* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Carbohydrate metabolism2
Proteolysis wikipedia , lookup
NADH:ubiquinone oxidoreductase (H+-translocating) wikipedia , lookup
Mitochondrion wikipedia , lookup
Lipid signaling wikipedia , lookup
Basal metabolic rate wikipedia , lookup
Microbial metabolism wikipedia , lookup
Metalloprotein wikipedia , lookup
Nicotinamide adenine dinucleotide wikipedia , lookup
Specialized pro-resolving mediators wikipedia , lookup
Lactate dehydrogenase wikipedia , lookup
Butyric acid wikipedia , lookup
Blood sugar level wikipedia , lookup
Adenosine triphosphate wikipedia , lookup
Phosphorylation wikipedia , lookup
Biosynthesis wikipedia , lookup
Evolution of metal ions in biological systems wikipedia , lookup
Oxidative phosphorylation wikipedia , lookup
Fatty acid synthesis wikipedia , lookup
Glyceroneogenesis wikipedia , lookup
Amino acid synthesis wikipedia , lookup
Fatty acid metabolism wikipedia , lookup
Biochemistry wikipedia , lookup
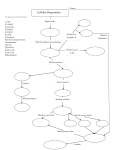
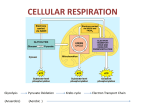
CAROHYDRATE METABOLISM PART 2 BY PROF.DR. SOUAD ABOAZMA OXIDATION OF GLUCOSE The pathways for oxidation of glucose are classified into two main groups: a- The major pathways for complete oxidation of glucose into CO2, H2O and energy are: 1- Glycolysis → convert one molecule of glucose into 2 mol of pyruvic acid + 2 NADH.H+. 2- Oxidative decarboxylation of pyruvic to acetyl CoA + NADH.H++CO2 3- Complete oxidation of acetyl CoA in Kerb’s cycle into CO2, H2O and energy . b- The minor pathways for oxidation, which are not for energy production. 1- Hexose monophosphate pathway (HMP). 2- Uronic acid pathway. GLYCOLYSIS EMBDEN-MEYERHOF PATHWAY Def.: oxidation of glucose to give pyruvic acid in presence of O2 and lactic acid in absence of mitochondria (RBCs) and in absence of O2 . Site: Cytoplasm of all cells especially muscles and RBCs. Steps: H–C=O H–C=O H C – OH OH – C – H H – C – OH Hexokinase, glucokinase H – C – OH H – C – OH CH2OH D-Glucose ATP OH – C – H Mg H – C – OH ADP H – C – OH CH2O-P G-6-P Mechanism of oxidation of glyceraldehydes 3-phosphate. Enz: glyceraldehydes 3-P dehydrogenase which is inhibited by the –SH poison iodoacetate, thus able to inhibit glycolysis. ENERGY PRODUCTION FROM GLYCOLYSIS: A. glycolysis in presence of O2 (Aerobic glycolysis): Reaction catalyzed by ATP production Stage I 1. Hexokinase/Glucokinase reaction (for phosphorylation) 2. Phosphofrutokinase-1 (for phosphorylation) -1 ATP -1 ATP Stage III 3. Glyceraldehyde-3-P dehydrogenase (oxidation of 2 NADH in electron transport chain) 4. Phosphoglycerate kinase (substrate level + 6 or +4 ATP +2 ATP phosphorylation) Stage IV 5. Pyruvate kinase (substrate level phosphorlyation) +2 ATP Net gain = 10 or 8 - 2 = 8 or 6ATP B. Glycolysis in Absence of O2 (Anaerobic glycolysis): •In absence of O2 re-oxidation of NADH at glyceraldehyde-3-Pdehydrogenase stage cannot take place in electron-transport chain. But the cells have limited coenzyme. Hence to continue the glycolytic pathway NADH must be oxidized to NAD+. This is achieved by reoxidation of NADH by conversion of pyruvate to lactate (without producing ATP) by the enzyme lactate dehydrogenase. Occurs in cells with no mitochondria as RBCs (mature) ,or under low O2 supply as intensive muscular exercise. In anaerobic glycolysis per molecule of glucose oxidation 4 - 2 = 2 ATP will be produced. REGULATION OF GLYCOLYSIS There are 3 types of mechanisms responsible for regulation of the enzyme activity which are: 1- Changed in rate of enzyme synthesis that affect the quantity of enzyme as: * Induction →↑ rate of enzyme synthesis at gene expression →↑ mRNA synthesis →increase enzyme concentration. * Repression →↓ rate of enzyme synthesis at gene expression →↓ mRNA synthesis →decrease enzyme concentration. 2- Covalent modification by reversible phosphorylation dephosphorylation. 