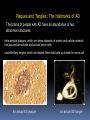
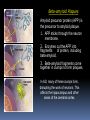
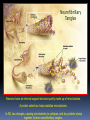
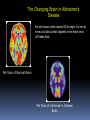
* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download AD Research: the Search for Causes
Blood–brain barrier wikipedia , lookup
Neuroinformatics wikipedia , lookup
Activity-dependent plasticity wikipedia , lookup
Artificial general intelligence wikipedia , lookup
Neurolinguistics wikipedia , lookup
Selfish brain theory wikipedia , lookup
Limbic system wikipedia , lookup
Human brain wikipedia , lookup
Environmental enrichment wikipedia , lookup
Embodied cognitive science wikipedia , lookup
Neurophilosophy wikipedia , lookup
Brain morphometry wikipedia , lookup
Neurogenomics wikipedia , lookup
Brain Rules wikipedia , lookup
Haemodynamic response wikipedia , lookup
Neuroeconomics wikipedia , lookup
Mental image wikipedia , lookup
Abnormal psychology wikipedia , lookup
Causes of mental disorders wikipedia , lookup
Neuroanatomy wikipedia , lookup
Neuroplasticity wikipedia , lookup
History of neuroimaging wikipedia , lookup
Metastability in the brain wikipedia , lookup
Nutrition and cognition wikipedia , lookup
Holonomic brain theory wikipedia , lookup
Neuropsychology wikipedia , lookup
Cognitive neuroscience wikipedia , lookup
Neuropsychopharmacology wikipedia , lookup
Alzheimer's disease wikipedia , lookup
Impact of health on intelligence wikipedia , lookup
Clinical neurochemistry wikipedia , lookup
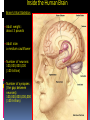
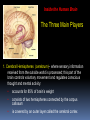
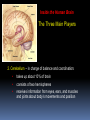
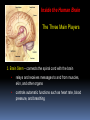
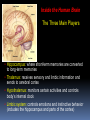
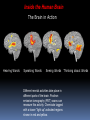
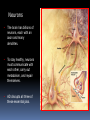
GERIATRIC NEUROLOGICAL CHANGES Hillcrest EMS March, 2013 OBJECTIVES Discuss normal/abnormal changes with aging of the nervous system. Discuss various nervous system diseases that are associated with aging. Review various symptoms related to the nervous system. Review types medications in use for these problems. GERIATRIC FACTS Per 2010 – 40 million >65 USA (13%) By 2030 - 72 million (20%) By 2050 – 87 million (17%) In 1990 – Very Old >85 = 100,000 In 2010 – 5.5 million Married -72% of men vs. 42% of women (majority are widows) Women outnumber men at 23 million to 17 million men. About 30% (11.3 million) of non-institutionalized older persons live alone 8.3 million women, 3.0 million men. Half of older women (49%) age 75+ live alone. GERIATRIC FACTS Healthcare: In 2010, 95.5% non-institutionalized persons 65+ were covered by Medicare. 5% of the non-institutionalized elderly were covered by Medicaid. For Medicare beneficiaries residing in nursing homes, over half (62%) were covered by Medicaid. Normal Changes with Age Not everyone has these changes to the same degree, and the resulting affects may be very different. PHYSICAL Declining endurance Increased health concerns Vision changes Hearing loss MENTAL Slowed learning speed Memory loss SOCIAL/EMOTIONAL Retirement Personal loss Loneliness New roles FINANCIAL Limited income Higher health care cost, cost of living Lifestyle change Normal Changes with Age Physiological aging changes in the Brain: Brain and spinal cord lose nerve cells and weight. Transmission of messages (synapses) slows down. Waste products from nerve cell breakdown may accumulate in the brain creating plaque and tangles to be formed. A fatty brown pigment (lipofuscin) can also build up in nerve tissue. Geriatric Mental Health -Anxiety Generalized anxiety disorder is characterized by persistent worry about major or minor concerns. Others — such as panic disorder, obsessive- compulsive disorder (OCD) and post-traumatic stress disorder (PTSD) — have more-specific triggers and symptoms. Anxiety is the most prevalent mental health problem for people over 50. Geriatric Mental Health - Anxiety Anxiety may happen as a normal part of life. It can be useful when it alerts you to danger. For some - anxiety persistently interferes with daily activities such as work, school, sleep relationships, and enjoyment of life. Medications to treat anxiety are very successful along with an understanding of what anxiety is. Geriatric Mental Health - MCI Mild Cognitive Impairment is an intermediate stage between the expected cognitive decline of normal aging and the more serious decline of dementia. MCI can involve problems with memory, language, thinking and judgment that are greater than normal age-related changes. A person with MCI may be aware that their memory or mental function has "slipped.