* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Spinal Nerves Posterior View
Feature detection (nervous system) wikipedia , lookup
Biological neuron model wikipedia , lookup
Central pattern generator wikipedia , lookup
Premovement neuronal activity wikipedia , lookup
Molecular neuroscience wikipedia , lookup
Neurotransmitter wikipedia , lookup
Proprioception wikipedia , lookup
Synaptic gating wikipedia , lookup
End-plate potential wikipedia , lookup
Synaptogenesis wikipedia , lookup
Nervous system network models wikipedia , lookup
Development of the nervous system wikipedia , lookup
Axon guidance wikipedia , lookup
Clinical neurochemistry wikipedia , lookup
Neural engineering wikipedia , lookup
Neuropsychopharmacology wikipedia , lookup
Neuromuscular junction wikipedia , lookup
Circumventricular organs wikipedia , lookup
Neuroanatomy wikipedia , lookup
Stimulus (physiology) wikipedia , lookup
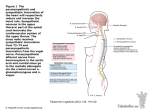
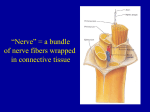
Peripheral Nervous System (PNS) Figure 12.16a Structure of a Nerve Each neuron is surrounded by a sheath called the endoneurium. Some axons have an additional sheath called myelin. A bundle of neurons travel together in a fascicle, and are surrounded by perineurium. A bundle of fascicles is surrounded by epineurium Figure 12.16a Spinal Nerves Posterior View Figure 14.9 Cut nerves • If a small nerve is cut, it will regenerate because where are the cell bodies? In the posterior root ganglion (sensory) or anterior horn (motor). • Since the cell body is about a meter away, axons can regrow. • Large nerves are harder to regrow, but you can still stitch the ends together at the epineurium and perineurium, and you may get healing. Pinched nerves • When a nerve gets pinched (e.g. herniated disc), it damages the nerve by interfering with its action potential, causing weakness, pain, or paralysis. Disruption of Blood Supply • When a body part “falls asleep”, the region has become ischemic, impairing the action potential of the nerves. Unlike the CNS, when blood is restored to the PNS, the nerves recover. Damage to the CNS tends to be permanent, but damage to the PNS tends to heal. DAMAGE TO THE NERVOUS SYSTEM • If a person has a spinal cord injury in their cervical region, they could have quadriplegia (arms and legs paralyzed). • If a person has a spinal cord injury in their thoracic region, they could have paraplegia (just legs are paralyzed). SOME CLINICALLY IMPORTANT PERIPHERAL NERVES: • Note: an epidural nerve block during child birth will numb the mother from her navel to her knees. • PUDENDAL NERVE: this is the nerve that can be anesthetized during childbirth as an alternative to an epidural (a pudendal nerve block is also called a saddle block because the numb areas are where you would be touching a saddle). • PHRENIC NERVE: allows the diaphragm to contract. If it gets severed, the person can no longer breathe without assistance. SENSORY NERVES • These come out of the spinal cord and go to specific regions of the body. Each region of the body is innervated by spinal nerves. • For example, nerve C4 innervates region C4 of the DERMATOME. • It’s important to know these dermatome regions (not for this class), especially physical therapists and nurses. Map of Dermatomes Figure 14.17a SENSORY NERVES • If a patient has a shooting pain down the anterior shin, what nerve is pinched? L5. • Numbness in pinky and ring finger is what nerve? C8. • If a workman’s comp patient comes in saying his whole hand is numb, no other symptoms, you know he’s lying because the nerves don’t run that way. • They also don’t run transversely across the body; they are on one side or the other. Nerve Plexus A PLEXUS is a network of nerves that primarily serves the limbs. There are four major plexi: cervical, brachial, lumbar, and sacral. 