3- Allosteric regulation by allosteric activator or inhibitor that affect the quality of the enzymes. A- Allosteric regulation of glycolysis: There are 4 regulatory enzymes which responsible for 3 irreversible reaction in glycolysis. Hexokinase 1.It is found in most tissues to give G-6-P when blood glucose level is low. 2.Acts on glucose and other hexoses to give hexose-6-P. 3.It has low km and Vmax→ acts maximally at fasting bl. glucose level. 4.It is inhibited by its products, which is G-6-P → allosteric feedback inhibition. Glucokinase 1.It is found in liver and acts maximally after meal. 2.Acts only on glucose. 3.It has a high km and high Vmax → so it is active when bl. glucose level is high (after meal). 4.It is induced (↑its rate of synthesis) by insulin. 5.It is not inhibited by G-6-P. Phosphofructokinase 1.It is the major regulatory enzyme in most tissues. 2.It is allosterically activated by F-6-P, AMP and inhibited by ATP, citrate, and H+. Pyruvate kinase 1.It is allosterically inhibited by ATP, fatty acids, alanine, and acetyl CoA. And activated by F-1-6 diphosphate. 2. It is phosphorylated by cAMP dependent protein kinase, which becomes inactive and dephosphorylated by phosphatase enzyme, which becomes active. B- Hormonal regulation:• Insulin/glucagons ratio is the main hormonal regulation of glucose utilization; it increases during glucose feeding and decreases during fasting. A.Glucagons: it is secreted in case of carbohydrates deficiency or in response to low blood glucose level (hypoglycemia). It affects liver cells mainly as follows: 1.It acts as repressor of glycolytic key enzymes except hexokinase. 2.Through cAMP-dependent protein kinase A, it produces phosphorylation of specific protein enzymes that lead to inactivation of glycolytic key enzymes( only for pyruvate kinase). B.Insulin: it is secreted after feeding of carbohydrate or in response to high blood glucose level (hyperglycemia). It stimulates all pathways of glucose utilization. Insulin binds to a specific cell membrane receptors and produces certain signal cascade, which results in the following: 1.It acts as inducer for glycolytic key enzymes. 2.It activats phosphodiesterase enzyme(decreases cAMP that leads to inhibition of protein kinase A). 3.It activats protein phosphatase-1 that produces dephosphorylation of glycolytic key enzymes and their activation. INHIBITORS OF GLYCOLYSIS: 1- Aresnate : which used in oxidative step insted of Pi→ so glycolysis proceeds in presence of arsenate but ATP, which formed from 1-3 diphosphoglycerate is lost. 2- Iodoacetate produces inhibition of glyceraldehydes-3-P dehydrogenase (inhibitor of SH group). 3- Flouride inhibits enolase →↓↓ glycolysis in bacteria →no production of lactic acid produced by bacteria, which cause dental caries. It used as anticoagulant in blood sample used for estimation of blood glucose →↓↓ glycolysis in RBCs . FORMATION OF 2,3 DIPHOSPHOGLYCERATE IN RBCS: 2:3 diphosphoglycerate has an effect on O2 binding power of haemoglobin→ It lowers O2 affinity by haemoglobin →↑ dissociation of O2 to the peripheral tissues as in cases of high altitude. CLINICAL SIGNIFICANCE OF 2,3 DIPHSOPHOGLYCERATE: 1- Persons who live at high altitude undergo state of low O2 affinity for HB due to simultaneous increase of 2,3 diphosphoglycerate. This increase can be reversed on returning to sea level. 2- Fetal HB has less 2,3 diphosphoglycerate than adult HB, so fetal HB has high O2 affinity. 3- During storage of blood in blood banks, there is decrease in 2,3 diphosphoglycerate so, stored blood has high O2 affinity, which is not suitable for blood transfusion especially to ill patients. If 2,3 diphosphoglycerate is added to stored blood, it can’t penetrate RBCs wall. So, it is advisable to add insoine, which is a substance that can penetrate RBCs wall and change it into 2,3 diphosphoglycerate through HMP shunt. DIFFERENCES BETWEEN AEROBIC AND ANAEROBIC GLYCOLYSIS - Site - End products - Energy production - Lactate dehdyrogenase Aerobic glycolysis Anaerobic glycolysis Cytoplasm of all tissues RBCs and skeletal muscle during muscular ex. Pyruvic acid + NADH.H+ Lactic acid + NAD+ 6 OR, 8 ATP 2 ATP Not needed Needed DISEASES ASSOCIATED WITH IMPAIRED GLYCOLYSIS 1- Hexokinase deficiency : •In patients with inherited defects of hexokinase activity, the red blood cells contain low concentrations of the glycolytic intermediates including the precursor of 2,3-DPG. •In consequence, the hemoglobin of these patients has an abnormally high oxygen affinity. •The oxygen saturation curves of red blood cells from a patient with hexokinase deficiency are shifted to the left, which indicates that oxygen is less available for the tissues. 