* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Lipoproteins
Survey
Document related concepts
Amino acid synthesis wikipedia , lookup
Biochemical cascade wikipedia , lookup
Polyclonal B cell response wikipedia , lookup
Ligand binding assay wikipedia , lookup
Human digestive system wikipedia , lookup
Biosynthesis wikipedia , lookup
G protein–coupled receptor wikipedia , lookup
Endocannabinoid system wikipedia , lookup
Biochemistry wikipedia , lookup
Lipid signaling wikipedia , lookup
Paracrine signalling wikipedia , lookup
Clinical neurochemistry wikipedia , lookup
Fatty acid synthesis wikipedia , lookup
Glyceroneogenesis wikipedia , lookup
Signal transduction wikipedia , lookup
Transcript
LIPOPROTEINS
A to Z
Lipid Digestion & Transport
Digestion & transport of lipids poses unique problems
relating to the insolubility of lipids in water.
Lipids, & products of their digestion, must be
transported through aqueous compartments within
the cell as well as in the blood & tissue spaces.
Free fatty acids are transported in the blood bound to
albumin
Within intestinal cells (and other body cells) some of the
absorbed cholesterol is esterified to fatty acids, forming
cholesteryl esters.
The enzyme that catalyzes cholesterol esterification is
ACAT (Acyl CoA: Cholesterol Acyl Transferase).
Intestinal epithelial cells synthesize triacylglycerols,
cholesteryl esters, phospholipids, free cholesterol, and
apoproteins, and package them into chylomicrons.
Chylomicron assembly
Fatty acids, 2-MAG
lumen
Fatty acids, 2-MAG
ATP
ADP
intestinal
epithelium
Triacylglycerol
Cholesterol
Apolipoproteins
Chylomicrons
Chylomicrons
lymphatics
Formation of Chylomicrons :
Chylomicrons are secreted by intestinal epithelial cells,
and transported via the lymphatic system to the blood.
Apoprotein CII on the chylomicron surface activates
Lipoprotein Lipase, an enzyme attached to the luminal
surface of small blood vessels. Lipoprotein Lipase
catalyzes hydrolytic cleavage of fatty acids from
triacylglycerols of chylomicrons.
Released fatty acids & monoacylglycerols are picked up
by body cells for use as energy sources.
Lipoprotein Lipase, is attached to the luminal surface
of small blood vessels. It catalyzes hydrolytic cleavage
of fatty acids from triacylglycerols of chylomicrons.
Released fatty acids & monoacylglycerols are picked up
by body cells for use as energy sources.
With removal of triacylglycerols and some proteins,
the % weight that is cholesteryl esters increases.
Chylomicron Metabolism
As triacylglycerols are removed by hydrolysis, chylomicrons
shrink in size, becoming chylomicron remnants with lipid
cores having a relatively high concentration of cholesteryl
esters.
Chylomicron remnants are taken up by liver cells, via
receptor-mediated endocytosis .
The process involves recognition of apoprotein E of the
chylomicron remnant by receptors on the liver cell surface.
Chylomicrons
Biosynthesis of membrane lipids and
steroids 1
10
Deliver dietary TG and PL to cells
dietary CHOL to liver . . .
apoCII is ligand to activate lipoprotein lipase
for removal of fatty acids in tissues . . .
apoE & apoB-48 are ligands for liver uptake of remnants . . .
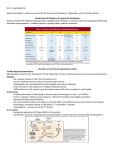
Lipoprotein content
of the chylomicron
changes as it
circulates
throughout the
body
- acquiring the
apo E & C2
from HDL
Questions
What are the lipids carried by CM?
Where is CM formed?
What is the source for lipids in CM?
How does the CM release FFA?
What is the fate of the FFA and Glycerol?
Where is the LPL found?
What are the components of Remnant CM?
. Liver cells produce, and secrete into the blood, very low
density lipoprotein (VLDL).
• The VLDL core has a relatively high triacylglycerol
content.
• VLDL has several apoproteins, including apoB-100.
As VLDL particles are transported in the bloodstream,
Lipoprotein Lipase catalyzes triacylglycerol removal by
hydrolysis.
With removal of triacylglycerols and some proteins, the
% weight that is cholesteryl esters increases.
