* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Molecular evidence for the existence of additional members of the
Zinc finger nuclease wikipedia , lookup
Koinophilia wikipedia , lookup
Whole genome sequencing wikipedia , lookup
United Kingdom National DNA Database wikipedia , lookup
Designer baby wikipedia , lookup
Nucleic acid analogue wikipedia , lookup
Epigenomics wikipedia , lookup
History of genetic engineering wikipedia , lookup
DNA sequencing wikipedia , lookup
DNA vaccination wikipedia , lookup
Molecular cloning wikipedia , lookup
Primary transcript wikipedia , lookup
Vectors in gene therapy wikipedia , lookup
Extrachromosomal DNA wikipedia , lookup
Genomic library wikipedia , lookup
Human genome wikipedia , lookup
Deoxyribozyme wikipedia , lookup
Therapeutic gene modulation wikipedia , lookup
No-SCAR (Scarless Cas9 Assisted Recombineering) Genome Editing wikipedia , lookup
Cre-Lox recombination wikipedia , lookup
Microevolution wikipedia , lookup
Cell-free fetal DNA wikipedia , lookup
Multiple sequence alignment wikipedia , lookup
Non-coding DNA wikipedia , lookup
Point mutation wikipedia , lookup
Site-specific recombinase technology wikipedia , lookup
Genome editing wikipedia , lookup
Sequence alignment wikipedia , lookup
Computational phylogenetics wikipedia , lookup
DNA barcoding wikipedia , lookup
Helitron (biology) wikipedia , lookup
SNP genotyping wikipedia , lookup
Pathogenomics wikipedia , lookup
Bisulfite sequencing wikipedia , lookup
Microsatellite wikipedia , lookup
Molecular Inversion Probe wikipedia , lookup
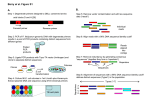
Microbiology (1999), 145, 41 1-417 Printed in Great Britain Molecular evidence for the existence of additional members of the order Chlamydiales Jacobus M. Ossewaarde and Adam Meijer Author for correspondence: Jacobus M. Ossewaarde. Tel: +31 30 274 3942. Fax: +31 30 274 4449. e-mail : [email protected] Research Laboratory for Infectious Diseases, National Institute of Public Health and the Environment, PO Box 1, 3720 BA Bilthoven, The Netherlands Respiratory tract infections in man may be caused by several members of the genus Chlamydia and also b y two Chlamydia-like strains, 'Simkania negewensis' (2-agent) and 'Parachlamydia acanthamoebae ' (Bn,). T o facilitate diagnostic procedures a PCR assay able to detect all known Chlamydiaceae sequences in one reaction was developed. For this purpose, primers were selected to amplify a fragment of the 165 rRNA gene. Characterization of the amplified fragments was done by hybridization with specific probes and by sequencing. PCR assays were carried out using DNA isolated from nosekhroat specimens or from peripheral blood mononuclear cells of patients with respiratory tract infections, and from vessel wall specimens of abdominal aneurysms. Six of the 42 nosekhroat swab specimens analysed yielded strong bands and one yielded a faint band. Three of these bands were identified as Chlamydia pneumoniae and one as Chlamydia trachomatis b y sequencing. Analysis of the three other bands yielded two different new sequences. DNA isolated from peripheral blood mononuclear cells of one patient yielded a third new sequence. DNA isolated from peripheral blood mononuclear cells of four healthy controls was negative. One of the abdominal aneurysm specimens also yielded a strong band. Sequencing revealed a fourth new sequence. All negative controls included during specimen processing and PCR analysis remained negative. The typical secondary structure of microbial 165 genes was present in all four new sequences indicating the validity of the sequence data. All four new sequences were distinct from other bacteria and clustered together with known Chlamydiaceae sequences. Phylogenetic analysis suggested a new lineage, separating the four new sequences, '5. negewensis' and 'P. acanthamoebae ' from the genus Chlamydia with the four known chlamydia1 species. In conclusion, this study provides evidence for the existence of several new members of the order Chlamydiales. Since the source of the Chlamydia-like strains has not been identified and serological and/or molecular cross-reactivities may be expected, results of identification of infecting recognized organisms should be interpreted cautiously. Keywords : Chlamydia, Parachlamydia, 16s rDNA, phylogeny INTRODUCTION Currently, four species are recognized within the genus Chlamydia in the family Chlamydiaceae in the order Chlamydiales. T w o of these four species, Chlamydia ....,.......,....,......,..........,...,.......,..............,..........,,...................................................................... Abbreviation: i.f.u., inclusion-forming units. The GenBank accession numbers for the Chlamydia-like strains are AF097184 (Chlamydia Research Group 1; CRGl), AF097185 (CRGZ), AF097186 (CRG3) and AF097187 (CRG4). 