly lymphocytes; found in HIV patients, mumps/glandular fever Distinguish between an epidural and subdural haemorrhage: Epidural/Extradulral: Usually due to a damaged meningeal artery between the skull and the dura after a head trauma. >> Arterial – High pressure – Quicker development of Lesion and Symptoms Subdural: Usually due to a damaged veinbetween the dura and the arachnoid membrane. >> Venous – Lower Pressure – Slower development of Lesion and Symptoms. BOTH can cause a space occupying lesion in the confined space of the cranium and hence neurological deficits Inferior aspect of brain Inside of base of skull NEUROSCIENCE 7 (page 1 of 2) The Peripheral Nervous System PNS The Peripheral Nervous System consists of the nerves emerging from the brain and spinal cord which innervate the peripheral organs. Axons are found in bundles; axon is surrounded by the endoneurium, which are bundled into fascicles surrounded by perineurium, which are bundled into whole nerves surrounded by epineurium >> NEURONS: cell bodies are located either in CNS (motor neurons) or in peripheral ganglia; axons project towards targets. >> GLIAL CELLS: Schwann cells and satellite glial cells Divisions The PNS is divided into efferent and afferent divisions, motor neurons/ANS neurons and sensory neurons respectively: (a) Efferent – responsible for transmission of information out of the CNS to effectors (i) Somatic motor neurons (innervating skeletal muscle) (ii) Autonomic neurons (innervating glands and viscera) (b) Afferent – responsible for transmitting information from recpetors to the CNS (i) Sensory neurons (innervating skin, joints, viscera) Spinal Nerves A typical spinal nerve supplies one region of the body (a dermatome of skin) They consist of: (a) a ventral root (motor) (b) a dorsal root (sensory) (c) a dorsal root ganglion where they meet The spinal nerves also divide into several branches called rami These are: (a) the dorsal ramus (innervating skin and muscle of the back) (b) the ventral ramus (innervating skin, chest muscles, limbs, pelvis) (c) the rami comunicantes(sympathetic neurons innervating viscera) There are 31 pairs of spinal nerves (SEE p1 Neuroscience 5) The upper limbs are supplied by nerves C5 to T1 via the Brachial plexus The lower limbs are supplied by nerves L2 to S2 via the Lumbo-sacral plexus Each nerve also supplies half the adjacent dermatome so that a lesion in one nerve will not result in complete loss of sensitivity (anaesthesia) but rather a decrease in sensitivity (hypoaesthesia) Knowing which spinal nerve supplies which area of skin means that loss of sensitivity in an area can point to the damaged region of the spinal cord The ventral rami of the spinal nerves (except T2-T12) form network of nerves called plexuses. The brachial and lumbo-sacral plexuses supply the innervation of the upper and lower limbs respectively In a plexus, the nerve fibres (axons) of different spinal nerves are recombined to form a peripheral nerve. Therefore, peripheral nerves contain axons from different spinal nerves. Peripheral nerve injury or nerve compression may result in complete sensory and motor loss over the area supplied by the nerve. Some examples of vulnerable nerves: o ulnar nerve: the nerve lies near the surface of the elbow and is easily damaged resulting in wasting of hand muscles and loss of sensation over the little finger. o median nerve: may become compressed and damaged as it passes a narrow tunnel in the wrist, resulting in wasting of the thumb muscles (carpal tunnel syndrome) o sciatic nerve: injured in the buttock by badly placed injections, resulting in paralysis of the foot and loss of sensation over the front and back of the lower leg and foot. Peripheral Nerves Each peripheral nerve forms bundles called fascicles which divide along its length supplying various regions of the body. Each part is surrounded by a connective tissue sheath: (a) epineurium loose connective tissue surrounding the whole nerve (b) perineurium dense connective tissue surrounding a fascicle (c) endoneurium loose connective tissue surrounding individual nerves Nerve fibre classification Nerve fibres can be classified on the basis of structural (e.g. size and whether or not the fibres are myelinated) and functional criteria (e.g. conduction velocity). In general, the larger the diameter the faster the axonal conduction velocity Peripheral nerves usually contain a mixture of fibres of different diameter and conduction velocity (CV). The compound action potential recorded from a nerve contains several peaks reflecting the CV of different classes of nerve fibres (see diagram below) Myelinated fibres Schwann cell membrane wraps around a single axon in a spiral fashion forming up to 100 layers of myelin. Each cell covers only a small segment of the axon (internode) The junction where two Schwann cells meet is devoid of myelin (node of Ranvier) Saltatory conduction: conduction velocity is faster in myelinated fibres because the