* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download FUNCTIONAL NEUROANATOMY OF SPINAL CORD LEARNING
Nervous system network models wikipedia , lookup
Neuropsychopharmacology wikipedia , lookup
Neuroanatomy wikipedia , lookup
Stimulus (physiology) wikipedia , lookup
Synaptic gating wikipedia , lookup
Microneurography wikipedia , lookup
Axon guidance wikipedia , lookup
Channelrhodopsin wikipedia , lookup
Eyeblink conditioning wikipedia , lookup
Feature detection (nervous system) wikipedia , lookup
Proprioception wikipedia , lookup
Synaptogenesis wikipedia , lookup
Development of the nervous system wikipedia , lookup
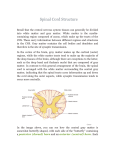
FUNCTIONAL NEUROANATOMY OF SPINAL CORD LEARNING OBJECTIVES At the end of this class the student should be able to Recall the knowledge of spinal cord Discuss the nuclei of spinal cord Discuss the ascending and descending tracts of spinal cord It is roughly cylindrical in shape Begins superiorly at foramen magnum Ends at lower border of first lumber vertebrae Occupy upper two thirds of vertebral canal It is surrounded by three meninges The dura matter. The arachnoid matter. The pia matter CSF is present in subarachnoid space around the spinal cord. Cervical and lumber enlargements? Tapers of at conus medullaris Filum terminale: From conus medullaris a prolongation of pia matter which descends down to be attached at the surface of coccyx Cauda equina? Anteriorly is anterior median fissure Posteriorly is posterior median sulcus There are thirty one pairs of spinal nerve Anterior motor and posterior sensory root? Each root is attached by rootlets which extend the whole length of corresponding segments of cord. Posterior root possesses posterior root ganglia. Structure of spinal cord: Inner core of gray matter and outer cover of white matter. There is no evidence that cord is segmented Gray matter: Is seen as ‘H’ shaped pillar with anterior and posterior gray column or horns united by a thin gray commissure containing small cord Lateral gray column is present in thoracic and lumber segments of cord Amount of gray matter is related to the muscle innervated by that segment i.e. cervical and lumbosacral segments Gray matter: Consists of nerve cells, their processes, neuroglia, blood vessels. Nerve cells are multipolar and neuroglial cells forms intricate network around. Nerve cells in anterior gray column: Large multipolar cells; their axons form alpha efferent to skeletal muscle Smaller multipolar cell; their axons form gamma efferents to innervate intrafusal fiber of neuromuscular spindles Smaller multipolar cell; their axons form gamma efferents to innervate intrafusal fiber of neuromuscular spindles . Nerve cells of anterior gray column may be divided into three basic groups or columns, medial, central and lateral (A), Medial group of cells: Innervate muscles of the neck, trunk, intercostal muscles and abdominal muscles. Present in most segments of the cord (B),Central group of cells: Smaller and is present in cervical and lumbosacral segment. 1. Cervical part: Segments C3,C4 and C5 innervates diaphragm and are collectively known as Phrenic nucleus. In upper five or six segments some of nerve cell innervate sternocleidomastoid and trapezius muscle and are known as accessory nucleus 2. Lumbosacral part: Present in second lumber segment and wards to the first sacral segment of the cord. Axon have unknown distribution (C) , lateral group: Present in cervical and lumbosacral segments of the cord and are responsible for innervating skeletal muscles. Nerve cell group in the posterior gray columns. Four nerve cell groups Two extend through out the length of spinal cord Other two are restricted to the thoracic and lumber segments. 1. SUBSTANTIA GELATINOSA. Present at apex through out the length of spinal cord. Largely Golgi type 2 neurons. Concerned with pain, temperature, and touch from posterior root. It receives input from descending fibers from supraspinal segments. Information is also modified. 2. NUCLEUS PROPRIUS Large group of nerve cells anterior to substantia gelatinosa through out the spinal cord. Forms main bulk of cells present in the posterior gray column. Receives information from the posterior white column that are associated with sense of position and movement (perception), two point discrimination and vibration. 3. NUCLEUS DORSALIS (CLARK’S COLUMN) At the base of posterior gray column. Extends from 8th cervical segment caudally to the 3rd or 4th lumber segment. Most of the cells are large and associated with proprioception. 