0002-2861 0 1999 SGM trachomatis and Chlamydia pneumoniae, naturally infect humans. C . trachomatis is the leading cause of preventable blindness in developing countries (Schachter & Dawson, 1990),a major cause of sexually transmitted diseases throughout the world (Centers for Disease Control and Prevention, 1993 ; Taylor-Robinson, 1993; World Health Organization Working Group, 1989) and a cause of respiratory tract infections in infants. C . pneumoniae is a major cause of upper and lower respiratory tract infections and has been associated with cardiovascular diseases (Danesh et al., 1997; Gupta & Downloaded from www.microbiologyresearch.org by IP: 88.99.165.207 On: Thu, 15 Jun 2017 08:57:04 41 1 J . M. O S S E W A A R D E a n d A. M E I J E R Camm, 1997; Kuo et al., 1995; Saikku, 1997). Chlamydia psittaci mainly infects animals, including birds, and is a cause of zoonotic respiratory tract infections. Chlamydia pecorum is not known to infect humans. Recently, two Chlamydia-like strains, ‘Simkania negevensis ’, or Z-agent (Kahane et al., 1993), and ‘ Parachlamydia acanthamoebae ’, or Bn, (Amann et al., 1997), have been described. Nucleic acid sequence analysis indicates that they probably belong to the family Chlamydiaceae, but not within one of the four currently recognized species. Both strains seem to be able to infect humans, causing respiratory tract infections (Birtles et al., 1997; Lieberman et al., 1997). Thus, many different Chlamydia species may cause respiratory tract infections in humans. Since isolation in cell culture of the Chlamydia-like strains is probably difficult, we decided to use amplification techniques to study the epidemiology of human chlamydia1 respiratory tract infections. The use of broad range bacterial primers and nucleotide sequencing for identification is only useful when one species is expected (Goldenberger et al., 1997; Greisen et al., 1994). The presence of more than one species would necessitate lengthy cloning and sequencing procedures. Therefore, this approach cannot be applied to detect bacteria in swabs from mucosal sites. Application of specific probes might identify specific pathogens (Monstein et al., 1996), but interference of other bacteria is likely to result in a low sensitivity for detection of some pathogens. Therefore, we developed a Chlamydiaceae-specific PCR assay able to detect all known Chlamydiaceae sequences in one reaction, including those of the recently described Chlamydia-like strains. Here we describe the design of the primers and probes used in this PCR assay and report on the analysis of the first results. METHODS Reference strains. C. pecorum strain E58 (ATCC, Manassas, VA, USA), C. psittaci (avian type, isolated from a human lung biopsy, typed by RFLP of the ompl gene) and C. trachomatis serovar L2 strain 434-B were propagated in monolayers of HeLa 229 (ATCC CCL2.1) cells. C. pneumoniae strain TW183 (Washington Research Foundation, Seattle, WA, USA) was propagated in monolayers of HEp2 cells (ATCC CCL23). Each monolayer was sonicated in 2 ml 0.4 M sucrose-phosphate buffer (4SP) and stored aliquoted at - 70 “C. Batches of C. pneumoniae and C. trachomatis were titrated by inoculating a tenfold serial dilution series onto 1-d-old monolayers in 96-well microtitre plates. After 2 or 3 d incubation the monolayers were fixed with methanol, stained with FITClabelled anti-LPS monoclonal antibodies, and the number of inclusions was counted. Results were expressed as inclusionforming units (i.f.u.) m1-I. Clinical specimens. Specimens were collected from a general practitioner’s surveillance of respiratory tract infections : 42 nose/throat swabs were collected in transport medium (5ml) during the first 3 weeks of January 1997. Aliquots (1ml) were centrifuged in a microcentrifuge, and the pellet was lysed in a buffer with proteinase K (Ossewaarde et al., 1992). After heating for 10 min at 100 “C, the specimens were used directly in the PCR assay. Peripheral blood mononuclear cells from one patient with acute bronchitis (from the acute and the 41 2 convalescent phases) and from four healthy controls working in the same workplace were collected. Mononuclear cells purified from 2.5 ml blood using Histopaque (Sigma-Aldrich) were centrifuged in a microcentrifuge and the pellet was processed as described above. Vessel wall tissue was obtained from six patients during surgical treatment of their abdominal aneurysms. DNA was isolated from three specimens taken from different locations of the aneurysm of each patient