* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Chapter 14 PowerPoint - Hillsborough Community College
Survey
Document related concepts
Nervous system network models wikipedia , lookup
Neuroregeneration wikipedia , lookup
Haemodynamic response wikipedia , lookup
Neuromuscular junction wikipedia , lookup
Neuropsychopharmacology wikipedia , lookup
Basal ganglia wikipedia , lookup
Clinical neurochemistry wikipedia , lookup
Molecular neuroscience wikipedia , lookup
Stimulus (physiology) wikipedia , lookup
Synaptogenesis wikipedia , lookup
Neuroanatomy wikipedia , lookup
Transcript
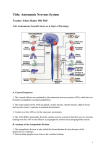
Chapter 14 Autonomic Nervous System © Annie Leibovitz/Contact Press Images © 2016 Pearson Education, Inc. PowerPoint® Lecture Slides prepared by Karen Dunbar Kareiva Ivy Tech Community College Why This Matters • Understanding the autonomic nervous system helps you to anticipate the effects and side effects of drugs on your patients © 2016 Pearson Education, Inc. Autonomic Nervous System • Automatic nervous system (ANS) consists of motor neurons that: – Innervate smooth muscles, cardiac muscle, and glands – Make adjustments to ensure optimal support for body activities • Shunts blood to areas that need it and adjusts heart rate, blood pressure, digestive processes, etc. – Operate via subconscious control • Also called involuntary nervous system or general visceral motor system © 2016 Pearson Education, Inc. Figure 14.1 Place of the ANS in the structural organization of the nervous system. Central nervous system (CNS) Peripheral nervous system (PNS) Sensory (afferent) division © 2016 Pearson Education, Inc. Motor (efferent) division Somatic nervous system Autonomic nervous system (ANS) Sympathetic division Parasympathetic division 14.1 ANS versus Somatic Nervous System • Both have motor fibers but differ in: – Effectors – Efferent pathways and ganglia – Target organ responses to neurotransmitters © 2016 Pearson Education, Inc. Effectors • Somatic nervous system innervates skeletal muscles • ANS innervates cardiac muscle, smooth muscle, and glands © 2016 Pearson Education, Inc. Efferent Pathways and Ganglia • SNS: cell body is in CNS, and a single, thick myelinated group A axon extends in spinal or cranial nerves directly to skeletal muscle • ANS: pathway uses a two-neuron chain 1. Preganglionic neuron: cell body in CNS with thin, lightly myelinated preganglionic axon extending to ganglion 2. Postganglionic (ganglionic) neuron (outside CNS): cell body synapses with preganglionic axon in autonomic ganglion with nonmyelinated postganglionic axon that extends to effector organ © 2016 Pearson Education, Inc. Neurotransmitter Effects • Somatic nervous system – All somatic motor neurons release acetylcholine (ACh) – Effect is always stimulatory • ANS – Preganglionic fibers release ACh – Postganglionic fibers release norepinephrine or ACh at effectors – Effect is either stimulatory or inhibitory, depending on type of receptors © 2016 Pearson Education, Inc. Overlap of Somatic and Autonomic Function • Higher brain centers regulate and coordinate both systems • Most spinal and many cranial nerves contain both somatic and autonomic fibers • Adaptations usually involve both skeletal muscles and visceral organs – Example: Active muscles require more oxygen and glucose, so ANS nerves speed up heart rate and open airways © 2016 Pearson Education, Inc. Figure 14.2 Comparison of motor neurons in the somatic and autonomic nervous systems. SOMATIC NERVOUS SYSTEM Cell bodies in central nervous system Neurotransmitter at effector Peripheral nervous system Effector organs Effect Single neuron from CNS to effector organs ACh Stimulatory Heavily myelinated axon Skeletal muscle Two-neuron chain from CNS to effector organs NE SYMPATHETIC Lightly myelinated preganglionic axons Nonmyelinated