“ Family and close friends also may notice a change. Mild Cognitive Impairment (MCI) Mild cognitive impairment may increase the risk of later progressing to dementia, caused by Alzheimer's disease or other neurological conditions. In general, cognitive function is preserved and activities of daily living, social relationships, and occupational responsibilities are not affected. Some people with mild cognitive impairment never get worse, and a few eventually get better. Treatment usually optional. Geriatric Mental Health - Depression IS NOT A NORMAL PART OF AGING estimated 6% > 65 (over 2.4 million) An illness that affects mind & body Can be dangerous Is not a sign of weakness Is often overlooked Can’t just snap out of it – need treated – one of the most successfully treated Geriatric Mental Health -Depression Common signs Deep sadness Hopelessness Loss of interest in old activities Significant + or – weight Inability to sleep Loss of energy Inability to concentrate Thoughts of death Geriatric Mental Health -Depression NEGATIVE FEELINGS Feel empty Sense of hopelessness Lack of feelings Loss of sexual desire Feel worthless Feel guilty Thoughts of death or suicide CHANGES IN BEHAVIOR, THINKING & ATTITUDE Trouble concentrating Irritability Poor memory Not care about appearance Withdrawing from family & friend PHYSICAL COMPLAINTS Unexplained aches/pains Sleep problems Fatigue Geriatric Mental Health -Depression Major depression – can be mild, moderate or severe; be triggered by a loss, crisis or change; make it hard to function day to day; continue for months or years if not treated Dysthymia –mild form, can last for years, may not remember what it feel like to be happy, can function day to day, but work and relationships suffer Bipolar disorder – periods of depression followed by periods of mania (unusually high energy, insomnia, overconfidence, racing thoughts, impulsive and reckless behavior (Manic depression) Seasonal Affective Disorder (SAD) – depression occurring in fall or winter – caused by seasonal change Geriatric Mental Health -Depression Once identified and treated, 80% return to their normal lives Common treatments include: Psychotherapy – for mild depression – Treat 10-20 weeks Antidepressant meds – work on the balance of neurotransmitter chemicals in the brain Treat ~ 6 months ECT (electroconvulsive therapy)– for life threatening depression not responsive to meds Depression & Suicide Rate is 50% higher than for any other age group For those >85 - highest of all Men >65 have a 7x higher rate than women Women’s rate goes up after 75 Most have seen PMD 20% (one day) – 40% (1 week) More than 30 percent of victims diagnosed & suffering from major depression. 6-9% living in primary setting report suicidal ideation Geriatric Mental Health - Dementia Dementia is not a specific disease. It's an overall term that describes a group of symptoms caused by various diseases or conditions. Dementia is a general term for a decline in mental ability severe enough to interfere with daily life. Alzheimer's is the most common type of dementia. Geriatric Mental Health - Dementia Forgetfulness Confusion Withdrawl Can progress over years or within weeks – depending on cause Irreversible conditions Alzheimers Stroke Rare viruses Parkinson’s Aids Reversible conditions Thyroid Alcohol Poor nutrition Mental problems Reactions to meds Geriatric Mental Health - Dementia Can be difficult to determine as neurologic symptoms may be the result of multiple causes. Use VITAMINS C & D mnemonic to help recall potential causes Vitamins C & D Vascular Inflammation Toxins, trauma, tumors Autoimmune Metabolic Infection Narcotics Systemic • Congenital • Degenerative Geriatric Mental Health - Dementia Symptoms can vary greatly. At least two of the following core mental functions must be significantly impaired to be considered dementia: Memory Communication and language Ability to focus and pay attention Reasoning and judgment Visual perception Geriatric Mental Health - Dementia People with dementia may likely have problems with: Short-term memory Keeping track of a purse or wallet Paying bills Planning and preparing meals Remembering appointments Traveling out of the neighborhood. Dementia Criteria Other signs & symptoms: 1. Impairment