* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download powerpoint lecture
Neuroregeneration wikipedia , lookup
Embodied language processing wikipedia , lookup
Neurotransmitter wikipedia , lookup
Feature detection (nervous system) wikipedia , lookup
Development of the nervous system wikipedia , lookup
Molecular neuroscience wikipedia , lookup
Neuropsychopharmacology wikipedia , lookup
Synaptic gating wikipedia , lookup
Caridoid escape reaction wikipedia , lookup
Nervous system network models wikipedia , lookup
Premovement neuronal activity wikipedia , lookup
Electromyography wikipedia , lookup
End-plate potential wikipedia , lookup
Central pattern generator wikipedia , lookup
Proprioception wikipedia , lookup
Neuroanatomy wikipedia , lookup
Circumventricular organs wikipedia , lookup
Stimulus (physiology) wikipedia , lookup
Neuromuscular junction wikipedia , lookup
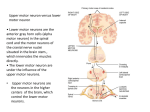
Anatomy & Physiology I Lecture 13 Chapter 13: The Reflex Arc Chapter 14: The Autonomic Nervous System Motor Integration (Review) • Skeletal Muscle – Takes place at neuromuscular junction – Neurotransmitter acetylcholine (ACh) released when nerve impulse reaches axon terminal • Smooth and Cardiac Muscle – Branches form synapses via varicosities – Acetylcholine and norepinephrine act indirectly via second messengers Figure 9.8 When a nerve impulse reaches a neuromuscular junction, acetylcholine (ACh) is released. Myelinated axon of motor neuron Action potential (AP) Axon terminal of neuromuscular junction Sarcolemma of the muscle fiber Synaptic vesicle containing ACh Axon terminal of motor neuron Synaptic cleft Fusing synaptic vesicles ACh Junctional folds of sarcolemma Sarcoplasm of muscle fiber Postsynaptic membrane ion channel opens; ions pass. ACh © 2013 Pearson Education, Inc. Acetylcholinesterase Degraded ACh Ion channel closes; ions cannot pass. Slide 1 Figure 9.26 Innervation of smooth muscle. Varicosities Autonomic nerve fibers innervate most smooth muscle fibers. Synaptic vesicles © 2013 Pearson Education, Inc. Smooth muscle cell Mitochondrion Varicosities release their neurotransmitters into a wide synaptic cleft (a diffuse junction). Levels of Motor Control • Cerebellum and basal nuclei are ultimate planners and coordinators of complex motor activities • Complex motor behavior depends on complex patterns of control – Segmental level – Projection level – Precommand level Segmental Level • Lowest level of motor hierarchy – Reflexes and automatic movements • Central pattern generators (CPGs) – circuits that activate networks of ventral horn neurons to stimulate specific groups of muscles – Controls locomotion and specific, repeated motor activity Projection Level • Direct control of the Spinal Cord • Consists of – Upper motor neurons initiate direct pathways to produce voluntary skeletal muscle movements – Brain stem motor areas oversee indirect pathways to control reflex and CPG-controlled motor actions • Projection motor pathways send information to lower motor neurons, and keep higher command levels informed of what is happening Precommand Level • Neurons in cerebellum and basal nuclei – Regulate motor activity – Precisely start or stop movements – Coordinate movements with posture – Block unwanted movements – Monitor muscle tone – Perform unconscious planning and discharge in advance of willed movements Figure 13.14a Hierarchy of motor control. Precommand Level (highest) • Cerebellum and basal nuclei • Programs and instructions (modified by feedback) Projection Level (middle) • Motor cortex (pyramidal pathways) and brain stem nuclei (vestibular, red, reticular formation, etc.) • Conveys instructions to spinal cord motor neurons and sends a copy of that information to higher levels Segmental Level (lowest) • Spinal cord • Contains central pattern generators (CPGs) Sensory input Reflex activity Motor output Levels of motor control and their interactions © 2013 Pearson Education, Inc. Precommand Level • Cerebellum – Acts on motor pathways through projection areas of brain stem – Acts on motor cortex via thalamus to fine-tune motor activity • Basal nuclei – Inhibit various motor centers under resting conditions Figure 13.14b Hierarchy of motor control. Precommand level • Cerebellum • Basal nuclei Projection