postganglionic axon Ganglion ACh Epinephrine and norepinephrine Adrenal medulla PARASYMPATHETIC AUTONOMIC NERVOUS SYSTEM ACh Acetylcholine (ACh) © 2016 Pearson Education, Inc. Blood vessel ACh ACh Lightly myelinated preganglionic axon Norepinephrine (NE) Ganglion Nonmyelinated postganglionic axon Smooth muscle (e.g., in gut), glands, cardiac muscle Stimulatory or inhibitory, depending on neurotransmitter and receptors on effector organs 14.2 Divisions of Autonomic Nervous System • Two arms of ANS: – Parasympathetic division: promotes maintenance functions, conserves energy – Sympathetic division: mobilizes body during activity • Dual innervation: all visceral organs are served by both divisions, but these divisions cause opposite effects – Dynamic antagonism between two divisions maintains homeostasis © 2016 Pearson Education, Inc. Role of the Parasympathetic Division • Keeps body energy use as low as possible, even while carrying out maintenance activities – Directs digestion, diuresis, defecation • Referred to as “rest-and-digest” system • Example: person relaxing and reading after a meal – Blood pressure, heart rate, and respiratory rates are low – Gastrointestinal tract activity is high – Pupils constricted, lenses accommodated for close vision © 2016 Pearson Education, Inc. Role of the Sympathetic Division • Mobilizes body during activity • Referred to as “fight-or-flight” system • Exercise, excitement, emergency, embarrassment activates sympathetic system – Increased heart rate; dry mouth; cold, sweaty skin; dilated pupils • During vigorous physical activity: – Shunts blood to skeletal muscles and heart – Dilates bronchioles – Causes liver to release glucose © 2016 Pearson Education, Inc. Key Anatomical Differences • Three main differences between sympathetic and parasympathetic divisions: 1. Sites or origin • Parasympathetic fibers are craniosacral; originate in brain and sacral spinal cord • Sympathetic fibers are thoracolumbar; originate in thoracic and lumbar regions of spinal cord © 2016 Pearson Education, Inc. Key Anatomical Differences (cont.) 2. Relative lengths of fibers • Parasympathetic has long preganglionic and short postganglionic fibers • Sympathetic has short preganglionic and long postganglionic 3. Location of ganglia • Parasympathetic ganglia are located in or near the their visceral effector organ • Sympathetic ganglia lie close to spinal cord © 2016 Pearson Education, Inc. Figure 14.3 Key anatomical differences between ANS divisions. Sympathetic Parasympathetic Eye Salivary glands Eye Brain stem Skin* Cranial Sympathetic ganglia Heart Lungs Stomach 1 Fibers originate in the brain stem (cranial fibers) or sacral spinal cord. 1 Fibers originate in the thoracic and lumbar spinal cord. 2a Preganglionic 2a Preganglionic Liver and gallbladder Bladder Genitals © 2016 Pearson Education, Inc. Lungs Heart fibers are long. fibers are short. Stomach 2b Postganglionic 2b Postganglionic fibers are long. Pancreas fibers are short. Pancreas T1 Salivary glands 3 Ganglia are within or near visceral effector organs. Sacral 3 Ganglia are close to spinal cord. L1 Liver and gallbladder Adrenal gland Bladder Genitals Table 14.1 Anatomical and Physiological Differences between the Parasympathetic and Sympathetic Divisions © 2016 Pearson Education, Inc. 14.3 Parasympathetic Division • Also called craniosacral division because fibers originate from brain stem and sacral regions or cord • Long preganglionic fibers extend from CNS almost to target organs – Synapse with postganglionic neurons in terminal ganglia that are close to or within target organs – Short postganglionic fibers synapse with effectors © 2016 Pearson Education, Inc. Figure 14.3-1 Key anatomical differences between ANS divisions. Parasympathetic Eye Salivary glands Heart Lungs Brain stem Cranial 1 Fibers originate in the brain stem (cranial fibers) or sacral spinal cord. 2a Preganglionic fibers are long. Stomach Pancreas Liver and gallbladder Bladder Genitals © 2016 Pearson Education, Inc. 2b Postganglionic fibers are short. 