* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Invulnerability of retinal ganglion cells to NMDA excitotoxicity
Survey
Document related concepts
Neuroanatomy wikipedia , lookup
Endocannabinoid system wikipedia , lookup
Multielectrode array wikipedia , lookup
Optogenetics wikipedia , lookup
Development of the nervous system wikipedia , lookup
Subventricular zone wikipedia , lookup
Long-term depression wikipedia , lookup
Signal transduction wikipedia , lookup
Chemical synapse wikipedia , lookup
Stimulus (physiology) wikipedia , lookup
Feature detection (nervous system) wikipedia , lookup
Neuropsychopharmacology wikipedia , lookup
Glutamate receptor wikipedia , lookup
Synaptogenesis wikipedia , lookup
Molecular neuroscience wikipedia , lookup
Channelrhodopsin wikipedia , lookup
Transcript
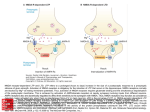
www.elsevier.com/locate/ymcne Mol. Cell. Neurosci. 26 (2004) 544 – 557 Invulnerability of retinal ganglion cells to NMDA excitotoxicity E.M. Ullian, a,*,1 W.B. Barkis, a,1 S. Chen, b J.S. Diamond, b and B.A. Barres a a b Department of Neurobiology, Stanford University School of Medicine, Stanford, CA 94305-5125, USA NIH/NINDS/SPU, Bethesda, MD 20892-4066, USA Received 15 August 2003; revised 22 March 2004; accepted 10 May 2004 NMDA excitotoxicity has been proposed to mediate the death of retinal ganglion cells (RGCs) in glaucoma and ischemia. Here, we reexamine the effects of glutamate and NMDA on rat RGCs in vitro and in situ. We show that highly purified RGCs express NR1 and NR2 receptor subunits by Western blotting and immunostaining, and functional NMDA receptor channels by whole-cell patch-clamp recording. Nevertheless, high concentrations of glutamate or NMDA failed to induce the death of purified RGCs, even after prolonged exposure for 24 h. RGCs co-cultured together with ephrins, astrocytes, or mixed retinal cells were similarly invulnerable to glutamate and NMDA, though their NMDA currents were 4-fold larger. In contrast, even a short exposure to glutamate or NMDA induced the rapid and profound excitotoxic death of most hippocampal neurons in culture. To determine whether RGCs in an intact retina are vulnerable to excitotoxicity, we retrogradely labeled RGCs in vivo using fluorogold and exposed acutely isolated intact retinas to high concentrations of glutamate or NMDA. This produced a substantial and rapid loss of amacrine cells; however, RGCs were not affected. Nonetheless, RGCs expressed NMDA currents in situ that were larger than those reported for amacrine cells. Interestingly, the NMDA receptors expressed by RGCs were extrasynaptically localized both in vitro and in situ. These results indicate that RGCs in vitro and in situ are relatively invulnerable to glutamate and NMDA excitotoxicity compared to amacrine cells, and indicate that important, as yet unidentified, determinants downstream of NMDA receptors control vulnerability to excitotoxicity. D 2004 Elsevier Inc. All rights reserved. Introduction Although glutamate is the major excitatory neurotransmitter in the CNS, it is sometimes able to kill neurons (Choi, 1992; Rothman and Olney, 1987). Excitotoxic neuronal death is thought to be an important contributor to neuron death caused by brain and spinal cord injuries as well as by many neurological diseases. An unsolved mystery, however, is why only some types of neurons are * Corresponding author. Department of Neurobiology, Stanford University School of Medicine, Fairchild Science Building D235, 299 Campus Drive, Stanford, CA 94305-5125. Fax: +1-650-725-3958. E-mail address: [email protected] (E.M. Ullian). 1 These authors contributed equally to this paper. Available online on ScienceDirect (www.sciencedirect.com.) 1044-7431/$ - see front matter D 2004 Elsevier Inc. All rights reserved. doi:10.1016/j.mcn.2004.05.002 vulnerable to glutamate excitotoxicity. The ionotropic glutamate receptors are ligand-gated ion channels that are grouped into three pharmacologically defined classes: NMDA, AMPA, and kainate receptors. These receptors are encoded by at least six gene families: a single family for AMPA receptors (GluR1, 2, 3, 4), two for kainate (GluR5, 6, 7 and KA1, 2), and three for NMDA (NR1, NR2A, B, C, D, and NR3A, B) (Dingledine et al., 1999). These subunits combine into multimeric complexes to form functional receptor channels. To form an NMDA receptor, for instance, two NR1 subunits must combine with at least two NR2 subunits. NMDA receptors have been linked to excitotoxic death that occurs in less than 1 h of exposure, whereas much longer exposures to kainate or AMPA produce excitotoxicity (Choi, 1992). We have focused on the effects of glutamate on retinal ganglion cells (RGCs) in the developing rat retina. RGC death is a leading cause of blindness resulting from glaucoma and retinal ischemia, and NMDA receptor-mediated excitotoxicity is presently thought to be an important contributor to RGC death in these conditions (Ritch, 2000; Wax and Tezel, 2002). The expression of glutamate receptors by retinal ganglion cells in developing and adult rats has been extensively studied. Based on in situ hybridization and immunohistochemical studies of rat retinal sections, RGCs have been shown to express NMDA, AMPA, and kainate receptors including NR1, NR2A, B, C, D, GluR2, GluR7, and KA2 (Brandstatter et al., 1994; Grunder et al., 2000a,b; Watanabe et al., 1994). Electrophysiological recordings of rat retinal ganglion cells in situ clearly indicate that they express functional NMDA and non-NMDA receptor-activated channels (Chen and Diamond, 2002). NMDA, AMPA, and kainate-activated currents can all be observed in RGCs in mixed retinal cultures over the 1day period in which these cells remained viable without added neurotrophic support (Aizenman et al., 1988; Taschenberger et al., 1995). In vitro and in vivo, rodent RGCs have been repetitively shown to be vulnerable to NMDA-mediated excitotoxicity (reviewed by Lipton, 2001; Sucher et al., 1997). For instance, both glutamate and NMDA induce the death of RGCs in postnatal and adult retinas (Izumi et al., 1995; Li et al., 1999; Mosinger et al., 1991; Sabel et al., 1995). Although kainate-elicited excitotoxicity of RGCs in culture has not generally been observed, one group reported that kainate killed rat RGCs in purified cultures (Otori et al., 1998); however, kainate-induced excitotoxicity in intact retinas appears to be mediated by release of glutamate which then activates NMDA receptors (Lipton, 2001; Sucher et al., 1997). Taken together, these studies indicate that the postnatal E.M. Ullian et al. / Mol. Cell. Neurosci. 26 (2004) 544–557 and adult RGCs express functional NMDA and non-NMDA receptors, and are vulnerable to NMDA-mediated excitotoxicity. Because of their expected vulnerability to glutamate, we initially took measures to avoid exposing RGCs to glutamate in our studies involving their purification and culture (Barres et al., 1988). But eventually we were surprised to find that glutamate exposure actually enhanced the survival of purified RGCs in culture (Meyer-Franke et al., 1995). We found that depolarization enhanced RGC survival by enhancing neurotrophic responsiveness (Goldberg and Barres, 2000; Goldberg et al., 2002; Meyer-Franke et al., 1998; Shen et al., 1999), but we remained puzzled by the invulnerability of the purified RGCs to excitotoxicity. Here, we have investigated the glutamate and NMDA invulnerability of purified RGCs in vitro. By culturing highly purified RGCs in serum-free conditions, we have found that RGCs in vitro continue to express the same glutamate receptor subunits that they do in vivo, yet are invulnerable to glutamate and NMDA excitotoxicity. We also found that in vitro, as in situ (Chen and Diamond, 2002), NMDA receptors are localized extrasynaptically and not synaptically. To our surprise, we found that RGCs in intact developing and adult retinas are completely invulnerable to glutamate and NMDA excitotoxicity. Glutamate and NMDA did kill many cells in the inner nuclear layer (INL) and ganglion cell layer, but these cells were amacrine cells. Taken together, these studies cast doubt on the relevance of excitotoxicity to RGC death in glaucoma and retinal ischemia and strikingly illustrate that the presence of functional NMDA receptors is insufficient to account for excitotoxicity. Results Expression of NMDA receptor proteins by purified RGCs in culture As an initial survey of glutamate receptor subunit expression by RGCs in culture, we first examined mRNA extracted from purified RGCs after 3 days of culture by Affymetrix gene chip analysis and found that mRNAs for NR1, NR2, GluR2, and KA2 subunits, but not KA1 or other AMPA subunits, were expressed (data not shown) closely mirroring the previously determined RGC pattern of expression in vivo (Brandstatter et al., 1994; Grunder et al., 2000a,b). We had previously reported that RGCs in vitro express functional non-NMDA glutamate receptors that 545 are blocked by CNQX and that GluR2 specific antiserum stain synaptic puncta in RGC cultures (Pfrieger and Barres, 1997; Ullian et al., 2001), and that in situ, RGCs express GluR2 (J.S.D., unpublished observations). However, we had not yet examined their NMDA receptor protein expression. To determine whether NMDA receptor proteins were present, we examined