using a PCR-inhibitor-free procedure as described previously (Meijer et al., 1998). Design of primers and probes. The 16s rRNA gene was chosen as the target, since it was the only gene of which the sequence was available for all known members of the Chlamydiaceae. All sequences were downloaded from GenBank and aligned. Possible primer and probe locations compatible with all known Chlamydiaceae sequences were selected by comparing this alignment with a quantitative map of nucleotide substitution rates (Van de Peer et al., 1996). Next, the 3’ ends of the primers were analysed for their homology with human sequences using the K-tuple frequency method included in the computer program PC-Rare (Griffais et al., 1996). Thermodynamic properties of the primers and probes were analysed by the computer program Oligo 4.1 (Rychlik & Rhoads, 1989). Finally, the primers and probes were analysed for similarity with other DNA sequences using the output of the BLAST server (Altschul et al., 1990). Out of several sets, one set of primers and probes (Table 1) was selected according to the following criteria : compatibility with all known Chlamydiaceae sequences, lowest homology with human DNA at the 3’ ends of the primers, thermodynamic suitability, and no significant similarity with other DNA sequences. A general family-specific Chlamydiaceae probe was designed using all known Chlamydiaceae sequences and the sequences obtained in this study. PCR reaction and hybridization. The PCR reaction mixture was as described previously including the dUTP-uracil-Nglycosylase contamination prevention system and anti-Taq antibodies (Meijer et al., 1998). The PCR assay was carried out in separate rooms using dedicated equipment (Ossewaarde et al., 1992).Negative controls were included after every three to five specimens during specimen processing and PCR analysis. The final volume was 25 p1 including 5 pl of the specimen. Ten picomoles of each of the eight primers (two forward and six reverse primers) was used. After amplification using a ‘touch-down’ protocol, 10 pl reaction mixture was electrophoresed in a 2 % agarose gel (Meijer et al., 1998). The gels were transferred to nylon membranes by vacuum blotting. The biotin-labelled probes were hybridized at 60 or 65 “C. Binding of the probes was detected by chemiluminescence using the ECL system (Amersham). Since this assay was originally developed to detect known respiratory tract pathogens, only the probes for ‘S. negevensis’, C. pneumoniae and C. psittaci were used for screening the clinical samples. In addition, the probe for ‘ P . acanthamoebae’ and the general Chlamydiaceae probe were used to characterize the new sequences. Sequence analysis. Strong bands in the agarose gels at or close to the expected length were sequenced directly using either the forward primer CHL16SFOR2 or the general sequencing forward primer in the sequencing reaction with the Thermo Sequenase Dye Terminator Cycle Sequencing Pre-Mix kit (Amersham) or the Big Dye Terminator Cycle Sequencing Ready Reaction kit (ABI) on an automated sequencer. Reverse sequencing was carried out using either the resolved reverse primer or the general sequencing reverse primer. Specimens yielding faint bands were amplified from either the original Downloaded from www.microbiologyresearch.org by IP: 88.99.165.207 On: Thu, 15 Jun 2017 08:57:04 New members in the order Chlarnydiales Table 1. Oligonucleotide sequences selected for primers and probes ............................................................................................................................................................... .................................................................................................................................................. Positioning of the oligonucleotideswas based on the alignment of complete 16s rDNA gene sequences. Name Forward primers CHL16SFOR1 Sequence (5’-+3’) Specificity GTGGATGAGGCATGCGAGTCGA CGTGGATGAGGCATGCAAGTCGA ‘S . negevensis ’ All others CTCTCAGCCCGCCTAGACGTCTTAG CAATCTCTCAATCCGCCTAGACGTCTTAG ATCTCTCAATCCGCCTAGACGTCAAAG ATCTCTCAATCCGCCTAGACGTCAAAA CAATCTCTCAATCCGCCTAGACGTCATAG ‘S. negevensis ’ CHL16SREV2 CHL16SREV3 CHL16SREV4 CHLlGSREVS CHL16SREV6 CTCTCAATCCGCCTAGACGTCATCG CHL16SFOR2 Reverse primers CHL 16SREV 1 Probes ‘ P . acanthamoebae’ C. psittaci C. psittaci C. trachomatis C. pecorum C . pneumoniae CHL16SPROBEOl CHL16SPROBE02 CHL16SPROBE03 CHL16SPROBE07 General 1 BIO*AGCTGGGGTAGCCTGGTTTCTT BI0”AAATGTGGTGGGGGTAATTAAATTTAC BIO*CGAATGTGGTATGTTTAGGCATCTAAAAC BIO*CCGAATGTAGTGTAATTAGGCATCTAATATATAT ‘S. negevensis ’ ‘ P. acanthamoebae ’ BIO*TAGTGGCGGAAGGGTTAGTAATACAT Chlamydiaceae General sequencing