3 Ganglia are within or near visceral effector organs. Sacral Cranial Part of Parasympathetic Division • Cell bodies are located in brain stem • Preganglionic fibers run in: – Oculomotor nerves (III): control smooth muscle of eye, cause pupils to constrict and lenses to bulge for focusing • Postganglion cell bodies located in ciliary ganglia within eye orbitals © 2016 Pearson Education, Inc. Cranial Part of Parasympathetic Division (cont.) – Facial nerves (VII): stimulate large glands in head • Fibers that activate nasal and lacrimal glands have synapse in pterygopalatine ganglia • Fibers that activate submandibular and sublingual salivary glands synapse in submandibular ganglia – Glossopharyngeal nerves (IX): stimulate parotid salivary glands • Fibers synapse in otic ganglia © 2016 Pearson Education, Inc. Cranial Part of Parasympathetic Division (cont.) – Vagus nerves (X): account for ~ 90% of all preganglionic parasympathetic fibers in body • Serve all thoracic and abdominal viscera • Preganglionic fibers arise from medulla and synapse in terminal ganglia (intramural ganglia) in walls of target organs • Cardiac plexus: slow heart rate • Pulmonary plexus: serve lungs and bronchi • Esophageal plexus: form anterior and posterior vagal trunks that sends branches to stomach, liver, gallbladder, pancreas, small intestine, and part of large intestine © 2016 Pearson Education, Inc. Sacral Part of Parasympathetic Division • Originates from neurons in S2–S4 and serves pelvic organs and distal half of large intestine • Axons travel in ventral root of spinal nerves – Branch off to form pelvic splanchnic nerves • Synapse with: – Ganglia in pelvic floor (inferior hypogastric [pelvic] plexus) – Intramural ganglia in walls of distal half of large intestine, urinary bladder, ureters, and reproductive organs © 2016 Pearson Education, Inc. Figure 14.4 Parasympathetic division of the ANS. Eye Ciliary ganglion Lacrimal gland Pterygopalatine ganglion Submandibular ganglion Nasal mucosa Submandibular and sublingual glands Otic ganglion Parotid gland Heart Cardiac and pulmonary plexuses Lung Celiac plexus Liver and gallbladder Stomach Pancreas S2 Large intestine S4 Small intestine Pelvic splanchnic nerves Inferior hypogastric plexus Rectum Urinary bladder and ureters Genitalia (penis, clitoris, and vagina) © 2016 Pearson Education, Inc. Preganglionic Postganglionic Cranial nerve Sacral nerve 14.4 Sympathetic Division • Sympathetic is more complex and innervates more organs than parasympathetic – Some structures are innervated only by sympathetic: sweat glands, arrector pili muscle of hair follicle, smooth muscles of all blood vessels • Sympathetic also called thoracolumbar division – Preganglionic neurons are in spinal cord segments T1–L2 – Form lateral horns of spinal cord © 2016 Pearson Education, Inc. Figure 14.3-2 Key anatomical differences between ANS divisions. Sympathetic Eye Skin* Sympathetic ganglia 1 Fibers originate in the thoracic and lumbar spinal cord. T1 Salivary glands Lungs Heart 2a Preganglionic fibers are short. Stomach 2b Postganglionic Pancreas fibers are long. 3 Ganglia are close to spinal cord. L1 Liver and gallbladder Adrenal gland Bladder Genitals © 2016 Pearson Education, Inc. 14.4 Sympathetic Division • Preganglionic fibers pass through white rami communicantes and enter sympathetic trunk (chain or paravertebral) ganglia • Paravertebral ganglia vary in size, position, and number © 2016 Pearson Education, Inc. 14.4 Sympathetic Division • There are 23 paravertebral ganglia in the sympathetic trunk (chain) – – – – – 3 cervical 11 thoracic 4 lumbar 4 sacral 1 coccygeal © 2016 Pearson