* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Autonomic Nervous System
Pharmacogenomics wikipedia , lookup
Pharmacognosy wikipedia , lookup
Discovery and development of antiandrogens wikipedia , lookup
Prescription costs wikipedia , lookup
Pharmacokinetics wikipedia , lookup
Pharmaceutical industry wikipedia , lookup
5-HT2C receptor agonist wikipedia , lookup
5-HT3 antagonist wikipedia , lookup
Drug interaction wikipedia , lookup
NMDA receptor wikipedia , lookup
Discovery and development of beta-blockers wikipedia , lookup
Toxicodynamics wikipedia , lookup
Theralizumab wikipedia , lookup
Norepinephrine wikipedia , lookup
Discovery and development of angiotensin receptor blockers wikipedia , lookup
Cannabinoid receptor antagonist wikipedia , lookup
Epinephrine autoinjector wikipedia , lookup
NK1 receptor antagonist wikipedia , lookup
Nicotinic agonist wikipedia , lookup
Psychopharmacology wikipedia , lookup
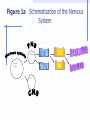
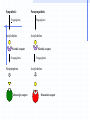
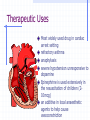
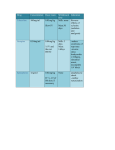
Autonomic Nervous System Part Dieu Atropine Anticholinergic, Parasympatholytic comes from ”belladonna” plant Figure 1a Schematization of the Nervous System PNSPN S Nervous System PNS How autonomic drugs work ANS transmits nerve impulses from the CNS to the effector organs over efferent neurons (preganglionic or postganglionic) Effector organs are the heart, smooth muscle and exocrine glands. Neurotransmittor at effector organ determines type of neuron norepinephrine or epinephrine=adrenergic (sympathetic) acethylcholine = cholinergic (parasympathetic) Receptors NOREPI ACH EPI If receptor responds to acethylcholine = muscarinic or nicotinic If receptor responds to norephinephrine or epinephrine = adrenergic muscarinic nicotinic adrenergic Sympathetic Preganglionic Acetylcholine Nicotinic receptor Postganglionic Norepinephrine Adrenergic receptor Parasympathetic Preganglionic Acetylcholine Nicotinic receptor Postganglionic Acetylcholine Muscarinic receptor Competitive Actions of Atropine Atropine competes and binds the muscarinic receptor sites thus preventing ACH from binding to that site. Acetylcholine Atropine Muscarinic Receptor Site Theraputic Uses of Atropine to increase the heart rate in symptomatic bradycardia reduce hyperactivity and spasms of the GI tract and bladder used in ophthalmology to cause mydriasis (pupil dilation) Atropine is used to treat organophosphate overdoses Atrovent (Impratropium) which is a mixture of atropine and Ventolin (blocks muscarinic effects) Anticholinergic Overdose Mnemonic red as a beet dry as a bone blind as a bat mad as a hatter hot as a hare Rationale Peripheral ganglionic blockade of nicotinic receptors Cholinergic nerves supply the sweat glands, anticholinergics can decrease or abate their activity. The sphincter muscle of the iris and the ciliary muscle are innervated by cholinergic nerve fibers. The sphincter muscle is not able to contract normally, the radial muscle causes the pupil to dilate. The patient is unable to focus (accommodate). Anticholinergics block cholinergic pathways and receptors in the CNS. This results in manic behavior and excitement. The inhibition of sweat glands causes the patients body temperature to rise. Special Prehospital Concerns Atropine should be given in doses of 0.5mg except in cases of bradyasystolic arrest Atropine should be used with extreme caution in the setting of myocardial infarct second-degree type II and 3 degree heart block with wide QRS complexes, transcutaneous pacing is a preferred method of therapy Epinephrine Adrenergic Agonist Sympathomimetic Drug Profile naturally occurring catecholamine that is produced in the body and released by the adrenal gland Epinephrine can be considered the emergency hormone and norepinephrine is mainly the transmitter hormone stimulates adrenergic neurons to bring about the various effects on the body Epinephrine Pharmacokinetics Both Alpha and Beta-receptors are stimulated by epinephrine. Epinephrine is a “direct acting” adrenergic agonist