* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Ictal SPECT in patients with rapid eye movement
Neurogenomics wikipedia , lookup
Dual consciousness wikipedia , lookup
Neuroscience in space wikipedia , lookup
Visual selective attention in dementia wikipedia , lookup
Externalizing disorders wikipedia , lookup
Premovement neuronal activity wikipedia , lookup
Biology of depression wikipedia , lookup
Biology and consumer behaviour wikipedia , lookup
Abnormal psychology wikipedia , lookup
Neural correlates of consciousness wikipedia , lookup
Neuropsychopharmacology wikipedia , lookup
Sleep apnea wikipedia , lookup
Neuroscience of sleep wikipedia , lookup
Sleep deprivation wikipedia , lookup
Delayed sleep phase disorder wikipedia , lookup
Sleep and memory wikipedia , lookup
Obstructive sleep apnea wikipedia , lookup
Sleep paralysis wikipedia , lookup
Sleep medicine wikipedia , lookup
Effects of sleep deprivation on cognitive performance wikipedia , lookup
Rapid eye movement sleep wikipedia , lookup
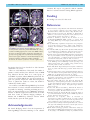
doi:10.1093/brain/awv042 BRAIN 2015: 138; 1263–1270 | 1263 Ictal SPECT in patients with rapid eye movement sleep behaviour disorder Geert Mayer,1,2 Marion Bitterlich,1 Torsten Kuwert,3 Philipp Ritt3 and Hermann Stefan4 See Mahowald and Schenck for a scientific commentary on this article (doi:10.1093/brain/awv058). Rapid eye movement sleep behaviour disorder is a rapid eye movement parasomnia clinically characterized by acting out dreams due to disinhibition of muscle tone in rapid eye movement sleep. Up to 80–90% of the patients with rapid eye movement sleep behaviour disorder develop neurodegenerative disorders within 10–15 years after symptom onset. The disorder is reported in 45– 60% of all narcoleptic patients. Whether rapid eye movement sleep behaviour disorder is also a predictor for neurodegeneration in narcolepsy is not known. Although the pathophysiology causing the disinhibition of muscle tone in rapid eye movement sleep behaviour disorder has been studied extensively in animals, little is known about the mechanisms in humans. Most of the human data are from imaging or post-mortem studies. Recent studies show altered functional connectivity between substantia nigra and striatum in patients with rapid eye movement sleep behaviour disorder. We were interested to study which regions are activated in rapid eye movement sleep behaviour disorder during actual episodes by performing ictal single photon emission tomography. We studied one patient with idiopathic rapid eye movement sleep behaviour disorder, one with Parkinson’s disease and rapid eye movement sleep behaviour disorder, and two patients with narcolepsy and rapid eye movement sleep behaviour disorder. All patients underwent extended video polysomnography. The tracer was injected after at least 10 s of consecutive rapid eye movement sleep and 10 s of disinhibited muscle tone accompanied by movements registered by an experienced sleep technician. Ictal single photon emission tomography displayed the same activation in the bilateral premotor areas, the interhemispheric cleft, the periaqueductal area, the dorsal and ventral pons and the anterior lobe of the cerebellum in all patients. Our study shows that in patients with Parkinson’s disease and rapid eye movement sleep behaviour disorder—in contrast to wakefulness—the neural activity generating movement during episodes of rapid eye movement sleep behaviour disorder bypasses the basal ganglia, a mechanism that is shared by patients with idiopathic rapid eye movement sleep behaviour disorder and narcolepsy patients with rapid eye movement sleep behaviour disorder. 1 2 3 4 Hephata Klinik, Department of Neurology, Schimmelpfengstr.6, 34613 Schwalmstadt-Treysa, Germany Philipps University Marburg, Department of Neurology, Baldingerstrasse, 35043 Marburg, Germany University of Erlangen, Department of Nuclear Medicine, Ulmenweg 18, 91054 Erlangen, Germany University of Erlangen, Department of Neurology, Schwabachanlage 6, 91054 Erlangen, Germany Correspondence to: Geert Mayer, Hephata Klinik, Schimmelpfengstr. 6, 34613 Schwalmstadt-Treysa, Germany E-mail: [email protected] Keywords: REM sleep behaviour disorder; ictal SPECT; basal ganglia; muscle atonia; sublaterodorsal nucleus Abbreviations: DTI = diffusion tensor imaging; HLA = human leukocyte antigen; REM = rapid eye movement; SPECT = single photon emission tomography Received September 8, 2014. Revised December 21, 2014. Accepted December 22, 2014. Advance Access publication March 2, 2015 ß The Author (2015). Published by Oxford University Press on behalf of the Guarantors of Brain. All rights reserved. For Permissions, please email: [email protected] 1264 | BRAIN 2015: 138; 1263–1270 Introduction Rapid eye movement (REM) sleep behaviour disorder is a parasomnia characterized by acting out dreams with