of Long Term Memory 2. Impairment of Abstract Thinking Ability 3. Impairment of Judgment 4. Personality Change 5. Disruption of High Cortical Function Aphasia – Speech Ataxia – Motor Function Agnosia – Object Recognition Dementia – Delirium Syndrome Considered a syndrome since symptoms come from various underlying causes Symptoms: Sudden onset Usually temporary & reversible Oriented to person – not time or place Disorganized thought process – can’t keep attention, cooperation Speech can be loud and argumentative/ can’t More Symptoms of Delirium Syndrome Altered perceptions, visual illusions/hallucinations – misinterpret the environment Lucid/confusion alternating Most are restless, agitated/ combative Emergency situation requiring attention now. Causes of Delirium Syndrome Systemic: Exacerbation of chronic illness/new disease process Infections – respiratory/UTI Drug toxicity/interactions Elimination problems Mechanical: – CVA, cardiac dysfunction, ca, brain tumor Psychosocial/environmental: Losses – loved one, possessions Sensory deprivation/overstimulation Treatments – based on symptoms. Geriatric Mental Health - Alzheimers The most common (50-60%) form of dementia among older people. About 5 .4 million Americans suffer from this condition. Is it genetic? Maybe - research has turned up evidence of a link between Alzheimer's disease and a number of genes . There is no proof it is caused by aluminum, zinc, a virus, or toxic food. Studies on-going. Dementia - Alzheimer’s Disease (AD) AD Statistics…. • One in eight over 65 have AD. Estimated 4 percent are under age 65, 6 percent are 65 to 74,44 percent are 75 to 84, and 46 percent are 85or older. • Chance of getting it doubles every 5 years after 65. 6th leading cause of death, only one that can’t be prevented, cured of slowed By 2050, 13.2 million older Americans are expected to have AD if the current numbers hold and no preventive treatments become available. Dementia - Alzheimer’s Disease (AD) Where are people with AD cared for? • 80% family @home The national cost of caring for people with AD is about $200 billion every year. $140 billion by Medicare,Medicaid. (add’l $210 B. in donated care) • Assisted living facilities (those in the early stages) • Nursing homes (special care units) Alzheimers vs. Normal Aging Signs of Alzheimer's Typical age-related changes Poor judgment and Making a bad decision decision making Inability to manage a budget Losing track of the date or the season Difficulty having a conversation Misplacing things and being unable to retrace steps to find them once in a while Missing a monthly payment Forgetting which day it is and remembering later Sometimes forgetting which word to use Losing things from time to time 10 Warning Signs of Alzheimers 1. Memory loss that disrupts daily life. 2. Unable to do planning or complete project. 3. Difficulty completing familiar tasks at home, at work or at leisure. 4. Confusion with time or place. 5. Trouble understanding visual images and spatial relationships. 10 Warning Signs of Alzheimers 6. New problems with words in speaking or writing. 7. Misplacing things and losing the ability to retrace steps. 8. Decreased or poor judgment. 9. Withdrawal from work or social activities. 10.Changes in mood and personality Inside the Human Brain Brain’s Vital Statistics • Adult weight: about 3 pounds • Adult size: a medium cauliflower • Number of neurons: 100,000,000,000 (100 billion) • Number of synapses (the gap between neurons): 100,000,000,000,000 (100 trillion) Inside the Human Brain The Three Main Players 1. Cerebral Hemispheres (cerebrum)– where sensory information received from the outside world is processed; this part of the brain controls voluntary movement and regulates conscious thought and mental activity: • accounts for 85% of brain’s weight • consists of two hemispheres connected by the corpus callosum • is covered by an outer layer called the cerebral cortex Inside the Human Brain The Three Main Players 2. Cerebellum – in charge of balance and coordination: • takes up about 10% of brain • consists of two hemispheres • receives information from eyes, ears, and muscles and joints about body’s movements and position Inside the Human Brain The Three Main Players 3. Brain Stem – connects the spinal cord with the brain • relays and receives messages to and from muscles, skin, and other organs • controls automatic functions such as heart rate, blood pressure, and