Education, Inc. Figure 14.5 Location of the sympathetic trunk. Spinal cord Dorsal root Ventral root Rib Sympathetic trunk ganglion Sympathetic trunk Ventral ramus of spinal nerve Gray ramus communicans White ramus communicans Thoracic splanchnic nerves © 2016 Pearson Education, Inc. 14.4 Sympathetic Division • Upon entering sympathetic trunk ganglion, short preganglionic fiber may follow one of three pathways: – Synapse in trunk ganglia: 1. Synapse with ganglionic neuron in same trunk ganglion 2. Ascend or descend sympathetic trunk to synapse in another trunk ganglion, or – Synapse in collateral ganglia 3. Pass through trunk ganglion and emerge without synapsing in trunk (only in abdomen and pelvis) – Synapse outside of trunk in collateral ganglia © 2016 Pearson Education, Inc. Table 14.2 Summary of Autonomic Ganglia © 2016 Pearson Education, Inc. Sympathetic Pathways with Synapses in Trunk Ganglia • Postganglionic axons enter ventral rami via gray rami communicantes – Gray rami communicantes: nonmyelinated postganglionic fibers – White rami communicantes: myelinated preganglionic fibers – White and gray rami communicantes contain sympathetic system neurons only • These fibers innervate sweat glands, arrector pili muscles, and vascular smooth muscle via pathways to the head and thorax © 2016 Pearson Education, Inc. Figure 14.6-1 Three pathways of sympathetic innervation. Lateral horn (visceral motor zone) Dorsal root Dorsal root ganglion Dorsal ramus of spinal nerve Ventral ramus of spinal nerve Ventral root Sympathetic trunk ganglion Sympathetic trunk Gray ramus communicans White ramus communicans 1 Synapse in trunk ganglion at the same level Skin (arrector pili muscles and sweat glands) © 2016 Pearson Education, Inc. Effectors Figure 14.6-2 Three pathways of sympathetic innervation. 2 Synapse in trunk ganglion at a higher or lower level Skin (arrector pili muscles and sweat glands) Effectors Blood vessels © 2016 Pearson Education, Inc. Sympathetic Pathways with Synapses in Trunk Ganglia (cont.) • Pathways to the head – Fibers emerge from T1 to T4 and synapse in the superior cervical ganglion – These fibers: • • • • • Innervate skin and blood vessels of the head Stimulate dilator muscles of the iris Inhibit nasal and salivary glands Innervate smooth muscle of upper eyelid Branch to the heart © 2016 Pearson Education, Inc. Sympathetic Pathways with Synapses in Trunk Ganglia (cont.) • Pathways to the thorax – Preganglionic fibers emerge from T1 to T6 and synapse in cervical trunk ganglia – Postganglionic fibers emerge from middle and inferior cervical ganglia and enter nerves C4 to C8 – These fibers innervate: • Heart via the cardiac plexus • Thyroid gland and the skin • Lungs and esophagus © 2016 Pearson Education, Inc. Figure 14.7 Sympathetic division of the ANS. Eye Lacrimal gland Nasal mucosa Pons Sympathetic trunk (chain) ganglia Blood vessels; skin (arrector pili muscles and sweat glands) Superior cervical ganglion Salivary glands Middle cervical ganglion Heart Inferior cervical ganglion T1 Cardiac and pulmonary plexuses Lung Greater splanchnic nerve Lesser splanchnic nerve Celiac ganglion Liver and gallbladder L2 Stomach White rami communicantes Sacral splanchnic nerves Superior mesenteric ganglion Spleen Inferior mesenteric ganglion Adrenal medulla Kidney Lumbar splanchnic nerves Small intestine Large intestine Rectum Preganglionic Postganglionic Genitalia (uterus, vagina, and penis) and urinary bladder © 2016 Pearson Education, Inc. Pathways with Synapses in Collateral Ganglia • Most fibers from T5 to L2 synapse in collateral ganglia outside of trunk, forming several splanchnic nerves – Greater, lesser, and least (thoracic splanchnic) splanchnic nerves – Lumbar splanchnic nerve – Sacral splanchnic nerves © 2016 Pearson Education, Inc. Figure 14.6-3 Three pathways of sympathetic