extracts from purified P6 RGCs by Western blotting with subunit specific antibodies. NR1, NR2A, and NR2B were all easily detected in RGC extracts prepared after 3 (Fig. 1A) and 7 (data not shown) days in culture. To examine the localization of these proteins, we performed immunostaining on RGCs after 7 days in culture using NMDA receptor-specific antibodies. Bright immunoreactivity for the NR1, NR2A, and NR2B subunits was distributed throughout the soma and dendritic processes of all RGCs (Figs. 1B, C; labeling for NR2A is not shown but is identical to that shown for NR2B). We could not discern whether these subunits were concentrated at synapses because high levels of staining precluded detection of discrete synaptic puncta. These data indicate that purified RGCs continue to express NR1, NR2A, NR2B subunit proteins after 7 days of culture and appropriately target them to their dendrites. Expression of functional NMDA channels by purified RGCs in culture Although RGCs in vitro express the appropriate subunits to form NMDARs, we did not know if the receptors are actually functionally expressed by the neurons. To determine if RGCs express functional NMDARs, we performed whole-cell patchclamp recordings on purified P6 RGCs cultured for 7 days. In response to applied NMDA (100 AM), we recorded inward currents that were blocked by the NMDA antagonist APV (50 AM; Fig. 2A). On average, these currents were small, about 50 pA (Fig. 2C, N = 6 per condition). These findings demonstrate that purified RGCs do express functional NMDARs. We wondered how the size of NMDA currents in our RGC cultures would compare to those of hippocampal neurons in culture. We prepared hippocampal cultures from E18 hippocampus and after 2 – 3 weeks of culture and analyzed their currents by whole-cell patch clamping. In response to applied NMDA (100 AM), we once again recorded inward currents that were blocked by APV (Fig. 2B). On average, these currents were significantly larger than those we recorded from RGCs, averaging about 1396 F 177 pA (mean F SEM, n = 5). Fig. 1. Purified retinal ganglion cells express NMDA receptor proteins in vitro. (A) Western blots performed on samples harvested from purified P5 – P6 RGCs after 3 days in culture (DIC) show the presence of NR1, NR2A, and NR2B subunit proteins. (B, C) Immunocytochemistry affirms the presence of NR1 and NR2B subunit proteins in these cultures. Scale bar, 20 Am. 546 E.M. Ullian et al. / Mol. Cell. Neurosci. 26 (2004) 544–557 Fig. 2. RGCs in vitro have functional NMDA currents. RGCs and hippocampal neurons were cultured for 3 weeks in defined, serum-free conditions. Whole-cell patch-clamp recordings reveal that NMDA (100 AM) results in a sustained, APV (50 AM)sensitive currents in both RGCs (A) and hippocampal neurons (B). The average whole-cell current amplitudes are greater in hippocampal neurons compared to RGCs. Example of NMDA current trace from RGCs treated with control FC antibody (C) or ephrin (D) shows increased current amplitude in response to ephrin. RGC NMDA current amplitudes change with culture conditions (E). RGCs cultured under conditions that increase synapse formation such as with astrocytes (RGC + Astro) or with mixed retina (RGC + Mixed Retina) show an increase in NMDA current. Addition of ephrin (RGC + Eph) also increases current amplitude both in the presence of astrocytes (RGC + Eph + Astro) and in the absence of astrocytes (RGC + Eph; P < 0.001 Kruskal – Wallis ANOVA, N = 6 per condition). Effects of glutamate and its agonists on RGCs in vitro We next investigated whether RGCs exposed to plateau levels of glutamate or its receptor agonists would undergo excitotoxic death. We cultured purified P6 RGCs for 3 days and then exposed them to glutamate (500 AM), NMDA (500 AM, 10 mM), AMPA (500 AM), or kainate (KA; 500 AM) for 1 h at 37jC in 10% CO2. We then measured the percentage of cells surviving using a calcein AM/ethidium homodimer-1 live/dead assay as well as by visualizing cellular and nuclear morphology under Nomarski differential interference contrast (DIC) optics and DAPI fluorescence (Figs. 3A – F; see Experimental methods). Surprisingly, RGCs were not killed by glutamate or its agonists including NMDA and kainate (Figs. 3A – F, 4). Indeed, 100% of the purified RGCs survived after exposure to these agonists for 1 h (Fig. 4) or even after 1 week (data not shown). Because it has been found that in some cases excitotoxicity is enhanced at low cell density (Tezel et al., 1999), in the presence of serum (Erdo et al., 1990), in the presence of chronic depolarization (Ha et al., 2002) or high levels of extracellular calcium (Hahn et al., 1988), or after ageing in culture for several weeks (Choi, 1992), we repeated these studies culturing the RGCs at low density (500 cells/cm2), in serum-containing media, in high concentrations of K+ (40 mM) or Ca2+ (10 mM), or for 2 weeks of maturation before glutamate agonist exposure or when RGCs were acutely platted into excitatory amino acids. In all cases, greater than 90% of the RGCs survived upon exposure to glutamate, kainate, or NMDA, compared with control RGC cultures lacking glutamate or its agonists. Thus, despite expression of functional NMDA and non-NMDA glutamate currents, purified RGCs in culture are invulnerable to glutamate and NMDA-mediated excitotoxicity. In contrast to these results, it has been reported that even a 5-min exposure to NMDA (200 AM) or glutamate (500 AM) produces widespread excitotoxic death in cultured cortical, hippocampal, and spinal neurons (Buisson et al., 1996; Choi, 1985). In particular, cultured hippocampal neurons are reported to be extremely vulnerable to NMDA-mediated excitotoxicity. (Peterson et al., 1989). Thus, to directly compare the effects of NMDA on RGCs and hippocampal neurons, to provide a positive control that our agonists were active and that we could elicit and detect excitotoxicity, we next applied NMDA to hippocampal neurons in culture at the same concentration (10 mM) and exposure time (1 h at 37jC in 10% CO2) used for the RGCs. In contrast to RGCs, virtually all of the hippocampal neurons were rapidly destroyed by NMDA exposure as assayed by the fluorescent live/dead assay (Figs. 3I, L) and by visualizing cellular and nuclear morphology under DIC optics and DAPI fluorescence (Figs. 3G – H, J – K). These results show that, as expected, cultured hippocampal neurons are highly vulnerable to NMDA-mediated excitotoxicity whereas cultured RGCs are not. Effects of ephrins, astrocytes, and synapse formation on RGC excitotoxicity One obvious difference between RGCs and hippocampal neurons is that the RGCs have far smaller NMDA currents. Ephrin signaling significantly increases NMDAR-dependent calcium influx into cultured cortical neurons (Dalva et al., 2000; Takasu et al., 2002). Because NMDA-induced calcium influx is thought to contribute to its excitotoxicity to RGCs (Hahn et al., 1988) and RGCs are well described to express ephrin receptors, we examined whether ephrin stimulation would increase NMDA currents in RGCs. We clustered ephrinB1 and ephrinB2 using antihuman Fc (50 ng/ml) at 500 ng/ml and activated the Eph receptors on RGCs with these clustered, multimeric ligands (Dalva et al., 2000; see Experimental methods). We found that ephrin treatment induced a 4-fold increase in NMDA currents in RGCs (Figs. 2C – E). This increase was not accounted for by a change in synapse number per RGC, which was not affected by ephrin (average number of E.M. Ullian et al. / Mol. Cell. Neurosci. 26 (2004) 544–557 547 Fig. 3. Purified retinal ganglion cells, but not hippocampal neurons, are invulnerable to NMDA-mediated excitotoxicity in culture. Purified RGCs (A – F) and hippocampal neurons (G – L) were cultured for 3 weeks in defined, serum-free conditions and were then treated for 1 h with NMDA (10 mM) (D – F; J – L) or control Neurobasal-Sato (A – C; G – I). Side-by-side Nomarski and DAPI-labeled fluorescent microscopy reveal the cellular and nuclear morphology of healthy RGCs in both control (A and B) and NMDA-treated (10 mM) (D and E) cultures. Additionally, the fluorescent live/dead assay of calcein AM (live cells; green) and ethidium homodimer-1 (dead cells, nuclear label; red) affirms the lack of RGC death in the same control (C) and NMDA-treated (F) cultures. In contrast, panels G – I show healthy hippocampal neurons in the control condition, while J – L show dead hippocampal neurons treated with NMDA (10 mM). Scale bars, 20 Am (A, B, D, E, G, H, J, K), 50 Am (C, F, I, L), N = 27 fields. synapses 6 F 1 synapses per cell with eprhin or control, N = 6). Despite the increased NMDA currents, however, the RGCs remained invulnerable to NMDA excitotoxicity (control survival 100 F 3%, NMDA 102 F 3%, GLUT 98 F 3%; P = 0.63, N = 46 fields per condition). Another obvious difference between the RGC and hippocampal cultures was that few synapses are present in our purified RGC cultures (Ullian et al., 2001), whereas many synapses are present in the hippocampal cultures which contain astrocytes. To determine if synapse number or astrocytes affect the levels of NMDA currents or the vulnerability of RGCs to NMDA, we increased the levels of synapse formation in RGCs by co-culturing purified, retrogradely labeled RGCs with a feeding layer of astrocytes. RGCs exposed to astrocytes have nearly 50 synapses per neuron, which is about 7fold more synapses than RGCs not exposed to astrocytes (Nagler et al., 2001; Ullian et al., 2001). Co-culture with astrocytes significantly enhanced the average NMDA receptor currents in RGCs by almost 3-fold (Fig. 2C). Despite their increased NMDA currents and synapse number, RGCs co-cultured with astrocytes were still invulnerable to NMDA-mediated excitotoxicity (control survival 100 F 2%; NMDA 99 F 2%; P = 0.782 by paired t test). These results indicate that synapse number does not affect RGC vulnerability to excitotoxicity in vitro. Finally, another difference between the RGC and hippocampal neuronal cultures is that multiple types of neurons are present in the hippocampal but not the purified RGC cultures. To test if other 548 E.M. Ullian et al. / Mol. Cell. Neurosci. 