* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Genetic analysis of a congenital nephrogenic diabetes insipidus
Genetic engineering wikipedia , lookup
Epigenetics of neurodegenerative diseases wikipedia , lookup
Cell-free fetal DNA wikipedia , lookup
Gene nomenclature wikipedia , lookup
Genome evolution wikipedia , lookup
Therapeutic gene modulation wikipedia , lookup
Vectors in gene therapy wikipedia , lookup
Genome (book) wikipedia , lookup
Gene expression programming wikipedia , lookup
Gene therapy wikipedia , lookup
Site-specific recombinase technology wikipedia , lookup
Population genetics wikipedia , lookup
Oncogenomics wikipedia , lookup
Neuronal ceroid lipofuscinosis wikipedia , lookup
Saethre–Chotzen syndrome wikipedia , lookup
Nutriepigenomics wikipedia , lookup
Gene therapy of the human retina wikipedia , lookup
Designer baby wikipedia , lookup
Artificial gene synthesis wikipedia , lookup
Epigenetics of diabetes Type 2 wikipedia , lookup
Microevolution wikipedia , lookup
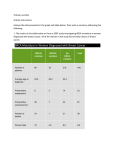
Genetic analysis of a congenital nephrogenic diabetes insipidus pedigree SHEN Yun-feng*1, LAI Xiao-yang1, XIAO Xin-lan2, LI Jing1, YU Rong1, GAO Hui1 and ZHANG Mei-ying1. 1 Department of Endocrinology and Metabolism, The second affiliated hospital of Nanchang university, Nanchang, Jiangxi 330006, China (Shen YF, Lai XY, Li J, Yu R, Gao H, Zhang MY) 2 Department of Magnetic Resonance Imaging, The second affiliated hospital of Nanchang university, Nanchang, Jiangxi 330006, China (Xiao XL) *Correspondence to: SHEN Yun-feng, Department of Endocrinology and Metabolism, the second affiliated hospital of Nanchang university, Nanchang, Jiangxi 330006, China (Tel: 86-791-86296440, 86-791-86296440, E-mail: [email protected]) Words: Abstract 217 Table: 2 Figure: 3 Text 1815 Fax: Abstract Background: As a X-linked recessive way, AVPR2 gene mutation resulted in a hereditary disease -- congenital nephrogenic diabetes insipidus (CNDI). We found a suspect clinical CNDI pedigree. In order to identify the genetic etiology, we performed the genetic analysis. Methods: The clinical features of the proband and his family members were recorded. The laboratory tests and imaging inspections were analyzed. The water deprivation and pituitrin loading test were performed in the proband and his brother. The genomic DNA of all the members of the pedigree were extracted and then PCR amplification on arginine vasopressin receptor 2 (AVPR2) gene were carried out. Sequencing in both directions was performed to identify mutation on AVPR2 gene. Results: Both the proband and his brother were diagnosed CNDI, meanwhile the other members of this pedigree was normal. No severe biochemical abnormality were found in the two CNDI patients. Both the patients had moderate urinary retention, severe megaloureter and hydronephrosis, and mild renal insufficiency. Two mutations of AVPR2 gene were discovered in the 3rd exon in the patients, a silent mutation L309L and a nonsense mutation R337X. The AVPR2 gene R337X mutation was co-segregated with CNDI. R337X mutation was not a reported mutation in Chinese Mainland. Conclusion: The AVPR2 gene R337X mutation was also a genetic etiology of CNDI patients in Chinese Mainland. [Key words] diabetes insipidus, nephrogeic; receptors, vasopressin; gene; mutation; Water homeostasis is partly maintained by the action of the antidiuretic hormone arginine vasopressin (AVP) on the collecting tubules of the kidney. Secreted by supraoptic nucleus and paraventricular nucleus in hypothalamus, and released from the posterior pituitary, AVP mediates its antidiuretic effect by binding to the AVP receptor 2 (AVPR2) on the basolateral surface of the principal cells. Congenital nephrogenic diabetes insipidus (CNDI) was a rare hereditary disease, which caused by AVPR2 or aquaporin (AQP)-2 gene mutation. AVPR2 gene mutation, showed as X-linked recessive inheritance, caused almost 90% of CNDI.1 AQP2 gene mutation showed as autosomal recessive or autosomal dominant inheritance, but only resulted in 10% of CNDI.1 AVPR2 gene encodes a 371 amino acid G protein-coupled receptor, and consist of 3 exons.2,3 After AVP binds with AVPR2, the AVP-AVPR2 complex activates Gs/adenylate cyclase which increases intracellular