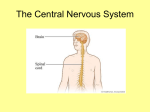
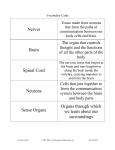
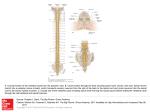
* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download molecular mechanisms of axonal regeneration in the central
Single-unit recording wikipedia , lookup
Subventricular zone wikipedia , lookup
Eyeblink conditioning wikipedia , lookup
Molecular neuroscience wikipedia , lookup
Multielectrode array wikipedia , lookup
Clinical neurochemistry wikipedia , lookup
Premovement neuronal activity wikipedia , lookup
Nervous system network models wikipedia , lookup
Stimulus (physiology) wikipedia , lookup
Node of Ranvier wikipedia , lookup
Central pattern generator wikipedia , lookup
Circumventricular organs wikipedia , lookup
Neural engineering wikipedia , lookup
Feature detection (nervous system) wikipedia , lookup
Synaptic gating wikipedia , lookup
Neuropsychopharmacology wikipedia , lookup
Optogenetics wikipedia , lookup
Development of the nervous system wikipedia , lookup
Synaptogenesis wikipedia , lookup
Channelrhodopsin wikipedia , lookup
Neuroanatomy wikipedia , lookup
Spinal cord wikipedia , lookup
PROCEEDINGS MOLECULAR MECHANISMS OF AXONAL REGENERATION IN THE CENTRAL NERVOUS SYSTEM* — Marion Murray, PhD† ABSTRACT The regeneration of injured axons in the adult central nervous system (CNS) is limited by a number of obstacles, including the loss of growth factors that promote neuron survival, expression of nerve growth inhibitors, activation of programmed cell death pathways, and physical obstruction caused by scar formation at the site of injury. Evidence from several animal models of CNS injury suggests it is possible to improve neuronal survival and support axon regeneration. Direct application of nerve growth factors to the site of injury, either by gelfoam, osmotic pump, or transplantation of genetically modified cells, has been shown to increase the number of neurons that survive axotomy and that can regenerate axons into or through the lesion site. Inhibitors of growth-suppressing or cell death pathways also enhance neuron survival. Combination treatments may be required to produce clinically meaningful improvements in patients with severe CNS injury. (Adv Stud Med. 2004;4(4B):S335-S338) lthough neurons of the adult central nervous system (CNS) are known for their inability to repair themselves following injury, it has long been recognized that these cells possess limited regenerative capacity.1 Three distinct types of axonal sprouting have been described as a result of axonal injury in the CNS. Axon transection is followed by a very short and abortive period of regenerative sprouting, A *Based on a presentation given by Dr Murray at an educational symposium held in New York City, December 2003. †Professor of Neurobiology and Anatomy, Drexel University College of Medicine, Philadelphia, Pennsylvania. Address correspondence to: Marion Murray, PhD, Drexel University College of Medicine, 3200 Henry Ave, Philadelphia, PA 19129. E-mail: [email protected]. Advanced Studies in Medicine ■ during which the severed axons extend briefly then retract. Compensatory sprouting occurs when the transected axon also emits collateral sprouts to targets proximal to the injury. Collateral sprouting is the growth by undamaged neurons. When an axon is transected, neighboring undamaged axons can extend sprouts to occupy the synaptic space formerly occupied by the transected axon. These observations suggest neurons can initiate regenerative growth following CNS injury but that obstacles prevent significant elongation. Adult neurons may fail to express growth-promoting genes that are normally active during CNS development. Axonal injury triggers programmed cell death (apoptosis) pathways that result in neuronal death. The formation of a cyst or scar at the injury site may act as a physical barrier preventing axon regrowth, and scar-forming cells may also secrete substances that suppress axon regeneration. Other targetderived chemical mediators that normally support neuronal survival may become unavailable to the neuron after axonal transection. Inflammation at the site of injury may cause the release of other chemical mediators that suppress axon growth. Although there are many obstacles to neuronal survival or regeneration following CNS injury, solutions have been devised to overcome many of them. Considerable experimental evidence suggests nerve growth factors can be delivered to injured neurons either by direct injection or transplantation of cells that secrete them. These growth factors improve neuronal survival and promote axonal regeneration. Within the lesion, the formation of a cyst or scar can be prevented by enzymatic digestion, and a “bridge” for regenerating axons can be formed using transplanted cells. Anti-inflammatory agents can be used to suppress activation of the immune system. RESCUING AXOTOMIZED NEURONS One model system that is