* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Enzymes lII: Clinical Applications
Polyclonal B cell response wikipedia , lookup
Ultrasensitivity wikipedia , lookup
Photosynthetic reaction centre wikipedia , lookup
NADH:ubiquinone oxidoreductase (H+-translocating) wikipedia , lookup
Catalytic triad wikipedia , lookup
Monoclonal antibody wikipedia , lookup
Metalloprotein wikipedia , lookup
Lipid signaling wikipedia , lookup
Biochemistry wikipedia , lookup
Nicotinamide adenine dinucleotide wikipedia , lookup
Human digestive system wikipedia , lookup
Western blot wikipedia , lookup
Proteolysis wikipedia , lookup
Amino acid synthesis wikipedia , lookup
Deoxyribozyme wikipedia , lookup
Lactate dehydrogenase wikipedia , lookup
Oxidative phosphorylation wikipedia , lookup
Biosynthesis wikipedia , lookup
Restriction enzyme wikipedia , lookup
Enzyme inhibitor wikipedia , lookup
Evolution of metal ions in biological systems wikipedia , lookup
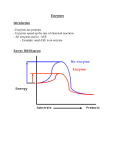
CHAPTER 8 Enzymes lII: Clinical Applications Enzymes are used clinically in three principal ways: 1. As indicators of enzyme activity or enzyme concentration in body fluids (e.g., serum and urine) in the diagnosis and prognosis of various diseases; 2. As analytical reagents in the measurement of activity of other enzymes or nonenzyme substances (e.g., substrates, proteins, and drugs) in body fluids; and 3. As therapeutic agents. 8.1 Diagnosis and Prognosis of Disease Enzyme assays employed in the diagnosis of diseases are one of the most frequently used clinical laboratory procedures. The most commonly used body fluid for this purpose is serum, the fluid that appears after the blood has clotted. The liquid portion of unclotted blood is calledplasma. Serum is used for many enzyme assays because the preparation of plasma requires addition of anticoagulants (e.g., chelating agents) that interfere with some assays. Enzymes in circulating plasma are either plasma-specific or nonplasma-specific. Plasma-specific enzymes are normally present in plasma, perform their primary function in blood, and have levels of activity that are usually higher in plasma than in tissue cells. Examples are those enzymes involved in blood clotting (e.g., thrombin), fibrinolysis (e.g., plasmin), and complement activation, as well as cholinesterase (also called pseudocholinesterase or choline esterase II to distinguish it from the acetylcholinesterase of nervous tissue; see Chapter 6) and ceruloplasmin. These enzymes are synthesized mainly in the liver and released into the circulation at a rate that maintains optimal steady-state concentrations. Hereditary enzyme defects or impaired liver function can cause suboptimal levels. For example, deficiency of thrombin or plasmin can cause defective blood coagulation or fibrinolysis, respectively. Cholinesterase deficiency can cause prolonged muscle paralysis when succinylcholine is administered as an adjunct to anesthesia to produce skeletal muscle relaxation. Succinylcholine, a structural analogue of acetylcholine, competes with acetylcholine receptors at the motor end-plate of the neuromuscular junction and brings about depolarization that leads to muscle relaxation. The effect of succinylcholine is terminated through the enzymatic action of plasma cholinesterase but is not significantly altered by acetylcholinesterase at the neuromuscular junction. Measurement of plasma cholinesterase before surgery may prevent this adverse effect. Non-plasma-specific enzymes are intracellular enzymes normally present in plasma at minimal levels or at concentrations well below those in tissue cells. Their presence in plasma is normally due to turnover of tissue cells, but they are released into the body fluids in excessive concentrations as a result of cellular damage or impairment of membrane function. Tissue injury and impairment of 121 1~ CHAPTER8 Enzymes II1: Clinical Applications membrane function can be caused by diminished oxygen supply (e.g., myocardial infarction), infection (e.g., hepatitis), and toxic chemicals. Proliferation of cells, with consequent increased turnover, can also raise levels in plasma of enzymes characteristic of those cells (e.g., elevation of serum acid phosphatase in prostatic carcinoma). Table 8-1 lists clinically useful enzymes and their tissue of origin. Intracellular enzymes are essentially confined to their cells of origin. A few are secretory enzymes that are secreted by some selected tissue (salivary gland, gastric mucosa, or pancreas) into the gastrointestinal tract, where they participate in digestion of food constituents (Chapter 12). Plasma levels of secretory enzymes increase when their cells of origin undergo damage or membrane impairment or when the usual pathways of enzyme secretion are obstructed. For example, large amounts of pancreatic amylase and triacylglycerol lipase (commonly known as lipase) enter the blood circulation in patients suffering from pancreatitis. These enzymes can digest the pancreas itself and surrounding adipose tissue in a process known as enzymatic necrosis (death of tissue cells). The diagnosis of organ disease is aided by measurement of a number of enzymes characteristic of that tissue or organ. Most tissues have characteristic enzyme patterns (Table 8-2) that may be reflected in the relative serum concentrations of the respective enzymes in disease. The diseased tissue can be further identified by determination of the isoenzyme pattern of one of these enzymes (e.g., lactate dehydrogenase, creatine kinase) in the serum, since many tissues have characteristic isoenzyme distribution patterns for a given enzyme. For example, creatine kinase (CK) is a dimer composed of two subunits, M (for muscle) and B (for brain), that occur in three isoenzyme forms, BB(CK1), MB(CK2) and MM(CK3), which catalyze the reversible phosphorylation of creatine with adenosine triphosphate (ATP) as