VLDL are converted to IDL, and eventually to LDL.
VLDL IDL LDL
VLDL Assembly
Plasma
Dietary Carbohydrate
glucose
B48
LDL receptor
TG/CE
LIVER
pyruvate
Acetyl CoA
Acetyl CoA
mitochondria
E
TG
Cholesterol
(endogenous)
CMr
cholesterol
(exogenous)
FFA
FFA
B100
TG
CE/TG
VLDL
VLDL
Control of VLDL production:
VLDL assembly is dependent on availability of lipids.
Transcription of genes for enzymes that catalyze lipid
synthesis is controlled by SREBP.
Availability of apoprotein B-100 for VLDL assembly
depends at least in part on regulated transfer of B-100
out of the ER for degradation via the proteasome.
Nascent VLDL (B-100) + HDL (apo C & E) = VLDL
LPL hydrolyzes TG forming IDL
IDL loses apo C-II (reduces affinity for LPL)
75% of IDL removed by liver through Apo E and Apo B mediated
receptors
25% of IDL converted to LDL by hepatic lipase
VLDL
Biosynthesis of membrane lipids and
steroids 1
17
VLDL Metabolism
• Nascent VLDL (B-100) + HDL (apo C & E) = VLDL
• LPL hydrolyzes TG forming IDL
– IDL loses apo C-II (reduces affinity for LPL)
• 75% of IDL removed by liver
– Apo E and Apo B mediated receptors
• 25% of IDL converted to LDL by hepatic lipase
– Loses apo E to HDL
• Very Low Density Lipoprotein (VLDL)
– Synthesized in liver
– Transport endogenous triglycerides
– 90% lipid, 10% protein
– Apo B-100
• Receptor binding
– Apo C-II
• LPL activator
– Apo E
• Remnant receptor binding
Delivers endogenous TG and PL to cells . . .
apoE is ligand for liver uptake &
apoB-100 is ligand for tissue uptake
. . . apoCII is ligand to activate
Lipoprotein lipase for removal of
fatty acids
Delivers CHOL to cells . . .
VLDL
Triglycerides
3 Fatty Acids
Adipose Skeletal
(storage) Muscle
(energy)
Glycerol
Heart
(energy)
Blood
Liver
Once VLDL looses much of its TG’s it becomes LDL
QUESTIONS
Where is VLDL formed?
What are the lipids Carried by VLDL?
Which lipid is delivered by VLDL?
What is the mechanism of FFA release from
VLDL?
What is the fate of Remnant VLDL?
What are the lipids present in excess when VLDL
becomes VLDLR?
• Low Density
Lipoprotein (LDL)
– Synthesized from IDL
– Cholesterol transport
– Apo B-100
• Receptor binding
• 30% degraded in
extra hepatic
tissues while 70%
in liver
The lipid core of LDL is predominantly cholesteryl
esters.
Whereas VLDL contains 5 apoprotein types (B100, C-I, C-II, C-III, & E), only one protein,
apoprotein B-100, is associated with the surface
monolayer of LDL.
LDL Metabolism
• LDL receptor-mediated
endocytosis
– LDL receptors on ‘coated pits’
• Clathrin: a protein polymer
that stabilizes pit
– Endocytosis
• Loss of clathrin coating
• uncoupling of receptor,
returns to surface
– Fusing of endosome with
lysosome
• Frees cholesterol & amino
acids
Cells take up LDL by receptormediated endocytosis, involving
formation of a clathrin-coated pit
& pinching off of a vesicle
incorporating the receptor & LDL
cargo. After the clathrin coat
disassembles, the vesicle fuses
with an endosome
.
LDL is released from the receptor within the acidic
environment of the endosome, and the receptor is
returned to the plasma membrane.
After LDL is transferred to a lysosome, cholesterol is
released & may be used, e.g., for membranes synthesis.
LDL Receptor (apoB-E receptor)
Regulates cholesterol synthesis and plasma cholesterol levels
HMG-CoA
reductase
LDL-Receptors
LDL
Receptors
Cholesteryl ester
(storage)
ACAT
Cholesterol
LDL
LDL
Endosome
Lysosome
Amino
acids
LDL
28
Control of LDL Receptor activity:
Synthesis of LDL Receptor is suppressed by high
intracellular cholesterol.