innervation. Splanchnic nerve Collateral ganglion (such as the celiac) 3 Pass through sympathetic trunk to synapse in a collateral ganglion anterior to the vertebral column © 2016 Pearson Education, Inc. Abdominal organs (e.g., intestine) Effectors Pathways with Synapses in Collateral Ganglia (cont.) • Splanchnic nerves interweave, forming abdominal aortic plexuses that contain several important ganglia – Celiac and superior and inferior mesenteric ganglia – Postganglionic fibers from these ganglia then travel pathways to abdomen and pelvis © 2016 Pearson Education, Inc. Pathways with Synapses in Collateral Ganglia (cont.) • Pathways to the abdomen – Preganglionic fibers from T5 to L2 travel through thoracic splanchnic nerves – Synapses occur in celiac and superior mesenteric ganglia – Postganglionic fibers serve the stomach, intestines, liver, spleen, and kidneys © 2016 Pearson Education, Inc. Pathways with Synapses in Collateral Ganglia (cont.) • Pathways to the pelvis – Preganglionic fibers originate from T10 to L2 and travel trunk to lumbar and sacral ganglia – Some synapse with postganglionic fibers that run in lumbar and sacral splanchnic nerves – Others pass directly to plexuses to collateral ganglia (example: inferior mesenteric) – Postganglionic fibers serve distal half of large intestine, urinary bladder, and reproductive organs • Primarily inhibit activity of muscles and glands in abdominopelvic visceral organs © 2016 Pearson Education, Inc. Figure 14.7 Sympathetic division of the ANS. Eye Lacrimal gland Nasal mucosa Pons Sympathetic trunk (chain) ganglia Blood vessels; skin (arrector pili muscles and sweat glands) Superior cervical ganglion Salivary glands Middle cervical ganglion Heart Inferior cervical ganglion T1 Cardiac and pulmonary plexuses Lung Greater splanchnic nerve Lesser splanchnic nerve Celiac ganglion Liver and gallbladder L2 Stomach White rami communicantes Sacral splanchnic nerves Superior mesenteric ganglion Spleen Inferior mesenteric ganglion Adrenal medulla Kidney Lumbar splanchnic nerves Small intestine Large intestine Rectum Preganglionic Postganglionic Genitalia (uterus, vagina, and penis) and urinary bladder © 2016 Pearson Education, Inc. Pathways with Synapses in the Adrenal Medulla • Some preganglionic fibers pass directly to adrenal medulla without synapsing • Upon stimulation, medullary cells secrete norepinephrine and epinephrine into blood – Also called noradrenaline and norepinephrine • Sympathetic ganglia and adrenal medulla arise from same tissue – Adrenal medulla can be considered “misplaced” sympathetic ganglion © 2016 Pearson Education, Inc. 14.5 Visceral Reflexes • Visceral reflex arcs have same components as somatic reflex arcs: receptor, sensory neuron, integration center, motor neuron, and effector • Two key differences between visceral and somatic: – Visceral reflex arc has two consecutive neurons in the motor pathway – Afferents fibers are visceral sensory neurons • Send info about chemical changes, stretch, or irritation • Cell bodies are located in cranial nerve sensory ganglia or dorsal root ganglia of cord © 2016 Pearson Education, Inc. 14.5 Visceral Reflexes • Examples of visceral reflex: reflexes that empty rectum and bladder • Three neuron reflex arcs exist in walls of gastrointestinal tract – Involve enteric nervous system made up of sensory neurons, interneurons, and motor neurons • Visceral sensory fibers involved in phenomenon of referred pain © 2016 Pearson Education, Inc. Figure 14.8 Visceral reflexes. Stimulus 1 Receptor in viscera 2 Visceral sensory Dorsal root ganglion Spinal cord neuron 3 Integration center • May be preganglionic neuron (as shown) • May be a dorsal horn interneuron • May be within walls of gastrointestinal tract 4 Motor neuron (two-neuron chain) • Preganglionic neuron • Postganglionic neuron 5 Visceral