screaming, hitting, thrashing and frequent self-injury. It has gained major attention because 81% of the patients with the idiopathic REM sleep behaviour disorder form convert within 10–15 years after onset to neurodegenerative disease such as Parkinson’s disease, multisystem atrophy, or dementia of the Lewy bodies (Schenck et al., 2013). Patients with idiopathic REM sleep behaviour disorder frequently show signs and symptoms associated with an increased risk of developing -synucleinopathy, e.g. hyposmia, depression, constipation, and hyperechogenicity of the substantia nigra (Stiasny-Kolster et al., 2005; Postuma et al., 2010, 2011). To date the best biomarker of REM sleep behaviour disorder is the amount of loss of muscle tone inhibition during REM sleep (REM sleep without atonia). Among the symptomatic REM sleep behaviour disorder forms, narcolepsy has a high association with REM sleep behaviour disorder. This form is less violent than idiopathic REM sleep behaviour disorder although in videometric evaluation, movements are not different compared to patients with idiopathic REM sleep behaviour disorder and Parkinson’s disease plus REM sleep behaviour disorder (Oudiette et al., 2012). Recently the European Narcolepsy Network studied 1099 HLA DQB1*0602 positive patients with clear-cut narcolepsy cataplexy retrospectively (Luca et al., 2013). In a subgroup of 295 patients who underwent polysomnography, 43% of the males and 54% of the females had REM sleep behaviour disorder, which is a much higher amount of affected females than in idiopathic REM sleep behaviour disorder. Little is known whether idiopathic and symptomatic REM sleep behaviour disorder share the same pathophysiology (Unger et al., 2010). Neuropathological studies of patients with idiopathic REM sleep behaviour disorder reveal the presence of Lewy bodies, a pathological accumulation of -synuclein in the brainstem (Iranzo et al., 2013). Narcolepsy patients with RBD show symptoms like hyposmia (Stiasny-Kolster et al., 2007), depression, constipation and hyperechogenicity of substantia nigra (Unger et al., 2009); however, the underlying pathology is the loss of hypocretinergic neurons. These neurons in the dorsolateral hypothalamus are vulnerable to damage by genetic, autoimmune, inflammatory or traumatic factors. In recent animal studies the sublaterodorsal nucleus (Lu et al., 2006; Clement et al., 2011) was identified as the nucleus being responsible for motor disinhibition in REM sleep. Reciprocal GABAergic connections between the sublaterodorsal (Lu et al., 2006) and the ventrolateral periaqueductal grey create a ‘flip-flop’ model for the switches between non-REM and REM sleep. The ventrolateral periaqueductal grey and surrounding areas are a REM-off region with inhibitory GABAergic efferents to the sublaterodorsal nucleus (Boissard et al., 2002, 2003; Pollock et al., 2003), whereas GABAergic REM-on nuclei G. Mayer et al. in the dorsal paragigantocellular reticular nucleus and the ventrolateral periaqueductal grey inhibit the REM-off regions (Rampon et al., 1999; Gervasoni et al., 2000; Verret et al., 2006).The sublaterodorsal nucleus has glutamatergic efferents (Krenzer et al., 2011) and receives glutamatergic input from the lateral periaqueductal grey and ventrolateral periaqueductal grey (Beitz, 1990), the primary motor area of the frontal cortex, the bed nucleus of the stria terminalis and the central nucleus of the amygdala (Boissard et al., 2003). Muscle atonia during REM can be explained by direct glutamatergic projection from the sublaterodorsal to the ventral horn, activating glycinergic and/or GABAergic spinal interneurons in lamina VIII of the ventral spinal horn (Krenzer et al., 2011) or by sublaterodorsal projections to the ventromedial medulla (Vetrivelan et al., 2009). A large population of REM-on GABAergic neurons in the gigantocellular nucleus and raphe magnus nucleus indicate that this medullary area, which has projections to the spinal cord, is responsible for motor inhibition during REM sleep (Sapin et al., 2009). Sublaterodorsal nucleus lesions can reduce excitation of the medullary magnocellular reticular formation resulting in a reduced inhibition of spinal motor neurons. Several imaging studies have been performed in patients with idiopathic REM sleep behaviour disorder in the recent years. MRI diffusion tensor imaging (DTI) alterations in the pons, the right substantia nigra, the olfactory region, the thalamic radiation in the anterior limb of the capsule, the left temporal lobe, the right occipital lobe and the fornix have been reported (Unger et al., 2010; Scherfler et al., 2012). Garcia-Lorenzo et al. (2013) found structural changes in the coeruleus/subcoeruleus complex correlating with abolished muscle atonia during REM sleep. A recent study found altered functional connectivity between the substantia