4. VICERAL AFFERENT NUCLEUS: Group of nerve cells of medium size. Situated lateral to nucleus dorsalis. From 1st thoracic to the 3rd lumber segment of spinal cord. Receiving afferent information. NERVE CELL GROUP IN LATERAL GRAY COLUMNS The intermediate group of cells from the small lateral gray column which extends from 1st thoracic to 2nd or 3rd lumber segments of spinal cord Cells are relatively small and gives rise to preganglionic sympathetic fibers. Similar group of cells found in the 2nd,3rd and 4th sacral spinal segments of spinal cord, and gives rise to preganglionic parasympathetic fibers. Gray commissure and central cannal : Anterior and posterior gray column on each side are connected by transverse gray commissure. In the centre is present central. Anterior gray column. Posterior gray column. Central cannal Cannal continues up wards to 4th ventricle Inferiorly conus medullaris into terminal ventricle and terminate below with in the root of filum terminale. Lined by ciliated columnar epithelium the ependyma. Closed inferiorly. Anterior white column: Lies between the midline and the point of emergence of anterior nerve root. Lateral white column: lies between emergence anterior nerve root and entry of posterior nerve root. Posterior white column: lies between entry of posterior nerve root and the midline. White matter is mixture of nerve fibers, neuroglia and blood vessels. It surrounds the gray matter and its white colour is due to the high proportion of myelinated nerve fibers. Relationship of spinal cord segments to vertebral numbers ASCENDING TRACTS Modality: Touch, Pain, Temperature, Kinesthesia Receptor: Exteroceptor, Interoceptor, Proprioceptor Primary Neuron: Dorsal Root Ganglion (Spinal Ganglion) Secondary Neuron: Spinal Cord or Brain Stem Tertiary Neuron: Thalamus (Ventrobasal Nuclear Complex) Termination: Cerebral Cortex, Cerebellar Cortex, or Brain Stem POSTERIOR WHITE COLUMN-MEDIAL LEMNISCAL PATHWAY MODALITY: Discriminative touch (including vibration) and proprioception (position sensation, kinesthesia). RECEPTOR: Most receptors except free nerve endings. FIRST NEURON: Dorsal root ganglion (Spinal ganglion) Posterior root – Posterior white column. SECOND NEURON: Dorsal column nuclei (nucleus cuneatus and gracillus). Internal arcuate fibers-Sensory decussation medial lemniscus. THIRD NEURON: Thalamus (VPL) to Internal capsule to corona radiata. TERMINATION: Primary Somesthetic area (SI) Fasciculus Gracilis : Carries two point discrimination, kinesthesis (from muscle & joints) sensations. Fasciculus cuneatus: Carries vibratory sense Lesion causes: Ipsilateral loss of discriminative touch sensation and conscious proprioception below the level of lesion SPINOTHALAMIC TRACT MODALITY: Pain and Temperature sensations and Light touch. RECEPTER: Free nerve endings. FIRST NEURON: Dorsal root ganglion (Spinal ganglion). SECOND NEURON: Dorsal horn (Lamina 4,5,6) spinothalamic tract (Spinal lemniscus). THIRD NEURON: Thalamus (VPLC,CL,POM). Internal capsule – corona radiata. TERMINATION: Primary Somesthetic area (SI) and Diffuse wide spread cortical region. LATERAL SPINOTHALAMIC TRACT Carries pain and temperature sensations which are transmitted in fast conducting delta A type and slow C type fibres. Posterior root ganglion → Tip of posterior gray column → Posteriolateral tract of Lissauer → Synapse in posterior column. Second order neuron axon cross obliquely to opposite side in anterior commissure ascend as lateral spinothalamic tract → In medulla joined by anterior spinothalamic and spinotectal forming spinal lemniscus. Third order neuron in VPL nucleus of thalamus → Fiber pass through posterior limb of internal capsule and corona radiata to reach somesthetic area in postcentral gyrus of cerebral cortex. ANTERIOR SPINOTHALAMIC TRACT Carries light touch and pressure sensations. Like the lateral tract fibres enter the tip of posterior column contribute to posteriolateral tract of lissauer and synapses with cells of substantia gelatinosa → Second order neuron axon cross obliquely in anterior commissure → Joins spinal lemniscus remaining course is same as Lateral spinothalamic. LESION Contralateral loss of pain and temperature sensation below the level of lesion POSTERIOR SPINOCEREBELLAR TRACT Muscle and joint sense pathway. Extends from C8 to L3-4 → Fibres from posterior root ganglia synapse in dorsal nucleus of Clark. → Axons of second order neuron runs in lateral column. → Through the inferior cerebellar peduncle reaches the cerebellum. Golgi tendon, muscle spindle and joint receptor information from trunk and lower limb are received by these fibres. ANTERIOR SPINOCEREBELLAR TRACT Concerned with muscle and joint movement information from lower limb. Cells of origin extend from coccygeal to L1 segment. Fibres are mostly crossed. Pathway has two neurons. 