2- Pyruvate kinase deficiency (hemolytic anemia): •All red blood cells are completely dependent upon glycolytic activity for ATP production. •Failure of the pyruvate kinase reaction, the production of ATP will decrease leading to hemolysis of red cells. •Inadequate production of ATP reduces the activity of the Na+ - and K+ -stimulated ATPase ion pump. 3- Lactic acidosis:•Blood levels of lactic acid are normally less than 1.2 mM. In lactic acidosis, the values for blood lactate may be 5 mM or more. •The high concentration of lactate results in lowered blood pH and bicarbonate levels. •High blood lactate levels can result from increased formation or decreased utilization of lactate. •Common cause of hyperlacticidemia is anoxia. •Tissue anoxia may occur in shock and other conditions that impair blood flow, in respiratory disorders, and in severe anemia. AEROBIC AND ANAEROBIC EXERCISE USE DIFFERENT FUELS Aerobic exercise is exemplified by long-distance running, while anaerobic exercise by sprinting or weight lifting. During anaerobic exercise there is really very little inter-organ cooperation. The vessels within the muscles are compressed during peak contraction, thus their cells are isolated from the rest of the body. Muscle largely relies on its own stored glycogen and phosphocreatine. Phosphocreatine serves as a source of high-energy phosphate for ATP synthesis for first 4-5 seconds until glycogenolysis and glycolysis are stimulated. Glycolysis becomes the primary source of ATP for want of oxygen. Aerobic exercise is metabolically more interesting. For moderate exercise, much of thet energy is derived from glycolysis of muscle glycogen.. However, a well-fed individual doesn't store enough glucose and glycogen to provide the energy needed for running long distances. The respiratory quotient, the ratio of carbon dioxide exhaled to oxygen consumed, falls during distance running. This indicates the progressive switch from glycogen to fatty acid oxidation during a race. Lipolysis gradually increases as glucose stores are exhausted, and, as in the fast state, muscles oxidize fatty acids in preference to glucose as the former become available. Marathon runner (42.2 KM or 26 Miles) •In the marathon runner predominantly red fibres (oxidative) are used. •Red fibres contain myoglobin and mitochondria. •The major sources of energy in marathon runner are:•Aerobic metabolism is the principal source of ATP. •Blood glucose. •Hepatic glycogen is degraded to maintain the level of blood glucose. •Muscle glycogen is also a source of fuel but it is degraded slowly than in sprinter . •Free fatty acids derived from the triacylglycerol of adipose tissue. Sources of fuel used by marathon runner and there duration of action Source of fuel Duration of action by minutes Blood glucose 4 Liver glycogen 18 Muscle glycogen 70 Triacylglycerol 4000 MAJOR FEATURES OF SKELETAL MUSCLE S METABOLISM 1.Skeletal muscle functions under both aerobic (resting) and anaerobic (eg, sprinting) conditions, so both aerobic and anaerobic glycolysis operate, depending on conditions. 2.Skeletal muscle contains myoglobin as a reservoir of oxygen. 3.Insulin acts on skeletal muscle to increase uptake of glucose. 4.In the fed state, most glucose is used to synthesize glycogen, which acts as a store of glucose for use in exercise, 'preloading' with glucose is used by some long-distance athletes to build up stores of glycogen. 5.Epinephrine stimulates glycogenolysis in skeletal muscle, whereas glucagon does not because of absence of its receptors. 6.Skeletal muscle cannot contribute directly to blood glucose because it does not contain glucose-6phosphatase. 