the phosphate donor: CK Creatine + ATP ~- phosphocreatine + ADP (adenosine diphosphate) This reaction provides ATP for muscle contraction (Chapter 21). Skeletal muscle contains predominantly CK3, whereas heart muscle (myocardium) contains CK3 and CK2. Serum normally contains a small amount of CK3 derived predominantly from skeletal muscle. Detection of CK2 in serum (in an appropriate clinical setting) is strongly suggestive of myocardial damage. Since an abnormal isoenzyme level may occur with apparently normal total activity of the enzyme, determination of the isoenzyme concentration is essential in the diagnostic enzymology. T A B L E 8-1 Tissues of Origin of Some Diagnostically Important Serum Enzymes Enzyme Principal Tissue Source Acid phosphatase Alanine aminotransferase (glutamate pyruvate transaminase) Alcohol dehydrogenase Alkaline phosphatase Prostate Liver Amylase* Arginase Aspartate aminotransferase (glutamate oxaloacetate transaminase) Ceruloplasmin Cholinesterase Chymotrypsin(-ogen)* Creatine kinase Fructose-bisphosphate aldolase -Glutamyltransferase Glutamate dehydrogenase Isocitrate dehydrogenase Lactate dehydrogenase Leucine aminopeptidase Ornithine carbamoyltransferase Pepsin(-ogen)* Prostatic specific antigen (a serine proteinase) Sorbitol dehydrogenase Triacylglycerol lipase* (lipase) Trypsin(-ogen)* Liver Bone, intestinal mucosa, hepatobiliary system, placenta, kidney Pancreas, salivary glands Liver Heart and skeletal muscle, liver kidney, brain Liver Liver Pancreas Skeletal and heart muscle, brain Skeletal and heart muscle Kidney, hepatobiliary system, prostate, pancreas Liver Liver Skeletal and heart muscle, liver, kidney, erythrocytes, pancreas, lungs Hepatobiliary system, intestine, pancreas, kidney Liver Gastric mucosa Prostate Liver Pancreas Pancreas *Secretory enzymes. Factors Affecting Presence and Removal of Intracellular Enzymes from Plasma Many factors are taken into consideration in the clinical interpretation of serum enzyme levels. Membrane permeability changes and cell destruction affect the release of SECTION 8.1 123 Diagnosisand Prognosis of Disease TABLE 8-2 Properties of Cardiac Markers Used in the Evaluation of Acute Myocardial Infarction (AM1) Marker Molecular Weight (Daltons) Elevation after Peak AMI Elevation (Hours) (Hours) Return to Normal Levels (Hours or Days) Myoglobin Total CK CKMB 17,200 86,000 86,000 1-3 4-8 4-6 4-6 12-24 12-24 20-24 hrs 36-48 hrs 24-48 hrs Cardiac Troponin T 39,700 4-6 18-36 5-14 days Cardiac Troponin I LDH 24,000 4-6 12-24 5-9 days 8-12 48-72 10-15 days 135,000 intracellular enzymes. These changes can result from a decrease in intracellular ATP concentration due to any of the followingconditions: deficiency of one or more of the enzymes needed in ATP synthesis (e.g., pyruvate kinase in red blood cells); glucose deprivation; localized hypoxia; and high extracellular K + (ATP depletion results from increased activity of the Na +, K+-ATPase in the cell plasma membrane required to maintain the proper K+/Na + ratio between the intracellular and extracellular environments). Localized hypoxia can result from poor blood flow, the result of obstruction of blood vessels responsible for the territorial distribution of the blood (a condition known as ischemia). Ischemia may result from narrowing of the lumen of the blood vessels (e.g., deposition of lipids in the vessel wall, which leads to atherosclerosis; see Chapter 20) or from formation of blood clots within the vessels. Ischemic necrosis leads to formation of an infarct (the process is called infarction). When cells of the myocardium die as a result of severe ischemia, the lesion is known as a myocardial infarct. The amount of enzymes released depends on the degree of cellular damage, the intracellular concentrations of the enzymes, and the mass of affected tissue. The nature of the insult (viral infection, hypoxia, or surgical, chemical, or mechanical trauma) has no bearing on the enzymes released into the circulation. The nature of the enzymes released also reflects the severity of the damage. Mild inflammatory conditions are likely to release cytoplasmic enzymes, whereas necrotic conditions yield mitochondrial enzymes as well. Thus, in severe liver damage (e.g., hepatitis), the serum as- Clinical Usefulness Earliest marker; not cardiac specific. A relatively early marker; not cardiac specific. A relatively early marker; has higher cardiac specificity over total CK. A relatively early marker; cardiac specific; however elevated in diseases of regeneration of skeletal muscle and chronic renal disease. A relatively early marker; cardiac specific. Late marker; not cardiac specific; LD 1/LD2 determination increases cardiac specificity. partate aminotransferase (AST) level is extremely high (much greater than that of alanine aminotransferase) because the mitochondrial isoenzyme of AST is released in addition to the corresponding cytoplasmic isoenzyme. The amount of enzyme released into the plasma from an injured tissue is usually much greater than can be accounted for on the basis of tissue enzyme concentration and magnitude of injury. Loss of enzymes from cells may stimulate further synthesis of enzymes. In experimental animals, biliary occlusion leads to increased synthesis of hepatic alkaline phosphatase. Many drugs cause an increase in drug-metabolizing enzymes as a result of an increase in de novo synthesis (i.e., enzyme induction). These drug-metabolizing enzymes, located in the smooth endoplasmic reticulum (microsomal fraction; see Chapter 2) of liver and other tissues, catalyze the following chemical reactions: hydroxylation, demethylation, deethylation, acetylation, epoxidation, deamination, glucuronidation, and dehalogenation. Thus, serum levels of some of these enzymes may be elevated following exposure to enzyme-inducing agents, such as ethanol, barbiturates, phenytoin, and polycyclic hydrocarbons. While plasma levels of enzymes can become elevated because of tissue injury, the levels may drop (in spite of continued progress of the injury) to normal (or below normal) levels when the blood circulation is compromised or when the functional part of the tissue is replaced by repair or nonfunctional tissue (e.g., connective tissue, as in extensive fibrosis of the liver in the disease known as cirrhosis). 