nigra and the putamen that was more impaired in patients with Parkinson’s disease than in patients with REM sleep behaviour disorder (Holtbernd et al., 2014). In patients with narcolepsy/cataplexy, DTI showed microstructural changes in the hypothalamus, mesencephalon, pons and medulla oblongata (Menzler et al., 2012). Within recent years, a few case reports on neurodegeneration in narcolepsy patients have been published (Economou et al., 2012; Scammell et al., 2012). Scammell et al. (2012) found evidence of Alzheimer’s disease in the brains of 12 deceased narcoleptic patients. Christine et al. (2012) found three narcoleptic patients in a cohort of 1152 patients with Parkinson’s disease, a number that is five times greater than expected. Within the past 15 years we have followed-up patients with idiopathic REM sleep behaviour disorder, narcolepsy with and without REM sleep behaviour disorder. Whereas many of the patients with idiopathic REM sleep behaviour disorder showed clinical signs of neurodegeneration, only 3 of 12 narcolepsy patients with REM sleep behaviour disorder that we followed from 2003 to 2013 (Mayer et al., Ictal SPECT in REM sleep behaviour disorder 2013) developed mild signs of Parkinson’s disease. To study the pathways of REM sleep behaviour disorder in vivo we performed ‘ictal’ single photon emission tomography (SPECT) immediately at the onset of REM sleep behaviour disorder in four patients. Materials and methods Recording was performed in the hospital as video-EEG longterm polysomnography (PSG) using an IT-Med System l. The following parameters were used for documentation: 22 channel EEG (including C3-mastoid and C4 to mastoid); EOG (four channels), respiration (nasal and oral thermistor, thoracal and abdominal effort), bilateral EMGs of musculus mentalis, musculus extensor digitorum brevis, musculus flexor digitorum brevis, musculus tibialis anterior and musculus gastrocnemius. A one-channel ECG was recorded. The polysomnography was performed under continuous observation by experienced medical staff. Ictal and interictal subtraction SPECT was performed after using a semi-automatic SPECT injection device permitting immediate intravenous application of the radioligand ECD (ethyl cysteinate dimer) with a latency 510 s between onset of clinical event and injection. SPECT scanning was carried out after the injection. For the SPECT acquisitions, the patients were injected with on average 898 (741–1210) MBq Tc-99m ECD (NEUROLITEÕ , Bristol-Myers Squibb). The time of injection for the ictal examinations was determined by EEG: REM sleep had to last for a minimum of 10 epochs, and complex behaviour in REM sleep had to be manifest for at least 10 epochs (Fig. 1). The interictal injection was started after at least 15 min resting conditions. The acquisitions began 30 min after the injection and were carried out on a MultiSpect 3 (Siemens Molecular Imaging) with low-energy high-resolution collimation. Counts were collected in an energy window of 140 keV, 10% over 120 views (40 per detector, every 3 ) with 25 s per view, a matrix size of 128 128 and a zoom of 1.23. The views were reconstructed into 3D data sets using filtered back projection with a Butterworth filter of fifth order and cut-off frequency of 0.6 Nyquist. Further corrections for scattered radiation were not applied. The photon attenuation was corrected using Chang’s algorithm, assuming a homogenously attenuating medium. In a post-processing step, the ictal and interictal reconstructed data sets were subtracted pixelwise from each other for every patient, after spatial co-registration and intensity normalization. Negative values were discarded, so that we obtained difference images that represented ictal hyperperfusion. Additionally, the difference images were coregistered to MRI images, for better anatomical assignment of the hyperperfusion. The method has been published previously; more details can be found in Hahn et al. (2009). The study was approved by the ethical committee of the Chamber of Physicians Hessen. All patients gave signed informed consent. Demographics We studied one patient with idiopathic REM sleep behaviour disorder, one patient with Parkinson’s disease and REM sleep behaviour disorder and two patients with long-standing BRAIN 2015: 138; 1263–1270 | 1265 narcolepsy/cataplexy and REM sleep behaviour disorder. All patients met the diagnostic criteria for REM sleep behaviour disorder and narcolepsy according to International Classification of Sleep Disorders, 2 (American Academy of Sleep Medicine, 2005). The female patient with idiopathic REM sleep behaviour disorder was diagnosed 20 years ago and had subsequently developed signs of full-blown Parkinson’s disease (Hoehn and Yahr stage 4) at the time of investigation. The patient demographic data are shown in Table 1. The movements during REM sleep prior