26 (2004) 544–557 in the mixed retinal cultures. After 7 days, the cultures were exposed to glutamate (500 AM) or NMDA (500 AM) for 1 h at 37jC. Once again, the RGCs were invulnerable to NMDA-mediated excitotoxicity (control survival 100 F 2%, NMDA 105 F 1%). Taken together, these results indicate that increasing synapse number, adding other retinal cell types, and enhancing the size of NMDA currents are all insufficient to enhance RGC vulnerability to glutamate or NMDA. Localization of NMDARs Fig. 4. Quantification of glutamate-mediated excitotoxicity in purified RGCs in culture. Graph of the percent of RGC survival determined by an MTT assay after 1-h exposure to glutamate (500 AM), NMDA (500 AM), AMPA (500 AM), and kainate (KA; 500 AM). No statistically significant difference was found among conditions (P = 0.202 by one-way ANOVA, N = 46 fields per condition). cells within the retina can induce RGC susceptibility to excitotoxicity, we cultured fluorogold retrogradely labeled RGCs with mixed retina (see Experimental methods). RGCs cultured with other neuronal types in mixed retinal cultures had a 4-fold increase in NMDA currents (Fig. 2C). To determine if RGCs had become susceptible to excitotoxicity, we next examined their vulnerability Another difference between RGCs and hippocampal neurons is that hippocampal neurons have both extrasynaptic and synaptic NMDARs (Sattler et al., 2000; Tovar and Westbrook, 1999) whereas RGCs in vivo have NMDA receptors primarily at extrasynaptic sites (Chen and Diamond, 2002; Taylor et al., 1995). To see if RGCs in vitro also express NMDARs at extrasynaptic sites, we recorded from RGCs cultured under lowdensity autaptic culture conditions where they are forced to form synapses onto themselves (Ullian et al., 2001). We used patch clamping to record spontaneous miniature postsynaptic currents (mEPSCs) from the autaptic RGCs cultured with astrocyte feeding layers. We found that all of the mEPSCs are sensitive to CNQX (Fig. 5A). We were unable to observe an NMDA-mediated component to the mEPSCs although we recorded under conditions that allow maximal activation of NMDARs by the synaptically released glutamate (Fig. 5A, 0 Mg2+ and 20 AM glycine). The mEPSCs decays were best fit by a single exponential with a fast Fig. 5. RGCs in vitro do not have an NMDA component to the spontaneous miniature currents (mEPSCs), but do have an NMDA component to the evoked response. (A) Spontaneous mEPSCs recorded in the presence of glycine (20 AM) and the absence of Mg2+. All events were blocked by CNQX (A, CNQX). (B) Average of mEPSCs taken from (A) is best fit by a single exponential of 1.1 ms time constant. No obvious slow component to the mEPSCs is present. (C). Evoked responses of the same cell recorded in (A) and (B) show a slow, APV-sensitive component to the evoked response. The slow component is insensitive to CNQX treatment (C). Similar results were found for all RGCs (N = 5). E.M. Ullian et al. / Mol. Cell. Neurosci. 26 (2004) 544–557 549 mediate a component of the EPSC indicating that the NMDARs expressed by RGCs in vitro are extrasynaptic (Chen and Diamond, 2002; Clark and Cull-Candy, 2002). Size of NMDA currents in RGCs in intact retinas Given the relatively small size of the NMDA currents that we observed in RGCs in vitro and their lack of vulnerability to excitotoxicity, we next investigated whether the reported vulnerability of RGCs in vivo might reflect the presence of larger NMDA currents in vivo. To examine the NMDA current in intact retina, we recorded from RGCs using whole-cell patch clamping in P21 retinal slices as previously described (Chen and Diamond, 2002). First, we determined the size of currents evoked by direct application of NMDA (100 AM) at a holding potential of +40 mV. The NMDA was puffed directly onto RGC dendrites in the inner plexiform layer. On average, this elicited a current of about 300 pA (Figs. 6A, C), surprisingly close to the average size of currents we recorded from RGCs in mixed retinal cultures. We also determined the size of NMDA currents induced by synaptic stimulations using whole-field illumination (Figs. 6B, C). The synaptic NMDA responses were on average about 200 pA (Fig. 6C). Thus, the NMDA currents elicited in RGCs in vitro and in situ are comparably small. Effects of glutamate and NMDA on RGC excitotoxicity in intact retinas Fig. 6. RGCs in retinal slices have an NMDA component to synaptic responses and small responses to applied NMDA. All experiments were performed at 35jC at a holding potential of +40 mV. (A) Responses to 100 AM NMDA puffed onto the IPL. Glycine (10 mM) and strychnine (10 AM) were included in the puff solution. (B) EPSCs evoked by full-field light stimuli. All experiments in (A) were performed in slices from P21 animals. (C) Summary of responses for the population of neurons (error bars indicate SEM, N = 8 puff, N = 10 light evoked). time constant (Fig. 5B, s = 1.1 F 0.17 ms, mean F SD, N = 5). This fast single-exponential time constant is consistent with the currents being mediated by AMPARs, but not also by NMDARs (Chen and Diamond, 2002; Gomperts et al., 2000; O’Brien et al., 1997; Taylor et al., 1995). In contrast to the spontaneous mEPSCs, evoked postsynaptic currents (EPSCs) in the autaptic RGCs showed both AMPA and NMDA components to the synaptic response. For instance, evoked current from the same neuron used to record the representative mEPSCs shown in Fig. 5B showed a slow decay component to the EPSC (Fig. 5C, Control). This slow component was eliminated by the NMDAR antagonist APV (Fig. 5C, APV) whereas only the fast component was eliminated by the AMPAR antagonist CNQX (Fig. 5C, CNQX). Thus, NMDARs do not mediate mEPSCs but do Because of the invulnerability of RGCs in vitro to excitotoxicity, but the similarity of RGC glutamate and NMDA responses in vitro and in situ, we decided to reexamine the vulnerability of RGCs in intact retinas to excitotoxicity. Rather than studying the effects of glutamate injection in vivo, we chose the intact isolated (ex vivo) rat retina (Izumi et al., 1995; Romano et al., 1998). This preparation offers important advantages in that glutamate (or agonist) levels can be retained at a stable high concentration without rapidly diffusing away as would occur in vivo, and furthermore allows analysis of excitotoxicity immediately after isolation of the retina so that glutamate receptor expression in the retinal cells matches that in vivo. It has been shown that the effects of glutamate excitotoxicity on the ex vivo retinas match those that occur after injection in vivo with extensive swelling and death of retinal cells in the inner nuclear layer and retinal ganglion cell layers. The RGC layer is composed of about equal numbers of RGCs and displaced amacrines (Linden and Esberard, 1987). Therefore, to ensure accurate identification of RGCs, we first retrogradely labeled the RGCs in P6 rats with fluorogold allowing us to selectively label greater than 99% of the RGCs (see Experimental methods). After 1 – 14 days, we sacrificed the pups, carefully dissected out their retinas, and immediately studied the effects of glutamate and NMDA on RGC survival in the intact retinas. We examined a large number of retinas over a large range of developmental ages. In a series of experiments, we examined the following age rats: P6 – P7 (25 retinas per condition), P10 (15 retinas per condition), P14 (5 retinas per condition), and P20 (10 retinas per condition). After carefully dissecting out the retinas, we immediately exposed them to either glutamate (500 AM or 10 mM) or NMDA (500 AM or 10 mM) in DPBS for 1 h at 37jC in 10% CO2. We then labeled the dead cells with propidium iodide, fixed the retinas, and finally either whole-mounted or sectioned the retinas for analysis (see Experimental Methods). 550 E.M. Ullian et al. / Mol. Cell. Neurosci. 