124 CHAPTER 8 Presence Removal Normal turnover of tissues Leakage through . ] cell membranes - ~ ~ Tissue necrosis/S Increased enzyme synthesis ~ ~___ Non-plasma- ~ specific enzymes ~.... Intravascular inactivation (dilution, lack of substrates and coenzymes, inhibitors, and proteinases) Uptake by tissues, with subsequentinactivation "" Removal by the ~,,N mticuloendothelialsystem Excretion in urine (of lowmolecular-weightenzymes) F I G U R E 8-1 Factors affecting the presence and removal of non-plasma-specific enzymes from plasma. Inactivation or removal of plasma enzymes may be accomplished by several processes: denaturation of the enzyme due to dilution in plasma or separation from its natural substrate or coenzyme; presence of enzyme inhibitors (e.g., falsely decreased activity of amylase in acute pancreatitis with hyperlipemia); removal by the reticuloendothelial system; digestion by circulating proteinases; uptake by tissues and subsequent degradation by tissue proteinases; and clearance by the kidneys of enzymes of low molecular mass (amylase and lysozyme). A schematic representation of the causes for the appearance and disappearance of non-plasma-specific enzymes is shown in Figure 8-1. Since enzymes differ in the rates of their disappearance from plasma, it is important to know when the blood specimen was obtained relative to the time of injury. It is also important to know how soon after the occurrence of injury various enzyme levels begin to rise. The biological half-lives for enzymes and their various isoenzymes are different. We can illustrate this by examining the disappearance rates of the lactate dehydrogenase (LDH) isoenzymes. LDH consists of four subunits of two different types: H (heart) and M (muscle). The subunits combine to yield a series of five tetramers: LDHI (H4), LDH2(H3M), LDH3(H2M2), LDH4(HM3), and LDHs(M4). The overall rate of disappearance of LDH activity from plasma is biphasic because of the more rapid disappearance of LDH5 (the predominant isoenzyme of liver and skeletal muscle), followed by the relatively slower removal of LDH1 (the predominant isoenzyme of heart, kidney cortex, and erythrocytes). The remaining LDH isoenzymes have intermediate rates of disappearance. In chronic disease states, the plasma enzyme levels continue to be elevated. The use of appropriate normal ranges is important in evaluating abnormal levels of plasma enzymes. However, an abnormal isoenzyme pattern may occur despite normal total activity (see above). The standard unit for enzyme activity was discussed in Chapter 6. The normal range is affected by a variety of factors: age, sex, race, degree of obesity, pregnancy, alcohol or other drug consumption, Enzymes II1: Clinical Applications and malnutrition. Drugs can alter enzyme level in vivo and interfere with their measurement in vitro. Enzyme activities may also be measured in urine, cerebrospinal fluid, bone marrow cells or fluid, amniotic cells or fluid, red blood cells, leukocytes, and tissue cells. Cytochemical localization is possible in leukocytes and biopsy specimens (e.g., from liver and muscle). Under ideal conditions, both the concentration of the enzyme and its activity would be measured. Radioimmunoassay (RIA) and its alternative modes such as fluorescence immunoassay (FIA), fluorescence polarization immunoassay (FPIA), and chemiluminescence immunoassay (CLIA) (discussed later), can be used to measure enzyme concentration as well as other clinically important parameters. M e a s u r e m e n t of Enzyme Activity In the assessment of enzyme levels in the clinical laboratory, the most frequently used procedure consists of measuring the rate of the enzyme-catalyzed chemical reaction. The initial rate of an enzymatic reaction is directly proportional to the amount of enzyme present when the substrate concentrations are maintained at saturating levels (i.e., zero-order kinetics with respect to substrate concentration) and other factors (e.g., pH, temperature, and cofactors) are maintained at optimal and constant levels (see Chapter 6). Under these conditions, the rate of substrate removal or product formation in a given time interval is directly related to enzyme activity. The reaction rate is determined by measuring product formation (or substrate removal) between two fixed times or by continuously monitoring the reaction with time. For accuracy, it is preferable to measure product formation rather than substrate removal because the former involves measurement of a change in concentration from an initial zero or low level to higher levels, which is analytically more reliable than the reverse. Both methods, fixed-time and continuous monitoring, are kinetic procedures. A schematic diagram of an enzymatic reaction is shown in Figure 8-2. The true rate of enzyme activity is obtained only when the reaction rate is measured in the linear region (a period of constant reaction rate and of maximum velocity). Inaccurate results are obtained if the rate is measured during nonlinear or nonmaximum phases. In fixed-time procedures, in which a single given interval of time is chosen to measure enzyme activity, it is essential to select reaction conditions, such as concentration of substrate, pH, temperature, and cofactors, that will provide linearity with maximum slope during the time period in question. False negative values for enzyme rates may arise from substrate depletion, inhibition of the enzyme by product, increase in the reverse reaction due to