primers Forward Reverse GTGGATGAGGCATGC(G/A)AGTCGA CTCTCAATCCGCCTAGACGTC Chlamydiaceae Chlamydiaceae C. psittaci C. pneumoniae amount of DNA equivalent t o 0.1 i.f.u. always yielded a clearly visible band of approximately 270 bp after agarose gel electrophoresis, and DNA equivalent to 0.01 i.f.u. yielded a clearly visible band in some experiments. DNA isolated from C. psittaci and C. pecorum reference strains equivalent to 0.1 i.f.u. also yielded a clearly visible band. In each run during this study, positive controls always confirmed this lower limit. Further optimization of the PCR assay was not attempted. specimen or the band recovered from the gel. The obtained sequences were compared with the sequences available in GenBank using the BLAST server (Altschul et al., 1990). The ‘Suggest Tree’ option of the Ribosomal Database Project (University of Illinois, Urbana-Champaign, USA) was used to add the new sequences to the existing tree of the Ribosomal Database Project. The ‘Check Chimera’ option was used to check for possible chimeric sequences created during amplification. All sequences were aligned manually taking into account the secondary structure obtained from the SSU database available at the Antwerp Ribosomal RNA Database (Universityof Antwerp, Antwerp, Belgium; Van de Peer et al., 1998). Phylogenetic analysis was carried out using the neighbour-joining method with a distance matrix calculated by the method of Jukes & Cantor (1969) using TREECON for Windows version 1.3b (Van de Peer & De Wachter, 1994). The corresponding sequence of the related bacterium Rickettsia prowazekii (GenBank M21789) was used to construct a root. The following sequences from GenBank were included: M83313, C. trachomatis (hamster); D85718, C. trachomatis (mouse); U73110, C. trachomatis (swine); D85721, C. trachomatis (man); D85717, C. pecorum (koala); D88317, C. pecorum (calf); D85708, C. psittaci (guinea pig) ; D85713, C. psittaci (bird); D85703, C. psittaci (cat); U73784, C. pneumoniae (horse); 249873, C. pneumoniae (man); L27666, ‘S. negevensis ’ ; Y07556, ‘P. acanthamoebae ’ ; AF097184, Chlamydia Research Group 1 (CRG1);AF097185, CRG2; AF097186, CRG3; AF097187, CRG4. Forty-two patients with upper respiratory tract infections were studied. Six nose/throat swab specimens yielded a strong band in agarose electrophoresis after amplification of the DNA. One specimen yielded a faint band. The first series of hybridization experiments did not result in definite identification of all positive reactions. Using a hybridization temperature lower than optimal (60 “C vs 65 “C), five bands reacted weakly with the C. pneumoniae-specific probe, but none reacted with the C. psittaci-specific probe or with the ‘ S. negevensis ’specific probe (data not shown). Therefore, all six strong amplification products were sequenced directly. The seventh specimen was re-amplified from the original specimen and subsequently sequenced. T w o of these specimens were identified as C. pneurnoniae and the third specimen as C. trachomatis. The fourth specimen yielded a mixture of sequences that could not be resolved. After re-isolation of the DNA from the original specimen and subsequent amplification in the PCR assay, the sequence obtained was identified as that of C. pneumoniae. T h e other three specimens yielded two RESULTS First, the lower limit of the PCR assay was determined using a dilution series of DNA isolated from C. pneumoniae and C. trachomatis reference strains. T h e ~ Downloaded from www.microbiologyresearch.org by IP: 88.99.165.207 On: Thu, 15 Jun 2017 08:57:04 413 J. M. O S S E W A A R D E a n d A. M E I J E R Tabre 2. Reactivity in hybridization of four biotin-labelled species-specific oligonucleotide probes and one biotinlabelled general Chlarnydiaceae oligonucleotide probe with eight amplification products +, Strong reaction, expected for the size of the band in the gel; f,weak reaction, less than expected for the size of the band in the gel ; - , no reaction in the hybridization assay. Probe specificity Hybridization temperature (“C) 60 65 60 65 60 65 60 65 60 C . pneumoniae C. psittaci ‘S.negevensts ’ ‘P. acanthamoebae’ Chlarnydiaceae <- Reaction with amplified product of: C. pneurnoniae C. trachornatis C . psittaci C. pecorurn CRGl CRG2 CRG3 CRG4 + + + - - - - - *- f k - k f - - - - + + f - f - + - - - - - - - - - - - - - - - - - - - - k + + - - - - ..... .. ... ..... ..... ..... .... .... .... .... ... .. + -1 C. t r a c h o m a t i s ACGGAGCAATTGT----- TTCG-----ACGATTGTTTAGTGGC C. pecorum AT. ..G.C---------G.T A......... C. p s i t t a c i .....AT ...GAC--------- GTTG A......... C. pneurnoniae AT...GAC----- ....