26 (2004) 544–557 Fig. 7. Retinal ganglion cells are invulnerable to NMDA-mediated excitotoxicity in the intact retina. P20 retinas were dissected, immediately exposed to agonist, and then fixed and whole-mounted. RGCs retrogradely labeled with fluorogold appear in green; propidium iodide-labeled nuclei, dead cells appear in red. In the whole mounts, both control (A) or NMDA (10 mM) (C) conditions show healthy RGCs in the ganglion cell layer (GCL) with almost exclusive nondouble-labeling of fluorogold (green) and propidium iodide-labeled nuclei (red), indicating that the affected cells are not RGCs but displaced amacrine cells. Cross-sections of P7 retinas from control (B) and NMDA-treated (10 mM; D) retina further illustrate the absence of RGC death. In sectioned, NMDA-treated retinas (D), a significant number of the propidium iodide-labeled nuclei (arrows) are in the inner-half of the inner nuclear layer (INL), suggesting that the affected cells are amacrine cells. In (C), the affected displaced amacrine cells are swollen and have primarily PI-labeled cytoplasm, whereas in (D) the affected amacrine cells have PI-labeled nuclei indicating that they are dead. Scale bar, 20 Am (A, C), 30 Am (B, D). In every retina that we examined, exposure to NMDA (Fig. 7) or glutamate (data not shown) produced no excitotoxic RGC death, as evidenced by counting the number of green fluorogold-labeled RGCs in the ganglion cell layer (GCL) that co-localized with red propidium iodide labeling of nuclei in whole mount P5 – P20 retinas. For instance, in P20 retinas, NMDA incubation did not induce propidium iodide labeling of RGC nuclei (Figs. 7A, C). Rare sporadic cells showed labeled nuclei in both control and test retinas presumably due to injury incurred during the retinal dissection. Similarly, retinal sections of NMDA-treated P7 retinas (Figs. 7B, D) show a nearly complete absence of co-labeled RGCs and propidium iodide-labeled nuclei in the GCL. However, in the same retinas, significant cell death occurs within the inner half of the inner nuclear layer (INL) in NMDA-treated retinas (Fig. 7D), as indicated by bright propidium iodide labeling of amacrine nuclei, indicating that amacrine cells are highly vulnerable to NMDA-mediated excitotoxicity. In addition, within the GCL layer, many non-fluorogold labeled neurons underwent dramatic swelling in response to glutamate or NMDA exposure and became strongly labeled with propidium iodide that leaked into their cytoplasm. As our fluorogold labeling procedure labels at least 99% of RGCs (Barres et al., 1988), these PI-labeled cells in the GCL are displaced amacrine cells, which constitute 40 – 50% of cells in the GCL (Figs. 7C, D). These results were found for retinas of all ages tested from P5 to P20. These findings indicate that in both developing and mature intact retinas, RGCs are invulnerable to glutamate and NMDA excitotoxicity whereas amacrine cells are highly vulnerable. Discussion Purified RGCs express functional extrasynaptic NMDARs and NMDA current density is greatly enhanced by other cell types RGCs in mixed retinal cultures have previously been shown to express NMDA currents (Aizenman et al., 1988; Taschenberger et al., 1995), but we investigated whether highly purified RGCs in culture similarly expressed NMDA currents because of their invulnerability to NMDA excitotoxicity. The present findings show that purified RGCs express the NMDA receptor subunits NR1, NR2A, and NR2B, as measured by immunostaining and Western blotting, and that these subunits are assembled into functional NMDARs. We found that the size of the NMDA currents in RGCs was significantly increased by ephrin signaling, but that this did not induce NMDA excitotoxicity. The ability of ephrin signaling to enhance NMDA-dependent calcium influx in cortical neurons is E.M. Ullian et al. / Mol. Cell. Neurosci. 26 (2004) 544–557 thought to be mediated by a posttranslational modification by NMDAR tyrosine phosphorylation (Dalva et al., 2000; Takasu et al., 2002). In these previous studies, however, the effects of ephrin signaling on NMDA-induced current size were not examined. Such a modification could increase NMDA current either by increasing the number of NMDA receptors on a neuron’s surface, their probability of opening, or their open times. Any of these changes would explain the increase in NMDA-induced calcium current. In these earlier studies, the possibility was raised that the increase in calcium influx was accounted for by an increased number of synapses per neuron. Our results show, however, that ephrin signaling can profoundly increase NMDA-induced currents without altering synapse number. The NMDA currents in RGCs were also increased severalfold by cell – cell interactions, including astrocytes and mixed retinal cell types containing astrocytes and Muller glia. Because astrocytes increase the number of synapses per RGC by 7-fold (Ullian et al., 2001), the increase in NMDA current could represent an increase in surface NMDAR expression following synapse formation. Alternatively, ephrins secreted by astrocytes could enhance the RGC NMDA currents (Murai et al., 2003). These results provide evidence that NMDA-current amplitudes in RGCs can be strongly regulated by cell – cell signaling interactions. We also investigated the localization of the functional NMDA receptors in RGCs. In hippocampal neurons, NMDA receptors are found both synaptically and extrasynaptically (Tovar and Westbrook, 1999). We found that the NMDA receptors expressed by purified RGCs in culture were predominantly extrasynaptic, even in the presence of astrocytes, as has been previously found for RGCs in vivo (Chen and Diamond, 2002; Matsui et al., 1998, but see Fletcher et al., 2000). It is not known how localization of NMDA receptors is controlled. Because in our purified cultures, RGCs synapse upon each other, whereas in vivo cone bipolar neurons synapse upon RGCs, it is likely that RGCs play the dominant role in determining NMDAR localization by directing them to extrasynaptic sites. RGCs are invulnerable to glutamate and NMDA excitotoxicity, in vitro and in intact retinas, whereas amacrine cells are highly vulnerable We have been unable to induce acute glutamate or NMDAmediated excitotoxicity in RGCs in intact rat retinas or in vitro, even under conditions where the NMDA currents are relatively large. In contrast, we observed that many amacrine cells in the inner nuclear layer were rapidly and dramatically injured or killed by glutamate and NMDA and that displaced amacrine cells in the GCL became swollen. Amacrine cells are well reported to express NMDAR proteins and currents in the rodent retina (Brandstatter et al., 1994; Grunder et al., 2000a,b; Hartveit and Veruki, 1997; Matsui et al., 2001). These studies suggest that AII (rod) amacrine cells, cholinergic amacrine cells, and displaced amacrine cells in particular express NMDARs. Remarkably, despite the presence of NMDA currents in these subsets of amacrine cells, electrophysiological recordings reveal only small NMDA currents on average of about 50 pA at a +40 mV holding potential in response to applied NMDA or evoked excitation (Hartveit and Veruki, 1997; Matsui et al., 2001). The toxic effects of NMDA and glutamate on amacrines in the intact retinas were manifested after only 1 h of exposure, which was 551 the earliest time point we examined. It is likely that this damage may have occurred even within minutes of exposure to glutamate and NMDA, as occurs with hippocampal neurons. Thus, our findings show that RGCs are invulnerable to glutamate and NMDA excitotoxicity, whereas amacrine cells are highly vulnerable yet have smaller NMDA currents. In contrast, a large previous body of literature has reported that RGCs are highly vulnerable to glutamate and NMDA excitotoxicity in vitro (Caprioli et al., 1996; Dreyer et al., 1994; Kawasaki et al., 2000, 2002; Kitano et al., 1996; Otori et al., 1998; Sucher et al., 1991a,b) and in intact ex vivo retinas or in vivo (Izumi et al., 1995; Kido et al., 2000; Li et al., 1999; Lucas and Newhouse, 1957; Moncaster et al., 2002; Moore et al., 2001; Mosinger et al., 1991; Olney, 1969; Romano et al., 1998; Sabel et al., 1995; Silprandi et al., 1992; Sisk and Kuwabara, 1985; Sun et al., 2000; Vorwerk et al., 1996). How can the discrepancy between our findings and these previous studies be explained? Lucas and Newhouse (1957), Olney (1969), and Sisk and Kuwabara (1985) were the earliest investigators to report that glutamate and NMDA agonists produced a rapid and severe destruction of the inner retinal layers including the retinal ganglion cell layer. As nearly half of the cells in the rodent ganglion cell layer are displaced amacrine cells, these observations were consistent either with amacrine cells being primarily affected or with both amacrine and retinal ganglion cells being affected. Similarly, the majority of later studies investigating ex vivo and in vivo studies of retinal glutamate exposure concluding that RGCs were affected failed to take any measure to distinguish RGCs from displaced amacrine cells, for instance by retrograde labeling or antigenic identification. Thus, whereas all studies agree that many retinal cells in the INL and RGC layers are vulnerable to excitotoxicity, the difference between the present study and these previous studies may be more of a matter of mistaken previous interpretations that RGCs were among the affected cells. The present findings, however, reveal that it is amacrine cells and not RGCs that are subject to rapid glutamate and NMDA excitotoxicity in intact retinas and in vivo. An important point is that our studies examined retinas acutely after a 1-h exposure to glutamate or NMDA. In many previous studies, retinas have been examined 1 – 7 days after intraocular injections of these drugs and a significant thinning of the GCL was found. In only two of these studies were the RGCs identified by using retrograde injection of a fluorescent dye (Manabe and Lipton, 2003; Sun et al., 2000). These investigators clearly identified death of some RGCs by apoptosis in response to NMDA and, interestingly, this death took at least 24 h to begin. Delayed apoptosis in the GCL several days after NMDA injection into rat retina was also observed by Lam et al. (1999), Kido et al. (2000), and Moore et al. (2001). Because we did not observe death of RGCs in culture in response to prolonged exposure of glutamate or NMDA, the simplest explanation of our findings taken together with these previous investigators is that NMDA induces rapid loss of amacrine cells and that apoptotic death of some RGCs follows because of trophic deprivation from loss of amacrine signals rather than delayed excitotoxicity. How can we account for the discrepancy between our culture studies and those of others who reported that RGCs in vitro are vulnerable to glutamate and NMDA excitotoxicity? RGC survival strongly depends on target-derived trophic signals and thus 552 E.M. Ullian et al. / Mol. Cell. Neurosci. 