level • Primary motor cortex • Brain stem nuclei Segmental level • Spinal cord © 2013 Pearson Education, Inc. Structures involved Reflexes • Inborn (intrinsic) reflex - rapid, involuntary, predictable motor response to stimulus – maintain posture, control visceral activities – Can be modified by learning and conscious effort • Learned (acquired) reflexes result from practice or repetition, – driving skills The Reflex Arc • The highly specific neural pathway that creates reflexes. • Receptors detect internal or external stimuli that elicit a rapid, stereotyped response – effectors are muscles or glands Components of a reflex arc 1. Receptor—site of stimulus action 2. Sensory neuron—transmits afferent impulses to CNS 3. Integration center—either monosynaptic or polysynaptic region within CNS 4. Motor neuron—conducts efferent impulses from integration center to effector organ 5. Effector—muscle fiber or gland cell that responds to efferent impulses by contracting or secreting Figure 13.15 The five basic components of all reflex arcs. Stimulus Skin 1 Receptor Interneuron 2 Sensory neuron 3 Integration center 4 Motor neuron 5 Effector Spinal cord (in cross scetion) © 2013 Pearson Education, Inc. Reflexes • Two Functional classifications • Somatic reflexes – Activate skeletal muscle • Autonomic (visceral) reflexes – Activate visceral effectors (smooth or cardiac muscle or glands) Spinal Reflexes • Somatic reflexes mediated by the spinal cord – No direct involvement of higher brain centers • brain does have overall control – Integration center in spinal cord – Effectors are skeletal muscle Stretch and Tendon Reflexes • For smooth coordination of skeletal muscle nervous system must receive proprioceptor input regarding – Length of muscle – Amount of tension in muscle Muscle Fibers • Specialized, non-contractile muscle fibers used for motor reflexes – Informs the brain on the status of the muscle • Intrafusal muscle fibers – noncontractile fibers receptive to the CNS/PNS – contraction on their ends • Extrafusal muscle fibers – Effector muscle fibers that contract in response to simulit Nerves and Nerve endings • Two types of afferent endings: • Anulospiral endings (primary sensory endings) – Stimulated by rate and degree of stretch • Flower spray endings (secondary sensory endings) – Respond to stretch Nerves and Nerve endings • Contractile end regions innervated by: • Gamma () efferent fibers – Innervate intrafusal muscle fibers – Maintain spindle sensitivity • Alpha () efferent fibers – Innervate extrafusal muscle fibers – Stimulate muscle contraction Figure 13.16 Anatomy of the muscle spindle and tendon organ. Flower spray endings (secondary sensory endings) Anulospiral endings (primary sensory endings) Muscle spindle Capsule (connective tissue) Tendon organ © 2013 Pearson Education, Inc. Efferent (motor) fiber to muscle spindle Efferent (motor) fiber to extrafusal muscle fibers Extrafusal muscle fiber Intrafusal muscle fibers Sensory fiber Tendon Muscle Spindle Excitement • Excited in two ways: • External stretch of muscle and muscle spindle • Internal stretch of muscle spindle – Activating motor neurons stimulates ends to contract, thereby stretching spindle • Stretch causes increased rate of impulses to spinal cord – Coactivation • – coactivation maintains tension and sensitivity of spindle during muscle contraction • Stimulating intrafusal fibers maintains the spindle’s tension and sensitivey during muscle contraction – brain continues to be notified of changes in the muscle length Figure 13.17a Operation of the muscle spindle. (1 of 2) How muscle stretch is detected Muscle spindle Intrafusal muscle fiber Sensory fiber Extrafusal muscle fiber Time © 2013 Pearson Education, Inc. Unstretched muscle. Action potentials (APs) are generated at a constant rate in the associated sensory fiber. Figure 13.17a Operation of the muscle spindle. (2 of 2) How muscle stretch is detected Time © 2013 Pearson Education, Inc. Stretched muscle. Stretching activates the muscle spindle, increasing the rate of APs. Figure 13.17b Operation of the muscle spindle. (1 of 2) The purpose of - coactivation Time © 2013 Pearson Education, Inc. If only motor neurons were activated. Only the extrafusal muscle fibers contract. The muscle spindle becomes slack