to injection of the tracer are shown in Table 2. Results All patients, independent of their REM sleep behaviour disorder type, displayed a similar pattern of activation in the ictal SPECT. The activation included the bilateral premotor areas, the interhemispheric cleft, the periaqueductal area, the dorsal and ventral pons and the anterior lobe of the cerebellum (Figs 2–5). The thalamus was activated in the female narcolepsy patient with REM sleep behaviour disorder (Fig. 5). Because of the ‘smearing’ principle of the filtered back projection reconstruction, some small amounts of residual activity can be projected outside of a patient’s skull, which is an artefact of the method. Discussion To our knowledge this is the first study to report results of ictal SPECT in patients with idiopathic REM sleep behaviour disorder, Parkinson’s disease (preceded by REM sleep behaviour disorder) and patients with narcolepsy and REM sleep behaviour disorder. Interestingly, the different forms use the same pathways and activate the same cortical and brainstem areas sparing the basal ganglia. This finding is surprising as the basal ganglia are involved in the neural loops of motor activity. The activated cortical, brainstem and cerebellar areas represent a network of structures responsible for motor activity, REM sleep, muscle tone during sleep and coordination. The involved structures have been described in animal studies (Krenzer et al., 2011; Luppi et al., 2011), post-mortem studies (Boeve et al., 2007; Dugger et al., 2012) and imaging studies (Unger et al., 2010) in humans. However, most of the studies on neural connectivity of movements in healthy subjects have been performed during the wake state, which makes comparison to movements in REM sleep difficult, if not impossible. In healthy subjects, voluntary leg movements during wake, as measured by blood oxygen level-dependent functional MRI, result in activations in the primary sensorimotor cortex, the supplementary motor area, cingulate motor area, the anterior cerebellar vermis, both cerebellar hemispheres, thalamus, and right putamen (Jaeger et al., 2014). Functional MRI studies using a finger tapping 1266 | BRAIN 2015: 138; 1263–1270 G. Mayer et al. Table 1 Demographic and test data Patient Age Sex Diagnosis Co-morbid years of RBD diseases CR 64 F Clinical PSG RD 65 M MH 63 F CF 41 F Clinical PSG Clinical PSG Clinical PSG RBD Duration Cataplexy MSLT: Number TDI Olfactory Any UPDRS Hyperech MMSE duration narcolepsy SL min SOREM dysfunction EMG III SN years years PD, sleep 24 apnoea, hypertension Sleep 10 apnoea Narcolepsy 14 Narcolepsy 30 NA NA NA NA NA NA NA NA 29 1 5.5 3 30 1 1.1 3 13 Severe 58.8 21 Y 29 Severe 17 0 Y 30 26.5 Mild 67.1 6 Y 28 27 67.2 0 Y 28 Mild Any EMG = 30 s epochs containing phasic and/or tonic muscle activity in REM; Hyperch SN = hyperechogeneity of substantia nigra; MMSE = Mini-Mental State Examination; MSLT = multiple sleep latency test (five tests); PD = Parkinson’s disease; PSG = polysomnography; SOREM = sleep onset REM; UPDRS III = Unified Parkinson’s Disease Rating Scale: motor score; RBD = REM sleep behaviour disorder; SL = sleep latency; TDI = threshold-discrimination-identification. Table 2 Behaviour of patients before and after tracer injection Patient Behaviour prior to tracer injection Behaviour after tracer injection CR RD MH CF Kicking with legs, shouting Twitching of both arms, spreading arms (right 4 left arm) Talking, twitching of arms and legs, grimacing Talking, kicking first left then right foot Kicking, punching, rocking movements Grasps for bedded grid, shaking it strongly, fumbling of hands Kicking of legs, movements of pelvis, grasping Shouting, kicking with feet, punching movements of arms paradigm showed hypo-activation in the bilateral putamen, right supplementary motor area and hyperactivation in the right premotor cortex in patients with Parkinson’s disease, which was considered to be a disruption of the corticostriatal processing (Taniwaki et al., 2013). In our patients the bilateral activation of the premotor (supplementary motor) areas shows the cortical activation of disinhibited motor activity in REM sleep. Whether this is due to activation by GABAergic or glutamatergic inputs from the ‘dysfunctional’ sublaterodorsal nucleus or primarily from the cortex needs to be answered by other methods than ictal SPECT. The activation of the interhemispheric motor cortex is in-line with the video polysomnographies prior to injection of the radioligand, which show movements in REM sleep in the lower limbs of three patients. The areas of the dorsal medulla may represent the region of the periaqueductal grey and the sublaterodorsal that are involved in the ‘REM-on’ mechanism. The activation of the anterior pontine region could represent the downstream inhibition of muscle tone during REM sleep by glycinergic