----- GTTG..A ‘S. n e g e v e n s i s ’ ...A..T.G.AA------ C.T.------ TT.C.AC ........ ‘P. acanthamoebae’ .A.A.GG--------- GCM--------- cc....... ... AG.T.GCA.G-----GCAA----- CTTGC.AC........ CRGl --------- GGA ATCC--------CRG2 CATG.GA.TTGCT....GGTAG.TC..ATG........ CRG3 ---------GG- ..C.. A-CC--------CRG4 ..... + - - - + helix 6 + - ......... ......... .... [- -_ .., _-.., ..,z ..,- ..,_ z * - _.., - + - - - + helix 11 - - - - + - -1 GAAGGGGATC--TTAG--GACCTTTC . . . . . . . . .--. . .c.--........ . . . . . . . . .--. . .c.-- ........ . . . . . . . . .--. . .c.--........ .TT......TCTGC.AAGA.....G. .TG.......--GC.A--.....CG. .T........TCG..AGA.....CG. .TG.......--G..A--.....CG. .T........TAG.GATA......A. .TG.......--G..A--.....CG. Fig. 7. Alignment of helices 6 and 11 (numbers and location from Van de Peer eta/., 1996) of the four recognized species of the family Chlamydiaceae, both Chlamydia-like strains and the four new sequences, taking into account the secondary structure obtained from the SSU database available at the Antwerp Ribosomal RNA Database. Dots represent nucleotides identical to the nucleotide in same position in the C. trachomatis sequence. Dashes represent gaps in the alignment. different new sequences not present in GenBank that clustered together with the Chlamydia-like strains. These sequences were designated CRG2 and CRG3. The DNA isolated from the peripheral blood mononuclear cells from a patient with acute bronchitis yielded a third new sequence not present in GenBank that clustered together with the Chlamydia-like strains. This sequence was designated CRG4. The convalescent specimens were negative. Two of the four healthy controls yielded a faint band slightly longer than the specific chlamydial bands. After re-amplification one contained a mixture of sequences and the other contained another bacterial sequence. One abdominal aneurysm specimen of one patient yielded a strong band, while four specimens of three other patients yielded a faint band. The strong band yielded a fourth new sequence not present in GenBank that clustered together with the Chlamydia-like strains. This sequence was designated CRG1. T w o of the faint bands yielded human sequences; the other faint bands could not be resolved. All faint bands differed in size from the specific chlamydial bands. Reference strains and positive specimens were freshly amplified and at suboptimal and optimal hybridization 41 4 temperatures the reactivity of five different probes was determined for the four recognized species and for all four new sequences (Table 2). The probes derived from the sequence of ‘S. negevensis’ - and of ‘ P . acanthamoebae’ did not react with any of the amplified fragments. The C. psittaci-specific probe showed weak cross-reactions with C. pneumoniae and C. pecorum. In all hybridization experiments, strong reactions were always reproducible, but weak reactions were not always reproducible. When applied to blots of bands of non-Chlamydiaceae sequences such as the human sequences described above, the Chlamydiaceae-specific probe discriminated clearly between chlamydial sequences and sequences from other origins. The validity of the sequence data was tested by constructing the secondary structure typical of all 16s molecules. This typical secondary structure could be produced for all four new sequences. Substantial differences in length were observed in helices 6 and 11 (Fig. 1).Nucleotide substitutions were observed throughout the sequence. The ‘Suggest Tree’ option of the Ribosomal Database Project suggested a phylogenetic tree in which all new seauences were ioined in one branch together with ‘S. negevensis’ and close to other Chlamydia sequences, but distinct from other bacterial Downloaded from www.microbiologyresearch.org by IP: 88.99.165.207 On: Thu, 15 Jun 2017 08:57:04 I New members in the order Chlamydiales - C. rruchomutis (hamster) Distance 0.1 C. trachomais (swine) C. truchomutis (man) C.psittuci (guinea pig) C.psiftuci (bird) 1Wh C. psittuci (cat) I C. pneumoniae (horse) C. pneumoniae (man) 98% ‘ I ? ucunthmoebae’ CRG3 S. negevensis’ CRG I I R.prowazekii Fig. 2. Phylogenetic analysis of the amplified region (216-224 bp) of the four recognized species of the family Chlamydiaceae, both Chlamydia-like strains and the four new sequences obtained in this study. The sequence CRGl was obtained from a vascular specimen; CRGZ and CRG3 from respiratory specimens; and CRG4 from a peripheral blood mononuclear cell specimen. Percentages represent the number of times the branch appeared in a tree during 1000 bootstrap samples. The genetic distance is represented as fixed mutations per site. Table 3. Percentage nucleotide similarity of the four new sequences, the two Chlamydia-like strains and example sequences of the four recognized Chlamydia species C. pecorttm C. psrttacr C. trachomatis C. pneumoniae ‘ S . negevensrs ’ * P. acanthamoebae‘ CRG 1 CRGZ CRG3 CRG4 C. pecorum C. psittaci C. trachomatis C. pneumoniae ‘S. negeuenris’ ‘D.acanthamoebae’ CRGl CRGZ CRG3 CRG4 100.0 93.5 1000 88% 865 100.0 89.0 93.5 8 41 100.0 71.0 70.6 71.0 7 1-4 1000 73.9 73.5 71.8 735 75.5 100.0 702 722 71.8 73.9 78.8 7.53 100.0 76.7 78.4 747 79.6 75.1 a37 75.5 1000 66.9 678 67.3 69.0 72.7 67.8 72.’’ 