cyclic adenosine monophosphate (cAMP).4,5 This initiates a phosphorylation cascade that promotes translocation of the water channel, AQP2, to the apical membranes of the renal tubules.6 Mutations of the AVPR2 gene result in impaired ability to concentrate the urine causing polyuria and maybe mental and/or growth retardation.7 To date, over 200 mutations in the AVPR2 gene in over 300 families have been identified, yielding approximately 56% missense mutations, 27% small deletions/insertions, 9% non-sense mutations and 8% large or complex deletions.1,8-10 Here, we reported a pedigree with congenital X-linked nephrogenic diabetes insipidus. A nonsense mutation (R337X) in the 3rd exon of the AVPR2 gene was found in the proband and the R337X mutation co-segregated with the CNDI in this pedigree. METHODS Subjects The 33-year-old male proband went into our outpatient clinic and complained persistent polydipsia and polyuria from his infancy. Because his urine special gravity (USG) was very low, diabetes insipidus was suspected. Then, he was hospitalized and 24 h urine volume was calculated. Next, complete physical examination, laboratory tests and instrument inspections were done. Water deprivation and pituitrin loading test was performed for differentiating central diabetes insipidus and nephrogenic diabetes insipidus. All tests were also done in the proband’s brother because he had the same symptoms as the proband. Urine routine were tested in the proband’s parents, wife and daughter. Informed consent was obtained from all the family members. The studies were performed according to the Declaration of Helsinki as revised in 2000 and approved by the corresponding ethical committees. Identification of arginine vasopressin receptor 2 (AVPR2) gene mutation by direct sequencing Peripheral whole blood of all members in this pedigree was drawn to sequence the AVPR2 gene. Genomic DNA was extracted from peripheral lymphocytes using a DNA extraction kit (Qiagen, Duesseldorf, Germany). The coding regions of exons 1-3 and the intron-exon boundaries of the AVPR2 gene were amplified by PCR, and primers were shown in Table 1. Due to over 1600 bp in exon 3, the exon 3 was divided into 3a, 3b, 3c, 3d for PCR amplification. PCR products were purified using QIAquick PCR purification columns (Qiagen, Duesseldorf, Germany), and both strands were sequenced using a BigDye terminator cycle sequencing kit (Applied Biosystems, Warrington, UK) according to the manufacturer’s recommendations. Reactions were analyzed on an ABI 3100 DNA sequencer (Applied Biosystems, Warringtion, UK). As controls, the AVPR2 gene of one hundred unrelated healthy individuals were also sequenced. RESULTS Clinical profiles of this pedigree Twenty-four hours urine volume was 11~12 L/24 h in the proband. Urine routine test showed that USG was 1.002 and negative sugar. No abnormalities were found in plasma glucose, blood routine, glutamic-alanine transaminase, glutamic-oxaloacetic transaminase, serum electrolyte and plasma osmotic pressure, but the serum urine nitrogen (8.7 mmol/L) and serum creatinine (156.1 μmol/L) were mildly elevated. Magnetic resonance imaging (MRI) of the pituitary showed T1 high signal disappeared, but T2 signal was normal. Magnetic resonance hydrography of the urinary system showed bilateral megaloureter and hydronephrosis (Figure 1). Ultrasonic inspection showed urinary retention (residual urine in bladder more than 300 ml). As listed in Table 2, the water deprivation and pituitrin loading test were negative, which indicated the central diabetes insipidus and psychogenic polydipsia were excluded, and then the CNDI was diagnosed. After 5 days given hydrochlorothiazide and amiloride, 24 h urine volume of the proband was reduced to 4.5~5 L. As shown in Figure 2, the proband’s brother was also diagnosed CNDI because of same symptoms and inspection results. Other members in this pedigree had normal USG and urine volume, and diabetes insipidus was excluded. Identification of a non-sense and a silent mutation in AVPR2 gene The 3 exons of AVPR2 gene were scanned for mutations using direct sequencing. As shown in Figure 3, two homozygous mutations (the 1008th base A→G and the 1090th base C→T) were found in the 3rd exon of AVPR2 gene in the proband