effector Response © 2016 Pearson Education, Inc. Autonomic ganglion 14.6 Neurotransmitters • Major neurotransmitters of ANS are acetylcholine (ACh) and norepinephrine (NE) – Ach (same as ACh used by somatic motor neuron) is released by cholinergic fibers at: • All ANS preganglionic axons and • All parasympathetic postganglionic axons – NE is released by adrenergic fibers at: • Almost all sympathetic postganglionic axons, except those at sweat glands (release ACh) • Effects of neurotransmitter depends on whether it binds to cholinergic receptor or adrenergic receptor © 2016 Pearson Education, Inc. Figure 14.2 Comparison of motor neurons in the somatic and autonomic nervous systems. SOMATIC NERVOUS SYSTEM Cell bodies in central nervous system Neurotransmitter at effector Peripheral nervous system Effector organs Effect Single neuron from CNS to effector organs ACh Stimulatory Heavily myelinated axon Skeletal muscle Two-neuron chain from CNS to effector organs NE SYMPATHETIC Lightly myelinated preganglionic axons Nonmyelinated postganglionic axon Ganglion ACh Epinephrine and norepinephrine Adrenal medulla PARASYMPATHETIC AUTONOMIC NERVOUS SYSTEM ACh Acetylcholine (ACh) © 2016 Pearson Education, Inc. Blood vessel ACh ACh Lightly myelinated preganglionic axon Norepinephrine (NE) Ganglion Nonmyelinated postganglionic axon Smooth muscle (e.g., in gut), glands, cardiac muscle Stimulatory or inhibitory, depending on neurotransmitter and receptors on effector organs Cholinergic Receptors • Two types of cholinergic receptors bind ACh 1. Nicotinic receptors 2. Muscarinic receptors • Named after drugs that bind to them and mimic ACh effects: nicotine and muscarine (mushroom poison) © 2016 Pearson Education, Inc. Cholinergic Receptors (cont.) • Nicotinic receptors – Found on: • All postganglionic neurons (sympathetic and parasympathetic) • Hormone-producing cells of adrenal medulla • Sarcolemma of skeletal muscle cells at neuromuscular junction – Effect of ACh at nicotinic receptors is always stimulatory • Opens ion channels, depolarizing postsynaptic cell © 2016 Pearson Education, Inc. Cholinergic Receptors (cont.) • Muscarinic receptors – Found on: • All effector cells stimulated by postganglionic cholinergic fibers – Effect of ACh at muscarinic receptors • Can be either inhibitory or excitatory • Depends on receptor type of target organ – Example: Binding of ACh to cardiac muscle cells slows heart rate, whereas binding to intestinal smooth muscle cells increases motility © 2016 Pearson Education, Inc. Adrenergic Receptors • Two major classes that respond to NE or epinephrine – Alpha () receptors • Divided into subclasses: 1, 2 – Beta () receptors • Divided into subclasses: 1, 2, 3 © 2016 Pearson Education, Inc. Adrenergic Receptors (cont.) • Effects depend on which subclass of receptor predominates on target organ – Example: NE binding to cardiac muscle 1 receptors causes increase in rate, whereas epinephrine causes bronchial relaxation when bound to 2 receptors © 2016 Pearson Education, Inc. Table 14.3 Cholinergic and Adrenergic Receptors © 2016 Pearson Education, Inc. Table 14.4 Selected Drug Classes That Influence the Autonomic Nervous System © 2016 Pearson Education, Inc. 14.7 Parasympathetic and Sympathetic Interactions • Most visceral organs have dual innervation • Action potentials continually fire down axons of both divisions, producing a dynamic antagonistic interaction – Works to precisely control visceral activity • Both ANS divisions are partially active, resulting in a basal sympathetic and parasympathetic tone • One division usually predominates, but in a few cases, divisions have a cooperative effect © 2016 Pearson Education, Inc. Antagonistic Interactions • Dynamic antagonism allows for precise control of visceral activity – Sympathetic division increases heart and respiratory rates