mechanisms. The activation of the cerebellum is more difficult to attribute to the known pathophysiology of REM sleep behaviour disorder, because the literature is scarce. A recent study showed reduced grey matter volume of the anterior lobes of both cerebellar hemispheres and the tegmental portion of the pons in patients with REM sleep behaviour disorder compared to healthy controls (Hanyu et al., 2012). This loss of grey matter is also found in synucleinopathies. Patients with dementia of the Lewy body type showed specific atrophy in the midbrain, pons and cerebellum in comparison to patients with Alzheimer’s disease (Nakatsuka et al., 2013). The anterior cerebellum is responsible for the fine motor regulation and the timing of movements. Based on these findings, we hypothesize that the cerebellar activation that we found in our study affects an atrophic cerebellum and results in an impaired coordination in REM sleep behaviour disorder patients with short, jerky and non-fluent movements. This movement pattern does not differ between REM sleep behaviour disorder patients with Parkinson’s disease, idiopathic REM sleep behaviour disorder, and REM sleep behaviour disorder in primary narcolepsy (Oudiette et al., 2012), suggesting a common motor pathway. Despite being non-fluent and jerky the movements of Parkinson’s disease patients with REM sleep behaviour disorder during REM sleep contrast with the typical hypokinetic parkinsonian movements during wakefulness (De Cock et al., 2007). This contrast has triggered the hypothesis that movements in REM sleep behaviour disorder are generated by the motor cortex bypassing the extrapyramidal tract. Our study seems to confirm this hypothesis in patients with Parkinson’s disease and REM sleep behaviour disorder and idiopathic REM sleep behaviour disorder. This hypothesis is of further interest as REM sleep is accompanied by typical EEG changes that are caused by cortical activation, and which are mediated by glutamatergic projections from REM-on regions in the brainstem (Luppi et al., 2012). If the degenerative changes in the brainstem can explain an activation of the motor cortex, this needs to be clarified by future studies. The REM sleep behaviour disorder movement Ictal SPECT in REM sleep behaviour disorder BRAIN 2015: 138; 1263–1270 | 1267 Figure 1 Polysomnography before, at and after tracer injection. Muscle activity of musculus mentalis started 12 epochs prior to injection of ECD tracer (blue line) and was accompanied by intermittent muscle activity of musculus mentalis (450%/epoch) and kicking movements of the left, followed by the right leg. F8–P3 = scalp electrodes for EEG recordings; VER1/2 = vertical eye movements; HOR1/2 = horizontal eye movements; NASAL = nasal flow; THORAKAL = thoracal excursion; ABDOMINA = abdominal excursion; EMG and EMG3 = mentalis muscle; EXT1/2 = musculus extensor digitorum brevis; FLEX1/2 = musculus flexor digitorum brevis; TA1/2 = musculus tibialis anterior; GAST1/2 = musculus gastrocnemius. pattern has never been explained sufficiently by animal or human studies. It can be hypothesized that it could be caused by instability of the activation of the sublaterodorsal nucleus, possibly depending on a certain threshold of afferent inputs. Recently two cell groups were identified during pharmacologically-induced REM sleep-like episodes in rodents (Stettner et al., 2013): the adrenergic cells of the C1 group and the cells of the lateral reticular nucleus. C1 cells are activated during REM sleep whereas lateral reticular nucleus cells are silent. Lateral reticular nucleus neurons belong to the spinoreticulo-cerebellar pathway in which the intended and actual movements are compared to allow corrections to enable swift movements. An impaired spinoreticular pathway and the reduction of the grey matter of the anterior lobe of the cerebellum may be the cause of the absence of smooth movements and walking during REM sleep without atonia. Activation of the thalamus was found in one narcolepsy patient. This finding differs from SPECT studies in normal REM sleep of narcolepsy patients, which is characterized by decreased blood flow in the thalamus (Asenbaum et al., 1995). In humans, a recent study of the brains of three patients with REM sleep behaviour disorder that had developed Parkinson’s disease and dementia of the Lewy body type (Iranzo et al., 2013) showed moderate to severe neuronal loss, gliosis, Lewy bodies, and Lewy neurites in the brainstem (especially in the coeruleus/subcoeruleus, pons, dorsal nucleus of the vagal nerve) and limbic system, and to a lesser extent in cortical areas. This finding is in-line with the results of imaging studies. Neurodegeneration is also present in patients with narcolepsy, as could be shown by DTI (Menzler et al., 2012). A longitudinal study in patients with narcolepsy without cataplexy, with