breathing Inside the Human Brain The Three Main Players • Hippocampus: where short-term memories are converted to long-term memories • Thalamus: receives sensory and limbic information and sends to cerebral cortex • Hypothalamus: monitors certain activities and controls body’s internal clock • Limbic system: controls emotions and instinctive behavior (includes the hippocampus and parts of the cortex) Inside the Human Brain The Brain in Action Hearing Words Speaking Words Seeing Words Different mental activities take place in different parts of the brain. Positron emission tomography (PET) scans can measure this activity. Chemicals tagged with a tracer “light up” activated regions shown in red and yellow. Thinking about Words Neurons • The brain has billions of neurons, each with an axon and many dendrites. • To stay healthy, neurons must communicate with each other, carry out metabolism, and repair themselves. • AD disrupts all three of these essential jobs. Plaques and Tangles: The Hallmarks of AD The brains of people with AD have an abundance of two abnormal structures: • beta-amyloid plaques, which are dense deposits of protein and cellular material that accumulate outside and around nerve cells • neurofibrillary tangles, which are twisted fibers that build up inside the nerve cell An actual AD plaque An actual AD tangle Beta-amyloid Plaques Amyloid precursor protein (APP) is the precursor to amyloid plaque. 1. APP sticks through the neuron membrane. 2. Enzymes cut the APP into fragments of protein, including beta-amyloid. 3. Beta-amyloid fragments come together in clumps to form plaques. In AD, many of these clumps form, disrupting the work of neurons. This affects the hippocampus and other areas of the cerebral cortex. Neurofibrillary Tangles Neurons have an internal support structure partly made up of microtubules. A protein called tau helps stabilize microtubules. In AD, tau changes, causing microtubules to collapse, and tau proteins clump together to form neurofibrillary tangles. The Changing Brain in Alzheimer’s Disease No one knows what causes AD to begin, but we do know a lot about what happens in the brain once AD takes hold. Pet Scan of Normal Brain Pet Scan of Alzheimer’s Disease Brain Preclinical AD • Signs of AD are first noticed in the entorhinal cortex, then proceed to the hippocampus. • Affected regions begin to shrink as nerve cells die. • Changes can begin 10-20 years before symptoms appear. • Memory loss is the first sign of AD. Mild to Moderate AD • AD spreads through the brain. The cerebral cortex begins to shrink as more and more neurons stop working and die. • Mild AD signs can include memory loss, confusion, trouble handling money, poor judgment, mood changes, and increased anxiety. • Moderate AD signs can include increased memory loss and confusion, problems recognizing people, difficulty with language and thoughts, restlessness, agitation, wandering, and repetitive statements. Severe AD • In severe AD, extreme shrinkage occurs in the brain. Patients are completely dependent on others for care. • Symptoms can include weight loss, seizures, skin infections, groaning, moaning, or grunting, increased sleeping, loss of bladder and bowel control, malnutrition. • Death usually occurs from aspiration pneumonia or other infections. Caregivers can turn to a hospice for help and palliative care. AD Research: the Search for Causes • AD develops when genetic, lifestyle, and environmental factors work together to cause the disease process to start. • In recent years, scientists have discovered genetic links to AD. • They are also investigating other factors that may play a role in causing AD AD Research: the Search for Causes Genetic Studies The two main types of AD are early-onset and late-onset: • Early-onset AD is rare, usually affecting people aged 30 to 60 • Late-onset AD is more common. It usually affects people over age 65. Researchers have identified a gene that produces a protein called apolipoprotein E (ApoE). Scientists believe this protein is involved in the formation of beta-amyloid plaques. • Researchers have identified mutations in nine genes that are implicated in AD. Studies at the Cellular and Molecular Level • Oxidative damage from free radical molecules can injure neurons. • Homocysteine, an amino acid, is a risk factor for heart disease. A study shows that an elevated level of homocysteine is associated with increased risk