and his brother. The 1008th base A→G suggested a silent mutation L309L (CTA→CTG). The 1090th base C→T suggested a termination codon TGA replaced original arginine codon CGA, which resulted in R337X non-sense mutation. Hemizygous R337X mutation were found in the proband’s mother and daughter. R337X mutation was co-segregated with CNDI (Figure 2). However, R337X mutation was not found in the 100 unrelated healthy individuals used as controls. DISCUSSION In this study, two patients with polydipsia, polyuria from their infancy were diagnosed CNDI, and a X-linked recessive inherent CNDI pedigree was found. Further AVPR2 gene analysis showed that the 1090th base C→T resulted in R337X nonsense mutation, which was not a reported mutaion in Chinese Mainland. The R337X nonsense mutation co-segregated with the CNDI. CNDI patients were usually found in the infancy due to persistent polyuria, frequent fever, severe dehydration, electrolyte imbalance, delayed growth, and mental retardation, which was firstly described by McIlraith in 1892. Mental retardation has long been considered an important complication of untreated NDI and assumed to be a sequel of recurrent episodes of severe brain dehydration and cerebral edema caused by overzealous attempts at rehydration.11 With breast milk feedings, infants usually thrive and do not develop signs of dehydration, because human milk has a low salt and protein content, and therefore a low renal osmolar load.12 Hence, some patients were delayed to diagnosis in their adults. In the present study, the 33-year-old proband and his brother had the characteristics of congenital diabetes insipidus such as persistent polyuria, repeat fever from their infancy. The proband’s mother and daughter had negative clinical manifestation. The congenital diabetes insipidus in this family showed X-linked recessive inheritance. Like reported in other studies, persistent polyuria in the proband and his brother resulted in the development of urinary retention, hydroureter, hydronephrosis, and mild renal insufficiency.13,14 Sometimes, in some patients, large-capacity hypotonic bladder dysfunction might require clean intermittent catheterization. Adult CNDI patients should be trained to void regularly on behalf of assuring that the maximal urinary bladder capacity remains within normal range. In the present study, a silent mutation L309L and another nonsense mutation R337X in AVPR2 gene were discovered. Among all of AVPR2 mutations, L309L is the most common polymorphism, with a global distribution, as it can be found in different ethnical groups, starting from South-, Central- and North-Americans, continuing through Europeans/Caucasians to Asians, Middle-Easterners and Africans.1 R337X was also a reported mutation,2,4,15,16 but as far as we know, it had not been documented in the mainland of China. In this study, R337X was homozygous in the proband and his brother, and was hemizygous in the proband’s mother and daughter. The R337X nonsense mutation co-segregated with the CNDI in this pedigree. Usually, defects in the AVPR2 gene have been classified as the following: (a) type-1 mutant receptors, which reach the cell surface but display impaired ligand binding and are unable to induce normal cAMP production;17 (b) type-2 mutant receptors with defective intracellular transport that can not reach the cell surface and are trapped in the interior of the cell;8,18,19 (c) type-3 mutant receptors which are inappropriately transcribed, leading to unstable mRNA, which is rapidly degraded. 20 Most of the AVPR2 mutations lead to type-2 mutant receptors.20 The non-sense mutation R337X found in this pedigree was previously characterized and resulted in formation of a truncated AVPR2 which showed significantly decreased cell surface expression and significantly reduced functionality.21-23 Moreover, Morello J. and his colleagues reported this truncated receptor was retained in the endoplasmic reticulum and never reached the Golgi compartment, which indicating that mis-folding provoked by the mutation did not allow the receptor protein to escape the endoplasmic reticulum quality control system.24 Hydrochlorothiazide, amiloride and indomethacin were typical drugs which often used to treat CNDI.25-27 Recently, aminoglycoside