7.Lactate produced by anaerobic metabolism in skeletal muscle passes to liver, which uses it to synthesize glucose, which can then return to muscle, (the cori cycle). 8.Skeletal muscle contains phosphocreatine, which acts as an energy store for short-term (seconds) demands. 9.Free fatty acids in plasma are a major source of energy, particularly under marathon conditions and in prolonged starvation. 10.Skeletal muscle can utilize ketone bodies during starvation. 11.Skeletal muscle is the principle site of metabolism of branched chain amino acids, which are used as energy source. 12.Proteolysis of muscle during starvation supplies amino acids for gluconeogenesis. 13.Major amino acids emanating from muscle are alanine (destined mainly for gluconeogenesis in liver and forming part of the glucose-alanine cycle) and glutamine (destined mainly for the gut and kidneys). Significance of glycolysis •Glycolysis is the principle route for glucose metabolism for the production of ATP molecules •It also provide pathway for the metabolism of fructose and galactose derived from diet. •It represent the only source of energy for RBCs and contracting muscle. •It provide mitochondria with pyruvic which give acetyle CoA (Kreb's Cycle) •Glycolysis give DHAP which reduced to α glycerophosphate which form backbone of triacylglycerol in lipogenesis •In erythrocytes glycolysis supplies 2,3 DPG which is required for haemoglobin function in transport of oxygen. OXIDATIVE DECARBOXYLATION OF PYRUVIC ACID Def.: It is conversion of pyruvic acid and other α-keto acids into CoA derivatives, CO2 & NADH.H+. Site: In mitochondrial matrix of all tissues except RBCs Steps: The conversion of pyruvic acid into acetyl CoA is catalyzed by pyruvate dehydrogenase complex, which composed of 3 enzymes act cooperative with each other in presence of 5 co-enzymes: TPP, lipoic acid, FAD, NAD+, and CoASH. Pyruvate +TTP + Lipoic acid + CoA +FAD+ NAD + --→ CO2 + Acetyl-CoA + NADH + H+ Steps of oxidative decarboxylation of pyruvic acid: •Pyruvate is decarboxylated to form a hydroxyethyl derivative bound to the reactive carbon of thiamine pyrophosphate, the coenzyme of pyruvate decarboxylase. •The hydroxyethyl intermediate is oxidized by transfer to the disulfide form of lipoic acid covalently bound to dithydrolipoyl transacetylase. •The acetyl group, bound as a thioester to the side chain of lipoic acid, is transferred to CoA. •The sulfhydryl form of lipoic acid is oxidized by FADdependent dihydrolipoyl dehydrogenase, leading to the regeneration of oxidized lipoic acid. •Reduced flavoprotein is reoxidized to FAD by dihydrolipoyl dehydrogenase and NAD+. REGULATION OF OXIDATIVE DECARBOXYLATION OF PYRUVIC ACID : 1- Product inhibition : The enzyme complex is inhibited by acetyl CoA, which accumulates when it is produced faster than it can be oxidized by citric acid cycle. The enzyme is also inhibited by elevated levels of NADH+.H, which occure when the electron transport chain is overloaded with substrate and oxygen is limited. 2- Covalent modification: The pyruvate dahydrogenase complex exists in two forms: an active nonphosphorylated form and an inactive phosphorylated form.Phosphorylated and nonphosphorylated pyruvate dehydrogenase can be interconverted by two separate enzymes, a kinase and a phosphatase. The kinase is activated by increase in the ratio of acetylCoA/ CoA or NADH/ NAD+. An increase in the ratio of ADP/ATP, which signals increased demand for energy production , inhibits the kinase and allows the phosphatase to produce more of the active ,nonphosphorylated enzyme. CLINICAL ASPECTS OF PYRUVATE METABOLISM: Inhibition of pyruvate metabolism leads to lactic acidosis, which may be due to : 1- Arsenite or mercuric ions complex the –SH group of lipoic acid. 2--Dietary deficiency of thiamin as in alcoholics. These two factors lead to inhibition of pyruvate dehydrogenase complex. 