70.6 1000 73.9 75.5 74.7 76.3 74.3 82.4 727 91.4 71.0 100.0 sequences. The ‘Check Chimera’ option did not show evidence for chimeric sequences. All new sequences and example sequences from the four recognized Chlamydia species, ‘ S. negevensis ’ and ‘P. acanthamoebae ’ were manually aligned taking into account the secondary structure obtained from the SSU database available at the Antwerp Ribosomal RNA Database. Fig. 2 shows the phylogenetic analysis carried out using the neighbour-joining method with a distance matrix calculated by the method of Jukes & Cantor (1969) using TREECON for Windows. The percentage similarity between sequences of the order Chlamydiales ranged between approximately 65 and 95 YO. Percentage similarities of type strains are listed in Table 3. DISCUSSION Using a new Chlamydiaceae-specific PCR we have obtained molecular evidence for the existence of at least four new strains. Sequence analysis showed that these strains were distinct from all other known bacteria and clustered together with ‘S. negevensis’ and ‘ P . acanthamoebae’ in a separate lineage in the order Chlamydiales. Currently, four species are recognized within a single genus Chlamydia belonging to the only family, Chlamydiaceae, within the order Chlamydiales : C . pecorum, C . pneumoniae, C. psittaci and C. trachomatis. Molecular, microbiological and immunological analyses have improved this classification by reclassifying several strains; for example, a horse strain and a koala bear strain are now classified as C. pneumoniae (Kaltenboeck et al., 1993; Storey et al., 1993). The species C. psittaci is very heterogeneous. Microbiological studies have defined eight biotypes (Spears & Storz, 1979) and serological studies have defined nine immunotypes (Perez-Martinez & Storz, 1985). The type strains of both C. pneumoniae and C. pecorum were originally classified as C . psittaci. Detailed molecular analysis of the nucleotide sequences of the 16s rRNA gene and of the ribosomal intergenic spacer has now revealed several sub-groups within C. psittaci and C. trachomatis (Everett & Andersen, 1997; Pudjiatmoko et al., 1997). Human C. trachornatis is subdivided into three biovars: the mouse biovar with one serotype (the mouse pneumonitis agent) ; the trachoma biovar consisting of the serovars A-K; and the lymphogranuloma venereum biovar consisting of the serovars Ll-L3. Downloaded from www.microbiologyresearch.org by IP: 88.99.165.207 On: Thu, 15 Jun 2017 08:57:04 41 5 J. M. O S S E W A A R D E a n d A. MEIJER Currently, 19 different human serovars of C . trachomatis are recognized (Grayston & Wang, 1975; Ossewaarde et al., 1994; Wang & Grayston, 1991). Recent evidence suggests that some strains isolated from swine and hamsters may also be classified as C . trachomatis (Everett & Andersen, 1997; Fox et al., 1993; Kaltenboeck & Storz, 1992; Pudjiatmoko et af., 1997). Two recently identified Chlamydia-like strains, ‘S. negeuensis’ and ‘ P . acanthamoebae’, have not been definitely classified yet. Using phylogenetic analysis they appear to be in a sub-branch distinct from, but closely related to, all other Chlamydia strains. Genetic analysis suggested that ‘S. negevensis’ might belong to a new genus within the family ChZamydiaceae (Kahane et af., 1995). The new sequences cluster together with known Chlamydia sequences apart from other bacteria using data from large 16s sequence databases. The genetic distances between all Chlamydia sequences suggest a division in two lineages : the four recognized Chlamydia species in one lineage and the Chlamydia-like strains in a second lineage. The phylogenetic branch separating these lineages was highly significant by bootstrap analysis. Although all our samples were from clinically ill patients, it is still too early to draw any conclusions on the pathogenicity of these new strains. One of the new sequences was derived from mononuclear cells of a patient with bronchitis. One and two weeks later comparable specimens from the same person were negative. In addition, four healthy controls, volunteers from the same workplace, were negative. These data suggest the involvement