of AD. • Scientists are also looking at inflammation in certain regions of the brain and strokes as risk factors for Epidemiologic Studies Scientists examine characteristics, lifestyles, and disease rates of groups of people to gather clues about possible causes of AD. Two of the studies focus on religious communities. Yearly exams of physical and mental status, and studies of donated brains at autopsy. Some early results indicate: • Mentally stimulating activity protects the brain in some ways. • In early life, higher skills in grammar and density of ideas are associated with protection against AD in late life. AD Research: Diagnosing AD Physicians today use a number of tools to diagnose AD: • a detailed patient history • information from family and friends • physical and neurological exams and lab tests • neuropsychological tests • imaging tools such as CT scan, or magnetic resonance imaging (MRI). PET scans are used primarily for research purposes AD Research: NIA Study Neuroimaging and Biomarkers of AD Initiative, to study how the brain changes in Mild Cognitive Impairment (MCI) and AD. • Using MRIs and PET scans conducted at regular intervals, researchers hope to learn precisely when and where in the brain problems occur. • Researchers will also examine blood samples to check for higher levels of abnormal substances that could be considered “biomarkers” of AD. • Also studying CSF markers. • Looking for subtle changes that may indicate the changes of AD Alzheimer’s Treatments Current medications cannot cure Alzheimer’s or stop it from progressing, they may help lessen symptoms, such as memory loss and confusion, for a limited time. The FDA has approved two types of medications These drugs treat the cognitive symptoms (memory loss, confusion), and problems with thinking and reasoning to help lessen or stabilize symptoms for a limited time by affecting certain chemicals involved in carrying messages among the brain's nerve cells. Alzheimer’s Treatments Cholinesterase inhibitors (Aricept, Exelon, Razadyne, Cognex) Alzheimer’s Treatments NMDA /receptor blocker, (Namenda or memantine HCL) Alzheimer’s Treatments Non-drug approaches may be used for behavior and personality changes such as: Irritability ,Anxiety Depression Agitation & Aggression Emotional distress, physical or verbal outbursts Restlessness, pacing, shredding paper or tissues Hallucinations (seeing, hearing or feeling things that are not really there) Delusions (firmly held belief in things that are not true) Sleep disturbances Monitor their conditions, anticipate their needs. Drugs used: Antidepressants (for mood), Anxiolytics (for anxiety/restlessness), Antipsychotic medications (for hallucinations) Managing Symptoms 70 to 90% of people with AD eventually develop behavioral symptoms: sleeplessness, wandering and pacing, aggression, agitation, anger, depression, hallucinations and delusions. Experts suggest coping strategies for managing difficult behaviors: • Stay calm and be understanding. • Be patient and flexible. Don’t argue or try to convince. • Acknowledge requests and respond to them. • Try not to take behaviors personally. Remember: It’s the disease talking. Experts encourage caregivers to try non-medical coping strategies first. However, medical treatment is often available if the behavior has become too difficult to handle. Helpful Hints to Reduce Agitation Decrease environmental stimulation Break down tasks into simple steps Provide choices, try humor/not demanding Be prepared to repeat yourself Ask one question at a time/ simple answers Be non-confrontational – limit number of people communicating to ONE Basic Patient Management For any patient with altered mental status, airway and breathing support have priority. Supplemental oxygen at a minimum Consider need for positive pressure ventilations. Monitor ECG, pulse Ox, and blood sugar. Determine dementia diagnosis, establish baseline and be slow, and supportive. Basic Patient Management Medical problems Medications – polypharmacy is common, need to know ALL meds including herbal/ OTC Psychological state; find out what is normal from family members May need nothing more than your presence and attention while taking to hospital Take note of the environment (possible abuse) Resources GEMS Medscape Web MD Alzheimer’s Association Cleveland Clinic/ CCF EMS Mayo Clinic National Institute on Aging, part of the National Institutes of Health (NIH) CDC