1st order in dorsal root ganglion 2nd in spinal cord. Axons of 2nd order neurons runs over superior cerebellar peduncle to enter the cerebellum. Concerned with coordinated movement and posture of lower limb. CUNEACEREBLLAR TRACT Some uncrossed fibres of F.cuneatus synapse on accessory cuneatus nucleus. Equivalent to dorsal nucleus of Clark which is absent above C8 level. Pass through inferior cerebellar peduncle to the cerebellum. Takes golgi tendon and muscle spindle information (i.e. muscle joint sense from cervical and upper thoracic region) to cerebellum. SPINOTECTAL TRACT Axons enter spinal cord from the posterior root ganglion to unknown second order neuron (crosses median plane and ascends as spinotectal tract) to superior colliculus for spinovisual reflexes and brings about movements of eyes and head towards the source of stimulation SPINORETICULAR TRACT Passes up through unknown second order neurons as Spinoreticular tract and synapse uncrossed to reticular formation. It has important role in influencing the level of consciousness. SPINO-OLIVARY TRACT Unknown second order. Crosses median plane and ascends as Spino-olivary tract. Synapse in olive. From it third order neuron pass to cerebellum through inferior cerebellar peduncle. Conveys cutaneous and proprioceptive information to cerebellum. DESCENDING TRACTS PYRAMIDAL TRACT OR CORTICOSPINAL TRACT Formed by the axons of pyramidal cells in the motor area of cerebral cortex mostly → Course through posterior limb of internal capsule → Midbrain → Pons → Medulla here 80% of fibres cross known as pyramidal decussation → Lateral corticospinal tract → Synapse with internuncial neurons in the base of ventral gray column. 20% fibres uncrossed form anterior corticospinal tract. They cross at different spinal levels. EXTRA PYRAMIDAL TRACT RUBEROSPINAL TRACT Formed by the axons of red nucleus cross in the tegmentum and form ventral tegmental decussation. Enters the lateral white column of spinal cord, terminates by synapsing through internuncial neurons with the anterior horn cells. Facilitates the activity of flexure muscles and inhibits the activity of extensors or antigravity muscles. TECTOSPINAL TRACT Formrd by the axons of neurons in the superior colliculus. Fibre terminate on anterior horn cells through internuncial neurons. Concerned with reflex postural movements in response to visual stimuli. VESTIBULOSPINAL TRACT Fibres arise from lateral vestibular nucleus. Uncrossed fibres reach the spinal cord and run in the anterior white column and synapse with anterior horn cells. The inner ear and the cerebellum by means of this tract facilitate the activity of extensor muscles and inhibits the activity of flexure muscles in association with the maintenance of balance. OLIVOSPINAL TRACT Fibre originate from inferior olivary nucleus descends in spinal cord in anterolateral column of white matter and synapse with the anterior horn cells. Influences the activity of motor neurons in the anterior gray column. RETICULOSPINAL TRACT Arises from reticular formation in medulla and pons. Crossed and uncrossed. Autonomic fibres from higher levels descends and traverse portions of reticular formation that give rise to the reticulospinal tract. Provide a pathway by which hypothalamus can control sympathetic out flow and sacral parasympathetic flow. COMMON LESIONS RELATED TO SPINAL CORD Herpes Zoster Inflammatory reactions of spinal ganglion Severe pain on the dermatomes of affected ganglion Tabes Dorsalis Common variety of neurosyphilis. Posterior column and spinal posterior root lesion Loss of discriminative touch sensation and conscious proprioception below the level of lesion and posterior column ataxia Brown - Sequard syndrome (spinal cord hemisection) Major Symptoms are 1. Ipsilateral UMN syndrome below the level of lesion 2. Ipsilateral LMN syndrome at the level of lesion 3. Ipsilateral loss of discriminative touch sensation and conscious proprioception below the level of lesion (posterior white column lesion 4. Contralateral loss of pain and temperature sensation below the level of lesion (spinothalamic tract lesion) Syringomyelia Lesion Central canal of spinal cord. Gradually extended to peripheral part of the cord Symptom Initial symptom is bilateral loss of pain (compression of anterior white commissure) Variety of symptoms appear according to the lesion extended from central canal Thankyou