action potential (AP) jumps from one node to the next Unmyelinated fibres Several nerve fibres lie within invaginations of the Schwann cell Axonal diameter (~1 µm) is much less than that of myelinated axons (1.5-20 µm) Continuous conduction: AP causes depolarisation of immediately adjacent membrane. If a peripheral nerve is damaged the can be regenerated by this process: (a) Within 48hrs the axon and sheath beyond the crush/cut is phagocytosed by macrophages (Wallerian degeneration) (b) The cell bodies undergo metabolic changes (Chromatolysis) (c) The proximal axon find Schwann cells and endoneurial sheaths (d) Failure causes trapped axons called a neuroma (e) Otherwise regeneration of the axon is 2-5 mm per day and will be complete from 1 month to 1 year Diagnostic Techniques (a) Nerve Conduction Velocity can determine if peripheral neuropathy is present, and whether it is demyelinating or axonal. (b) Nerve biopsy of a small peripheral nerve can be used to study pathogenesis of the disease. NEUROSCIENCE 8 (page 1 of 3) The Autonomic Nervous System Functions The autonomic nervous system (ANS) is the part of the nervous system that controls involuntary activity (eg homeostasis) Examples include: (a) Blood Pressure Regulation (b) Respiration Regulation (c) Gastrointestinal Motility (d) Temperature Regulation It is divided into two separate systems: (a) Parasympathetic (“Eat and Sleep” functions) Discrete and specific (b) Sympathetic (“Fight or Flight” functions) Diffuse stimulating whole body Baroreceptor Reflex This maintains blood pressure. Increased arterial pressure stimulates baroreceptors which increase afferent nerve activity which in turn decreases sympathetic activity which leads to decreased heart rate and vasodilation which decreases blood pressure Fight or Flight Reflex This is a mass Sympathetic discharge in response to stress or alarm and induces: (a) increased blood pressure (b) increased blood flow to muscle (c) decreased blood flow in other areas (eg splanchnic bed) (d) increased blood glucose (e) increased respiration Sympathetic Anatomy The sympathetic nerves are from T1 to L3 down the spinal cord There are many more post-ganglionic nerves than there are pre-ganglionic. This causes diffuse sympathetic effects. ParasympatheticThe parasympathetic nerves are from either the cranial or sacral outflow. Anatomy There are five main ganglia: (a) Occulomotor nerve (IIIrd Cranial) (b) Facial nerve (VIIth Cranial) (c) Glossopharyngeal nerve (IXth Cranial) (d) Vagus nerve (Xth Cranial) (e) Splanchnic nerve Describe the sympathetic and parasympathetic pathways and their central/spinal connections Sympathetic preganglionic neurons have their soma in the lateral horns of the grey matter in the 12 thoracic segments and first 2 lumbar segments. Ganglia are either sympathetic trunk ganglia or prevertebral ganglia, servicing organs above and below the diaphragm respectively; they are close to the CNS and so preganglionic sympathetic neurons are usually short; preganglionic neurons can also synapse with the adrenal medulla which secretes products into the bloodstream – it is a neuroendocrine organ Parasympathetic preganglionic neuron soma are located in the nuclei of the 4 cranial nerves in the brain stem, and in the lateral grey horns of S2-S4 (sacral); ganglia are terminal, located close to or within the wall of the visceral organ – the preganglionic neurons are therefore long Identify the neurotransmitter substances released at different levels within the autonomic nervous system Parasympathetic solely use ACh; Sympathetic use ACh at the ganglion then NA/NE at the effector; o preganglionic fibres to the adrenal medulla use ACh; o sympathetic fibres to sweat glands however use ACh as both the pre and post ganglionic neurotransmitters Sympathetic: (i) typical Effector cell Pre-ganglionic fibre ACh Nicotinic receptor Post-ganglionic fibre NA Adrenoceptor ( or ) (ii) adrenal medulla Adrenaline + noradrenaline ( 20%) are transported by the blood stream to their receptors Pre-ganglionic fibre AC Nicotinic receptor h Chromaffin (a) Parasympathetic Pre-ganglionic fibre ACh Nicotinic receptor Postganglionic fibre cell Effector cell (iii) exceptions ACh Muscarinic receptor Pre-ganglionic fibre AC h Nicotinic receptor Post-ganglionic fibre AC h Effector cell (e.g. sweat gland) Muscarinic receptor Describe the biosynthesis and metabolism of ACh, NA and A ACh is formed from acetyl-CoA and choline, which, via the enzyme choline acetyl transferase, produces ACh and CoA; on the receptor ACh is broken down by acetylcholinesterase into acetate and choline, which is transported back into the pre-synaptic bulb and reused NA is formed from the amino acid tyrosine → DOPA (tyrosine hydroxylase); → dopamine (DOPA decarboxylase; → NA (dopamine β hydroxylase); from the receptor NA is actively taken back into the pre-synaptic bulb where it is metabolised by Monoamine oxidase A. Or it is taken into Glial Cells and degraded (COMT). Giving