26 (2004) 544–557 RGCs in culture rapidly undergo cell death unless appropriate neurotrophic support is specifically added to the culture medium. As appropriate trophic signals sufficient to support longterm RGC survival were not available before 1995, most of the early studies of RGC excitotoxicity involved short-term culture studies of 1 or 2 days at most, during which time the RGCs were rapidly dying even without any glutamate exposure. In contrast, our study involved use of RGCs highly purified using immunopanning that were provided with strong neurotrophic signals such as BDNF, CNTF, IGF-1, and laminin that promote their survival (Meyer-Franke et al., 1995). Otori et al. (1998), however, also used purified cultures of RGCs under conditions somewhat similar to those we used, yet observed severe kainate excitotoxicity that we did not observe. One difference is that IGF-1 was omitted from their culture conditions; thus, it is likely that RGC viabilities in their cultures were substantially lower than under the conditions we used (unfortunately they did not report their raw viabilities). Kainate activates both AMPA and kainate classes of glutamate receptors, at least some of which are calcium permeable in RGCs (Leinders-Zufall et al., 1994), and thus could be toxic particularly if viabilities were low. Nonetheless, Otori et al. (1998) is one of the few reports of kainate toxicity of RGCs in culture; most other reports of RGC excitotoxicity in culture have focused on NMDA toxicity (Aizenman et al., 1988; Lipton, 2001; Pang et al., 1999). Moreover, any toxicity of kainate in mixed retinal cultures and in intact retinas is thought to be due to release of glutamate, which then acts upon NMDA receptors on RGCs (Sucher et al., 1991a, 1997). Finally, another important variable increasingly coming to light is that the cell type affected by excitotoxicity, as well as the degree of excitotoxicity, may depend on the species and even the strain of the experimental animal used (Bakalash et al., 2002; Luo et al., 2001; Schori et al., 2002). We cannot exclude the possibility of some other variable between ours and previous studies that may account for why we do not observe excitotoxicity of RGCs in vitro. Whatever the explanation for the differences between our findings and previous findings of others, our studies show clearly that the purified RGCs in our cultures are behaving exactly the way they behave in intact retinas in that they are invulnerable to glutamate and NMDA excitotoxicity. Glutamate excitotoxicity probably does not contribute substantially to RGC death in retinal ischemia and glaucoma It is presently thought that glutamate and NMDA excitotoxicity contributes to loss of RGCs in retinal ischemia and glaucoma (Dreyer et al., 1996; Lipton, 2001; Naskar and Dreyer, 2001; Osborne et al., 1999). Our findings raise some doubts. Glutamate concentrations become acutely elevated in ischemia and are reported to be elevated chronically in glaucoma (Dreyer et al., 1996; Naskar and Dreyer, 2001, but see Dalton, 2001). However, RGCs die within a few hours after retinal ischemia (Osborne et al., 1999), whereas only delayed death of RGCs is observed in response to excitotoxicity (Manabe and Lipton, 2003). Similarly, chronic elevation of glutamate would be expected to kill amacrine cells, which are highly vulnerable to excitotoxicity, yet in glaucoma only loss of RGCs is observed (Quigley, 1999; Wax and Tezel, 2002). Thus, our observations do not lend support to an important contribution of glutamate excitotoxicity to retinal ischemia and glaucoma and in fact suggest that it does not. Why are RGCs invulnerable to NMDA excitotoxicity whereas amacrine cells are highly vulnerable? Why are RGCs not killed by NMDA when amacrine cells with similarly small NMDA currents are highly vulnerable? One factor that has been linked to excitotoxicity is the presence of functional synapses. Embryonic hippocampal neurons are not vulnerable to NMDA excitotoxicity until they have been cultured for 3 weeks and synaptogenesis has occurred (Choi et al., 1987). Perhaps the most striking example of uncoupling the level of glutamate current to the level of excitotoxicity has been found in the striatum. Striatal neurons are highly vulnerable to kainate exposure but are much less sensitive after synapses are removed by decortication, which does not alter their kainate sensitivity (Biziere and Coyle, 1978; McGeer and McGeer, 1976). Similarly, striatal NMDA excitotoxicity is largely eliminated by decortication to remove glutamatergic synapses (Orlando et al., 2001). However, when we increased the number of synapses that formed between the RGCs, we were unable to induce glutamate or NMDA excitotoxicity although we did increase their NMDA currents 4-fold. One intriguing difference between RGCs and hippocampal neurons is that RGCs do not appear to localize NMDARs directly underneath sites of vesicle release both in situ (Chen and Diamond, 2002) and in vitro (Taschenberger et al., 1995; this paper) but instead are extrasynaptic. Could NMDAR localization play a role in susceptibility to excitotoxicity? Synaptic NMDARs may have a different subunit composition, different kinetics, and be associated with different signaling components (Hardingham et al., 2002; Li et al., 2002; Tovar and Westbrook, 1999, 2002; Washbourne et al., 2002). Perhaps when NMDARs are not localized under release sites cells are intrinsically more resistant to excitotoxicity, both because currents are reduced and because signaling molecules that contribute to cell death are not activated. On the other hand, in cortical neurons, both synaptic and extrasynaptic NMDA receptors are able to mediate excitotoxic death (Sattler et al., 2000). Furthermore, in preliminary studies, the NMDA receptors of amacrine cells appear to be extrasynaptically localized (JSD and Joshua Singer, unpublished observations). Thus, as amacrine cells are highly vulnerable, the extrasynaptic localization of NMDA receptors on RGCs is probably not sufficient to account for their invulnerability to excitotoxicity. There are several other apparent differences between retinal ganglion cells and amacrine cells that may contribute to their different vulnerabilities to NMDA. First, it has recently been found that the NR3A subunit of the NMDA receptor is expressed strongly by RGCs but not by amacrine cells in the INL (Sucher et al., 2003). Consistent with the known dominant negative action of NR3 family members (Nishi et al., 2001), Sucher et al. (2003) found that NMDA-evoked intracellular calcium responses were significantly greater in NR3A deficient retinas. Thus, the expression of NR3A by RGCs but not by amacrine cells in the INL could help to explain a lower vulnerability to NMDA. Second, neuronal NOS bound to NMDARs via PSD-95 enhances excitotoxicity (Sattler et al., 1999) and amacrine cells and displaced amacrines have been reported to have much higher levels of nNOS (Kim et al., 2000; Shin et al., 1999; Yamamoto et al., 1993). Whatever the mechanism, the difference in excitotoxic vulnerability between RGCs and amacrine cells adds to the growing evidence that E.M. Ullian et al. / Mol. Cell. Neurosci. 