intermediate hypocretin-1 in the CSF, has shown that many develop cataplexy up to 26 years after the onset of excessive daytime sleepiness, meaning that a critical threshold of age- 1268 | BRAIN 2015: 138; 1263–1270 G. Mayer et al. Figure 2 Ictal SPECT of Patient CR, female with Parkinson’s disease with REM sleep behaviour disorder. Difference images of cerebral perfusion, measured by Tc-99m ECD SPECT (in colour), overlaid on T1-MRI (greyscale). The colour of the SPECT indicates the degree of ictal hyperperfusion, ranging from weak (blue and green) to strong (orange and red). The arrows indicate hyperperfusion in brain regions. Median, precentral activation (premotor area), activation of left brainstem and right anterior cerebellum. A =anterior; H =head; P =posterior; F =foot; R=right; L =left. Figure 3 Ictal SPECT of Patient RD, male with idiopathic REM sleep behaviour disorder. Difference images of cerebral perfusion, measured by Tc-99m ECD SPECT (in colour), overlaid on T1-MRI (greyscale). The colour of the SPECT indicates the degree of ictal hyperperfusion, ranging from weak (blue and green) to strong (orange and red). The arrows indicate hyperperfusion in brain regions. Bifrontal activation in premotor area, pons and anterior cerebellum. A =anterior; H =head; P =posterior; F =foot; R =right; L=left. Figure 4 Ictal SPECT Patient MH, female with narcolepsy with REM sleep behaviour disorder. Difference images of cerebral perfusion, measured by Tc-99m ECD SPECT (in colour), overlaid on T1-MRI (greyscale). The colour of the SPECT indicates the degree of ictal hyperperfusion, ranging from weak (blue and green) to strong (orange and red). The arrows indicate hyperperfusion in brain regions. Activation of median interhemispheric cleft, bilateral activation of brainstem and left vermis. A =anterior; H =head; P =posterior; F =foot; R =right; L=left. dependent degeneration of hypocretinergic cells may have occurred (Andlauer et al., 2012). DTI in narcoleptic patients has found microstructural changes of the hypothalamus, mesencephalon, pons and medulla oblongata. Our findings do not show involvement of the substantia nigra, as in awake patients with idiopathic REM sleep behaviour disorder (Unger et al., 2009; Scherfler et al., 2012). In contrast to all the neural networks of REM sleep behaviour disorder found during wakefulness (Holtbernd et al., 2014), our findings show no involvement of the basal ganglia. The activation of this different connectivity could be one explanation for a more fluent behaviour of patients with Parkinson’s disease and REM sleep behaviour disorder during REM sleep. SPECT is only one among many methods to display activation of brain areas in actual states. It does not show the process causing activation and localization is not very precise. Therefore investigations identifying neurotransmitters involved in the activation of this neural network must be carried out. In contrast to idiopathic REM sleep behaviour disorder, and Parkinson’s disease and REM sleep behaviour disorder, which are considered to be -synucleinopathies in narcolepsy with REM sleep behaviour disorder, hypocretins are involved in the pathology as confirmed in animal and human studies (Knudsen et al., 2010). The activation of the thalamus in one patient is the opposite of the Ictal SPECT in REM sleep behaviour disorder BRAIN 2015: 138; 1263–1270 | 1269 comments. We express our gratitude to PD Dr. Matthias Dütsch for technical assistance during SPECT application. Funding No funding was received for this work. References Figure 5 Ictal SPECT Patient CF, female with narcolepsy with REM sleep behaviour disorder. Difference images of cerebral perfusion, measured by Tc-99m ECD SPECT (in colour), overlaid on T1-MRI (greyscale). The colour of the SPECT indicates the degree of ictal hyperperfusion, ranging from weak (blue and green) to strong (orange and red). The arrows indicate hyperperfusion in brain regions. Activation of median interhemispheric cleft, asymmetric activation of brainstem, activation of thalamus. A =anterior; H =head; P =posterior; F =foot; R =right; L=left. deactivation that has been described in older literature (Asenbaum et al., 1995). There are some limitations of this study: the number of patients is small, and they have different forms of REM sleep behaviour disorder. There is no control group, as ictal SPECT in patients without REM sleep behaviour disorder is not possible. SPECT does not show anatomic regions very precisely. Despite the small and heterogeneous cohort of patients the results are robust, but should be confirmed by further studies. In conclusion, ictal SPECT during REM sleep has shown that a network of cortical, cerebellar and brainstem areas— responsible for initiating, controlling and timing motor activity—are activated in the process of REM sleep behaviour disorder of different origin. The activated areas are in-line with those found by different imaging techniques in humans and in REM sleep behaviour disorder animal models, but they spare the basal ganglia. Acknowledgements We thank Wolfgang Oertel from the Department of Neurology/Philipps University Marburg for his valuable American Academy of Sleep Medicine. The international classification of sleep disorders: diagnostic and coding manual. 