and no APs are fired. It is unable to signal further length changes. Figure 13.17b Operation of the muscle spindle. (2 of 2) The purpose of coactivation Time © 2013 Pearson Education, Inc. But normally - coactivation occurs. Both extrafusal and intrafusal muscle fibers contract. Tension is maintained in the muscle spindle and it can still signal changes in length. The Stretch Reflex • The brain sets a muscle’s length – Stretch reflex makes sure muscle stays this length • Maintains muscle tone in large postural muscles, and adjusts it reflexively – Causes muscle contraction in response to increased muscle length (stretch) Stretch Reflex • How stretch reflex works – Stretch activates muscle spindle – Sensory neurons synapse directly with motor neurons in spinal cord – motor neurons cause stretched muscle to contract – Reciprocal inhibition also occurs – fibers synapse with interneurons that inhibit motor neurons of antagonistic muscles Figure 13.18 Stretch Reflex (1 of 2) Slide 2 The events by which muscle stretch is damped 1 When stretch activates muscle spindles, the associated sensory neurons (blue) transmit afferent impulses at higher frequency to the spinal cord. Sensory neuron Cell body of sensory neuron Initial stimulus (muscle stretch) + + – Spinal cord Muscle spindle Antagonist muscle © 2013 Pearson Education, Inc. Figure 13.18 Stretch Reflex (1 of 2) Slide 3 The events by which muscle stretch is damped Sensory neuron Initial stimulus (muscle stretch) 2 The sensory neurons synapse directly with alpha motor neurons (red), which excite extrafusal fibers of the stretched muscle. Sensory fibers also synapse with interneurons (green) that inhibit motor neurons (purple) controlling antagonistic muscles. Cell body of sensory neuron + + – Spinal cord Muscle spindle Antagonist muscle © 2013 Pearson Education, Inc. Figure 13.18 Stretch Reflex (1 of 2) Slide 4 The events by which muscle stretch is damped Sensory neuron Cell body of sensory neuron Initial stimulus (muscle stretch) + + – Spinal cord Muscle spindle Antagonist muscle 3a Efferent impulses of alpha motor neurons cause the stretched muscle to contract, whichresists or reverses the stretch. © 2013 Pearson Education, Inc. Figure 13.18 Stretch Reflex (2 of 2) Slide 7 The patellar (knee-jerk) reflex—an example of a stretch reflex + Quadriceps (extensors) 1 + Patella Muscle spindle Hamstrings (flexors) + Excitatory synapse – Inhibitory synapse © 2013 Pearson Education, Inc. Patellar ligament – Spinal cord (L2–L4) 1 Tapping the patellar ligament stretches the quadriceps and excites its muscle spindles. Figure 13.18 Stretch Reflex (2 of 2) Slide 8 The patellar (knee-jerk) reflex—an example of a stretch reflex 2 + Quadriceps (extensors) 1 + Patella Muscle spindle Hamstrings (flexors) + Excitatory synapse – Inhibitory synapse © 2013 Pearson Education, Inc. Patellar ligament – Spinal cord (L2–L4) 2 Afferent impulses (blue) travel to the spinal cord, where synapses occur with motor neurons and interneurons. Figure 13.18 Stretch Reflex (2 of 2) Slide 9 The patellar (knee-jerk) reflex—an example of a stretch reflex 2 Quadriceps (extensors) 1 + 3a + Patella Muscle spindle Hamstrings (flexors) – Spinal cord (L2–L4) Patellar ligament 3a The motor neurons (red) send activating impulses to the quadriceps causing it to contract, extending the knee. + Excitatory synapse – Inhibitory synapse © 2013 Pearson Education, Inc. Figure 13.18 Stretch Reflex (2 of 2) Slide 10 The patellar (knee-jerk) reflex—an example of a stretch reflex 2 Quadriceps (extensors) 1 3a + 3b Patella Muscle spindle Hamstrings (flexors) + Excitatory synapse – Inhibitory synapse © 2013 Pearson Education, Inc. + 3b – Spinal cord (L2–L4) Patellar ligament 3b The interneurons (green) make inhibitory synapses with ventral horn neurons (purple) that prevent the antagonist muscles (hamstrings) from resisting the contraction of the quadriceps. The Tendon Reflex • Opposite effect of stretch reflex – Muscles relax and lengthen in response to tension • Helps prevent damage due to excessive stretch • Important for smooth onset and termination of muscle contraction The Tendon Reflex • Produces muscle relaxation (lengthening) in response to tension • Contraction or passive stretch activates tendon reflex – Afferent impulses