It is metabolized primarily by enzymes in the synaptic cleft Pharmacokinetics of Epi Cardiovascular Effects SVR B/P Electrical activity in the heart cerebral and coronary blood flow strength of myocardial contraction MVO2 automaticity Adrenergic Receptor Response to Epi Alpha Receptor Vasoconstriction Iris Dilatation Intestinal relaxation Intestinal sphincter contraction Pilomotor contration Bladder sphincter contraction Beta Receptor Vasodilatation (B2) Cardioacceleration (B1) Increased myocardial strength (B1) Intestinal relaxation (B2) Uterus relaxation (B2) Bronchodilatation (B2) Calorigenesis (B2) Glycogenolysis (B2) Lipolysis(B2) Bladder wall relaxation(B2) Therapeutic Uses Most widely used drug in cardiac arrest setting refractory asthma anaphylaxis severe hypotension unresponsive to dopamine Epinephrine is used extensively in the resuscitation of children (210mcg) an additive in local anaesthetic agents to help cause vasoconstriction Adverse Effects Overdose is unlikely as the drug is quickly metabolized Increased HR/BP,Sweating increase MVO2 demands and have to given with caution to those patients with ischemic heart disease Dosage/Supplied Adult- For anaphylactic reactions (1:1,000) 0.3mg subcutaneous. For Cardiac arrest 1:10,000 1mg IV q 3-5 mins. 2mgs ETT q 3-5 mins. Pediatric- For anaphylactic reactions (1:1,000) 0.01mg/kg max 0.3mg For severe hypotension (shock) 210mcg/min IV Special Prehospital Concerns Epinephrine can be administered in via IV, ETT, SC, bolus or infusion ideal dose of epinephrine epinephrine infusion,. and titrate to effect Epinephrine is light sensitive Salbutamol Adrenergic agonist (beta-2) Bronchodilator Drug Profile (FYI – Do not memorize!) beta agonists are thought to work is by increasing the intracellular concentrations of cAMP causes epithelial chloride channels to open As the chloride ions move they draw sodium ions along with them. The in sodium ions create a gradient to draw water along with them. This in water acts to lubricate the mucous How it works #1 Ventolin #2 Increase in cAMP #4 H2O follows sodium #3 Activates chloride channels. As channels open Chloride ions enter. Sodium is drawn in to maintain ionic balance. Therapeutic Uses Therapeutic Uses Ventolin is used to treat bronchospasm brought about from a number of factors. The fact that Ventolin is predominantly a beta 2 receptor stimulator, the effects on the beta 1 receptors of the heart are minimal. Adverse Effects •nervousness • tremors • agitation • dizziness • palpitations • headache • tachycardia •nausea. •allergic reactions include angioedema, urticaria, bronchospasm, hypotension, rash and anaphylaxis •Overdosage may cause tachycardia, cardiac arrhythmias, hypertension, hypokalemia and in extreme cases, sudden death Dosage -Adult and Pediatric Dose: Salbutamol via Nebulizer: <10kg – 1.25 mg 10 – 30 kg – 2.5 mg >30 kg – 5.0 mg Salbutamol via MDI 0-2 years: 1 puff followed by 4 breaths, repeat this 3 times 2-5 years: 1 puff followed by 4 breaths, repeat this 4 times 5-8 years: 1 puff followed by 4 breaths, repeat this 6 times > 8 years: 1 puff followed by 4 breaths, repeat this 8 times Special PreHospital Concerns administered by MDI (metered dose inhaler) or by nebulizer mask driven by oxygen or air. Aerochamber is better To test how full an MDI container is -see figure Drug Profile Barbituates act by suppressing impulses to the limbic system and the RAS Also act by augmenting GABA inhibitory effect throughout the entire brain Result can be a profound depression in consciousness Adverse Effects Low doses –euphoria, Respiratory depression Diminished reflexes and motor response Unconsiousness Death Hypotension Other CNS Depressants Alcohols – common use Methanol, ethanol, choral hydrate Paraldehyde – older use, ETOH withdrawal Antihistamines – Benadryl, Gravol (side effects) Side effects of many non-CNS drugs Prehospital Administration Versed Phenobarb Ativan Gravol Valium Narcotics For Next Class Please read Chapter 7 pages 82-95 Stimulants (antidepressants) Chapter 9 – 114-131 Common prescription Drugs Do YOU know your drugs?