product accumulation, denaturation of the SECTION 8.1 Diagnosis and Prognosis of Disease F I G U R E 8-2 Diagrammatic representation of the measurement of the activity of an enzyme, showing product formation as a function of time. The true activity of the enzyme is calculated from data obtained when the reaction rate is linear with maximum velocity. The reaction rate is directly proportional to the amount of active enzyme only when the substrate concentrations are maintained at saturating levels and when other variables (e.g., pH, and cofactors) are held constant at optimal conditions. enzyme, presence of certain endogenous metabolites, and drugs (or their metabolites). In the design of an enzyme assay, a key element is selection of a suitable physical or chemical technique for following the appearance of a product or the disappearance of a substrate. The rate of enzymatic reactions can be monitored continuously by photometric procedures (such as light absorption, fluorescence, or optical rotation) if the reaction is accompanied by a change in optical properties. For example, serum alkaline phosphatase, used in the diagnosis of hepatobiliary and bone diseases, is measured by employing its ability to catalyze the hydrolysis at alkaline pH of the colorless synthetic substrate p-nitrophenylphosphate to the yellow-colored product p-nitrophenol. The rate of reaction can be measured from changes in absorption at 405 nm. Many enzymatic reactions can be followed by a change in absorbance at 340 nm if they are linked (either directly or indirectly) to a dehydrogenase reaction requiring a nicotinamide adeninedinucleotide (NAD + or NADP +). The coenzyme absorbs ultraviolet light at 340 nm in the reduced state but not in the oxidized state (Figure 8-3). Hence, changes in reaction rate in either direction can be followed by measurement of the absorbance at 340 nm. An example of one such enzyme assay is given below. Red cell glucose-6-phosphate dehydrogenase (Chapter 15) can be specifically assayed in a red cell hemolysate. The enzyme catalyzes the reaction D-Glucose 6-phosphate + NADP + D-glucono-6-1actone 6-phosphate + NADPH + H + 125 F I G U R E 8-3 Absorption spectra of NAD + (NADP +) and NADH (NADPH). At 340 nm, the reduced coenzymes (NADH or NADPH) show significant absorbance, whereas the oxidized forms (NAD + or NADP +) show negligible absorbance. Thus, many enzymatic reactions can be monitored at 340 nm if the reaction is directly or indirectly dependent upon a dehydrogenase reaction involving a nicotinamide adenine dinucleotide as a coenzyme. Since NADPH absorbs light at 340 nm and NADP + does not (Figure 8-3), this reaction can be followed by measurement of the change in absorbance at this wavelength with time. A similar assay (with lactate and NAD +) can be used for serum lactate dehydrogenase. The difference in absorbance is measured so readily that a number of assays make use of it directly or indirectly. In the latter case, the reaction to be measured is linked by one or more steps to a reaction in which a nicotinamide adenine dinucleotide is oxidized or reduced. Thus, in the measurement of aminotransferases (Chapter 17), one of the products of the primary reaction serves as a substrate for a secondary reaction in which NADH is required. For example, in the assay of aspartate aminotransferase, L-Aspartate + c~-ketoglutarate ~ oxaloacetate (also known as 2-oxoglutarate) § L-glutamate (primary reaction) the oxaloacetate formed in the primary reaction is reduced to L-malate by NADH in the presence of malate dehydrogenase: malate Oxaloacetate § NADH § H + >L-malate dehydrogenase § NAD + (indicator reaction) This secondary reaction is an indicator reaction, i.e., the one whose rate is followed. The primary, not the secondary, 126 CHAPTER 8 reaction must be the rate-limiting step. The indicator reaction should be capable of instantaneous removal of the product formed in the primary reaction to prevent or minimize reversal of the primary reaction. Maintenance of a large excess of the second enzyme (malate dehydrogenase) in the reaction mixture fulfills this requirement. The indicator reaction must function at the concentration of the substrate (oxaloacetate) of the indicator enzyme, so that the rate of the indicator reaction is directly proportional to substrate concentration. Under these conditions, the rate of reaction catalyzed by the indicator enzyme is directly proportional to the rate of product formation in the primary reaction. Thus, during the initial phase of the reaction, the indicator reaction must wait for a period of time known as the lag phase for the primary reaction to generate adequate quantities of oxaloacetate to permit the maximum rate of conversion of NADH to NAD +. In nicotinamide adenine dinucleotide-linked assays, endogenous metabolites and enzymes in the serum may cause oxidation or reduction of the coenzyme, thereby introducing errors. For example, in the AST assay, the NADH of the indicator reaction may be oxidized by the presence of pyruvate and of LDH in the serum: Pyruvate + NADH + H + ~ L-lactate + NAD + This reaction falsely raises the measured activity of AST. A way to prevent this is to include a preincubation step in the assay procedure. This step consists of a time period during which all components of the reaction mixture except one of the substrates of the primary reaction (in this case, c~-ketoglutarate) are allowed to incubate. This period permits all undesirable reactions to reach completion before the primary reaction is initiated by addition of o~-ketoglutarate. Because of the need for rapid and accurate measurement, automated procedures have been introduced. 