1. CERVICAL PLEXUS comes out of the neck and are cutaneous nerves (sensory input of the skin) of the neck and back of the head. Cervical Plexus BRACHIAL PLEXUS 2. BRACHIAL PLEXUS • This is the major group of nerves that supply the upper limbs. It runs through the axilla. • If a person leans their armpits on their crutches, they can damage this plexus and lose the use of their arms. • The nerves in the brachial plexus change names as they go to different regions in the arm. The Brachial Plexus Figure 14.12a Axillary Musculocutaneus Major Nerves of the Upper Extremity Axillary Nerve • Deltoid Musculocutaneus Nerve • Supplies anterior muscles of the arm Median Nerve • Supplies no muscles of the arm • Supplies anterior forearm (except flexor carpi ulnaris) • Carpal Tunnel Syndrome – Hand of benediction Carpel Tunnel Syndrome • The median nerve travels under the transverse carpal ligament. • The nerve is pinched in carpal tunnel syndrome. Carpel Tunnel Syndrome Carpel Tunnel Syndrome MEDIAN NERVE • This is the nerve that gets cut when people try to slit their wrists. • The arteries are so small in the wrist; people rarely die from this type of suicide attempt. However, they live with a lot of tissue damage. They are not able to move the thumb towards the little finger, so it is hard to pick up small objects. This is called “ape hand”. Ulnar Nerve • Supplies flexor carpi ulnaris • “Funny Bone” • Damage can cause claw hand; cannot adduct or abduct fingers Radial Nerve • Supplies muscles on the posterior arm and forearm • Damage can cause wrist drop Carpel Tunnel Syndrome Axillary, Radial, Ulnar, Median Nerves Figure 14.4 Brachial Plexus • Damage to Brachial Plexus – Klumpke’s paralysis (brachial plexus damaged during birth) – Acquired Brachial Plexus injuries • Crutch paralysis (total upper extremity paralysis) • Claw Hand / Ape hand • Hand of benediction • Wrist Drop (Waiter’s Hand) LUMBAR PLEXUS 3. LUMBAR PLEXUS • FEMORAL NERVE is the main nerve to the anterior thigh. Lumbo-Sacral Plexus • Lumbar: – Femoral nerve • Sacral: – Sciatic nerve The Lumbar Plexus Figure 14.15 Sacral Plexus 4. SACRAL PLEXUS are spinal nerves from L4-S5 • Some of the fibers from the lumbar plexus mix with the sacral plexus, so these are often referred to together as the lumbosacral plexus. • SCIATIC NERVE is the largest branch of the sacral plexus and the largest nerve in the body; it leaves the pelvis through the sciatic notch. • A short, thick muscle (Piriformis muscle) covers the sciatic notch, and when it contracts, it can pinch the sciatic nerve, causing a type of sciatica (sciatic nerve irritation) known as piriformis syndrome. • This can be alleviated by stretching exercises. However, sciatica can also be caused if there is a herniated lumbar disc, in which case stretching exercises make it worse. The Sacral Plexus Figure 14.16a, c Obturator Femoral Nerves of the Lower Extremity The sciatic nerve supplies the back of the thigh, then branches out into the TIBIAL and FIBULAR (peroneal) nerves, which supply the leg and foot. The fibular nerve branches into superficial and deep. Lower Extremity Nerves Obturator Nerve Supplies adductor muscles Sciatic Nerve Supplies back of thigh, leg and foot Femoral Nerve Supplies anterior Thigh Tibial Nerve Supplies posterior leg and foot Common Fibular Nerve Superficial branch Supplies lateral side of leg Deep branch Supplies anterior leg Injury causes “Foot Drop” Tibial Nerve • Sometimes a small branch of the tibial nerve in the foot gets pinched between the metatarsal heads, and the irritation causes nerve swelling and pain. • It is called a neuroma (“nerve tumor”) and manifests as pain in the ball of the foot, made worse with high heels. • An injury to the fibular nerve may result in “foot drop”, where the foot cannot be dorsiflexed. AUTONOMIC NERVOUS SYSTEM • We don’t have voluntary control over these nerves. • They are involved digestion, blood flow, urination, defecation, glandular secretion. • Therefore, the ANS supplies the glands, smooth muscle, and cardiac muscle, but NOT the skeletal muscle. • For this reason, the ANS is also called the general visceral motor system. Sympathetic Division of the ANS Figure 15.7 ANS • All of the neurons of the ANS are motor neurons (there are no sensory neurons in the ANS). • The ANS differs from the CNS reflex arc because the ANS has two lower motor neurons in the periphery (the cell body of one is in the spinal cord and the cell body of the other is in the periphery), whereas the CNS has one lower motor neuron, and its cell body is within the spinal cord, not in the periphery. ANS • The ANS neuron comes from the spinal cord and synapses on the cell body of another neuron, which then synapses on the