of this new Chlamydia strain in respiratory tract infections, but pathogenicity of these new strains has to be established in more extensive studies. O n the other hand, both ‘S. negevensis’ and ‘ P . acanthamoebae ’ could be considered environmental contaminants : ‘S. negevensis ’ was originally found as a cell culture contaminant and ‘ P . acanthamoebae’ as an intracellular parasite of possibly free-living amoebae. Therefore, we cannot exclude the possibility that these new strains caused positive PCR assay results by contamination somewhere in the diagnostic chain, either in the patient or during specimen processing. However, the existence of these new organisms might have significant consequences for serological and molecular laboratory diagnosis of chlamydia1 respiratory tract infections. So far, there are no data suggesting antigenic cross-reactions between the new strains and recognized species. If such cross-reactions exist, however, serological data should be more carefully interpreted. For example, serological cross-reactions between C. pneumoniae and C . trachomatis are well-documented (Kern et al., 1993; Moss et al., 1993). This study shows the existence of three regions of highly conserved sequences in the 16s rRNA gene within the family Chlamydiaceae. The existence of more regions can be expected in the remaining part of the 16s rRNA gene. If primers and probes have been chosen from these locations during the design of PCR assays, positive reactions might be incorrectly interpreted as a positive 416 diagnosis of a C . pneumoniae infection. At least, the possible existence of serological or molecular biological cross-reactions should be taken into account when interpreting already published data. In conclusion, we have identified four new previously unrecognized Chfamydiaceae sequences. Phylogenetic analysis strongly suggests that they belong to a separate lineage within the order Chfamydiales. ACKNOWLEDGEMENTS T h e authors thank J. de Jong and J. A . van der Vliet for providing the patient specimens and T. M. Bestebroer for assistance in DNA sequencing. REFERENCES Altschul, 5. F., Gish, W., Miller, W., Myers, E. W. & Lipman, D. J. (1990). Basic local alignment search tool. J Mol Biol215,403410. Amann, R., Springer, N., Schanhuber, W., Ludwig, W., Schmid, E. N., MUller, K. D. & Michel, R. (1997). Obligate intracellular bacterial parasites of Acanthamoebae related to Chlamydia spp. Appl Environ Microbiol63, 115-121. Birtles, R. J., Rowbotham, T. J., Storey, C., Marrie, T. 1. & Raoult, D. (1997). Chlamydia-like obligate parasite of free-living amoebae. Lancet 349,925-926. Centers for Disease Control and Prevention (1993). Recom- mendations for the prevention and management of Chlamydia trachomatis infections. Morb Mortal W k l y Rep 42, 1-9. Danesh, J., Collins, R. & Peto, R. (1997). Chronic infections and coronary heart disease: is there a link? Lancet 350, 430-436. Everett, K. D. E. & Andersen, A. A. (1997). The ribosomal intergenic spacer and domain I of the 23s rRNA gene are phylogenetic markers for Chlamydia spp. lnt ] Syst Bacteriol47, 461473. Fox, 1. G., Stills, H. F., Paster, B. 1.. Dewhirst, F. E., Yan, L., Palley, L. & Prostak, K. (1993). Antigenic specificity and morphologic characteristics of Chlamydia trachomatis, strain SFPD, isolated from hamsters with proliferative ileitis. Lab Anim Sci 43,405-410. Goldenberger, D., KUnzli, A., Vogt, P., Zbinden, R. &Altwegg, M. (1997). Molecular diagnosis of bacterial endocarditis by broad- range PCR amplification and direct sequencing. J Clin Microbiol 35,2733-2739. Grayston, 1. T. & Wang, 5. P. (1975). New knowledge of Chlamydiae and the diseases they cause. J lnfect Dis 132,87-105. Greisen, K., Loeffelholz, M., Purohit, A. & Leong, D. (1994). PCR primers and probes for the 16s rRNA gene of most species of pathogenic bacteria, including bacteria found in cerebrospinal fluid. ] Clin Microbiol 32, 335-351. Griffais, R., AndrB, P. M. & Thibon, M. (1996). K-tuple frequency in the human genome and polymerase chain reaction. Nucleic Acids Res 19, 3887-3891. Gupta, 5. & Camm, A. 1. (1997). Chlamydia pneumoniae and coronary heart disease : coincidence, association, or causation ? BY Med ] 314, 1778-1779. Jukes, T. H. & Cantor, C. R. (1969). Evolution of protein molecules. In Mammalian Protein Metabolism, pp. 21-132. Edited by H. H. Munro. New York: Academic Press. Kahane, S., Gonen, R., Sayada, C., Elion, J. & Friedman, M. G. (1993). Description and partial characterization of a new chlamydia-like microorganism. FEMS Microbiol Lett 109, 329-334. Downloaded from www.microbiologyresearch.org by IP: 88.99.165.207 On: Thu, 15 Jun 2017 08:57:04 New members in the