2nd edn. Westchester, Illinois: American Academy of Sleep Medicine; 2005. Andlauer O, Moore H, Hong SC, Dauvilliers Y, Kanbayashi T, Nishino S, et al. Predictors of hypocretin (orexin) deficiency in narcolepsy without cataplexy. Sleep 2012; 35: 1247–55. Asenbaum S, Zeithofer J, Saletu B, Frey R, Brucke T, et al. Technetium-99m-HMPAO SPECT imaging of cerebral blood flow during REM sleep in narcoleptics. J Nucl Med 1995; 36: 1150–5. Beitz AJ. Relationship of glutamate and aspartate to the periaqueductal gray-raphe magnus projection: analysis using immunocytochemistry and microdialysis. J Histochem Cytochem 1990; 38: 1755–65. Boeve BF, Silber MH, Saper CB, Ferman TJ, Dickson DW, Parisi JE, et al. Pathophysiology of REM sleep behaviour disorder and relevance to neurodegenerative disease. Brain 2007; 130: 2770–88. Boissard R, Gervasoni D, Schmidt MH, Barbagli B, Fort P, Luppi PH. The rat ponto-medullary network responsible for paradoxical sleep onset and maintenance: a combined microinjection and functional neuroanatomical study. Eur J Neurosci 2002; 16: 1959–73. Boissard R, Fort P, Gervasoni D, Barbagli B, Luppi PH. Localization of the GABAergic and non-GABAergic neurons projecting to the sublaterodorsal nucleus and potentially gating paradoxical sleep onset. Eur J Neurosci 2003; 18: 1627–39. Christine CW, Marks WJ Jr, Ostrem JL. Development of Parkinson’s disease in patients with Narcolepsy. J Neural Transm 2012; 119: 697–9. Clement O, Sapin E, Berod A, Fort P, Luppi PH. Evidence that neurons of the sublaterodorsal tegmental nucleus triggering paradoxical (REM) sleep are glutamatergic. Sleep 2011; 34: 419–23. De Cock VC, Vidailhet M, Leu S, Texeira A, Apartis E, Elbaz A, et al. Restoration of normal motor control in Parkinson’s disease during REM sleep. Brain 2007; 130 (Pt 2): 450–6. Dugger BN, Murray ME, Boeve BF, Parisi JE, Benarroch EE, Ferman TJ, et al. Neuropathological analysis of brainstem cholinergic and catecholaminergic nuclei in relation to rapid eye movement (REM) sleep behaviour disorder. Neuropathol Appl Neurobiol 2012; 38: 142–52. Economou NT, Manconi M, Ghika J, Raimondi M, Bassetti C. Development of Parkinson’s and Alzheimer diseases in two cases of narcolepsy-cataplexy. Eur Neurol 2012; 67: 48–50. Holtbernd F, Gagnon J-F, Postuma RB, Ma Y, Tang CC, Feigin A, et al. Abnormal metabolic network activity in REM sleep behavior disorder. Neurology 2014; 82: 620–27. Garcia-Lorenzo D, Longo-Dos Santos C, Ewenczyk C, Leu-Semenescu S, Gallea C, Quattrocchi G, et al. The coeruleus/ subcoeruleus complex in rapid eye movement sleep behaviour disorders in Parkinson’s disease. Brain 2013; 136 (Pt 7): 2120–9. Gervasoni D, Peyron C, Rampon C, Barbagli B, Chouvet G, et al. Role and origin of the GABAergic innervation of dorsal raphe serotonergic neurons. J Neurosci 2000; 20: 4217–25. Hahn D, Daum V, Hornegger J, Kuwert T. Data-driven density estimation applied to SPECT subtraction imaging for epilepsy diagnosis. In: Proceedings of the MICCAI workshop on probabilistic models 1270 | BRAIN 2015: 138; 1263–1270 for medical image analysis (Medical image computing and computer-assisted intervention -MICCAI 2009, 12th International Conference). London, 2009. p. 115–26. Hanyu H, Inoue Y, Sakurai H, Kanetaka H, Nakamura M, Miyamoto T, et al. Voxel-based magnetic resonance imaging study of structural brain changes in patients with idiopathic REM sleep behavior disorder. Parkinsonism Relat Disord 2012; 18: 136–9. Iranzo A, Tolosa E, Gelpi E, Molinuevo JL, Valldeoriola F, Serradell M, et al. Neurodegenerative disease status and post-mortem pathology in idiopathic rapid-eye-movement sleep behaviour disorder: an observational cohort study. Lancet Neurol 2013; 12: 443–53. Jaeger L, Marchal-Crespo L, Wolf P, Riener R, Michels Land Kollias S. Brain activation associated with active and passive lower limb stepping. Front Hum Neurosci 2014; 8: 828. Knudsen S, Jennum PJ, Alving J, Sheikh SP, Gammeltoft S. Validation of the icsd-2 criteria for csf hypocretin-1 measurements in the diagnosis of narcolepsy in the Danish population. Sleep 2010; 33: 169–76. Krenzer M, Anaclet C, Vetrivelan R, Wang N, Vong L, et al. Brainstem and spinal cord circuitry regulating REM sleep and muscle atonia. PLoS One 2011; 6: e24998. Lu J, Sherman D, Devor M, Saper CB. A putative flip-flop switch for control of REM sleep. Nature 2006; 441: 589–94. Luca G, Haba-Rubio J, Dauvilliers Y, Lammers GJ, Overeem S, Donjacour CE, et