and inhibits digestion and elimination – Parasympathetic division decreases heart and respiratory rates and allows for digestion and discarding of wastes © 2016 Pearson Education, Inc. Sympathetic and Parasympathetic Tone • Almost all blood vessel smooth muscle is entirely innervated by sympathetic fibers only, so this division controls blood pressure, even at rest © 2016 Pearson Education, Inc. Sympathetic and Parasympathetic Tone (cont.) • Sympathetic tone (vasomotor tone): continual state of partial constriction of blood vessels – If blood pressure drops, sympathetic fibers fire faster than normal to increase constriction of blood vessels and cause blood pressure to rise – If blood pressure rises, sympathetic fibers fire less than normal, causing less constriction (dilation) of vessels, which leads to decrease in blood pressure – Allows sympathetic system to shunt blood where needed © 2016 Pearson Education, Inc. Sympathetic and Parasympathetic Tone (cont.) • Parasympathetic division normally dominates heart and smooth muscle of digestive and urinary tract organs, and it activates most glands except for adrenal and sweat glands – Slows the heart and dictates normal activity levels of digestive and urinary tracts – These organs also exhibit parasympathetic tone where they are always slightly activated © 2016 Pearson Education, Inc. Sympathetic and Parasympathetic Tone (cont.) • The sympathetic division can override these effects during times of stress • Drugs that block parasympathetic responses increase heart rate and cause fecal and urinary retention © 2016 Pearson Education, Inc. Cooperative Effects • Best example of cooperation between two divisions seen in control of external genitalia • Parasympathetic fibers cause vasodilation and are responsible for erection of penis or clitoris • Sympathetic fibers cause ejaculation of semen in males and reflex contraction of a female's vagina © 2016 Pearson Education, Inc. Unique Roles of the Sympathetic Division • Adrenal medulla, sweat glands, arrector pili muscles, kidneys, and almost all blood vessels receive only sympathetic fibers • Other unique functions of sympathetic division include: – Thermoregulatory responses to heat • When body temperatures rise, sympathetic nerves: 1. Dilate skin blood vessels, allowing heat to escape 2. Activate sweat glands • When body temperatures drop, blood vessels constrict © 2016 Pearson Education, Inc. Unique Roles of the Sympathetic Division (cont.) – Release of renin from kidneys • Sympathetic system causes release of renin from kidneys that in turn activates a system that increases blood pressure – Metabolic effects • Increases metabolic rates of cells • Raises blood glucose levels • Mobilizes fats for use as fuels © 2016 Pearson Education, Inc. Localized Versus Diffuse Effects • Parasympathetic division tends to elicit shortlived and highly localized control over effectors – ACh is quickly destroyed by acetylcholinesterase • Sympathetic division tends to be longer-lasting with bodywide effects – NE is inactivated more slowly than ACh – NE and epinephrine hormones from adrenal medulla have prolonged effects that last even after sympathetic signals stop © 2016 Pearson Education, Inc. Table 14.5 -1 Effects of the Parasympathetic and Sympathetic Divisions on Various Organs © 2016 Pearson Education, Inc. Table 14.5-2 Effects of the Parasympathetic and Sympathetic Divisions on Various Organs (continued) © 2016 Pearson Education, Inc. Clinical – Homeostatic Imbalance 14.1 • Autonomic neuropathy: damage to autonomic nerves that is a common complication of diabetes mellitus • Early signs include sexual dysfunction • Other frequent symptoms include dizziness after standing suddenly (poor blood pressure control), urinary incontinence, sluggish eye pupil reactions, and impaired sweating • Best way to prevent