target (gland, blood vessel, etc). Ganglia • The area where the two neurons come together is the AUTONOMIC GANGLIA. • The first neuron is the PRE-GANGLIONIC NEURON. • The second neuron is the POSTGANGLIONIC NEURON. • Some of these ganglia (those in the sympathetic division of the ANS) are lined up along the vertebral column, called a structure called the sympathetic trunk ganglia. ANS • The ANS motor unit is characterized by having more than one lower motor neuron, the axons may be myelinated or unmyelinated, conduction is slow, and the axons are thin. • The ANS has two divisions: sympathetic and parasympathetic. ANS has TWO lower motor neurons Preganglionic neuron CNS has just one lower motor neuron Post-ganglionic neuron Ganglion (where the cell bodies of the postganglionic neurons are) SYMPATHETIC DIVISION • ↑heart rate and blood pressure, • ↑metabolic activity (increased blood glucose), • decreased peristalsis (decreased food digestion) • dilation of bronchioles • control of blood flow to the skin • sweating Sympathetic Division • E.g. when running, ↑heart rate = sympathetic. • When hot sweat = sympathetic. • The term “Fight or Flight” is inaccurate; it refers to the ↑ heart rate, etc, but the sympathetic division is also active when relaxing on a nice beach with a cool drink on a hot day, because whenever you’re sweating, that’s the sympathetic division. ANATOMY OF THE SYMPATHETIC DIVISION • The sympathetic neurons exit the spinal cord at the thorax and lumbar regions. • The axons of most pre-ganglionic neurons in the sympathetic division are fairly short, and they synapse quickly on a ganglia. • All these ganglia together are the SYMPATHETIC TRUNK (CHAIN) GANGLIA. • Therefore, the postganglionic cell bodies of the sympathetic nervous system are in the chain ganglia. • There are also nerves that connect the ganglia to each other. Sympathetic Trunk Ganglia Figure 15.8 Sympathetic Division In Sympathetic division, preganglionic axons are SHORT because they terminate in ganglia that are close to the spinal cord That means the postganglionic axons are LONG, because they have to reach all the way to the target muscle. Sympathetic Division • The axons of POST-GANGLIONIC NERVES are very long, and go to the target organs. • Some pre-ganglionic neurons bypass the sympathetic chain ganglia and go directly to the abdomen. • They create a group of ganglia in the abdomen called the SOLAR PLEXUS (“sun”). When you get punched in the abdomen, you are punched in the solar plexus, and get the wind knocked out of you. PARASYMPATHETIC DIVISION • Unlike the sympathetic division, the axons of the preganglionic neurons of the parasympathetic division are long, and the axons of the postganglionic neurons are short. • The nerve cell bodies (peripheral ganglia) of the parasympathetic division are closer to the organs being innervated than in the sympathetic division. • In fact, the cell bodies are either next to or inside of the target organs. Therefore, they have short post-ganglionic fibers. Parasympathetic Division In the Parasympathetic division, preganglionic axons are LONG because they terminate in ganglia that are close to the target organ That means the postganglionic axons are SHORT PARASYMPATHETIC DIVISION • Involved in vegetative activities, such as digestion, urination, defecation • Has postganglionic cell bodies in terminal ganglia, located either near or within target organs • Has both preganglionic and postganglionic neurons that secrete acetylcholine • Has preganglionic cell bodies located in the cranial and sacral areas. Parasympathetic Division • The function of this division is often antagonistic (opposite) of the sympathetic, but actually, they work together. • The parasympathetic division inhibits cardiac contraction, so there is: ↓heart rate, constricts bronchioles, activates digestive system, and causes salivation, urination, and defecation. • When you are lounging on the beach, the heart rate decreases (parasympathetic), but the sweat increases (sympathetic). Vagus Nerve • The parasympathetic neurons come out of either the brain or the sacral region of the spinal cord. • The majority of the parasympathetic outflow from the head is by the vagus nerve. Vasovagal Syncope (Fainting) • The most common type of