pretreatment was reported partially restored the function of truncated R337X V2 vasopressin receptors.28 In addition, other studies also discovered some high-affinity non-peptide compounds or pharmacological chaperones could promote maturation and membrane rescue of L44P, A294P, and R337X CNDI mutants and restore a functional AVP-dependent cAMP signal.8,29 In conclusion, we found a CNDI pedigree with AVPR2 gene R337X nonsense mutation. As far as we knew, it was the first reported in the CNDI patients of Chinese Mainland. The R337X mutation was also a genetic etiology of CNDI patients in Chinese Mainland. Identifying variations in AVPR2 in CNDI patients and confirming their functional significance are important for accurate genetic counseling. In the near future, some new drugs may be developed to treat CNDI. REFERENCES 1. Spanakis E, Milord E, Gragnoli C. AVPR2 variants and mutations in nephrogenic diabetes insipidus: review and missense mutation significance. J Cell Physiol 2008; 217: 605-617. PMID: 18726898. 2. Chen CH, Chen WY, Liu HL, Liu TT, Tsou AP, Lin CY, et al. Identification of mutations in the arginine vasopressin receptor 2 gene causing nephrogenic diabetes insipidus in Chinese patients. J Hum Genet 2002; 47: 66-73. PMID: 11916004. 3. Seibold A, Brabet P, Rosenthal W, Birnbaumer M. Structure and chromosomal localization of the human antidiuretic hormone receptor gene. Am J Hum Genet 1992; 51: 1078-1083. PMID: 1415251. 4. Boson WL, Della Manna T, Damiani D, Miranda DM, Gadelha MR, Liberman B, et al. Novel vasopressin type 2 (AVPR2) gene mutations in Brazilian nephrogenic diabetes insipidus patients. Genet Test 2006; 10: 157-162. PMID: 17020465. 5. Morello JP, Bichet DG. Nephrogenic diabetes insipidus. Annu Rev Physiol 2001; 63: 607-630. PMID: 11181969. 6. Sadeghi H, Robertson GL, Bichet DG, Innamorati G, Birnbaumer M. Biochemical basis of partial nephrogenic diabetes insipidus phenotypes. Mol Endocrinol 1997; 11: 1806-1813. PMID: 9369448. 7. Bichet DG, Turner M, Morin D. Vasopressin receptor mutations causing nephrogenic diabetes insipidus. Pro Assoc Am Physicians 1998; 110: 387-394. PMID: 9756088. 8. Böselt I, Tramma D, Kalamitsou S, Niemeyer T, Nykänen P, Gräf KJ, et al. Functional characterization of novel loss-of-function mutations in the vasopressin type 2 receptor gene causing nephrogenic diabetes insipidus. Nephrol Dial Transplant 2012; 27: 1521-1528. PMID: 21917732. 9. Schöneberg T, Schulz A, Biebermann H, Hermsdorf T, Römpler H, Sangkuhl K. Mutant G-protein-coupled receptors as a cause of human disease. Pharmacol Ther 2004; 104: 173-206. PMID: 15556674. 10. Böselt I, Römpler H, Hermsdorf T, Thor D, Busch w, Schulz A, et al. Involvement of the V2 vasopressin receptor in adaptation to limited water supply. PLoS One 2009; 4: e5573. PMID: 19440390. 11. Forssman H. Is hereditary diabetes insipidus of nephrogenic type associated with mental deficiency? Acta Psychiatr Neuro Scand 1955; 30: 577-587. PMID: 13301914. 12. Wesche D, Deen PMT, Knoers NVAM. Congenital nephrogenic diabetes insipidus: the current state of affairs. Pediatr Nephrol 2012; 27: 2183-2204. PMID:22427315. 13. Nakada T, Miyauchi T, Sumiya H, Shimazaki J. Nonobstructive urinary tract dilation in nephrogenic diabetes insipidus. Int Urol Nephrol 1990; 22: 419–427. PMID: 2076930. 14. Uribarri J, Kaskas M. Hereditary nephrogenic diabetes insipidus and bilateral nonobstructive hydronephrosis. Nephron 1993; 65: 346–349. PMID: 8289981. 15. Bichet DG, Birnbaumer M, Lonergan M, et al. Nature and recurrence of AVPR2 mutations in X-linked nephrogenic diabetes insipidus. Am J Hum Genet 1994; 55: 278-286. PMID: 8037205. 16. Van Lieburg AF, Knoers NVAM, Monnens LAH. Clinical presentation and follow-up of 30 patients with congenital nephrogenic diabetes insipidus. J Am Soc Nephrol 1999; 10: 1958-1964. PMID: 10477148. 17. Rosenthal W, Antaramian A, Gilbert S, Birnbaumer M. Nephrogenic diabetes insipidus: a V2 vasopressin receptor unable to stimulate adenylyl cyclase. J Biol Chem 1993; 268: 13030-13033. PMID:8514744. 18. Moon S, Kim J, Shim J, Lim DJ, Cha BY, Han JH. Analysis of a novel AVPR2 mutation in a family with nephrogenic diabetes insipidus. Int J Clin Exp Med 2011; 4: 1-9. PMID: 21394280. 