* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Skeletal System
Neuromuscular junction wikipedia , lookup
Optogenetics wikipedia , lookup
Neurotransmitter wikipedia , lookup
Molecular neuroscience wikipedia , lookup
Central pattern generator wikipedia , lookup
Neuroregeneration wikipedia , lookup
Perception of infrasound wikipedia , lookup
Neuropsychopharmacology wikipedia , lookup
Axon guidance wikipedia , lookup
Anatomy of the cerebellum wikipedia , lookup
Development of the nervous system wikipedia , lookup
Clinical neurochemistry wikipedia , lookup
Feature detection (nervous system) wikipedia , lookup
Caridoid escape reaction wikipedia , lookup
Nervous system network models wikipedia , lookup
Synaptic gating wikipedia , lookup
Premovement neuronal activity wikipedia , lookup
Stimulus (physiology) wikipedia , lookup
Basal ganglia wikipedia , lookup
Synaptogenesis wikipedia , lookup
Neuroanatomy wikipedia , lookup
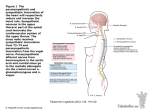
The Autonomic Nervous System Chapter 14 Introduction The stability of our internal environment depends largely on the autonomic nervous system Autonomic nervous system(ANS) receives signals from visceral organs The ANS makes adjustments as necessary to ensure optical support for body system Overview of the ANS The autonomic nervous system differs in it’s – Effectors – Efferent pathways – Target organs Effectors of ANS The somatic nervous system stimulates skeletal muscles The ANS innervates cardiac and smooth muscles and glands Efferent Pathways and Ganglia In the somatic system – Cell bodies are within the central nervous system – Axons extend to the muscles they serve – Somatic motor fibers are thick, heavily myelinated Type A fibers that conduct impulses very rapidly Efferent Pathways and Ganglia In the autonomic nervous system – The motor unit is a two neuron chain – The cell body of the first neuron, the preganglionic neuron, resides in the brain or spinal cord – Its axon, the preganglionic axon, synapses with the second motor neuron, the postganglionic neuron, in an autonomic ganglion outside the central nervous system – The postganglionic axon then extends to the effector organ Efferent Pathways and Ganglia Axons of most preganglionic neurons run from the CNS to synapse in a peripheral autonomic ganglion with a postganglionic neuron Efferent Pathways and Ganglia Axons of postganglionic neurons run from the ganglion to the effectors (cardiac and smooth muscle fibers and glands) Efferent Pathways and Ganglia Preganglionic axons are lightly myelinated thin fibers Postganglionic axons are even thinner and are unmyelinated Conduction though the autonomic chain is slower than through the somatic motor Many pre and postganglionic fibers are incorporated into spinal or cranial nerves for most of their course Efferent Pathways and Ganglia Remember that autonomic ganglion are motor ganglia, containing the cell bodies of motor neurons They are sites of synapse and information transmission from pre to postganglionic neurons Also note that the somatic motor division lacks ganglia entirely Neurotransmitter Effects All somatic motor neurons release acetylcholine at their synapses with their effectors, skeletal muscle fibers The effect is always excitatory, and if stimulation reaches threshold, the skeletal muscle fibers contacts Neurotransmitter Effects Neurotransmitters released onto visceral effector organs by postganglionic autonomic fibers include – Norepinephrine secreted by most sympathetic fibers – Acetylcholine released by parasympathetic fibers Depending on the receptors present on the target organ, its response to these neurotransmitters may be either excitation or inhibition Overlap of Somatic & Autonomic Higher brain centers regulate and coordinate both somatic and visceral motor activities Nearly spinal nerves and many cranial nerves contain both somatic and autonomic fibers Most of the body’s adaptations to changing internal and external conditions involve both skeletal activity and enhanced response of visceral organs Divisions of ANS There are two division of the ANS – Parasympathetic – Sympathetic Generally the two divisions serve the same visceral organs but cause essentially opposite effects If one division stimulates certain smooth muscle to contract or a gland to secrete, the other division inhibits that action Through this process of duel innervation the two systems counterbalance each other Divisions of ANS The sympathetic part mobilizes the body during extreme situations (such as fear, exercise or rage) The parasympathetic division allows us to unwind as it performs maintenance activities and conserves body energy Role of Parasympathetic Division The parasympathetic division is most effective in non-stressful situations This division is chiefly concerned with keeping body energy use as