transmitted to spinal cord – Contracting muscle relaxes; antagonist contracts (reciprocal activation) – Information transmitted simultaneously to cerebellum and used to adjust muscle tension Figure 13.19 The tendon reflex. Slide 2 1 Quadriceps strongly contracts. Tendon organs are activated. Interneurons Quadriceps (extensors) Hamstrings (flexors) © 2013 Pearson Education, Inc. – + + Spinal cord Tendon organ + Excitatory synapse – Inhibitory synapse + Figure 13.19 The tendon reflex. Slide 3 2 Afferent fibers synapse with interneurons in the spinal cord. Interneurons Quadriceps (extensors) Hamstrings (flexors) © 2013 Pearson Education, Inc. – + + Spinal cord Tendon organ + Excitatory synapse – Inhibitory synapse + Figure 13.19 The tendon reflex. Slide 4 Interneurons + Quadriceps (extensors) – Hamstrings (flexors) © 2013 Pearson Education, Inc. + Spinal cord Tendon organ + Excitatory synapse – Inhibitory synapse + 3a Efferent impulses to muscle with stretched tendon are damped. Muscle relaxes, reducing tension. Figure 13.19 The tendon reflex. Slide 5 Interneurons Quadriceps (extensors) + – + + Spinal cord Tendon organ Hamstrings (flexors) 3b Efferent impulses to antagonist muscle cause it to contract. + Excitatory synapse – Inhibitory synapse © 2013 Pearson Education, Inc. The Flexor Reflexes • Flexor (withdrawal) reflex – Initiated by painful stimulus – Causes automatic withdrawal of threatened body part – Protective; important • Brain can override – finger stick for blood test Crossed-Extensor Reflex • Crossed extensor reflex – Occurs with flexor reflexes in weight-bearing limbs to maintain balance – step barefoot on broken glass • Stimulated side withdrawn (flexed) • Contralateral side extended Figure 13.20 The crossed-extensor reflex. + Excitatory synapse – Inhibitory synapse Interneurons + + – + Afferent fiber + – Efferent fibers Efferent fibers Extensor inhibited Flexor stimulated Site of stimulus: A noxious stimulus causes a flexor reflex on the same side, withdrawing that limb. © 2013 Pearson Education, Inc. Arm movements Flexor inhibited Extensor stimulated Site of reciprocal activation: At the same time, the extensor muscles on the opposite side are activated. Central nervous system (CNS) Peripheral nervous system (PNS) Sensory (afferent) division Motor (efferent) division Somatic nervous system Autonomic nervous system (ANS) Sympathetic division Parasympathetic division Figure 14.1 Place of the ANS in the structural organization of the nervous system. Central nervous system (CNS) Peripheral nervous system (PNS) Sensory (afferent) division © 2013 Pearson Education, Inc. Motor (efferent) division Somatic nervous system Autonomic nervous system (ANS) Sympathetic division Parasympathetic division The Autonomic Nervous System • ANS consists of motor neurons that – Innervate smooth and cardiac muscle, and glands – Make adjustments to ensure optimal support for body activities – Operate via subconscious control • Also called involuntary nervous system or general visceral motor system Somatic Versus Autonomic Nervous Systems • Both have motor fibers • Differ in – Effectors – Efferent pathways and ganglia – Target organ responses to neurotransmitters Effectors • Somatic nervous system – Skeletal muscles • ANS – Cardiac muscle – Smooth muscle – Glands ANS Neuron Chain ANS pathway uses two-neuron chain • Preganglionic neuron (in CNS) has a thin, lightly myelinated axon. • Postganglionic neuron (outside CNS) has nonmyelinated axon that extends to effector organ Neurotransmitters • Preganglionic fibers release Ach • Postganglionic fibers release norepinephrine or ACh at effectors – Effect is either stimulatory or inhibitory, depending on type of receptors Figure 14.2 Comparison of motor neurons in the somatic and autonomic nervous systems. Cell bodies in central nervous system Neurotransmitter at effector Peripheral nervous system Effector organs Effect SOMATIC NERVOUS SYSTEM Single neuron from CNS to effector organs + ACh Stimulatory Heavily myelinated axon Skeletal muscle Two-neuron chain from CNS to effector organs NE SYMPATHETIC Lightly myelinated preganglionic axons Nonmyelinated postganglionic axon Ganglion ACh Acetylcholine (ACh) Norepinephrine (NE) © 2013 Pearson Education, Inc. Ganglion Stimulatory or inhibitory, depending