19. Takahashi K, Makita N, Manaka K, Hisano M, Akioka Y, Miura K, et al. V2 vasopressin receptor (V2R) mutations in partial nephrogenic diabetes insipidus highlight protean agonism of V2R antagonists. J Biol Chem 2012; 287: 2099-2106. PMID: 22144672. 20. Fujiwara TM, Bichet DG. Molecular biology of hereditary diabetes insipidus. J Am Soc Nephrol 2005; 16: 2836-2846. PMID: 16093448. 21. Oksche A, Dehe M, Schülein R, Wiesner B, Rosenthal W. Folding and cell surface expression of the vasopressin V2 receptor: requirement of the intracellular C-terminus. FEBS Lett 1998; 424: 57-62. PMID: 9537515. 22. Wenkert D, Schoneberg T, Merendino JJ Jr, Rodriguez Pena MS, Vinitsky R, Goldsmith PK, et al. Functional characterization of five V2 vasopressin receptor gene mutations. Mol Cell Endocrinol 1996; 124: 43-50. PMID: 9027323. 23. Sadeghi HM, Innamorati G, Birnbaumer M. An X-linked NDI mutation reveals a requirement for cell surface V2R expression. Mol Endocrinol 1997; 11: 706-713. PMID: 9171234. 24. Morello JP, Salahpour A, Petäjä-Repo UE, Laperrière A, Lonergan M, Arthus MF, et al. Association of calnexin with wild type and mutant AVPR2 that cause nephrogenic diabetes insipidus. Biochemistry 2001; 40: 6766-6775. PMID: 11389590. 25. Kirchlechner V, Koller DY, Seidl R, Waldhauser F. Treatment of nephrogenic diabetes insipidus with hydrochlorothiazide and amiloride. Arch Dis Child 1999; 80: 548-552. PMID: 10332005. 26. Knoers N, Monnenes LA. Amiloride-hydrochlorothiazide versus indomethacin-hydrochlorothiazide in the treatment of nephrogenic diabetes insipidus. J Pediatr 1990; 117: 499-502. PMID: 2391611. 27. Kortenoeven MLA, Li Y, Shaw S, Gaeggeler HP, Rossier BC, Wetzels JF, et al. Amiloride blocks lithium entry through the sodium channel thereby attenuating the resultant nephrogenic diabetes insipidus. Kidney Int 2009; 76: 44-53. PMID: 19367330. 28. Schulz A, Sangkuhl K, Lennert T, Wigger M, Price DA, Nuuja A, et al. Aminoglycoside pretreatment partially restores the function of truncated V2 vasopressin receptors found in patients with nephrogenic diabetes insipidus. J Clin Endocrinol Metab 2002; 87: 5247-5257. PMID: 12414899. 29. Jean-Alphonse F, Perkovska S, Frantz M, Durroux T, Méjean C, Morin D, et al. Biased agonist pharmacochaperones of the AVP V2 receptor may treat congenital nephrogenic diabetes insipidus. J Am Soc Nephrol 2009; 20: 2190-2203. PMID: 9729439. Table Table 1 Primers in 3 exons of AVPR2 gene Exons Forward Primer Reverse Primer Exon1 ACCTTGGCACTCACAGAGCCCTTTC CTAGGGCGAGGAATCCATGCTAA Exon2 GCCACCTTCACGCCACCGCCCAGCT TTCCCTGAATCGTCAAACCCACTCT Exon3a TCTAACCAGGCCCTCTTCCCGACTC CACGAACACCATCAGGGCAATCC Exon3b CGTCGCACCTATGTCACCTGGATT TGAGGACACGCTGCTGCTGAAAGAT Exon3c CTGAACCCAACCTAGATCCTCCACC GGGAGGGATTAGAAAGGCGGAGA Exon3d GAGGAGTGGCAGGAAAGAGGGAGCAG CAGGTGGGTGCTGGAGGTGAGAA Table 2 Time Water deprivation and vasopressin test Urine Volume (h) USG (ml) Plasma Osmolality (mOsm/L) Body Weight (Kg) 1 460 1.002 297.56 48.7 2 450 1.002 298.23 48.2 3 480 1.002 296.95 47.8 4 450 1.002 296.48 47.3 5 470 1.002 298.72 46.9 6 460 1.002 293.66 46.4 7 440 1.002 295.28 45.8 8 450 1.002 294.91 45.2 Note: 5 U vasopressin subcutaneously injected in the beginning of the 7th hour. Legend Figure 1. The Magnetic Resonance Imaging Feature of the Proband. A-D: The MRI of pituitary. A/B showed T1 high signal disappeared, C/D showed T2 signal were normal. E-F: The magnetic resonance hydrography of urinary system showed megaloureter, hydronephrosis and megacystis. Figure 2. The CNDI pedigree with AVPR2 gene mutation. The CNDI with X-linked recessive inheritance was segregated with R337X mutation. Black: the CNDI patients with homozygous R337X mutation and clinical symptoms. Gray: the individuals with heterozygous R337X mutation but no clinical symptoms. White: no clinical and genetic abnormality. Figure 3. The sequencing of the 3rd exon in AVPR2 gene. A: forward sequencing, the 1008th base A was substitute of G which suggested a silent mutation L309L. B: reverse sequencing in the 1008th base. C/D: Normal forward and reverse sequencing in the 1090th base. D: Normal reverse sequencing in R337. E: forward sequencing, the 1090th base C was substitute of T which suggested a non-sense mutation R337X. F: reverse sequencing in the 1090th base. Figure 1 Ⅰ Ⅱ Ⅲ Figure 2 A T G C Figure 3