fainting. • After a stressful trigger, the parasympathetic nervous system is enhanced by the Vagus nerve. • The heart rate speeds up, then suddenly drops. • Then the blood pressure drops. • Unconsciousness results. • Treatment: elevate the legs above the heart for a few minutes, and make sure the airway remains open. • A cold, wet cloth on the forehead and back of the neck may make the person feel better as they recover. Path of the Vagus Nerve Figure 15.6 Reynaud's Phenomenon • Autonomic nervous system is hyperactive in the ANS neurons that innervate the walls of blood vessels. • It causes spasms of peripheral blood vessels, cuts off some blood supply, and causes the fingers and toes to be white or blue. • Emotional stress and being cold tend to trigger the discoloration. VISCERAL (“organ”) SENSES • A visceral nerve innervates involuntary effectors (smooth muscles in organs). • A somatic motor nerve innervates voluntary effectors (skeletal muscle). – (don’t confuse this with a somatic sensory nerve for the sense of touch; sensory nerves are not part of the ANS) VISCERAL (“organ”) SENSES • Internal organs also have sensory nerves that tell you when you have eaten enough or your bladder is full. These are not part of the ANS because they are sensory. • Not all organs have sensory nerves, for instance, you can’t feel when you have high blood pressure. • You can also have visceral reflexes, which trigger the parasympathetic system to contract the bladder when full, etc. • Reflexes are hard to localize. Referred Pain • Pain in an organ may not be where the organ is. • Heart pain usually manifests in the left side of chest, the left shoulder, arm, but not the heart. • This is REFERRED PAIN. • Pain in the lungs usually shows up as neck pain. • These areas of referred pain are important to know, but not for this class. A Map of Referred Pain Figure 15.15 Caffeine • With frequent use, tolerance to many of the effects of caffeine will develop. At doses of 600 milligrams (about six cups of coffee) or more daily, caffeine can cause nervousness, sweating, tenseness, upset stomach, anxiety, and insomnia. It can also prevent clear thinking and increase the side effects of certain medications. This level of caffeine intake represents a significant health risk. Caffeine • Caffeine can be mildly addictive. Even when moderate amounts of caffeine are withdrawn for 18 to 24 hours, one may feel symptoms such as headache, fatigue, irritability, depression, and poor concentration. The symptoms peak within 24 to 48 hours and progressively decrease over the course of a week. To minimize withdrawal symptoms, experts recommend reducing caffeine intake gradually. Caffeine • At levels over 200 milligrams per day, caffeine may delay conception and doubles the risk of miscarriages and low birth weight babies. • Caffeine and tannin in tea decreases iron and protein absorption, and is especially dangerous during pregnancy. • Caffeine taken during pregnancy is thought to increase the probability of a child contracting diabetes. • Because children have developing nervous systems, it is important to moderate their caffeine consumption. Caffeine • • • • • • • • • • • • Expresso: 502 mg Jolt Energy: 280 mg Coffee: 85 mg Red Bull: 80 mg Mountain Dew: 55 mg Green tea: 50 mg Tea: 47 mg Coke: 37 mg Dark Chocolate (1.5 oz): 20 mg Milk Chocolate (1.5 oz): 9 mg Hot Chocolate: 5 mg Root Beer, Ginger ale, Lemon-Lime: 0 mg Symptoms of Excess Caffeine • nervousness • anxiety • irritability • agitation • tremors • insomnia • depression headache upset stomach GI irritation heartburn diarrhea fatigue dizziness increased heart rate irregular heartbeat elevated BP increased cholesterol nutritional deficiencies poor concentration bed wetting Caffeine Withdrawal Symptoms • • • • • • • headache craving irritability insomnia fatigue depression apathy constipation runny nose anxiety nausea nervousness vomiting shakiness cramps dizziness ears ringing drowsiness hot and cold inability to concentrate The Autonomic Nervous System Def: The ANS consists of all visceral motor neurons innervating smooth muscle, cardiac muscle and glands. 