particularly well suited for studies of neurodegeneration and regeneration is the S335 PROCEEDINGS transection of axons that originate from neurons in Clarke’s nucleus of the spinal cord. Clarke’s nucleus is anatomically well defined and projects entirely ipsilaterally to targets within the spinal cord and the cerebellum.2 Injury of the spinal cord along this pathway results in the axotomy of all of the axons that project from Clarke’s nucleus on that side of the spinal cord. After several weeks, extensive cell death is observed in the Clarke’s nucleus on the hemisected side, whereas on the contralateral side, the nucleus remains intact. Calculating the ratio of neurons remaining on the axotomized side to the number on the intact side provides an index of neurodegeneration that can be used to test various strategies to improve neuron survival following axotomy. This model was used to demonstrate that transplanting tissue grafts of fetal neural tissue into the lesion site protected many of the Clarke’s nucleus axons from death.2 In hemisected animals that did not receive fetal tissue grafts, the number of cells surviving in Clarke’s nucleus decreased by 30% over a 2-month period compared with control animals. Transplantation with tissue grafts obtained from fetal spinal cord, cerebellum, or neocortex within the first few days after axotomy resulted in nearly complete rescue of Clarke’s nucleus neurons. Embryonic striatal tissue transplants, in contrast, did not improve survival of the axotomized neurons (Figure 1). Animals treated with the growth factor neurotrophin-3 (NT-3) into the site of spinal hemisection exhibited significant improvement in survival of Clarke’s nucleus neurons compared with untreated animals, whereas administration of several other growth factors (ie, nerve growth factor, brain-derived neurotrophic factor, ciliary neurotrophic factor) did not improve survival.3 In a subsequent study in which animals received grafts of fibroblasts that were genetically modified to secrete growth factors, fibroblasts that secreted NT-3 appeared to completely protect Clarke’s nucleus neurons from death, and nerve growth factor provided partial protection.4 It has also been shown that transfer of the human BCL-2 gene (which is believed to prevent apoptotic cell death) to cells in the spinal cord above and below the lesion site significantly improved the survival of neurons in Clarke’s nucleus following spinal hemisection.5 Similar outcomes were observed in studies that examined the effects of transection on neurons of the rubrospinal tract. In this case, axons from cell bodies that originate in the red nucleus of the brainstem project almost entirely to the contralateral spinal cord. Using this model system, fibroblasts that were genetically mod- S336 ified to secrete brain-derived neurotrophic factor (BDNF)—a growth factor that is of particular importance for the survival or rubrospinal neurons—were transplanted into the site of hemisection. In the red nucleus contralateral to the spinal cord hemisection, about 65% of cells survived in untreated animals, whereas approximately 90% of neurons survived in animals that received the genetically modified fibroblasts. In a second study, administration of apoptosis-inhibiting BCL-2 rescued many (but not all) of the axotomized neurons in the rubrospinal tract.6 These studies confirm that cell death in axotomized neurons can be prevented if the cells are provided appropriate neurotrophic factors. AXON REGENERATION As described previously, transected axons often exhibit a brief transitory period of spontaneous regeneration. Two general approaches have been used to increase axonal regeneration following CNS injury: Figure 1. Survival of Axotomized Neurons in Clarke’s Nucleus *Significantly fewer neurons vs other groups. Cell survival at the L1 level of Clarke’s nucleus of adult rats following hemisection of the ipsilateral spinal cord, expressed as the ratio of the number of cells on the operated side to the number on the control side. Cell survival was significantly reduced (indicated by asterisks) in animals that underwent spinal hemisection alone or spinal hemisection followed by a graft of fetal striatal tissue. Grafts of tissue from fetal spinal cord, cerebellum, or cortex prevented the loss of cells in the hemisected Clarke’s nucleus. HX = hemisection only; HX-SC = hemisection with spinal cord transplant; HX-CB = hemisection with cerebellum transplant; HX-CTX = hemisection with neocortex transplant; HX-STR = hemisection with striatum transplant. Adapted with permission from John Wiley & Sons, Inc. Himes et al. Grafts of fetal central nervous system tissue rescue axotomized Clarke’s nucleus neurons in adult and neonatal operates. J Comp Neurol. 