8.2 Serum Markers in the Diagnosis of Tissue Damage Myocardium Coronary artery occlusion causes heart tissue damage due to ischemia and can lead to myocardial infarction (MI). The immediate and common cause of artery obstruction is formation of a thrombus. Antithrombolytic therapy (Chapter 36), with streptokinase or recombinant tissue plasminogen activator, protects the myocardium from permanent damage by restoring of blood flow. An early diagnosis of acute MI (AMI) is crucial for proper Enzymes ii1: Clinical Applications management. A patient's history, presence of chest pain, and electrocardiograms are problematic in the diagnosis of AMI. Therefore, measurements of circulatory proteins (enzymes and nonenzyme proteins) released from the necrotic myocardial tissue are useful in the diagnosis of AMI. Characteristics of an ideal myocardial injury marker are cardiac specificity, rapid appearance in the serum, substantial elevation for a clinically useful period of time and ease and rapidity of the analytical essay. At present, no serum marker fulfills all of these criteria. Some cardiac markers that appear in plasma are myoglobin, LDH, CK, and troponins. Measurements are made at the appropriate time intervals based upon the appearance of the marker in the plasma (Table 8-1). Frequently utilized markers are CKMB and cardiac troponin I (cTn I). Troponins consist of three different proteins I, C, and T, and are expressed in both cardiac and skeletal muscle. The tripartite troponin complex regulates the calcium-dependent interaction of myosin with actin (Chapter 21). Troponins are encoded by different genes. Cardiac I and T isoforms have unique structural differences from their skeletal muscle counterparts. However, cTn T like CKMB undergoes ontogenic recapitulation and is reexpressed in regenerating skeletal muscle and in patients with chronic renal failure. CKMB is also present in the skeletal muscle, albeit in small concentration. Compared to the myocardium (about 360- 400 g), skeletal muscle consists of a much larger mass (about 40% of total body mass). In rhabdomyolysis (disintegration or breakdown of muscle) CKMB and myoglobin appear in plasma in significant quantities. Myoglobin, although an early marker (Table 8-1), lacks specificity, and CKMB is elevated in many circumstances other than cardiac injury, e.g., rhabdomyolysis, chronic renal disease, and degenerative diseases of skeletal muscle. CKMB has a subform in the plasma due to the fact the M subunit undergoes cleavage of a lysine residue from the carboxy terminus by the plasma enzyme carboxypeptidase N. Tissue and the plasma subforms of CKMB have been designated as CKMB2 and CKMBI, respectively. The ratio of the serum levels, CKMB2/CKMB1 can also yield information useful in the early diagnosis of MI. Measurement of LDH isoenzymes (LDHI and LDH2) also lacks specificity; they appear significantly later after the myocardia! injury and show ontogenic recapitulation. Cardiac troponin I, a highly specific marker for AMI, does not suffer from these disadvantages and appears in the plasma as early as CKMB and persists as long as LDH isozymes. For these reasons, serial serum cTn I measurements may be superior in the detection of MI even in patients with chronic renal disease, rhabdomyolysis, or diseases of skeletal muscle regeneration (e.g., muscle dystrophies). SECTION8.2 Serum Markers in the Diagnosis of Tissue Damage Gallbladder Common bile duct 127 f tomac i _ ~ ~ ~ - - ~- Pancreas Accessory pancreatic duct (duct of Santorini) Gallstone in Ampulla of Vater Main pancreatic duct (duct of Wirsung) Duodenum F I G U R E 8-4 Pancreatic duct obstruction by a gallstone at the ampulla of Vater. Obstruction can lead to pancreatitis, from induction of bile reflux, which eventually damages acinar cells of the pancreas. Pancreas The pancreas is both an exocrine and an endocrine gland. The exocrine function is digestion of food substances (Chapter 12); the endocrine function involves glucose homeostasis (Chapter 22). Acute pancreatitis is characterized by epigastric pain; it is an inflammatory process and potentially fatal. Obstruction of the pancreatic duct (Figure 8-4), which delivers pancreatic juice to the small intestine, by gallstones (Chapter 12) or alcohol abuse is the most common cause of acute pancreatitis, representing 80% of all causes. The pathophysiology is due to inappropriate release of pancreatic enzymes and their premature activation. The principal pancreatic enzyme is trypsinogen, which after activation to trypsin converts many other enzymes to their active forms. Some of these are kallikrein, phospholipase A2, elastase, enzymes of blood coagulation and fibrinolysis, and complement. Effects of these abnormal processes are autodigestion of the pancreas, vasodilation, increased capillary permeability, and disseminated intravascular coagulation. These can result in circulatory collapse, renal insufficiency, and respiratory failure. Laboratory diagnosis of acute pancreatitis involves the measurement of the pancreatic digestive enzymes: amylase and lipase (Chapter 12). Elevated serum amylase level is a sensitive diagnostic indicator in the assessment of acute pancreatitis, but it has low specificity because there are many nonpancreatic causes of hyperamylasemia. Furthermore, amylase (M.W. 55,000) is rapidly cleared by the kidneys and returns to normal levels by the third or fourth day after onset of the abdominal pain. Amylase activity in the serum appears within 2-12 hours after the onset of pain. Serum lipase also is used to assess pancreatic disorders and has a higher specificity than serum amylase. It appears in the plasma within 4-8 hours, peaks at about 24 hours and remains elevated for 8-14 days. Measurements of amylase and lipase provide 90-95 % accuracy in the diagnosis of acute pancreatitis with abdominal pain. Pancreatic isoamylase level has not proven useful in comparison with measurements of both amylase and lipase. The catalytic activity of lipase requires the presence of both bile salts and colipase (Chapter 12) and must be incorporated in assays of serum lipase activity. Since