al. Clinical, polysomnographic and genome-wide association analyses of narcolepsy with cataplexy: a European narcolepsy network study. J Sleep Res 2013; 22: 482–95. Luppi PH, Clement O, Sapin E, Gervasoni D, Peyron C, Leger L, et al. The neuronal network responsible for paradoxical sleep and its dysfunctions causing narcolepsy and rapid eye movement (REM) behavior disorder. Sleep Med Rev 2011; 15: 153–63. Luppi PH, Clement O, Sapin E, Peyron C, Gervasoni D, Léger L, et al. Brainstem mechanisms of paradoxical (REM) sleep generation. Pflugers Arch 2012; 463: 43–52. Mayer G, Kesper K, Oertel W, Höffken H, Stiasny-Kolster K. REM Sleep behavior disorder (RBD) in narcolepsy patients as a predictor of neurodegeneration: results of a prospective clinical and imaging investigation. Sleep 2013; ; 36 (Suppl): A236. Menzler K, Belke M, Unger MM, Ohletz T, Keil B, Heverhagen JT, et al. DTI reveals hypothalamic and brainstem white matter lesions in patients with idiopathic narcolepsy. Sleep Med 2012; 13: 736–42. Nakatsuka T, Imabayashi E, Matsuda H, Sakakibara R, Inaoka T, Terada H. Discrimination of dementia with lewy bodies from Alzheimer’s disease using voxel-based morphometry of white matter by statistical parametric mapping 8 plus diffeomorphic anatomic registration through exponentiated Lie algebra. Neuroradiology 2013; 55: 559–66. Oudiette D, Leu-Semenescu S, Roze E, Vidailhet M, De Cock VC, Golmard JL, Arnulf I. A motor signature of REM sleep behavior disorder. Mov Disord 2012; 27: 428–31. Pollock MS, Mistlberger RE. Rapid eye movement sleep induction by microinjection of the GABA-A antagonist bicuculline into the dorsal subcoeruleus area of the rat. Brain Res 2003; 962: 68–77. Postuma RB, Gagnon JF, Vendette M, Desjardins C, Montplaisir JY. Olfaction and color vision identify impending neurodegeneration in rapid eye movement sleep behavior disorder. Ann Neurol 2011; 69: 811–18. G. Mayer et al. Postuma RB, Lanfranchi PA, Blais H, Gagnon JF, Montplaisir JY. Cardiac autonomic dysfunction in idiopathic REM sleep behavior disorder. Mov Disord 2010; 25: 2304–10. Rampon C, Peyron C, Gervasoni D, Pow DV, Luppi PH, Fort P. Origins of the glycinergic inputs to the rat locus coeruleus and dorsal raphe nuclei: a study combining retrograde tracing with glycine immunohistochemistry. Eur J Neurosci 1999; 11: 1058–66. Sapin E, Lapray D, Berod A, Goutagny R, Leger L, Ravassard P, et al. Localization of the brainstem GABAergic neurons controlling paradoxical (REM) sleep. PLoS One 2009; 4: e4272. Scammell TE, Matheson JK, Honda M, Thannickal TC, Siegel JM. Coexistence of narcolepsy and Alzheimer’s disease. Neurobiol Aging 2012; 33: 1318–19. Schenck CH, Boeve BF, Mahowald MW. Delayed emergence of a parkinsonian disorder or dementia in 81% of older men initially diagnosed with idiopathic rapid eye movement sleep behavior disorder: a 16-year update on a previously reported series. Sleep Med 2013; 14: 744–8. Scherfler C, Frauscher B, Schocke M, Nocker M, Gschliesser V, Ehrmann L, et al. White and gray matter abnormalities in narcolepsy with cataplexy. Sleep 2012; 35: 345–51. Stettner GM, Lei Y, Benincasa Herr K, Kubin L. Evidence that adrenergic ventrolateral medullary cells are activated whereas precerebellar lateral reticular nucleus neurons are suppressed during REM sleep. PLoS One 2013; 8: e62410. Stiasny-Kolster K, Doerr Y, Moller JC, Hoffken H, Behr TM, Oertel WH, et al. Combination of ‘idiopathic’ REM sleep behaviour disorder and olfactory dysfunction as possible indicator for alphasynucleinopathy demonstrated by dopamine transporter FP-CITSPECT. Brain 2005; 128: 126–37. Stiasny-Kolster K, Clever SC, Moller JC, Oertel WH, Mayer G. Olfactory dysfunction in patients with narcolepsy with and without REM sleep behavior disorder. Brain 2007; 130 (Pt 2): 442–9. Taniwaki T, Yoshiura T, Ogata K, Togao O, Yamashita K, Kida H, et al. Disrupted connectivity of motor loops in Parkinson’s disease during self-initiated but not externally-triggered movements. Brain Res 2013; 28: 45–59. Unger M, Moller JC, Ohletz T, Stiasny-Kolster K, Oertel WH, Mayer G. Transcranial midbrain sonography in narcoleptic subjects with and without concomitant idiopathic REM sleep behavior disorder. J Neurol 2009; 256: 135–7. Unger MM, Belke M, Menzler K, Heverhagen J, Keil B, StiasnyKolster K, et al. Diffusion tensor imaging in idiopathic REM sleep behavior disorder reveals microstructural changes in the brainstem, substantia nigra, olfactory region, and other brain regions. Sleep 2010; 33: 767–73. Verret L, Fort P, Gervasoni D, Leger L, Luppi PH. Localization of the neurons active during paradoxical (REM) sleep and projecting to the locus coeruleus noradrenergic neurons in the rat. J Comp Neurol 2006; 495: 573–86. Vetrivelan R, Fuller PM, Tong Q, Lu J. Medullary circuitry regulating rapid eye movement sleep and motor atonia. J Neurosci 2009; 29: 9361–9.