26 (2004) 544–557 NMDA current density is not the sole determinant of susceptibility, but that other downstream signaling mechanisms play critical roles (Arundine and Tymianski, 2003). Experimental methods Cell purification and culture Step-by-step protocols for all procedures are available on request from [email protected]. RGCs from postnatal days 5 – 21 (P5 – P21) albino rats (Simonson rats; Simonson Labs, Gilroy, CA) were purified as previously described (Barres et al., 1988). Briefly, dissected retinas were enzymatically dissociated in papain in Dulbecco’s phosphate-buffered saline; Gibco, Carlsbad, CA) to create a single-cell suspension. RGCs were isolated from this suspension using sequential immunopanning to greater than 99.5% purity (Barres et al., 1988). Purified RGCs were plated on 12-mm glass coverslips (Carolina Science and Math, Burlington, NC) in 24-well tissue culture plates (BD Biosciences, San Jose, CA) at a density of 30,000 cells per coverslip (approximately 26,000 cells/cm2). Coverslips were coated with poly-D-lysine (PDL, 70 kDa, 10 Ag/ml; Sigma, St. Louis, MO) at room temperature followed by overnight incubation with mouse laminin (Sigma). RGCs were cultured in 500 Al of defined, serum-free medium, modified from Bottenstein and Sato (1979). Neurobasal media (Gibco) contained B27, selenium, putrescine, triiodo-thyronine, transferrin, progesterone, pyruvate (1 mM; Sigma), glutamine (2 mM; Sigma), ciliary neurotrophic factor (CNTF; 10 ng/ml; Regeneron Pharmaceuticals, Inc., Tarrytown, NY), brain-derived neurotrophic factor (BDNF; 50 ng/ml; Regeneron Pharmaceuticals, Inc.), insulin (5 Ag/ml; Sigma), and forskolin (10 AM, Sigma), as defined in Meyer-Franke et al. (1995). Cultures were maintained at 37jC in a humidified environment of 10% CO2 (Praxair, Danbury, CT). Under these conditions, more than half of RGCs survive in vitro for at least 1 month (Meyer-Franke et al., 1995). Cortical astrocyte cultures were prepared from first- to second-day postnatal (P1 – P2) albino rats as previously described (McCarthy and de Vellis, 1980). Briefly, the cortex was dissected and digested in trypsin and plated in tissue culture flasks (BD Biosciences) in a medium that does not allow survival of neurons (Dulbecco’s minimum essential medium, fetal bovine serum (10%), penicillin (100 U/ml), streptomycin (100 mg/ml), glutamine (2 mM), and Na-pyruvate (1 mM). After 4 days in culture, nonadherent cells were removed from flasks by shaking. Remaining cells were removed from flasks enzymatically and cultured on PDL (10 Ag/ml; Sigma) coated tissue culture plates (BD Biosciences). Purified RGC excitotoxicity experiments After 3 – 28 days in culture, the RGCs were exposed to NMDA, glutamate, AMPA, or kainic acid, each at 500 AM or 10 mM for 1 h, followed by a survival assay (see below). Cells in the 24-h agonist exposure experiment were cultured for 3 days and then treated with glutamate or NMDA (500 AM) for 24 h. Neuronal survival was determined using the 3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyl tetrazolium bromide (MTT; Sigma) survival assay as described by Mosmann (1983). MTT (500 553 Ag/ml) was added to cultures and incubated at 37jC for 1 h. The viable and dead cells in each well were counted by bright-field microscopy. Alternatively, cells were incubated for 10 min in calcein-AM (2 AM) and ethidium homodimer-1 (2 AM) following the manufacturer’s protocol (Molecular Probes, Eugene, OR, USA). Four fields of cells containing approximately 20 cells per field were counted for viability in each of three wells per condition. Experiments were repeated three times. Purified hippocampal neuron excitotoxicity experiments Hippocampal neurons from E19 Sprague – Dawley rat embryos were purified according to the methods of Banker and Goslin (1998) and cultured in Neurobasal plus Sato reagents with B27 (Gibco) in the presence of astrocyte feeder layers. Astrocyte or mixed retina co-culture excitotoxicity experiments RGCs were retrogradely labeling with fluorogold (2.5%, 0.5 Al; Fluorochrome, Englewood, CO) bilaterally injected into the superior collicular brachium. Sixteen to twenty-four hours postinjection, P5 – P6 animals were sacrificed and their retinas removed. The labeled RGCs were then purified as described above and plated at 15,000 RGCs per 12-mm coverslip. Concurrently, a mixed retinal dissociate was done by removing P5 – P6 retinas and dissociating enzymatically with papain to make a suspension of single cells, essentially as described by Huettner and Baughman (1986) and plated at 500,000 per well with the labeled RGCs. In the case of the astrocyte co-cultures, a feeding layer of astrocytes on a Falcon insert (BD, Franklin Lakes, NJ) was added after the RGCs had been in culture for 1 day. After day 3 in culture, the cultures were exposed to NMDA at 500 AM or 10 mM as described above. Two hundred micromolars of NMDA is a non-desensitizing dose (Aizenman et al., 1988, Hahn et al., 1988). The agonist was then gently rinsed off the cells and the cells were fixed with paraformaldehyde (PFA, 4%). The coverslips were then mounted on glass slides using Vectashield mounting and counted by fluorescent microscopy. Cell death was determined by morphology and live/dead assay on fluorescently labeled RGCs. Addition of ephrins EphrinB1 and ephrinB2 (500 ng/ml; R & D Systems, Minneapolis, MN) were pre-clustered for 1 h at room temperature using antihuman Fc (50 ng/ml; Jackson Labs). Following clustering, the ligands were added to the RGC cultures for 2 days. Cultures were then assayed for cell death or NMDA current amplitude. RGC excitotoxicity assay in whole mount retina and retinal sections Sixteen hours to sixteen days after retrogradely labeling RGCs with fluorogold, animals were sacrificed and their retinas removed. The retinas were then placed in a solution of Dulbecco’s phosphatebuffered saline (DPBS) and the experimental condition was treated with 500 AM or 10 mM NMDA or glutamate for 1 h while the control was placed only in DPBS. In some experiments, APV (100 AM) or MK-801 (60 AM) was added 15 min before and during the 554 E.M. Ullian et al. / Mol. Cell. Neurosci. 26 (2004) 544–557 hour exposure to glutamate or NMDA. After the 1 h exposure, the retinas were incubated with propidium iodide for 15 min at 37jC to label dead cell nuclei. The retinas were then fixed with 4% PFA for 1 h at room temperature and dissected by making four cuts from the edge into the center of the retina to flatten them (see Shen et al., 1999). The whole retinas were mounted on glass slides in Vectashield mounting medium containing DAPI (Vector Laboratories Inc., Burlingame, CA). For sectioning, after fixation, the retinas were sunk in 30% sucrose overnight at 4jC and mounted in OCT (Sakura Finetek, Torrance, CA). Neuronal death was determined for experimental and control retinas by analyzing the number of propidium iodide-labeled nuclei and fluorogold-labeled RGCs in the same area of each retina. NMDAR immunostaining Cells were fixed for 10 min in 4% PFA, washed three times in PBS, and blocked in Blocking buffer (50% goat serum, 50% PBS, 0.1% NP40). Following blocking, primary antibody incubation were done overnight at 4jC. Primary antibodies used were NR1 1:500 (PharMingen, San Diego, CA) or NR2B 1:50 (Transduction Laboratories, Lexington, KY). Secondary antibodies, goat anti-mouse Alexa 488 or Alexa 594 conjugates (Molecular Probes) were used at a dilution of 1:200 for 1 h at room temperature. Western blot analysis Standard SDS-PAGE gel electrophoresis was done as previously described (Meyer-Franke et al., 1998). Samples were collected in boiling 2% SDS and resolved on polyacrylamide gels and transferred onto polyvinylidene difluoride (Millipore, Bedford, MA). Blots were probed with monoclonal antibodies against NR1 (1 Ag/ml; PharMingen), rabbit polyclonal anti-NR2A (1 Ag/ ml; Upstate Biotechnology, Charlottesville, VA), and monoclonal anti-NR2B (1 Ag/ml; Transduction Labs). Horseradish peroxidase-conjugated secondary antibodies (Jackson ImmunoResearch, Westgrove, PA) were used in combination with chemiluminescent horseradish peroxidase substrate (ECL+Plus; Amersham, Arlington Heights, IL) at 1:30,000 and SuperSignal WestPico (Pierce, Rockford, IL) at 1:100,000 to produce the signals on chemiluminescent sensitive film (Scientific Imaging Systems, Eastman Kodak Company, Rochester, NY). Electrophysiology Membrane currents were recorded by whole-cell patch clamping at room temperature (18jC to 22jC) at a holding potential of 70 mV unless otherwise specified. Patch pipettes (3 – 10 MV) were pulled from borosilicate capillary glass (WPI). For recordings of synaptic currents, the bath solution contained (in mM) 120 NaCl, 3 CaCl2, 2 MgCl2, 5 KCl, and 10 Hepes (pH 7.3). For recording in Mg2+-free conditions, the external bath solution contained (in mM) 140 NaCl, 3.5 KCl, 10 HEPES, 20 glucose, 3 CaCl2, and 20 AM glycine (pH 7.3). The internal solution contained (in mM) 100 K-gluconate, 10 KCl, 10 EGTA (Ca2+buffered to 10 6), and 10 Hepes (pH 7.3). For recordings of autaptic currents, the internal solution contained (in mM) 122.5 K-gluconate, 8 NaCl, 10 Hepes, 0.2 EGTA, 2 Mg-ATP, 0.3 NaGTP, 20 K2-creatine phosphate, and phosphocreatine kinase (50 U/ ml). Currents were recorded using pClamp software for Windows (Axon Instruments, Foster City, CA). NMDA currents were expressed as pA as the membrane capacitances of RGCs were similar under all conditions. Mini-excitatory postsynaptic events (mEPSCs) were analyzed using Mini Analysis Program (SynaptoSoft, Decatur, GA) and plotted using SigmaPlot or Origin (Microcal, Northampton, MA). Electrophysiology of retinal slices Retinal slices were prepared from Sprague – Dawley rats (17 – 22 days) in accordance with the National Institute of Neurological Disorders and Stroke Animal Care and Use Committee guidelines. Both eyes were removed and immersed in oxygenated extracellular solution at room temperature. Extracellular solution contained (in mM): 119 NaCl, 2.5 KCl, 1.3 MgCl2, 2.5 CaCl2, 26.2 NaHCO3, 1 NaH2PO4, 20 glucose, 2 Na pyruvate, and 4 Na lactate, bubbled with 95% O2 and 5% CO2. The cornea, iris, lens, and vitreous were removed from one eye with scissors. The retina was mechanically detached from the eyecup and immersed in 2% agarose (low-gelling temperature, type