exocrine cells of the pancreas contain many enzymes, attempts have been made to use markers other than amylase and lipase to diagnose acute pancreatitis. One such enzyme is trypsinogen. It is a 25,000-Da protein that exists in two isoenzyme forms: trypsinogen-1 (cationic) and trypsinogen-2 (anionic). Both forms are readily filtered through the kidney glomeruli. However, the tubular reabsorption of trypsinogen-2 is less than for trypsinogen-1; a dipstick method has been developed to detect trypsinogen-2 in the urine of patients suspected of having acute pancreatitis. The test strip contains monoclonal antibodies specific for trypsinogen-2. Liver The liver is the largest glandular organ and its parenchymal cells are called hepatocytes. Liver has numerous functions, including metabolism, detoxification, formation and excretion of bile, storage, and synthesis. Liver diseases include alcohol abuse, medication, chronic hepatitis B and C infections, steatosis and steatohepatitis, autoimmune 128 hepatitis, hemochromatosis, Wilson's disease, otlantitrypsin deficiency, malignancy, and poisons and infectious agents. These disorders require specific laboratory testing procedures and are discussed at the appropriate places in the text. The serum enzymes used in assessment of liver function are divided into two categories: (1) markers used in hepatocellular necrosis and (2) markers that reflect cholestasis. Serum enzymes used as markers of cholestasis include alkaline phosphatase, 5'-nucleotidase, and y-glutamyl transferase. Alanine aminotransferase and aspartate aminotransferases are markers for hepatocellular necrosis. Other tests used in the assessment of liver disorders include measurement of bilirubin, albumin, and ot-fetoprotein. 8.3 Enzymes as Analytical Reagents The use of enzymes as analytical reagents in the clinical laboratory has found widespread application in the measurement of substrates, drugs, and activity of other enzymes. Above we discussed the use of enzymes as reagents in the coupled assay of aspartate aminotransferase. Enzyme-dependent procedures, used in the assay of substrates such as glucose, urea, uric acid, and cholesterol, provide many advantages over classical chemical procedures. These advantages include specificity of the substrate that is being measured and direct measurement of the substrate in a complex mixture that avoids preliminary separation and purification steps such as serum. A reagent enzyme can be used in substrate measurements by two methods: end-point and rate assays. In an end-point assay, the substrate is completely converted to product before it is measured; in the rate assay, a change in substrate concentration produced during a fixed-time interval is measured. This second method, also referred to as the two-point kinetic method, when carried out under constant conditions of pH, temperature, amount of enzyme, and time interval, yields very accurate values for substrate concentration. This procedure is calibrated with standard solutions of the substrate. Of course, the first-order reaction condition with respect to substrate must be maintained by keeping the reagent enzyme concentration high. Under these conditions, when average velocities during the chosen time interval are plotted against various standard substrate concentrations, the profile obtained should exhibit a straight line from which unknown values of substrate can be calculated. Optical properties can be used in monitoring assay procedures as they are in measuring enzyme activity. If the primary substrate or product does not have a suitable optical property (e.g., absorption in visible or ultravio- CHAPTER 8 Enzymes II1: Clinical Applications let light), then a coupled assay is constructed in which one or more auxiliary enzymes are employed to form an ultimate product that possesses an easily measured optical property. For example, glucose in a biological specimen can be measured by the following reactions under optimal conditions: hexokinase D-Glucose + ATP >D-glucose 6-phosphate + ADP glucose-6-phosphatase dehydrogenase D-Glucose 6-phosphate + NADP + < > D-glucono-8-1actone 6-phosphate + NADPH + H + The second reaction (in which NADPH is formed) functions as the indicator reaction. Although the hexokinase reaction is relatively nonspecific and acts on hexoses other than glucose (Chapter 13) to form 6-phosphate esters, the indicator reaction is specific for glucose 6-phosphate making the overall assay procedure highly specific for glucose. Enzymes immobilized on an insoluble surface can be used repeatedly in substrate assays. This type of assay is feasible if the reaction product can be measured directly. Immobilization can be accomplished through chemical linkages involving diazo, triazine, and azide groups with many types of insoluble matrices, such as diethylaminoethylcellulose, carboxymethylcellulose, agarose, microcrystalline cellulose, and inner walls of plastic tubings. Enzymes immobilized on the inner surface of plastic tubings are particularly useful in continuous-flow analyzers. Reagent enzymes that have been immobilized include glucose oxidase, urease, c~-amylase, trypsin, and leucine aminopeptidase. Reagent enzymes and antibodies formed against specific molecules can be combined to determine the concentration of a variety of molecules to which antibodies (Chapter 35) can be formed. Such analytical procedures are known as enzyme immunoassays (EIAs). The reagent enzyme can be linked to antibodies or antigens such that the complexes possess immunological or enzymatic activity. Antibodies can be raised in vertebrate animals when injected with specific proteins (antigens) foreign to them. Macromolecules other than proteins can also be antigenic. Low-molecular-weight compounds (e.g., substrates, drugs) by themselves do not elicit antibodies but do so if covalently linked to a carrier protein (e.g., albumin) before