on neurotransmitter and receptors on effector organs Blood vessel ACh ACh Lightly myelinated preganglionic axon +– Epinephrine and norepinephrine Adrenal medulla PARASYMPATHETIC AUTONOMIC NERVOUS SYSTEM ACh Nonmyelinated postganglionic axon Smooth muscle (e.g., in gut), glands, cardiac muscle ANS vs PNS Motor Neurons • Conduction is slower in ANS than PNS neurons • Autonomic glanglia are motor ganglia • Somatic motor neurons lack ganglia – dorsal root ganglia are for sensory neurons The ANS/PNS Connection • Most spinal and many cranial nerves contain both somatic and autonomic fibers • Adaptations usually involve both skeletal muscles and visceral organs ANS Divisions • Sympathetic division • Parasympathetic division • Dual innervation – All visceral organs served by both divisions, but cause opposite effects – Dynamic antagonism between two divisions maintains homeostasis Parasympathetic Division: “Rest and Digest” • Promotes maintenance activities and conserves body energy – Directs digestion, diuresis, defecation • Think about relaxing and reading after a meal: – Blood pressure, heart rate, and respiratory rates are low – Gastrointestinal tract activity high – Pupils constricted; lenses accommodated for close vision Sympathetic Division: “fight or flight” • Mobilizes body during activity • Exercise, excitement, emergency, embarrassment – Increased heart rate; dry mouth; cold, sweaty skin – dilated pupils and bronchioles – cause liver to release glucose into blood Figure 14.3 The subdivisions of the ANS. Parasympathetic Eye Brain stem Salivary glands Heart Sympathetic Eye Skin* Cranial Sympathetic ganglia Salivary glands Cervical Lungs Lungs T1 Heart Stomach Thoracic Stomach Pancreas Pancreas Liver and gallbladder L1 Liver and gallbladder Adrenal gland Lumbar Bladder Genitals © 2013 Pearson Education, Inc. Bladder Sacral Genitals Parasympathetic (Craniosacral) Division • Long preganglionic fibers from brain stem and sacrum – Extend from CNS almost to target organs – Synapse with postganglionic neurons in terminal ganglia close to/within target organs • Short postganglionic fibers synapse with effectors Figure 14.4 Parasympathetic division of the ANS. Eye Ciliary ganglion CN III Lacrimal gland CN VII Pterygopalatine ganglion CN IX CN X Submandibular ganglion Otic ganglion Nasal mucosa Submandibular and sublingual glands Parotid gland Heart Cardiac and pulmonary plexuses Lung Celiac plexus Liver and gallbladder Stomach Pancreas S2 Large intestine S4 Small intestine Pelvic splanchnic nerves Inferior hypogastric plexus Rectum Urinary bladder and ureters Genitalia (penis, clitoris, and vagina) © 2013 Pearson Education, Inc. CN S Preganglionic Postganglionic Cranial nerve Sacral nerve Parasympathetic (Craniosacral) Division • Cranial Part – Consists of CN III, CN VII, and CN IX for smooth muscles of the eyes, nasal, lacrimal and parotid glands – Vagus Nerve (CN X) acdount for 90% of preganglionic fibers in body • Heart, Lungs, Liver, Stomach, Pancreas, Small Intestines and Early Large Intestines Parasympathetic (Craniosacral) Division • Sacral Part – Neurons cord segments S2-S4 – Genitals (Penis, Vagina, Clitoris) – Urinary bladder – Sigmoid Colon (Large Intestines) and Rectum Sympathetic (Thoracolumbar) Division • Preganglionic neurons are in spinal cord segments T1 – L2 • Preganglionic fibers pass through white rami communicantes and enter sympathetic trunk ganglia – Also called paravertebral since it runs alongside the vertebra Sympathetic Trunks and Pathways • Paravertebral ganglia vary in size, position, and number • There are 23 paravertebral ganglia in the sympathetic trunk (chain) – – – – – 3 cervical 11 thoracic 4 lumbar 4 sacral 1 coccygeal Figure 14.5a Sympathetic trunks and pathways. Spinal cord Dorsal root Ventral root Rib Sympathetic trunk ganglion Sympathetic trunk Ventral ramus of spinal nerve Gray ramus communicans White ramus communicans Thoracic splanchnic nerves © 2013 Pearson Education, Inc. Location of the sympathetic trunk Figure 14.6 Sympathetic division of the ANS. Eye Lacrimal gland Nasal mucosa Pons Sympathetic trunk (chain) ganglia Superior cervical ganglion Salivary glands Middle cervical ganglion Inferior cervical ganglion T1 Blood vessels; skin (arrector pili muscles and sweat glands) Heart