VII; Sigma) and cut into 200-Am-thick slices on a vibratome (Leica, Nussloch, Germany). Slices were prepared and stored in oxygenated extracellular solution; they were transferred one at a time to the recording chamber, in which picrotoxin (100 AM) and strychnine (10 AM) were added to oxygenated extracellular solution to block inhibitory synaptic transmission. The patch pipette solution contained (in mM): 120 Cs methanesulfonate, 10 EGTA, 20 HEPES, 2 MgATP, and 0.2 NaGTP. All solutions were adjusted to pH 7.4 with NaOH or CsOH and adjusted to 290 – 300 mOsm with sucrose. Reagents were obtained from Sigma. All recordings were made from RGCs (identified post recording by filling neurons and identifying an axonal process) with an Axopatch 1D amplifier (Axon Instruments) in voltage-clamp mode. Patch electrodes (#0010 glass; World Precision Instruments, Sarasota, FL) had tip resistances of 4 – 5 MV when filled with internal solution. Access resistance was 10 – 20 MV and was monitored continuously. Data acquisition and analysis were performed with custom macros written in IgorPro (WaveMetrics, Lake Oswego, OR). Data were filtered at 5 kHz and sampled at 10 kHz. Responses were elicited by puffing NMDA (100 AM) onto RGC dendrites in the inner plexiform layer or the distal part of the inner nuclear layer, or by field illumination. Acknowledgments This work was supported by the National Eye Institute (R01 11030 to B.A.B.), and the March of Dimes Birth Defects Foundation (FY01-0503 to B.A.B.), a Zaffaroni Fellowship (E.M.U.), a HHMI undergraduate fellowship (W.B), and the NINDS Intramural Research Program (S.C and J.S.D.). We thank Regeneron for generously providing BDNF and CNTF. References Aizenman, E., Forsch, M.P., Lipton, S.A., 1988. Responses mediated by excitatory amino acid receptors in solitary retinal ganglion cells from rat. J. Physiol. 396, 75 – 91. E.M. Ullian et al. / Mol. Cell. Neurosci. 26 (2004) 544–557 Arundine, M., Tymianski, M., 2003. Molecular mechanisms of calciumdependent neurodegeneration in excitotoxicity. Cell Calcium 34, 325 – 337. Bakalash, S., Kipnis, J., Yoles, E., Schwartz, M., 2002. Resistance of retinal ganglion cells to an increase in intraocular pressure is immune-dependent. Invest. Ophthalmol. Visual Sci. 43, 2648 – 2653. Banker, G., Goslin, K., 1998. Culturing Nerve Cells. Second ed. MIT Press, Cambridge, MA. Barres, B.A., Silverstein, B.E., Corey, D.P., Chun, L.L.Y., 1988. Immunological, morphological, and electrophysiological variation among retinal ganglion cells purified by panning. Neuron 1, 791 – 803. Biziere, K., Coyle, J.T., 1978. Influence of corticostriatal afferents on striatal kainic acid neurotoxicity. Neurosci. Lett. 8, 303 – 310. Bottenstein, J.E., Sato, G.H., 1979. . Proc. Natl. Acad. Sci. U. S. A. 76, 514 – 517. Brandstatter, J.H., Hartveit, E., Sassoe-Pognetto, M., Wassle, H., 1994. Expression of NMDA and high affinity kainate receptor subunit mRNAs in the adult rat retina. Eur. J. Neurosci. 6, 1100 – 1112. Buisson, A., Yu, S.P., Choi, D.W., 1996. DCG-IV selectively attenuates rapidly triggered NMDA-induced neurotoxicity in cortical neurons. Eur. J. Neurosci. 8, 138 – 143. Caprioli, J., Kitano, S., Morgan, J.E., 1996. Hyperthermia and hypoxia increase tolerance of retinal ganglion cells to anoxia and excitotoxicity. Invest. Ophthalmol. Visual Sci. 47, 2376 – 2381. Chen, S., Diamond, J., 2002. Synaptically released glutamate activates extrasynaptic NMDA receptors on cells in the ganglion cell layer of the rat retina. J. Neurosci. 22, 2165 – 2173. Choi, D.W., 1985. Glutamate neurotoxicity in cortical cell culture is calcium dependent. Neurosci. Lett. 58, 293 – 297. Choi, D.W., 1992. Excitotoxic cell death. J. Neurobiol. 23, 1261 – 1276. Choi, D.W., Maulucci-Gedde, M.A., Kriegstein, A.R., 1987. Glutamate neurotoxicity in cortical cell culture. J. Neurosci. 7, 336 – 357. Clark, B.A., Cull-Candy, S.G., 2002. Activity-dependent recruitment of extrasynaptic NMDA receptor activation at an AMPA receptor-only synapse. J. Neurosci. 22, 4428 – 4436. Dalton, R., 2001. Private investigations. Nature 411, 129 – 130. Dalva, M.B., Takasu, M.A., Lin, M.Z., Shamah, S.M., Hu, L., Gale, N.W., Greenberg, M.E., 2000. EphB receptors interact with NMDA receptors and regulate excitatory synapse formation. Cell 103, 945 – 956. Dingledine, R., Borges, K., Bowie, D., Traynelis, S., 1999. The glutamate receptor ion channels. Pharm. Rev. 51, 7 – 61. Dreyer, E.B., Pan, Z.H., Storm, S., Lipton, S.A., 1994. Greater sensitivity of larger retinal ganglion cells to NMDA mediated cell death. Neuroreport 5, 629 – 631. Dreyer, E.B., Zuracowski, D., Schumer, R.A., Podos, S.M., Lipton, S.A., 1996. Elevated glutamate levels in the vitreous body of humans and monkeys with glaucoma. Arch. Ophthalmol. 114, 299 – 305. Erdo, S.L., Michler, A., Wolff, J.R., Tytko, H., 1990. Lack of excitotoxic cell death in serum-free cultures of rat cerebral cortex. Brain Res. 526, 328 – 332. Goldberg, J.L., Barres, B.A., 2000. The relationship between neuronal survival and regeneration. Annu. Rev. Neurosci. 23, 579 – 612. Goldberg, J.L., Espinosa, J.S., Xu, Y., Davidson, N., Kovacs, G.T., Barres, B.A., 2002. Retinal ganglion cells do not extend axons by default: promotion by neurotrophic signaling and electrical activity. Neuron 33, 689 – 702. Gomperts, S.N., Carroll, R., Malenka, R.C., Nicoll, R.A., 2000. Distinct roles for ionotropic and metabotropic glutamate receptors in the maturation of excitatory synapses. J. Neurosci. 15, 2229 – 2237. Grunder, T., Kohler, K., Guenther, E., 2000a. Distribution and developmental regulation of AMPA receptor subunit proteins in rat retina. Invest. Ophthalmol. Visual Sci. 41, 3600 – 3606. Grunder, T., Kohler, K., Kaletta, A., Guenther, E., 2000b. Distribution and developmental regulation of NMDA receptor subunit proteins in the rat retina. J. Neurobiol., 333 – 342. Ha, B.K., Vicini, S., Rogers, R.C., Bresnahan, J.C., Burry, R.W., Beattie, M.S., 2002. Kainate-induced excitotoxicity is dependent upon extracel- 555 lular potassium concentrations that regulate the activity of AMPA/KA type glutamate receptors. J. Neurochem. 83, 934 – 945. Hahn, J.S., Aizenman, E., Lipton, S.A., 1988. Central mammalian neurons normally resistant to glutamate toxicity are made sensitive by elevated extracellular Ca2+: toxicity is blocked by the N-methyl-Daspartate antagonist MK-801. Proc. Natl. Acad. Sci. U. S. A. 85, 6556 – 6560. Hardingham, G.E., Fukunaga, Y., Bading, H., 2002. Extrasynaptic NMDARs oppose synaptic NMDARs by triggering CREB shut-off and cell death pathways. Nat. Neurosci. 5, 405 – 413. Hartveit, E., Veruki, M.L., 1997. AII amacrine cells express functional NMDA receptors. Neuroreport 8, 1219 – 1223. Huettner, J.E., Baughman, R.W., 1986. Primary culture of identified neurons from the visual cortex of postnatal rats. Neuroscience 6, 3044 – 3060. Izumi, Y., Benz, A.M., Kirby, C.O., Labrueyer, J., Zorumski, C.F., Price, M.T., Olney, J.W., 1995. An ex vivo rat retinal preparation for excitotoxicity studies. J. Neurosci. Methods 60, 219 – 225. Kawasaki, A., Otori, Y., Barnstable, C.J., 2000. Muller cell protection of rat retinal ganglion cells from glutamate and nitric oxide neurotoxicity. Invest. Ophthalmol. Visual Sci. 41, 3444 – 3450. Kawasaki, A., Han, M., Wei, J., Hirata, K., Otori, Y., Barstable, C.J., 2002. Protective effects of arachidonic acid on glutamate neurotoxicity in rat retinal ganglion cells. Invest. Ophthalmol. Visual Sci. 43, 1835 – 1842. Kido, N., Tanihara, H., Honjo, M., Inatani, M., Tatsuno, T., Nakayama, C., Honda, Y., 2000. Neuroprotective effects of BDNF in eyes with NMDA induced neuronal death. Brain Res. 884, 59 – 67. Kim, K.Y., Ju, W.K., Oh, S.J., Chun, M.H., 2000. The immunocytochemical localization of neuronal nitric oxide synthase in the developing rat retina. Exp. Brain Res. 133, 419 – 424. Kitano, S., Morgan, J., Caprioli, J., 1996. Hypoxic and excitotoxic damage to cultured rat retinal ganglion cells. Exp. Eye Res. 63, 105 – 112. Lam, T., Abler, A., Kwong, J., Tso, M., 1999. NMDA induced apoptosis in rat retina. Invest. Ophthalmol. Visual Sci. 40, 2391 – 2397. Leinders-Zufall, T., Rand, M.N., Waxman, S.G., Kocsis, J.D., 1994. Differential role of two Ca(2+)-permeable non-NMDA glutamate channels in rat retinal ganglion cells: kainate-induced cytoplasmic and nuclear Ca2+ signals. J. Neurophysiol. 72, 2503 – 2516. Li, Y., Schlamp, C.L., Nickells, R.W., 1999. Experimental induction of retinal ganglion cell death in adult mice. Invest. Ophthalmol. Visual Sci. 40, 1004 – 1008. Li, B., Chen, N., Luo, T., Otsu, Y., Murpy, T., Raymond, L.A., 2002. Differential regulation of synaptic and extrasynaptic NMDA receptors. Nat. Neurosci. 5, 833 – 834. Linden, R., Esberard, C.E., 1987. Displaced amacrine cells in the ganglion cell layer of the hamster retina. Vision Res. 27, 1071 – 1076. Lipton, S., 2001. Retinal ganglion cells, glaucoma, neuroprotection. Prog. Brain Res. 131, 712 – 719. Lucas, D.R., Newhouse, J.P., 1957. The toxic effect of glutamate on the inner layers of the retina. Arch. Ophthalmol. 