injection. The term hapten designates the low-molecular-weight substance that can combine with the antibody produced against the cartier protein complex. EIAs are either heterogeneous or homogeneous. A heterogeneous assay consists of at least one separation step in which the bound enzyme-labeled 129 SECTION8.3 Enzymes as Analytical Reagents Specific antibody against the antigen Adsorption of antibody onto a solid surface, followed by washing procedure. An inert solid surface (e.g., a bead) Ant~en 1111111111111111 llllll llF Incubation with the test specimen containing antigen, which binds to the specific antibody, followed by aspiration and washing procedure. Incubation with enzyme-linked specific antibody, which binds wherever the antigen is affixed, followed by washing and aspiration procedure. Incubation with specific substrate, and quantitation •'•./Substrates of products formed. Under standardized and optimal conditions, the concentrations of products are directly proportional to the concentration of antigen. F I G U R E 8-5 Diagrammatic representation of an ELISA (solid-phase, sandwich technique) for an antigen. reagent is separated from the unbound enzyme, enabling the measurement of either bound or free activity. A procedure based upon this principle is the enzyme-linked immunosorbent assay (ELISA), which is analogous to an RIA. An example of a heterogeneous immunoassay that uses a solid-phase system is shown in Figure 8-5. This method consists of coating or adsorbing antibodies generated in an animal (e.g., guinea pig) against a human antigen, whose concentration is to be determined in a test serum sample, onto a solid surface (e.g., beads or inner surface of a test tube) and incubating with the serum specimen. During the first incubation step, the antigen combines with its specific antibody and is fixed to a solid surface. Subsequently, the unreacted serum components are removed by aspiration of the fluid, and the solid surface (containing antibody-antigen complexes) is washed with suitable buffers. Incubation with antibodies covalently linked to enzyme molecules follows. During this step, the enzymelabeled antibody (E-Ab) will combine wherever the antigens are affixed; a washing procedure then removes the unbound E-Ab conjugates. Finally, incubation with the substrate specific for the enzyme yields a colored product that is quantitated by suitable spectrophotometric methods. The time interval for the substrate incubation step and other reaction conditions must be kept constant for both test sera and the standards. The enzyme reaction is stopped by altering the pH of the reaction mixture by adding an acid solution (e.g., 1 N hydrochloric acid). The change in absorbance of color is proportional to the concentration of antigen in the test sera. A standard curve is obtained by plotting known antigen concentrations against their absorbances. Various modifications of this technique are in use. For example, if the concentration of an antibody is to be determined, the process can begin with immobilization of the antigen onto the solid phase. The enzymes used as labels should have a high turnover number, act on substrates that are stable and soluble, yield easily measurable products, be obtainable in a highly purified form, and be relatively inexpensive. Enzymes that fit these criteria are horseradish peroxidase, glucose oxidase, E. coli or calf-intestine alkaline phosphatase, catalase, and/3-D-galactosidase. The covalent linkage of the enzyme to the protein (antigen or antibody) through free amino groups can be accomplished with the bifunctional reagent glutaraldehyde. The periodate oxidation method (Chapter 9), involving the carbohydrate side-chains of proteins, also yields reactive groups useful in the preparation of enzyme conjugates. The ELISA exhibits high levels 130 of both sensitivity and specificity. The sensitivity, which is due to the amplification factor introduced by way of the catalytic activity of the labeled enzyme, can equal (with comparable precision) that obtainable with RIA. The specificity is attributable to specific molecular recognition properties of antigens and antibodies. The ELISA may be more advantageous than RIA because ELISA reagents have longer shelf lives than do many radioisotopes (e.g., 125I-labeled reagents) and present no health hazards. The ELISA also has been adapted to identify antigens or antibodies in tissue slices by the use of protein-peroxidase conjugates. Homogeneous EIA procedures have been especially useful for rapid determination of low-molecular-weight substances (haptens). Thus, these procedures have found application in therapeutic drug monitoring and toxicology. A commercial reagent for the assay of many drugs is available under the trade name of EMIT (EnzymeMultiplied Immunoassay Technique). Figure 8-6 diagrams the steps involved in this procedure. The principle is based on competition between the enzyme-labeled hapten and free hapten in the test serum for binding with a limited amount of a specific antibody. This assay requires a hapten covalently linked to an enzyme (e.g., glucose-6-phosphate dehydrogenase, lysozyme, or malate dehydrogenase), with retention of enzymatic activity, and antibodies raised against the hapten (through injection into an animal of the hapten covalently linked to a carrier protein) that inhibit enzyme activity when they combine with the hapten-linked enzyme reagents. The inhibition by the antibody of catalytic activity of the enzyme-linked hapten complex may be due to steric hindrance or to conformational constraints affecting access of substrate of the active center. This reaction system consists of the test specimen, the enzyme-labeled hapten, a limited amount of the antibody specific to the hapten, and the substrate. Any haptens present in the test serum compete with the hapten linked to the enzyme for binding with the