low as possible, even as it directs body processes such as digestion and elimination Resting and digesting division Role of Sympathetic Division Its activity is evident when we are excited or find ourselves in emergency or threatening situations (frightened) Pounding heart; rapid, deep breathing; cold, sweaty skin; and dilated eyes are signs Also changes in brain wave patterns Its function is to provide the optimal conditions for an appropriate response to some threat (run / see / think) Role of Sympathetic Division During exercise the sympathetic division also promotes physiological adjustments – Visceral blood supply is diminished – Blood is shunted to working musculature – Bronchioles of the lungs dilate to increase ventilation – Liver releases more sugar into blood stream to support metabolism Anatomy of ANS The sympathetic and parasympathetic divisions are distinguished by – Unique sites of origin – Different lengths of their fibers – Location of their ganglia Anatomy of ANS Unique origin sites – Parasympathetic fibers emerge from the brain and spinal cord at the sacral level – Sympathetic fibers originate from the thoracic and lumbar regions of the spinal cord Anatomy of ANS Different Lengths of their Fibers – Parasympathetic division has long preganglionic and short postganglionic fibers – Sympathetic is the opposite with short preganglionic and long postganglionic fibers Anatomy of ANS Length of their Ganglia – Most parasympathetic ganglia are located in the visceral effector organs – Sympathetic ganglia lie close to the spinal cord Parasympathetic Division The parasympathetic emerge from opposite ends of the central nervous system The preganglionic axons extend from the CNS nearly all the way to the structures to be innervated Parasympathetic Division The preganglionic neurons synapse with the ganglionic neurons located in terminal ganglia Very short post ganglionic axons issue from the terminal ganglia and synapse with effector cells in their immediate area Parasympathetic Division Several cranial nerves contain outflow of the parasympathetic Preganglionic fibers run in the oculomotor, facial, glossopharyngeal, and vagus nerve Cranial Outflow Oculomotor nerve III – The parasympathetic fibers of the oculomotor nerves innervate smooth muscles of the eye • Constrictor muscles of iris cause pupil to constrict • Ciliary muscle within the orbits of the eye controls lense shape for visual focusing • Allow the eye to focus on close objects in the visual field Cranial Outflow Facial Nerves VII – The parasympathetic fibers of the facial nerves stimulate the secretory activity of many large glands of the head • The pathway activates the nasal glands and the lacrimal glands of the eyes • The preganglionic fibers then run to synapse with ganglionic neurons in the pterygopalatine ganglia stimulating the submandibular and sublingual salivary glands Cranial Outflow Glossopharyngeal (IX) – The parasympathetic nerves originate in the medulla and activate the parotid salivary gland Cranial Outflow Vagus nerves (X) – The major portion of the parasympathetic cranial outflow is via the vagus nerves – The two vagus nerves account for an estimated 90% of all preganglionic parasympathetic fibers in the body – They provide fibers to the neck and contribute to nerve plexuses that serve virtually every organ in the thoracic and abdominal cavity Cranial Outflow The vagus nerve fibers arise from the dorsal motor of the medulla and terminate by synapsing in terminal ganglia that are usually located in the walls of the target organ Cranial Outflow Most of the terminal ganglia are not individually named; instead they are collectively called intramural ganglia, literally ganglia “within the walls” As the vagus nerves passes into the thorax, they send branches to autonomic plexuses – Cardiac plexuses – Pulmonary plexuses – Esophageal plexuses Cranial Outflow When the vagus nerves reach the esophagus, their fibers intermingle to form the anterior and posterior vagal trunks Each trunk carries fibers from both vargus nerves Cranial Outflow The vagal trunks ride the esophagus down to enter the abdominal cavity They send fibers to form the aortic plexuses (formed by the celiac, superior mesenteric and hypogastric) Cranial Outflow Abdominal organs which receive vagal innervation include the liver, gallbladder, stomach, small intestine, kidneys, pancreas, and the proximal half of the large intestine The rest of the cavity are innervated by the sacral outflow Sacral Outflow The sacral outflow arises from neurons located in the lateral horn of the spinal cord at S2 - S4 The axons of these neurons run in the ventral roots of the spinal nerves to the ventral rami Sacral Outflow From the ventral rami the neurons branch to form the pelvic splanchnic nerves Most neurons synapse in the intramural