1994;339(1): 117-131.2 Copyright © 2000, Wiley-Liss, Inc, A Wiley Company. Vol. 4 (4B) ■ April 2004 PROCEEDINGS providing the regenerating cells with growth factors or other substances that stimulate growth or preventing the development of injury processes that suppress growth. Both approaches have been shown to improve axon regeneration in animal injury models. The use of genetically modified cells (eg, fibroblasts) that secrete neurotrophic factors is of particular interest in studies that examine axon regeneration. The growth factors may stimulate axonal sprouting and regrowth while the fibroblasts form a physical bridge for the growing axons. Axonal regeneration following the transplantation of genetically modified fibroblasts has been studied in the rubrospinal tract model system. Fibroblasts modified to secrete BDNF were transplanted into the lesion site, and axonal regeneration was assessed using 2 methods.7 The regenerating axons were examined using an anterograde staining procedure in which a dye (biotinylated dextran amine, or BDA) was injected into the red nucleus. BDA is taken up by the cell bodies and transported down the length of the axons. Retrograde staining was performed by injecting a different dye (fluorogold) into the spinal cord below the level of the injury. Fluorogold is taken up by axons that extend into the dye-injected region and transported back along the axon to the cell bodies of neurons whose axons have regenerated beyond the lesion. In transplanted animals, BDA-labeled axons were observed extending through the grafted fibroblasts and into the caudal portion of the spinal cord. Some of these axons could be seen leaving the spinal cord white matter and projecting into gray matter. Although it could not be determined whether these axons established functional synapses, they did project to the appropriate spinal laminae for rubrospinal neurons. With the retrograde tracing technique, no red nucleus neurons were stained in animals that underwent transection without receiving the modified fibroblasts. In treated animals, the number of stained neurons was about 7% to 10% of the number observed in normal animals that did not undergo spinal hemisection. Although this is a relatively small fraction of the total number of red nucleus axons projecting to the normal spinal cord, even a few axons forming synapses in the spinal cord could produce clinically significant improvement in patients with severe spinal cord damage. the injured spinal cord. These findings suggest it may be possible to significantly improve recovery following some types of CNS injury. However, they also illustrate that providing growth-promoting molecules may not be sufficient to produce extensive axonal regrowth. A significant obstacle to axon regeneration is the development of a scar at the site of injury. Scarring within the CNS creates a physical barrier to axon regrowth and is associated with the release of many chemical mediators that interfere with axonal regeneration. Several inhibitory molecules have been identified in CNS lesions, and strategies to suppress the growth-inhibiting effects of these mediators are in development. Myelin-associated inhibitors may be the principal impediment to axon regeneration immediately after injury.8 Recent research suggests that there are at least 3 of these inhibitors, all of which appear to bind to a common neuronal receptor. These include Nogo, a protein found on the cell surface of oligodendrocytes and on the myelin membrane; myelin-associated glycoprotein; and the recently identified oligodendrocyte myelin glycoprotein, which is expressed by oligodendrocytes and neurons in the CNS and in the peripheral nervous system. All of these ligands activate a common receptor (the Nogo receptor, or Ngr), and recent studies suggest that infusion of a peptide antagonist to this receptor into the site of CNS injury improves axon regeneration following transection.9 Semaphorins are a group of molecules that are important in the developing nervous system, where they provide inhibitory guidance by causing growth cone collapse and thus prevent inappropriate growth. In the adult they may act to prevent regenerative growth. Development and administration of new broad-spectrum protein kinase inhibitors can block these effects (G. Gallo, oral communication). Several inhibitory molecules have also been identified that are related to the scar that forms after CNS injury. These include chondroitin sulfate proteoglycans (CSPGs) and semaphorins. Chondroitinase ABC, an enzyme that cleaves CSPG and dissolves the scar, improved histologic and functional measures of axonal regeneration after cervical dorsal column crush injury (Figure 2).10 SUMMARY AND CONCLUSIONS THE HOSTILE ENVIRONMENT Providing injured axons with appropriate growth factors supports neuronal survival and allows some axons to regenerate for relatively long distances within Advanced Studies in Medicine ■ Several techniques have been developed to improve neuronal survival and enhance axonal regeneration after CNS injury. Similar techniques may be applicable in