3- Inherited pyruvate dehydrogenase deficiency, which may be due to defects in one or more of the components of the enzyme complex. CITRIC ACID CYCLE TRICARBOXYLIC ACID CYCLE (KREB’S CYCLE) Def.: It is the series of reactions in mitochondria, which oxidized acetyl CoA to CO2, H2O & reduced H2 carriers (as NADH.H+ & FADH2) that oxidized through respiratory chains for ATP synthesis. Site: Mitochondria of all tissue cells except RBCs, which not contain mitochondria. The enzymes of the cycle are present in mitochondrial matrix except succinate dehydrogenase, which is tightly bound to inner mitochondrial membrane. Steps: ENERGY PRODUCTION: ENERGY PRODUCTION FROM OXIDATION OF ONE MOLECULE OF GLUCOSE: REGULATION OF KREB’S CYCLE: 1- As the primary function of TCA cycle is to provide energy, respiratory control via the E.T.C and oxidative phosphorylation exerts the main control. 2- In addition to this overall and coarse control, several enzymes of TCA cycle are also important in the regulation. Three key enzymes are: (a)Citrate synthase. (b)Mitochondrial isocitrate dehydrogenase. (c)α-ketoglutarate dehydrogenase. These enzymes are responsive to the energy status as expressed by the [ATP]/[ADP] ratio and [NADH]/[NAD+] ratio. (a)Citrate synthase enzymes is allosterically inhibited by ATP and long-chain acyl CoA. (b)NAD+-dependent mitochondrial iso-citrate dehydrogenase (ICD) is activated allosterically by ADP and is inhibited by ATP and NADH. (c)α-ketoglutarate dehyrogenase complex which allosterically inhibited by succinyl CoA, NADH-H+ and ATP. 3- In addition to above succinate dehydrogenase enzyme is inhibited by oxaloacetate (OAA) and the avability of OAA is controlled by malate dehydrogenase, which depends on [NADH]/[NAD+] ratio. FUNCTIONS OF KREB’S CYCLE 1- It is the final pathway for complete oxidation of all foodstuffs CHO, lipids • and protein, which are converted to acetyl CoA. 2- It is the major source of energy for cells except cells without mitochondria as RBCs. 3- It is the major source of succinyl CoA, which used for: 1.Porphyrine and HB synthesis. 2.Ketone bodies activation. 3.Converted to OAA → glucose. 4. Detoxication by conjugation 4- Synthetic functions of Kreb’s cycle:• a- Amphibolic reactions. Some components of Kreb’s cycle are used in synthesis of other substances as: In fasting state, oxaloacetic acid is used for synthesis of glucose by gluconeogenesis. In fed state, citric acid is used for synthesis of fatty acids. Reactions of Kreb’s cycle are used for synthesis of amino acid (transamination into non essential amino acids) eg: -OAA + glutamic acid aspartic acid + α-ketoglutarate. -Pyruvic acid + glutamic acid alanine + α-ketoglutarate. A anabolic role of the citric acid cycle b- Anaplerotic reactions.• Synthesis of one or more component of Kreb’s cycle from outside the cycle: O.A.A. can be synthesized from pyruvic acid by pyruvate carboxylase, and from aspartic acid by transamination. Fumarate can be synthesized from phenylalanine and tyrosine. Succinyl CoA can be synthesized from valine, isoleucine, methionine, and threonine. α-ketogluterate can be synthesized from glutamic acid by transamination. Inhibitors of Citric Acid Cycle 1-Flouro-acetate reacts with oxalacetate forming flourocitrate, which inhibits the aconitase enzyme. 2-Arsenite inhibits α-ketogluterate dehydrogenase. 3-Malonate acts as competitive inhibitor for succinate dehydrogenase. Major anaplerotic pathways of citric acid cycle ROLES OF VITAMINS IN CITRIC ACID CYCLE Four of the soluble vitamins of B complex have important roles in cirtic acid cycle. They are: 1-riboflavin, in the form of FAD, a cofactor in αketogluterate dehydrogenase complex and in succinate dehydrogenase; 2-niacin, in the form of NAD, the coenzyme for three dehydrogenases in the cycle, isocitrate dehydrogenase, α-ketogluterate dehydrogenase and malate dehydrogenase; 3-thiamin (vitamin B1), as TPP, the coenzyme for decarboxylation in α-ketogluterate dehyrdogenase reaction; and 4-pantothenic acid, as part of coenzyme A, which present in the form of acetyl-CoA and succinyl-CoA. CO2 fixation or carboxylation It is an addition of CO2 to the molecule in presence of CO2, biotin, Mn++, ATP, and specific carboxylase - CO2 is produced by α – ketoglutarate dehydrogenase , isocitrate dehydrogenase and pyruvate dehydrogenase complex examples for carboxylation :1-Pyruvic acid ATP Pyruvate carboxylase O.A.A biotin, Mn ++,CO2 ADP Propionyl CoA carboxylase → methylmalonyl CoA -D 2-PropionylCOA biotin ,Mn++ ,CO2 ATP L-MMCoA ADP CAC ← Succinyl CoA Acetyl CoA carboxylase 3- Acetyl CoA Malonyl CoA biotin ,Mn++ ,CO2 ATP 4- Pyruvic acid- ADP Malic enzym Biotin NADPH-H CO2 Malic acid 5- Synthesis of carbomyl phosphate of urea cycle and pyrimidine. 