73 74 Sympathetic and Parasympathetic Divisions of the ANS • How they are similar: – Both divisions are part of the ANS – Both have effects on smooth muscle, cardiac muscle and glands • How they differ: – Stimulation of effectors by each system vary from one body system to another. Effects may be stimulatory or inhibitory. – Location – Length of pre and postganglionic fiber – Neurotransmitters used 75 Comparison of ANS and Somatic Motor Pathways • Somatics – Single neuron from spinal cord to effector – One neuron innervates the effector cell – NTS is acetylcholine (ACh) • Autonomics – Two neurons relay (ganglion) to effector – Dual innervation of effectors – NTS at ganglia (ACh); NTS at effector can be ACh or norepinephrine 76 Location and neurotransmitters used by Sympathetic/Parasymp adrenergic receptors sympathetic preganglionic neuron postganglionic neuron parasympathetic nicotinic receptors muscarinic receptors Characteristics of Sympathetic and Parasympathetic Function • Post-ganglionic sympathetic nerves release norepinephrine at their nerve endings – these nerves are called adrenergic nerves • Pre and post-ganglionic parasympathetic nerves release acetylcholine at their nerve endings (Nitric oxide- corpora cavernosa) – these nerves are called cholinergic nerves • EXCEPTION FOR SYMPATHETIC: – Cholinergic: mACH; used in body wall. – Vasodilation of vessels in brain and skeletal muscle – Piloerector muscles – Sweat glands – Nitric oxide: vasodilation of vessels in brain, skeletal muscle Sympathetic Nervous System “Thoracolumbar” When active? Length of pre and postganglionic nerve? Location of cell bodies of preganglionic nerve? Location of cell bodies of postganglionic nerve? Neurotransmitters released? 79 Adrenal medulla Figure 60-1; Guyton & Hall Parasympathetic Nervous System “cranio-sacral” Parasympathetic nerves originate from cranial nerves III, VII, IX, and X and the sacral spinal cord. occulomotor nerve - fibers to the pupillary sphincters and ciliary muscle facial nerve - fibers to lacrimal and submandibular gland glossopharyngeal nerve - fibers to parotid gland vagus nerve - motor inputs to visceral organs sacral segments - fibers to descending colon, rectum, bladder and genitalia Figure 60-3; Guyton & Hall 80 Effects of the ANS on the Organs • eye – sympathetic --pupillary dilation (alpha 1 receptor) – parasympathetic--pupillary constriction and accommodation (focusing) of the lens (mACh receptor) • glands of the body – parasympathetic stimulate the nasal, lacrimal, salivary, and G.I. glands (mACh receptor) – sympathetic stimulates the sweat glands (mACh receptor) Effect of the Autonomic Nervous System on the Organs • G.I. tract – parasympathetic stimulates overall activity including G.I. smooth muscle – sympathetic has very little effect • heart – sympathetic increases the rate and contractility – parasympathetic decreases heart rate • blood vessels – sympathetic causes vasoconstriction. Reduced sympathetic response accounts for most vasodilation. – parasympathetic causes some vasodilation (e.g., penis) Sympathetic and Parasympathetic “Tone” • the basal rate of activity of each system • this background activity allows for an increase or decrease in activity by a single system – sympathetic tone normally causes about a 50 % vasoconstriction • increasing or decreasing “tone” can change vessel diameter – parasympathetic tone provides background G.I. activity adrenergic or sympathomimetic drugs act like norepinephrine • these drugs have an effect which is much more prolonged than that of either norepinephrine – phenylephrine stimulates alpha receptors – isoproterenol stimulates both beta1 and beta2 receptors – albuterol stimulates only beta2 receptors • some drugs act indirectly by increasing the release of norepi from its storage terminals – ephedrine, amphetamine, pseudoephedrine, Pharmacology of the Sympathetic Nervous System • drugs that block the effect of norepinephrine • alpha blockers – phentolamine – Cheap Viagra! • beta blockers – beta1 and 2 propranolol Pharmacology of the Parasympathetic Nervous System • parasympathomimetic drugs – muscarine – pilocarpine • activates muscarinic receptors, cause profuse sweating (why if sweat glands are controlled by sympathetic system?) • cholinesterase inhibitors – neostigmine, potentiates the effect of acetylcholine • antimuscarinic drugs – atropine blocks the effect of acetylcholine on effector cells