order Chlamydiales Kahane, S., Metzer, E. & Friedman, M. G. (1995). Evidence that the novel microorganism 'Z' may belong to a new genus in the family Chlamydiaceae. FEMS Microbiol Lett 126, 203-208. Perez-Martinez, 1. A. & Storz, J. (1985). Antigenic diversity of Chlamydia psittaci of mammalian origin determined by microimmunofluorescence. Infect Immun 50, 905-910. Kaltenboeck, B. & Storz, J. (1992). Biological properties and genetic analysis of the o m p A locus in Chlamydiae isolated from swine. Am J Vet Res 53, 1482-1487. Pudjiatmoko, Fukushi, H., Ochiai, Y., Yamaguchi, T. & Hirai, K. (1997). Phylogenetic analysis of the genus Chlamydia based on Kaltenboeck, B., Kousoulas, K. G. & Storz, 1. (1993). Structures of Rychlik, W. & Rhoads, R. E. (1989). A computer program for and allelic diversity and relationships among the major outer membrane protein (ompA)genes of the four chlamydial species. J Bacteriol 175, 487-502. Kern, D. G., Neill, M.A. & Schachter, 1. (1993). A seroepidemiologic study of Chlamydia pneumoniae in Rhode Island. Chest 104, 208-2 13. Kuo, C. C., Jackson, L. A., Campbell, L. A. & Grayston, 1. T. (1995). Chlamydia pneumoniae (TWAR).Clin Microbiol Rev 8,451-461. Lieberman, D., Kahane, S., Lieberman, D. & Friedman, M. G. (1997). Pneumonia with serological evidence of acute infection with the chlamydia-like microorganism " Z". Am J Respir Crit Care Med 156,578-582. Meijer, A,, Van der Vliet, 1. A., Schouls, L. M., De Vries, A., Roholl, P. J. M. & Ossewaarde, 1. M. (1998). Detection of microorganisms in vessel wall specimens of the abdominal aorta : development of a PCR assay in the absence of a gold standard. Res Microbioll49, 577-583. Monstein, H. J., Kihlstrom, E. & Tiveljung, A. (1996). Detection and identification of bacteria using in-house broad range 16s rDNA PCR amplification and genus-specific DNA hybridization probes, located within variable regions of 16s rRNA genes. APMIS 104,451458. Moss, T. R., Darougar, S., Woodland, R. M., Nathan, M., Dines, R. 1. & Cathrine, V. (1993). Antibodies to Chlamydia species in patients attending a genitourinary clinic and the impact of antibodies to C. pnetlmoniae and C . psittaci on the sensitivity and the specificity of C . trachomatis serology tests. Sex Transm Dis 20, 61-65. Ossewaarde, J. M., Rieffe, M., Rozenberg-Arska, M., Ossenkoppele, P. M., Nawrocki, R. P. & Van Loon, A. M. (1992). Development and clinical evaluation of a polymerase chain reaction test for detection of Chlamydia trachomatis. J Clin Microbiol30, 2122-2128. Ossewaarde, J. M., Rieffe, M., De Vries, A., Derksen-Nawrocki, R. P., Hooft, H. J., Van Doornum, G. 1. J. &Van Loon, A. M. (1994). Comparison of two panels of monoclonal antibodies for determination of Chlamydia trachomatis serovars. J Clin Microbiol 32,2968-2974. 16s rRNA gene sequences. lnt J Syst Bacteriol47, 425431. choosing optimal oligonucleotides for filter hybridization, sequencing and in vitro amplification of DNA. Nucleic Acids Res 17, 8543-8551. Saikku, P. (1997). Chlamydia pneumoniae and atherosclerosis an update. Scand J Infect Dis 104 (Suppl.), 53-56. Schachter, J. & Dawson, C. R. (1990). The epidemiology of trachoma predicts more blindness in the future. Scand J Infect Dis 69 (Suppl.), 55-62. Spears, P. & Storz, J. (1979). Biotyping of Chlamydia psittaci based on inclusion morphology and response to diethylaminoethyl-dextran and cycloheximide. lnfect Immun 24, 224-23 2. Storey, C., Lusher, M., Yates, P. & Richmond, 5. (1993). Evidence for Chlamydia pneumoniae of non-human origin. J Gen Microbiol 139, 2621-2626. Taylor-Robinson, D. (1993). Chlamydia trachomatis and sexually transmitted disease. What do we know and what shall we d o ? Br Med J 308, 150-151. Van de Peer, Y. & De Wachter, R. (1994). TREECON for Windows: a software package for the construction and drawing of evolutionary trees for the Microsoft Windows environment. Comput Appl Biosci 10, 569-570. Van de Peer, Y., Chapelle, S. & De Wachter, R. (1996). A quantitative map of nucleotide substitution rates in bacterial rRNA. Nucleic Acids Res 24, 3381-3391. Van de Peer, Y., Caers, A., De Rijk, P. & De Wachter, R. (1998). Database on the structure of small ribosomal subunit RNA. Nucleic Acids Res 26, 179-182. Wang, 5. P. & Grayston, 1. T. (1991). Three new serovars of Chlamydia trachomatis: Da, Ia, and L2a. J Infect Dis 163, 403-405. World Health Organization Working Group (1989). Guidelines for the prevention of genital chlamydial infections. WHO Report EUR/ICP/CDS 199. Geneva : WHO. Received 3 August 1998; revised 14 October 1998; accepted 22 October 1998. Downloaded from www.microbiologyresearch.org by IP: 88.99.165.207 On: Thu, 15 Jun 2017 08:57:04 417