6- Formation of Carbon number 6 of purine. 7- Synthesis of H2CO3/NaHCO3 buffer system GLUCONEOGENESIS It is the formation of glucose from non CHO sources. Its main function is to supply blood glucose in cases of carbohydrate deficiency (fasting, starvation, and low carbohydrate diet). Sites: Cytoplasm and mitochondria of liver and kidney due to presence of glucose-6-phophatase and fructose-1, 6-biphosphatase. Steps: A.These mechanisms are concerned with conversion of glucogenic amino acids., lactate, glycerol, and propionic acid to glucose, which are reverse to glycolytic pathway (except for three irreversible kinases) to supply erythrocytes, skeletal muscles, nervous system, and mammary glands with their need of glucose. B.Energy barrier will obstruct reversal of glycolysis at the following sites: 1- Conversion of pyruvate to phosphoenol pyruvate This can be overcomed by dicarboxylic acid shuttle, as the following :1.In mitochondria, pyruvic acid is converted to oxalacetate in presence of pyruvate carboxylase, ATP, biotin, Mn++ and CO2. 2.Oxalacetate can not diffuse outside mitochondria → converted into compounds that can diffuse from mitochondria as malate, aspartate, and citrate → they are converted once again to oxalacetate in extramitochondria portion of the cells. -Oxalacetate reformed in extramitochondria compartment is converted to phosphoenol pyruvate in presence of phosphoenol pyruvate carboxykinase enzyme and GTP. Phosphoenol pyruvate Carbocxykinase Oxalacetate Pyruvic acid Aspartate Malate Citrate Pyruvate 2CO ATP ++ Mn Mitochondria Pyruvate carboxylase Attachment to acetyl CoA Citrate ADP NH2 Oxalacetic acid Transamination Reduction H2 Aspartic acid Malate 2- Conversion of fructose 1:6 biphosphate to F-6-P: This occurs by fructose 1:6 biphosphatase, which present in liver and kidneys. 3- Conversion of Glucose-6-P to glucose: This is catalysed by another enzyme, which is G-6-Phosphatase that is present in liver, intestine, and kidney. Carbon sources for glucoeogenesis: 1- Propionic acid: 1.It is the product of odd number fatty acid oxidation by β oxidation. 2.It is converted into succinyl CoA, which converted into oxalacetic acid → phosphoenol pyruvic →→Glucose. 2- Glycerol: glycerol-3-P converted into dihydroxy acetone-P, which can be converted by trio’s isomerase into glyceraldehydes-3-P→→→ glucose. Glycerokinase is present in liver and kidney mainly 3- Glucogenic amino acids: Amino acids by deamination can be converted into α-keto acids as pyruvic, α-ketoglutaric and OAA → they can be converted into glucose. Proteins are considered as one of the main sources of blood glucose especially after 18 hours due to deplation of liver glycogen. 4- Lactic acid: In vigorous skeletal muscle activity, large amount of lactic acid produced → passes to the liver through blood stream → converted in liver into pyruvic acid and lastly to glucose → reach muscle once again through blood → this cycle called Cori cycle. Importance of Cori cycle: •It prevents loss of lactate as waste products in urine. •Oxidation of reduced NAD. •It supplies red cells and contracting muscles with glucose for reutilization and ATP production. •Prevent accumulation of lactic acid, which change pH of blood. 