ganglia located in the walls of the distal large intestine, urinary bladder and reproductive organs Sympathetic Division The sympathetic division innervates more organs It supplies not only the visceral organs in the internal body cavities, but also the visceral structures in the superficial part of the body – Sweat glands – Arrector pili – Arteries and veins Sympathetic Division All preganglionic fibers in the sympathetic division arise from cell bodies of preganglionic neurons located in spinal cord segments from T1 through L2 It is also called the thoracolumbar Sympathetic Division After leaving the cord via the ventral root, the preganglionic sympathetic fibers pass through a white ramus communicans to enter the adjoining chain (paravertebral) ganglion forming part of the sympathetic trunk or chain Sympathetic Division The sympathetic trunks flank each side of the vertebral column and appear as strands of white beads Sympathetic Division Although the sympathetic trunks extend from the neck to the pelvis, sympathetic fibers arise only from the thoracic and lumbar spinal cord segments Sympathetic Division The ganglia vary in size, position, and number, but there are typically 23 ganglia in each sympathetic chain… – – – – – 3 cervical 11 thoracic 4 lumbar 4 sacral 1 coccygeal Sympathetic Division Once a preganglionic axon reaches a paravertebral ganglion one of three things can happen to it Sympathetic Division Once a preganglionic axon reaches a paravertebral ganglion one of three things can happen to it… 1. It can synapse with a ganglionic neuron within the same chain ganglion Sympathetic Division Once a preganglionic axon reaches a paravertebral ganglion one of three things can happen to it… 2. It can ascend or descend the sympathetic chain to synapse in another chain ganglion Sympathetic Division Once a preganglionic axon reaches a paravertebral ganglion one of three things can happen to it… 3. It can pass through the chain ganglion and emerge from the sympathetic chain without synapsing Sympathetic Division Preganglionic fibers which emerge from the sympathetic chain without synapsing help to form the splanchnic nerves which synapse with prevertebral or collateral ganglia Sympathetic Division The prevertebral ganglia are located anterior to the vertebral column Sympathetic Division Unlike the paravertebral ganglia the prevertebral ganglia . . . – Are neither paired nor segmentally arranged – They occur only in the abdomen and pelvis Sympathetic Division Note: Regardless of where the synapse occurs, all sympathetic ganglia lie close to the spinal cord The postganglionic fibers which run from the ganglion to the organs are typically much long than the preganglionic fibers Visceral Reflexes The visceral sensory neurons are the first link in the autonomic reflexes These neurons send information concerning chemical changes, stretch, and irritation of the viscera Visceral Reflexes Visceral reflex arcs have essentially the same components as somatic reflex arcs – – – – – Receptor Sensory neuron Integration center Motor neuron Effector Visceral Reflexes Visceral reflex arcs differ in that they have a two-neuron chain Visceral Reflexes Nearly all sympathetic and parasympathetic fibers are accompanied by afferent fibers conducting sensory impulses from glands or muscular structures Thus, peripheral processes of visceral sensory neurons are found in cranial nerves, VII, IX, and X, the splanchnic nerves, and the sympathetic trunk, as well as the spinal nerves Visceral Reflexes Like sensory neurons serving somatic structures (skeletal muscles and skin) The cell bodies of visceral sensory neurons are located in the sensory ganglia of associated cranial nerves or in the dorsal root ganglia of the spinal cord Visceral Reflexes Visceral sensory reflexes are also found within sympathetic ganglia where synapses with preganglionic neurons occur Complete three-neuron reflex arcs (sensory, motor, and intrinsic neurons) exist within the walls of the gastrointestinal tract – Enteric nervous system – Controls gastrointestinal activity Visceral Reflexes The fact that visceral pain travels along the same pathways as somatic pain fibers helps to explain the phenomenon of referred pain in which pain stimuli arising in the viscera is perceived as somatic in origin Visceral Reflexes A heart attach may produce a sensation of pain that radiates to the superior thoracic wall and along the medial aspect of the left arm Visceral Reflexes Since the same spinal segments (T1T5) innervate both the heart and the regions to which pain signals from heart tissue are referred, the brain interprets most such inputs as coming from the somatic pathway Visceral Reflexes Additional cutaneous areas to which visceral pain is referred Chapter 14 This concludes the material for which you will be responsible