Cardiac and pulmonary plexuses Greater splanchnic nerve Lesser splanchnic nerve Celiac ganglion L2 Lung Liver and gallbladder Stomach White rami communicantes Sacral splanchnic nerves Superior mesenteric ganglion Inferior mesenteric ganglion Spleen Adrenal medulla Kidney Lumbar splanchnic nerves Small intestine Large intestine Rectum Preganglionic Postganglionic © 2013 Pearson Education, Inc. Genitalia (uterus, vagina, and penis) and urinary bladder Serving the Head • Fibers emerge from T1 – T4 and synapse in the superior cervical ganglion • These fibers – Innervate skin and blood vessels of the head – Stimulate dilator muscles of the iris – Inhibit nasal and salivary glands – Innervate smooth muscle of upper eyelid – Branch to the heart (cardiac and pulmonary plexus) Collateral Ganglia • Most fibers from T5 – L2 synapse in collateral ganglia • They form thoracic, lumbar, and sacral splanchnic nerves • Their ganglia include the celiac and the superior and inferior mesenteric Ganglions • Celiac Ganglion – serves the liver, gallbladder, stomach and spleen adrenal gland • Superior mesenteric Ganglion – serves the small and large intestines • Inferior mesenteric Ganglion – serves the sigmoid colon and rectum • Sacral splanchnic nerve directly serves genitals, and bladder Visceral Reflexes • Visceral reflex arcs have same components as somatic reflex arcs – visceral reflex arc has two neurons in motor pathway Figure 14.7 Visceral reflexes. Stimulus 1 Receptor in viscera 2 Visceral sensory Dorsal root ganglion Spinal cord neuron 3 Integration center • May be preganglionic neuron (as shown) • May be a dorsal horn interneuron • May be within walls of gastrointestinal tract 4 Motor neuron (two-neuron chain) • Preganglionic neuron • Postganglionic neuron 5 Visceral effector © 2013 Pearson Education,Response Inc. Autonomic ganglion Neurotransmitters of ANS • Cholinergic fibers release neurotransmitter ACh – All ANS preganglionic axons – All parasympathetic postganglionic axons at effector synapse • Adrenergic fibers release neurotransmitter NE – Most sympathetic postganglionic axons Cholinergic Receptors • Two types of receptors bind ACh – Nicotinic – Muscarinic • Named after drugs that bind to them and mimic ACh effects – Nicotine – Muscarine (mushroom poison) Nicotinic Receptors • Found on – Sarcolemma of skeletal muscle cells (Chapter 9) at NMJ – All postganglionic neurons (sympathetic and parasympathetic) – Hormone-producing cells of adrenal medulla • Effect of ACh at nicotinic receptors is always stimulatory – Opens ion channels, depolarizing postsynaptic cell Muscarinic Receptors • Found on – All effector cells stimulated by postganglionic cholinergic fibers • Effect of ACh at muscarinic receptors – Can be either inhibitory or excitatory – Depends on receptor type of target organ Adrenergic Receptors • Two major classes – Alpha ( ) (subtypes 1, 2) – Beta ( ) (subtypes 1, 2 , 3) • Effects of NE depend on which subclass of receptor predominates on target organ – effects vary and can be adjusted depending on receptors present Control of ANS Function • Hypothalamus—main integrative center of ANS activity • Subconscious cerebral input via limbic system structures on hypothalamic centers • Other controls come from cerebral cortex, reticular formation, and spinal cord Hypothalamic Controls • Control may be direct or indirect (through reticular system) • Centers of hypothalamus control – Heart activity and blood pressure – Body temperature, water balance, and endocrine activity – Emotional stages (rage, pleasure) and biological drives (hunger, thirst, sex) – Reactions to fear and "fight-or-flight" system Figure 14.8 Levels of ANS control. Communication at subconscious level Cerebral cortex (frontal lobe) Limbic system (emotional input) Hypothalamus The “boss”: Overall integration of ANS Brain stem (reticular formation, etc.) Regulates pupil size, heart, blood pressure, airflow, salivation, etc. Spinal cord Reflexes for urination, defecation, erection, and ejaculation © 2013 Pearson Education, Inc. The End of the Nervous System • Lab Today – Continue working on lab exercises: – Lab Exercise 21 • Activity 1 – 3 only (Activity 3 Wednesdays' lecture) – Lab Exercise 22 • Introduction to the reflex arc (Wednesday) • Optional Activities 1 - 4