5- Glucose-alanine cycle: During starvation there is muscle protein catabolism →in presence of NH3 and pyruvic acid (produced from glycolysis), alanine is formed →reach liver and converted into pyruvic acid, which give glucose through glucogenesis and NH3 which converted into urea →excreted in urine. Significant of glucose alanine cycle: •Disposal of NH3 produced from muscle protein catabolism through formation of urea, which excreted in urine. •Conserve NAD/NADH.H+ ratio. REGULATION OF GLUCONEOGENESIS Key enzymes which regulate gluconeogeneis are: Pyruvate carboxylase, Phospho-enol-Pyruvate carboxykinase (PEPCK), Fructose-1, 6-biphosphatase and Glucose-6-phosphatase. A -short time regulation:- 1- Effect of increased fatty acid oxidation on gluconeogenesis : Fasting, low carbohydrates in diet, stress and sever muscular exercise stimulate secretion of anti-insulin hormones which increase lipolysis in adipose tissues. The increased fatty acids oxidation acts as a signal to inhibit glycolysis and stimulate gluconeogenesis in the liver by the following mechanisms: *It increases the production of ATP which produce allosteric inhibition of phosphofructokinase-1 (PFK-1) and pyruvate kinase. *The excess acetyl-CoA, produced by fatty acid oxidation allosterically stimulate pyruvate carboxylase and inhibites pyruvate dehydrogenase thus direct pyruvate to gluconeongesis. *Excess citrate (produced from acetyl CoA) produces allosteric inhibition of PFK-1 and PFK-2. . 2- Fructose 2,6-bisphosphate plays a unique role in the regulation of glycolysis and gluconeogenesis in liver Fructose 2,6 bisphosphate is formed by phosphorylation of fructose 6-phosphate by PFK-2, the same enzyme is also responsible for its breakdown, since it has fructose 2,6 bisphosphatase activity. Fructose 2,6 bisphosphatase (bifunctional enzyme ) is under the allosteric control of fructose 6-phosphate which stimulate kinase and inhibit phosphatase. Carbohdrate feeding and insulin stimulate PFK-2 and inhibite fructose 2,6 bisphosphatase, producing accumulation of fructose 2,6 bisphosphate which produce allosteric activation of glycolytic key enzyme PFK-1 and allosteric inhibition of gluconeogenesis key enzyme fructose 1,6 bisphosphatase. In fasting state, glucagons stimulate production of cAMP which activate cAMP dependent protein kinase-A which in turn inactivates PFK-2 and activate fructose 2,6 bisphosphatase. Hence gluconeogenesis is stimulated by decrease in the concentration of fructose 2,6 bisphosphate which inactivate PFK-1 and relieves the inhibition of Fructose 1,6 bisphosphate. Control of glycolysis and gluconeogenesis in liver by fructose 2,6- bisphosphate Gluconeogenesis favoured ATP PFK-2 PFK-2 ADP F2-6Bp ATP Fructose-6-p ATP + PFK-1 ADP P F-1,6 Bpase F-1,6-bisphosphate glycolysis ADP F2-6Bp B- long time regulation:- Glucagon and insulin also have longterm effects on hepatic glycolysis and gluconeogenesis by induction and repression of key enzymes of both pathway. A high glucagon/insulin ratio in blood increases the capacity for gluconeogenesis and decreases that for glycolysis in liver. A low glucagon/insulin ratio has the opposite effects. Glucagon signals induction of greater quantities of PEP carboxykinase, Fructose 1,6 bisphosphatase and glucose 6-phosphatase. Pentose phosphate pathway Definition •The penstose phosphate pathway is an alternative rout for the metabolism of glucose, ATP neither produced nor utilized. It is the pathway for formation of pentose phosphate. •The pentose phosphate pathway is also described as a shunt rather than pathway because it shunts (to move from one trak to another) hexoses from glycolysis forming pentoses, which may be cycled back into the pathway of glycolysis by conversion into fructose 6-phosphate and glycerldehde-3 phosphate and used for resynthesis of glucose-6 phospahte so named hexose monophosphate shunt is also phosphogluconate pathway. • It is a multicyclic process in which three molecules of glucose 6-phosphate give rise to : -Three molecules of Co2 -Three molecules of pentoses -6 molecular of NADPH The pentoses are rearranged to generate two molecules of glucose-6-phosphate and one molecule of glycerldehyde 3-phosphate . Site: occurs in cytoplasm of many tissues including liver, adipose tissues, adrenal, ovary, testis, red cell and retina The main functions of pentose shunt are: 1-Production of NADPH-H+, which used in: Synthesis of fatty acids and cholesterol. Reduction of oxidized glutathione. Activation of folic acid. 2-Formation of pentoses in the form of ribose-5 P, which used in: Synthesis of nucleotides either free as ATP, or polynucleotides as DNA and RNA. Synthesis coenzymes as FAD, NAD+. Steps: I- Oxidative irreversible reaction ( phase I) which include: •the oxidative portion of HMP consists of three reactions that lead to formation of ribulose-5-P, CO2 and two molecules of NADPH-H+ for each glucose-6 phosphate oxidized. 