MS; it has recently been noted that embryonic S337 PROCEEDINGS Figure 2. ChAB Promotes Regeneration of Corticospinal Tract Neurons spinal cord injury is that the distal portion of the spinal cord often remains largely intact despite its physical separation from the more rostral regions of the CNS. It may therefore be possible to develop neurologic prostheses that can exploit the surviving circuitry and supplement repair processes. REFERENCES ChAB promoted regeneration of corticospinal tract neurons following crush injury in adult rats. Corticospinal tract neurons were counted in white matter tracts extending 4 mm rostral and caudal to the site of injury. Compared with sham-injury animals, crush injury resulted in the significant loss of axons in the spinal cord rostral to and projecting through the lesion in vehicle-treated animals. Treatment with ChAB significantly increased the number of axons projecting to and through the lesion site. *P <.05 between vehicle and ChAB treatment groups. ChAB = chondroitinase ABC. Adapted with permission from Bradbury et al. Chondroitinase ABC promotes functional recovery after spinal cord injury. Nature. 2002;416(6881):636-640.10 stem cells implanted into injured spinal cord are capable of differentiating into oligodendrocytes and thus of myelinating axons.11 Many techniques have produced at least some degree of success in improving neuronal survival and function after CNS injury. Benefits observed to date, however, have been relatively limited. Due to the large number of molecular mediators of axonal growth and the many different targets for these mediators, it will probably be necessary to develop combination therapies to substantially improve functional outcomes. This may add regulatory obstacles to the already difficult scientific problems that must be overcome to develop new therapies for clinical use. Developing interventions for chronic spinal cord injury is further complicated because many of the cells that survive injury may exhibit markedly reduced activity and may never regenerate. Established chronic lesions also have extensive permanent scarring, making it difficult for axons to grow. However, it has been shown that implanting fibroblasts engineered to secrete neurotrophic factors can improve neuronal survival even when implantation is delayed for several weeks after spinal cord hemisection.12 A significant feature of S338 1. Murray M, Tobias CA. Regeneration and sprouting in the injured spinal cord. Topics in Spinal Cord Injury Rehabilitation. 2003;8(4):37-51. 2. Himes BT, Goldberger ME, Tessler A. Grafts of fetal central nervous system tissue rescue axotomized Clarke’s nucleus neurons in adult and neonatal operates. J Comp Neurol. 1994;339(1):117-131. 3. Shibayama M, Hattori S, Himes BT, Murray M, Tessler A. Neurotrophin-3 prevents death of axotomized Clarke’s nucleus neurons in adult rat. J Comp Neurol. 1998; 390(1):102-111. 4. Himes BT, Liu Y, Solowska JM, Snyder EY, Fischer I, Tessler A. Transplants of cells genetically modified to express neurotrophin-3 rescue axotomized Clarke’s nucleus neurons after spinal cord hemisection in adult rats. J Neurosci Res. 2001;65(6):549-564. 5. Takahashi K, Schwarz E, Ljubetic C, Murray M, Tessler A, Saavedra RA. DNA plasmid that codes for human Bcl-2 gene preserves axotomized Clarke’s nucleus and reduces atrophy after spinal cord hemisection in adult rats. J Comp Neurol. 1999;404(2):159-171. 6. Shibata M, Murray M, Tessler A, Ljubetic C, Connors T, Saavedra RA. Single injections of a DNA plasmid that contains the human Bcl-2 gene prevent loss and atrophy of distinct neuronal populations after spinal cord injury in adult rats. Neurorehabil Neural Repair. 2000;14(4):319-330. 7. Liu Y, Kim D, Himes BT, et al. Transplants of fibroblasts genetically modified to express BDNF promote regeneration of adult rat rubrospinal axons and recovery of forelimb function. J Neurosci. 1999;19(11):4370-4387. 8. Filbin MT. Myelin-associated inhibitors of axonal regeneration in the adult mammalian CNS. Nat Rev Neurosci. 2003;4(9): 703-713. Erratum in: Nat Rev Neurosci. 2003;4(12):1019. 9. GrandPre T, Li S, Strittmatter SM. Nogo-66 receptor antagonist peptide promotes axonal regeneration. Nature. 2002;417(6888):547-551. 10. Bradbury EJ, Moon LD, Popat RJ, et al. Chondroitinase ABC promotes functional recovery after spinal cord injury. Nature. 2002;416(6881):636-640. 11. McDonald JW, Howard MJ. Repairing the damaged spinal cord: a summary of our early success with embryonic stem cell transplantation and remyelination. Prog Brain Res. 2002;137:299-309. 12. Tobias CA, Shumsky JS, Shibata M, Tuszynski MH, Fischer I, Tessler A et al. Delayed grafting of BDNF and NT-3 producing fibroblasts into the injured spinal cord stimulates sprouting, partially, rescues axotomized red nucleus neurons from loss and atrophy, and provides limited regeneration. Exp Neurol. 2003;184:97-113. Vol. 4 (4B) ■ April 2004