MOPEG and VMA which are conjugated (glucuronide/sulphate) and excreted. A is formed from NA via phenylethanolamine methyl transferase Describe the influence of the sympathetic and parasympathetic nervous systems on principal organs/systems of the body Organ/System Effect of sympathetic Effect of parasympathetic Cardiovascular ↑ - Increases cardiac output ↑ - Slows HR; vasodilatation of (ionotropic effect SV and certain blood vessels to discrete chronotropic effect HR); glands and organs (e.g. willy) increased TPR ↓ - vasodilatation (due to decreased sympathetic tone) Gastrointestinal Decreases motility and tone; Increases motility and tone; stimulates contraction of relaxation of sphincters; stimulates sphincters; inhibits secretory secretory activity activity Eye muscles Relaxes ciliary muscle, lens Contracts ciliary muscle, lens flattens for distant vision; bulges for near vision; contracts contracts radial muscle (pupil pupillary sphincter (pupil dilation) contraction) Bladder ↓ - relaxation of the sphincter Main influence; ↑ - contraction of vesicae (via hypogastric nerve) detrussor muscle and relaxation of sphincter vesicae (via pelvic nerve) Lungs ↑ - dilates bronchi and bronchioles (↑ O2 delivery) Willy ↑ - penile flaccidity; ejaculation ↑ - boner Describe the concept of dual innervation Most organs have both sympathetic and parasympathetic innervation each of which usually has an opposite effect (Control of HR and Bronchiole Diameter). There is also a certain amount of Autonomic tone which contrivutes to the normal firmness of a tissue/organ. Give an example of an autonomic reflex – pupil constriction in response to light In the eye there are two sets of muscles, the circular and the radials. In moments of high drama the sympathetic fires and contracts the Radial muscles (lens flattens for distant vision) - pupil dilatation. Mydriasis - ATROPINE In quieter times the parasympathetic is dominant and contracts the Circular muscles (lens bulges for near vision) - pupil contraction. Miosis – Pilocarpine. Retinal photoreceptors detect the light; optic nerve (cranial II sensory) transmits a signal to the pretectal nucleus; then to the Edinger Westphal Nucleus; signal then transmitted along the occulomotor nerves (cranial III motor) to the ciliary ganglia causing parasympathetic innervation of the pupillary sphincter Classify the cholinergic receptors within the ANS Nicotinic receptors on post ganglionic fibres and Chromaffin cells of the nicotinic receptor; transmission is fast as these are ligand gated ion channels; Muscarinic receptors on receptor organs; transmission is relatively slow and is mediated by G-protein coupled receptors produce a magnifying effect and are found on a) effector organs with parasympathetic innervation, b) sweat glands, which have sympathetic innveration). Classify the adrenergic receptors within the ANS Adrenoceptors are primarily found on the effector cells of the sympathetic nervous system. They are classifid into alpha and beta subclasses depending on the specific responses they elicit and the selective binding of drugs that activate or block them. Alpha examples – radial muscle in eye, salivary glands, sphincter muscles of stomach and bladder. Beta examples – cardiac muscle, smooth muscle of airways (qv asthma), liver. These are also G-protein coupled Generally speaking Alpha1 and Beta1 receptors generally produce excitation whilst Alpha2 and Beta2 receptors generally cause inhibition. There is a third type, Beta3, which are found only on brown adipose tissue and bring about thermogenesis. Describe how autonomic activity can be estimated with physiological and biochemical examples Monitoring blood pressure and heart rate; responses to heat (i.e. no sweat); control of organs e.g. constipation, emptying of bladder, sexual function Sympathetic activity monitored by plasma NA and A levels Postural hypotension, tachycardia, loss of pupil reflexes, loss of pulse response to forced expiration, no sweating or pupil reflexes on the injection of certain agents. Take blood pressure in different positions to check postural hypotension. CLASSIFY DISORDERS OF THE AUTONOMIC NERVOUS SYSTEM WITH EXAMPLES OF LOCALISED AND GENERALISED DISORDERS. Disorder may be a systemic one or confined to a particular region; for example in Pheochromocytoma, a mass in the adrenal gland, which causes excessive release of adrenaline and noradrenaline and causes headaches, palpitations, raised blood pressure, tachycardia and other adrenergic effects. Or the condition may be confined to a particular region, such as with trauma patients who have damaged their spine in a certain area and lost autonomic function at nerves below that point. DESCRIBE THE MAIN ABNORMALITIES IN AUTONOMIC FAILURE. Postural hypotension, tachycardia, impotence, ejaculatory failre, incontinence, constipation, diarrhoea, inability to sweat, dry mouth and eyes, Horner’s syndrome, held dilatation or constriction, sluggish or absent light response.