2- Non oxidative revesible reaction which include: a- Phase II: Ribulose-5-P by ribulose-5-phospho epimerase is converted into xylulose-5-P while by ribulose-5 phosphe isomerase is converted into ribose-5-P. b- phase III :pentose-5-P is converted into glyceraldehydes-3-P and fructose-6-P by transketolase and transaldolase. These enzymes create a reversible link between pentose phosphate pathway and glycolysis by catalyzing these 3 reactions. . Function of non oxidative reversible phase : Formation of different pentoses 5-P In skeletal muscles due to deficiency of G-6-pD, so muscle can synthesize ribose 5 phosphate from fructose-6-phosphate and glyceraldehydes 3-phosphate by pathway reversible to phase II. RBCs need more NADPH it than pentose-5 so convert three pentose-5-p into glycolytic intermediate. REGULATION OF PENTOSE PHOSPHATE PATHWAY ( PPP): 1- G-6-P dehydrogenase increased in amount when diet contains excess carbohydrates. 2- The regulatory enzymes of PPP are g-6-P dehydrogenase and lactonase enzymes.Insulin acts as inducer for their synthesis. 3- NADPH.H+ accumulation produces feedback inhibition of g-6dehydrogenase. PPP is the major sources of NADPH.H+ but there are 2 other sources for NADPH.H+ which present in cytoplasme: 1)cytoplasmic isocitrate dehydrogenase. 2)malic enzyme which convert malic acid into pyruvic acid ,CO2 and NADPH.H+ . 4- Depending on the needs of the cell, conversion of pentose-5-P to hexose-6-P can occure. The reaction favour the formation of glyceraldehydes-3-P → glycerol-3-P which used in synthesis of phosphoglycerides as triacylglycerol. Also glyceraldehydes-3-P can be converted to 2,3 diphosphoglycerate in RBCs which ↓↓ O2 association with HB→↑O2 dissociation to the tissues. Role of NADPH in Red blood cell: •Red blood cells need NADPH to maintain glutathione in reduced form to protect themselves from oxidizing agents. •The red cell is exposed to large amount of molecular oxygen. Some of the molecular oxygen is converted to superoxide and H2O2 that can cause irreversible damage to the cell. •Reduced glutathione, a strong reducing agent protects against damage by reducing H2O2 to H2O. •The role of NADPH is to maintain glutathione in reduced form which is essentially required to preserve the integrity of RBCs. It also keeps iron of the haemoglobin in reduced ferrous state and prevents formation of methaemoglobin Role of NADPH in disposal of H2O2 Deficiency of glucose 6-phosphate dehydrogenase. •Several types of X-linked inherited deficiency of the enzyme glucose-6phosphate dehydrogenase have been recognized. •Enzyme deficient cells have a lower rate of NADPH production, resulting in a deficiency of reduced glutathione (GSH) which is essential to maintain the integrity of erythrocyte membrane and for keeping HB in the ferrous state. •Most individuals who have G-6-pD mutation are asymptomatic. Some individuals develop haemolytic anaemia if they are exposed to : •Certain oxidant drugs e.g. Antibiotic (sulphamethoxazole), antimalarial (primaquine), Antipyretic (acetoaminiphen). •Certain type of infection: The inflammatory response of infection generate free radicals which can damage the red cells easily if G6-PD is deficient. •Favism (due to ingestion of fava beans) •Favism is the haemolytic anaemia due to ingestion of fava beans (broad beans) in individuals with G-6-pD deficiency •Fava beans contain the purine glycosides these compound react with glutathione leading to reduced level of glutathione (GSH). •Favism is not observed in all individuals with G-6-PD deficiency but all patients with favism have G-6-PD deficiency.