158, 193 – 201. Luo, X., Heidinger, V., Picaud, S., Lambrou, G., Dreyfus, H., Sahel, J., Hicks, D., 2001. Selective excitotoxic degeneration of adult pig retinal ganglion cells in vitro. Invest. Ophthalmol. Visual Sci. 42, 1096 – 1106. Manabe, S., Lipton, S.A., 2003. Divergent NMDA signals leading to proapoptotic and antiapoptotic pathways in rat retina. Invest. Ophthalmol. Visual Sci. 44, 385 – 392. Matsui, K., Hosoi, N., Tachibana, M., 1998. Excitatory synaptic transmission in the inner retina: paired recordings of bipolar cells and neurons in the ganglion cell layer. J. Neurosci. 18, 4500 – 4510. Matsui, K., Hasegawa, J., Tachibana, M., 2001. Modulation of excitatory synaptic transmission by GABA(C) receptor-mediated feedback in the mouse inner retina. J. Neurophysiol. 86, 2285 – 2298. McCarthy, K.D., de Vellis, J., 1980. Preparation of separate astroglial and oligodendroglial cell cultures from rat cerebral tissue. J. Cell Biol. 85, 890 – 902. 556 E.M. Ullian et al. / Mol. Cell. Neurosci. 26 (2004) 544–557 McGeer, E., McGeer, P., 1976. Duplication of biochemical changes of Huntington’s chorea by intrastriatal injections of glutamic and kainic acid. Nature 263, 517 – 519. Meyer-Franke, A., Kaplan, M.R., Pfrieger, F.W., Barres, B.A., 1995. Characterization of the signaling interactions that promote the survival and growth of developing retinal ganglion cells in culture. Neuron 15, 805 – 819. Meyer-Franke, A., Wilkinson, G.A., Kruttgen, A., Hu, M., Munro, E., Hanson, M.G., Reichardt, L.F., Barres, B.A., 1998. Depolarization and cAMP elevation rapidly recruit TrkB to the plasma membrane of CNS neurons. Neuron 21, 681 – 693. Moncaster, J.A., Walsh, D.T., Gentleman, S.M., Jen, L.S., Aruoma, O.I., 2002. Ergothioneine treatment protects neurons against N-methyl-D-aspartate excitotoxicity in an in vivo rat retinal model. Neurosci. Lett. 328, 55 – 59. Moore, P., El-sherbeny, A., Roon, P., Schoenlein, P.V., Ganapthy, V., Smith, S.B., 2001. Apoptotic cell death in the mouse retinal ganglion cell layer is induced in vivo by the excitatory amino acid homocysteine. Exp. Eye Res. 73, 45 – 57. Mosinger, J.L., Price, M.T., Bai, H.Y., Xiao, H., Wozniak, D.F., Olney, J.W., 1991. Blockade of both NMDA and non-NMDA receptors is required for optimal protection against ischemic neuronal degeneration in the in vivo adult mammalian retina. Exp. Neurol. 113, 10 – 17. Mosmann, T., 1983. Rapid colorimetric assay for cellular growth and survival: application to proliferation and cytotoxicity assays. J. Immunol. Methods 16, 55 – 63. Murai, K.K., Nguyen, L.N., Irie, F., Yamaguchi, Y., Pasquale, E.B., 2003. Control of hippocampal dendritic spine morphology through ephrin-A3/ EphA4 signaling. Nat. Neurosci. 6, 153 – 160. Nagler, K., Mauch, D.H., Pfrieger, F.W., 2001. Glia-derived signals induce synapse formation in neurones of the rat central nervous system. J. Physiol. 15, 665 – 679. Naskar, R., Dreyer, E.B., 2001. New horizons in neuroprotection. Surv. Ophthalmol. 45, S250 – S255. Nishi, M., Hinds, H., Lu, H.P., Kawata, M., Hayashi, Y., 2001. Motoneuron-specific expression of NR3B, a novel NMDA-type glutamate receptor subunit that works in a dominant-negative manner. J. Neurosci. 21, RC185. O’Brien, R.J., Mammen, A.L., Blackshaw, S., Ehlers, M.D., Rothstein, J.D., Huganir, R.L., 1997. The development of excitatory synapses in cultured spinal neurons. J. Neurosci. 17, 7339 – 7350. Olney, J.W., 1969. Glutamate-induced retinal degeneration in neonatal mice. Electron microscopy of the acutely evolving lesion. J. Neuropathol. Exp. Neurol. 28, 455 – 474. Orlando, L., Alsdorf, S., Penney, J., Young, A.B., 2001. The role of group I and group II metabotropic glutamate receptors in modulation of striatal NMDA and quinolinic acid toxicity. Exp. Neurol. 167, 196 – 204. Osborne, N.N., Wood, J.P.M., Chidlow, G., Bae, J., Melena, J., Nash, M.S., 1999. Ganglion cell death in glaucoma: what do we really know? Br. J. Ophthalmol. 83, 980 – 986. Otori, Y., Wei, J.Y., Barnstable, C.J., 1998. Neurotoxic effects of low doses of glutamate on purified rat retinal ganglion cells. Invest. Ophthalmol. Vis. Sci. 39, 972 – 981. Pang, I., Wexler, E., Nawy, S., Kapin, M., 1999. Protection by cliprodil against excitotoxicity in cultured rat retinal ganglion cells. Invest. Ophthalmol. Visual Sci. 40, 1170 – 1176. Peterson, C., Neal, J.H., Cotman, C.W., 1989. Development of N-methyl-Daspartate excitotoxicity in cultured hippocampal neurons. Brain Res. Dev. Brain Res. 48, 187 – 195. Pfrieger, F.W., Barres, B.A., 1997. Synaptic efficacy enhanced by glial cells in vitro. Science 277, 1684 – 1687. Quigley, H.A., 1999. Neuronal death in glaucoma. Prog. Retinal Eye Res. 18, 39 – 57. Ritch, R., 2000. Neuroprotection: is it already applicable to glaucoma therapy? Curr. Opin. Ophthalmol. 11, 78 – 84. Romano, C., Chen, Q., Olney, J.W., 1998. The intact isolated (ex vivo) retina as a model system for the study of excitotoxicity. Prog. Retinal Eye Res. 17, 465 – 483. Rothman, S.M., Olney, J.W., 1987. Excitotoxicity and the NMDA receptor. Trends Neurosci. 10, 299 – 302. Sabel, B.A., Sautter, J., Stoehr, T., Siliprandi, R., 1995. A behavioral model of excitotoxicity. Exp. Brain Res. 106, 93 – 105. Sattler, R., Xiong, Z., Lu, W., Hafner, M., MacDonald, J., Tymianski, M., 1999. Specific coupling of NMDA receptor activation to nitric oxide neurotoxicity by PSD-95 protein. Science 284, 1845 – 1848. Sattler, R., Xiong, Z., Lu, W., MacDonald, J., Tymianski, M., 2000. Distinct roles of synaptic and extrasynaptic NMDA receptors in excitotoxicity. J. Neurosci. 20, 22 – 33. Schori, H., Yoles, E., Wheeler, L.A., Raveh, T., Kimchi, A., Schwartz, M., 2002. Immune-related mechanisms participating in resistance and susceptibility to glutamate toxicity. Eur. J. Neurosci. 16, 557 – 564. Shen, S., Wiemelt, A.P., McMorris, F.A., Barres, B.A., 1999. Retinal ganglion cells lose trophic responsiveness after axotomy. Neuron 23, 285 – 295. Shin, D.H., Lee, H.Y., Kim, H.J., Lee, E., Lee, K.H., Lee, W.J., Cho, S.S., Baik, S.H., 1999. In situ localization of neuronal nitric oxide synthase (nNOS) mRNA in the rat retina. Neurosci. Lett. 270, 53 – 55. Silprandi, R., Canella, R., Carmignoto, G., Schiavo, N., Zanellato, Z., Zanoni, R., Vantani, G., 1992. NMDA induced neurotoxicity in the adult rat retina. Vis. Neurosci. 8, 567 – 573. Sisk, D.R., Kuwabara, T., 1985. Histological changes in the inner retina of albino rats following intravitreal injection of glutamate. Graefe’s Arch. Clin. Exp. Ophthalmol. 223, 250 – 258. Sucher, N.J., Aizenman, E., Lipton, S.A., 1991a. NMDA antagonists prevent kainate neurotoxicity in rat retinal ganglion cells in vitro. J. Neurosci. 11, 966 – 973. Sucher, N.J., Lei, S.Z., Lipton, S.A., 1991b. Calcium channel antagonists attenuate NMDA receptor-mediated neurotoxicity of retinal ganglion cells in culture. Brain Res. 551, 297 – 302. Sucher, N.J., Lipton, S.A., Dreyer, E.B., 1997. Molecular basis of glutamate toxicity in retinal ganglion cells. Vision Res. 37, 3483 – 3493. Sucher, N.J., Kohler, K., Tenneti, L., Wong, H.K., Grunder, T., Fauser, S., Wheeler-Schilling, T., Nakanishi, N., Lipton, S.A., Guenther, E., 2003. N-methyl-D-aspartate receptor subunit NR3A in the retina: developmental expression, cellular localization, and functional aspects. Invest. Ophthalmol. Visual Sci. 44, 4451 – 4456. Sun, Q., Oooi, V., Chan, S., 2000. NMDA induced excitotoxicity in the adult rat retina is antagonized by single systemic injection of MK-801. Exp. Brain Res. 138, 37 – 45. Takasu, M.A., Dalva, M.B., Zigmond, R.E., Greenberg, M.E., 2002. Modulation of NMDA receptor dependent calcium influx and gene expression through EphB receptors. Science 295, 491 – 495. Taschenberger, H., Engert, F., Grantyn, R., 1995. Synaptic current kinetics in a solely AMPA receptor operated glutamatergic synapse formed by rat retinal ganglion neurons. J. Neurophysiol. 74, 1123 – 1136. Taylor, W.R., Chen, E., Copenhagen, D.R., 1995. Characterization of spontaneous excitatory synaptic currents in salamander retinal ganglion cells. J. Physiol. 486, 207 – 221. Tezel, G.M., Seigel, G.M., Wax, M.B., 1999. Density-dependent resistance to apoptosis in retinal cells. Curr. Eye Res. 19, 377 – 388. Tovar, K.R., Westbrook, G.L., 1999. The incorporation of NMDA receptors with a distinct subunit composition at nascent hippocampal synapses in vitro. J. Neurosci. 19, 4180 – 4188. Tovar, K.R., Westbrook, G.L., 2002. Mobile NMDA receptors at hippocampal synapses. Neuron 34, 255 – 264. Ullian, E.M., Sapperstein, S.K., Christopherson, K.S., Barres, B.A., 2001. Control of synapse number by glia. Science 291, 657 – 661. Vorwerk, C.K., Lipton, S.A., Zurakowski, D., Hyman, B.T., Sabel, B.A., Dreyer, E.B., 1996. Chronic low-dose glutamate is toxic to retinal ganglion cells. Toxicity blocked by memantine. Invest. Ophthalmol. Visual Sci. 37, 1618 – 1624. E.M. Ullian et al. / Mol. Cell. Neurosci. 26 (2004) 544–557 Washbourne, P., Bennett, J.E., McAllister, A.K., 2002. Rapid recruitment of NMDA receptor transport packets to nascent synapses. Nat. Neurosci. 5, 751 – 759. Watanabe, M., Masayoshi, M., Inone, Y., 1994. Differential distributions of the NMDA receptor channel subunit mRNAs in the mouse retina. Brain Res. 634, 328 – 332. 557 Wax, M.B., Tezel, G., 2002. Neurobiology of glaucomatous optic neuropathy: diverse cellular events in neurodegeneration and neuroprotection. Mol. Neurobiol. 26, 45 – 55. Yamamoto, R., Bredt, D.S., Snyder, S.H., Stone, R.A., 1993. The localization of nitric oxide synthase in the rat eye and related cranial ganglia. Neuroscience 54, 189 – 200.