antibody. The unbound hapten-linked enzyme acts on the substrate to convert it to an easily measurable product. Thus, the enzyme activity is directly correlated with the free hapten concentration in the test specimen. The method is calibrated with known standard concentrations of the hapten. The ELISA and EIA receptor systems measure substances at concentrations as low as a few nanograms (10 -9 g). This sensitivity is not sufficient for detecting many substances and alternate methods have been devised. One is chemiluminescence immunoassay (CLIA), which can measure concentrations in femtogram (10-15 g) quantities. CLIA depends on the detection of emitted light associated with the dissipation of energy from a substance CHAPTER8 Enzymes II1: Clinical Applications F i ( ; U R E 8-6 Diagrammatic representation of a homogeneous enzyme immunoassay procedure for the determination of low-molecular-weight compounds (haptens). excited electronically as a result of a chemical reaction. An example of a chemiluminescent tracer is acridinium ester conjugated to a desired protein, polypeptide, or other organic molecule (Figure 8-7). CLIA is similar to EIA and ELISA techniques except that the final receptor enzyme assay is replaced with a chemiluminescent tracer followed by measurement of light released as a result of the chemical reaction. The principles of a chemiluminescence competitive binding assay are shown in Figure 8-8. 8.4 Enzymesas Therapeutic Agents Enzymes have found a few applications as therapeutic agents. Some examples are transfusion of fresh blood or its active components in bleeding disorders, oral administration of digestive enzymes in digestive diseases SECTION8.4 Enzymes as Therapeutic Agents CH3 131 C !~ H202, Alkaline pH (H02") ~ I ~0 0 H = C .O, o ~C=O O" (.) R=protein or peptide or an organic R molecule Acridinium Ester C !~ OH3 ! -- f 0 Light, C02 10-methylacridinium (Electronically excited) F I G U R E 8-7 Acridinium ester used as a chemiluminescent tracer. Labeled acridinium ester in the presence of alkaline hydrogen peroxide undergoes chemical changes producing light that is detected at 430 nm by a photomultiplier detector. ~ + ~ + ~ 0 Solid Phase Antibody Antigen in Serum Sample cc cc cc Antigen Labeled with Chemiluminescent Compound (CC) CC CC CC F I G U R E 8-8 Competitive binding chemiluminescence assay. The chemiluminescent competitve binding assay is similar to a RIA. The acridinium ester-labeled substance and the endogenous substance compete with the specific antibody that is available in limited concentration. The concentration is determined by the quantity of tracer that binds to the antibody. The use of solid-phase antibody simplifies separation of free from bound tracer. 132 (e.g., cystic fibrosis),administration of fibrinolytic enzymes (e.g., streptokinase) to recanalize blood vessels occluded by blood clots (thrombi) in thromboembolic disorders (e.g., pulmonary embolism, acute myocardial infarction), treatment of selected disorders of inborn errors of metabolism (e.g., Gaucher's disease), and cancer therapy (e.g., L-asparaginase in acute lymphocytic leukemia). For enzymes to be therapeutically useful, they should be derived from human sources to prevent immunological problems. Although enzymes derived from human blood are readily obtainable, enzymes derived from tissues, which would be particularly useful in the treatment of inborn errors of metabolism, are difficult to obtain in adequate quantities. Transport of specific enzymes to target tissues is also a problem, but some recent advances and commercial applications (e.g., propagation of human tissue culture cell lines, isolation and cloning of specific genes) have the potential of overcoming these difficulties. Such techniques have been used in the production of peptide hormones such as somatostatin and insulin, interferon, and tissue plasminogen activator. In the treatment with enzymes or proteins, covalent attachment of an inert polymer polyethylene glycol (PEG) provides many therapeutic benefits. These include slowing the clearance, diminished immunogeneity, prevention of degradation, and binding to antibody. PEG-enzyme therapy is used in the treatment of immunodeficiency disease caused by adenosine deaminase deficiency (Chapter 27) CHAPTER8 Enzymes II1: Clinical Applications and PEG-interferon alfa complex (peginterferon alfa-2a) is used in treatment of chronic hepatitis C infection. Ultimately, however, when a gene is cloned, techniques will be developed to incorporate it into the genome of persons lacking the gene or having a mutated gene. Supplemental Readings and References N. V. Bhagavan, A. R Goldstein, S. A. A. Honda, et al.: Role of cardiac troponin I in the evaluation of myocardial injury. Journal of Clinical Laboratory Analysis 12, 276 (1998). L. Coudrey: The troponins. Archives oflnternal Medicine 158, 1173 (1998). R. E Dudley: Chemiluminescence immunoassay: An alternative to RIA. Laboratory Medicine 21, 216 (1990). A. H. Gershlick and R. S. More: Treatment of myocardial infarction. British Medical Journal 316, 280 (1998). E. A. Kemppainen, J. I. Hedotrom, E A. Puolakkainen, et al.: Rapid Measurement of Urinary Trypsinogen-2 as a screening test for acute pancreatitis. New England Journal of Medicine 336, 1788 (1997). K. Mergener and J. Baillie: Acute Pancreatitis. British Medical Journal 316, 44 (1998). D. S. Pratt and M. M. Kaplan: Evaluation of abnormal liver-enzyme results in asymptomatic patients. New England Journal of Medicine 342, 1266 (2OOO). J. J. Reichling and M. M. Kaplan: Clinical use of serum enzymes in liver disease. Digestive Diseases and Sciences 33, 1601 (1988). W. Steinberg and S. Tenner: Acute pancreatitis. New England Journal of Medicine 330, 1198 (1994). S. Zeuzem, S. V. Feinman, J. Rasenack, et al: Peginterferon alfa-2a in patients with chronic hepatitis C. New England Journal of Medicine 343, 1666 (2OOO).