diabetic neuropathy is to maintain good blood glucose levels © 2016 Pearson Education, Inc. 14.8 Control of ANS Function • ANS is under control of CNS centers in: – Brain stem and spinal cord, hypothalamus, and cerebral cortex – Hypothalamus is generally main integrative center of ANS activity • Cerebral input may modify ANS but does so subconsciously – Works through limbic system structures on hypothalamic centers © 2016 Pearson Education, Inc. 14.8 Control of ANS Function – Brain stem and spinal cord controls • Brain stem reticular formation appears to exert most direct influence over ANS • Medullary centers regulate heart rate and blood vessel diameter, as well as gastrointestinal activities • Midbrain controls muscles of pupil and lens • Spinal cord controls defecation and micturition but are subject to conscious override © 2016 Pearson Education, Inc. 14.8 Control of ANS Function – Hypothalamic controls • Anterior regions direct parasympathetic functions; posterior region directs sympathetic • Control may be direct or indirect through reticular system or spinal cord • Centers of hypothalamus controls: – Heart activity, blood pressure, temperature of body, water balance, and endocrine activity – Emotional responses (rage, fear, pleasure) activated through limbic system signal hypothalamus to activate fight-or-flight system © 2016 Pearson Education, Inc. 14.8 Control of ANS Function – Cortical controls • Connections of hypothalamus to limbic lobe allow cortical influence on ANS • Voluntary cortical control of some visceral activities is possible – Biofeedback » Awareness of physiological conditions with goal of consciously influencing them » Biofeedback training allows some people to control migraines and manage stress © 2016 Pearson Education, Inc. Figure 14.9 Levels of ANS control. Communication at subconscious level Cerebral cortex (frontal lobe) Limbic system (emotional input) Hypothalamus The “boss”: Overall integration of ANS Brain stem (reticular formation, etc.) Regulates pupil size, heart, blood pressure, airflow, salivation, etc. Spinal cord Reflexes for urination, defecation, erection, and ejaculation © 2016 Pearson Education, Inc. 14.9 Disorders of the ANS • Many ANS disorders involve deficient control of smooth muscle activity – Hypertension (high blood pressure) • Overactive sympathetic vasoconstrictor response to stress • Heart must work harder, and artery walls are subject to increased wear and tear • Can be treated with adrenergic receptor-blocking drugs © 2016 Pearson Education, Inc. 14.9 Disorders of the ANS – Raynaud’s disease • Painful, exaggerated vasoconstriction in fingers and toes – Digits turn pale, then cyanotic – Treated with vasodilators – Autonomic dysreflexia • Life-threatening, uncontrolled activation of autonomic neurons in quadriplegics and people with spinal cord injuries above T6 • Blood pressure skyrockets, posing increased risk for stroke © 2016 Pearson Education, Inc. Developmental Aspects of the Autonomic Nervous System • ANS preganglionic neurons derive from neural tube (as do somatic motor neurons) • ANS structures in PNS derive from neural crest – Postganglionic neurons, adrenal medulla, and all ganglia • Nerve growth factor and signaling chemicals aid axons in finding path to target organs • During youth, ANS impairments are usually due to injury © 2016 Pearson Education, Inc. Developmental Aspects of the Autonomic Nervous System • ANS efficiency declines in old age, partially because of structural changes at preganglionic axon terminals • Effects of age on ANS – Constipation – Dry eyes and frequent eye infections – Orthostatic hypotension • Low blood pressure after position change • Pressure receptors are less responsive to blood pressure changes • Cardiovascular centers fail to maintain healthy blood pressure © 2016 Pearson Education, Inc.