This process involves decreased release of SREBP.
Members of the SREBP family of transcription factors
activate transcription of genes for the LDL receptor, as
well as for enzymes essential to cholesterol synthesis
such as HMG-CoA Reductase.
The decreased synthesis of LDL receptor prevents
excessive cholesterol uptake by cells.
It has the deleterious consequence that excess dietary
cholesterol remains in the blood as LDL.
Mutations affecting the LDL receptor are associated
with the most common form of the disease familial
hypercholesterolemia (high blood cholesterol).
Cells lacking functional LDL receptors cannot take up
LDL.
As a result, the amount of circulating LDL increases,
leading to enhanced risk of developing atherosclerosis.
Other hereditary hypercholesterolemias relate to
genetic defects in structure of apolipoproteins.
E.g., familial defective apoprotein B100 leads to
impaired binding of LDL to cell surface receptors, with
elevated levels of circulating LDL.
Summary of Control of Cholesterol Uptake
and Synthesis
• Increased uptake of LDL-cholesterol results
in:
• inhibition of HMG-CoA reductase
– reduced cholesterol synthesis
• stimulation of acyl CoA:cholesterol acyl transferase
(ACAT)
– increased cholesterol storage
– TG + C -> DG + CE
• decreased synthesis of LDL-receptors
– “down-regulation”
– decreased LDL uptake
• High Density Lipoprotein (HDL)
– Synthesized in liver and intestine
– Reservoir of apoproteins
– Reverse cholesterol transport
– Apo A
• Activates lecithin-cholesterol
acyltransferase (LCAT)
– Apo C
• Activates LPL
– Apo E
• Remnant receptor binding
HDL (high density lipoprotein) is secreted as a small
protein-rich particle by liver (and intestine).
One HDL apoprotein, A-1, activates LCAT (LecithinCholesterol Acyl Transferase), which catalyzes synthesis
of cholesteryl esters using fatty acids cleaved from the
membrane lipid lecithin.
The cholesterol is scavenged from cell surfaces & from
other lipoproteins.
HDL may transfer cholesteryl esters to other lipoproteins.
Some remain associated with HDL, which may be taken up
by liver & degraded.
HDL thus transports cholesterol from tissues & other
lipoproteins to the liver, which can excrete excess
cholesterol as bile acids.
High blood levels of HDL ("good" cholesterol) correlate
with low incidence of atherosclerosis.
Bacterial & viral infections, & some inflammatory disease
states decrease HDL & increase VLDL production by the
liver.
These & other changes associated with inflammation can
lead to increased risk of atherosclerosis if prolonged.
HDL (high density lipoprotein) is secreted as a small
protein-rich particle by liver (and intestine).
One HDL apoprotein, A-1, activates LCAT (LecithinCholesterol Acyl Transferase), which catalyzes synthesis
of cholesteryl esters using fatty acids cleaved from the
membrane lipid lecithin.
The cholesterol is scavenged from cell surfaces & from
other lipoproteins.
HDL Metabolism: Functions
• Apoprotein exchange
– provides apo C and apo E to/from VLDL
and chylomicrons
• Reverse cholesterol transport
HDL
Biosynthesis of membrane lipids and
steroids 1
37
Reverse cholesterol transport
• Uptake of cholesterol
from peripheral tissues
(binding by apo-A-I)
• Esterification of HDL-C
by LCAT
– LCAT activated by
apoA1
• Transfer of CE to
lipoprotein remnants
(IDL and CR) by CETP
• removal of CE-rich
remnants by liver,
converted to bile acids
and excreted
Reverse Cholesterol Transport
Delivery of peripheral tissue cholesterol to the liver for catabolism
Requires HDL, apoA-I and LCAT
Peripheral
Cell
UC
diffusion
HDL
UC
HDL
Macrophage/ Foam cell
ABCA1
UC
LCAT
PL
LCAT
Nascent
HDL
HDL
CE
CE
CE
apoA-I
SR-B1
TG
UC = unesterified cholesterol
CE = esterified cholesterol
PL = phospholipid
LDLr = LDL receptor
ABC = ATP Binding Cassette transporter
VLDL
or LDL apoB
CE
Liver
LDLr
Chol
Bile acids
Bile to gut