* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Health, Gnotobiology and Infectious Diseases
Monoclonal antibody wikipedia , lookup
Immunocontraception wikipedia , lookup
Herd immunity wikipedia , lookup
Transmission (medicine) wikipedia , lookup
Social immunity wikipedia , lookup
DNA vaccination wikipedia , lookup
Hepatitis B wikipedia , lookup
Vaccination wikipedia , lookup
Sociality and disease transmission wikipedia , lookup
Sjögren syndrome wikipedia , lookup
Globalization and disease wikipedia , lookup
Adoptive cell transfer wikipedia , lookup
Germ theory of disease wikipedia , lookup
Autoimmunity wikipedia , lookup
African trypanosomiasis wikipedia , lookup
Immune system wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
Molecular mimicry wikipedia , lookup
Adaptive immune system wikipedia , lookup
Immunosuppressive drug wikipedia , lookup
Polyclonal B cell response wikipedia , lookup
Innate immune system wikipedia , lookup
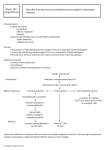
LATG: Chapters 10-11 Infectious Diseases Immunology Health Maintenance • Maintaining lab animal health requires – Proper environment. – Proper food and water. – Disease prevention program. – Disease detection program. – Contingency plan if disease is detected. Disease Prevention • Type of program depends upon species. • Rodents--primarily review of vendor data and procedures in place to prevent introduction and spread of disease. • Nonrodents--As for rodents but may also have other facets such as vaccinations, dewormings etc. Disease Detection • Like NORAD, PADDS (Pfizer Animal Disease Detection System) relies on • Early warning system--technicians who check animals daily. • Early response--veterinary technicians who evaluate reported problems. • Final response--delivered after evaluation and consultation with veterinarian and PI. Disease Detection • A rodent sentinel program is in place to screen for potential viral, bacterial and parasitic contaminants. • In the rare instance of an actual infection steps are taken to evaluate the extent of the infection and eliminate it. Pathogenic Organisms • Life forms that have the potential to cause disease under the proper conditions. • Text classifications – Bacteria – Fungi – Viruses – Parasites Biology Influencing Organisms • In laboratory animal science we are also very concerned with biology influencing organisms. • These organisms may or may not cause clinical disease. • Biological systems can be influenced even by subclinical infections. Viruses • Small particles made up of nucleic acid and a protein capsule. • Viruses may also be covered by an envelope • Many viruses can infect laboratory animals, most do not cause clinical disease. • Viruses are divided into two main classes. – DNA viruses – RNA viruses DNA Viruses of Mice • • • • • Mousepox (Ectromelia) Minute virus of mice Cytomegalovirus Polyoma virus Mouse parvo virus DNA viruses of rats • • • • Polyoma virus (in nude rats) Adenovirus Kilham rat virus Rat parvo virus RNA viruses of mice • • • • • • Mouse hepatitis virus (MHV) Sendai Lymphocytic choriomeningitis Reovirus Hantavirus Retroviruses--mouse leukemia virus and mouse mammary tumor virus RNA viruses of rats • • • • Sialodacryoadenitis virus (SDAV) Sendai Pneumonia virus of mice Hantaan virus Bacteria • Many bacteria in nature are beneficial. • In nearly all mammals there are more bacterial cells than mammalian cells • Consist of a cell membrane, a cell wall and cytoplasm. Bacteria • Classified by – Morphology – Size – Staining characteristics – Formation of spores – Nutrient requirements – Biochemical reactions • All are prokaryotes Bacterial Morphology • Cocci (spherical) – Pairs--Diplococci – Chains--Streptococci – Clusters--Staphylococci • Rods, may be straight or slightly curved • Spiral shaped Bacterial Staining Characteristics • Classified into Gram negative and Gram positive groups • Gram positive--dark blue/violet stain, due to a thick cell wall • Gram negative--red stain, due to a thin cell wall with high lipid content Fungi • Many fungi in nature are beneficial • Used to make – bread – beer – wine – antibiotics • A few fungi are pathogenic • All are eukaryotes Beneficial fungus • Saccharomyces cervisae Fungi • Pathogenic species classified into – Superficial mycoses – Systemic mycoses Superficial mycoses • Infect superficial tissues; skin, hair and nails. • Commonly called “ringworm” • See scaliness and alopecia (hairloss), sometimes redness Systemic mycoses • Infect deep tissues; lung, bone, CNS, GI tract. • Often associated with certain geographic areas – Lower Sonoran desert--Coccidioides immitis – Central and southeastern US-Blastomyces spp. Parasites • Large group of single cell (protozoans) and multi-cell (metazoans) animals which must coexist on another animal during some part of their life cycle • A parasite must also have the potential for causing disease in the host Parasites • Websites of interest • Parasites and Parasitological Resources – http://www.biosci.ohiostate.edu/~parasite/home.html • Identification and Diagnosis of Parasites of Public Health Concern – http://www.dpd.cdc.gov/DPDx/Default.htm Parasite Lifecycles • “If you know the enemy and know yourself, you need not fear the result of a hundred battles.” Sun-tzu, “The Art of War” • Knowing the life cycle of a parasite is the key to knowing how to prevent and treat infestation. Parasite Lifecycles • Life cycles can be direct or indirect. – Direct--parasite eggs/larva can infect definitive host – Indirect--parasite needs to pass through an intermediate host prior to infecting the definitive host Parasite Hosts • Definitive host--the species of animal responsible for housing the reproductive stage of the parasite • Intermediate host--the species of animal responsible for housing any of the nonreproductive stages of the parasite • Disease can occur in both types of host Protozoan Parasite • • • • Amoebas Flagellates Ciliates Sporozoa Toxoplasma gondii • A sporozoan parasite • Definitive host--cat • Intermediate host--almost any other mammal or bird • Causes self-limiting diarrhea in cats • May cause severe disease in immunosuppressed intermediate host Toxoplasma gondii • Trophozoites in lung fluid from an HIVinfected person • Tissue cyst from a cat T. gondii life cycle Other protozoa • Giardia • Trypanosome Metazoan Parasites • • • • Trematodes--Flukes Cestodes--Tapeworms Nematodes Arthropods--insects, ticks, mites Cestodes--Tapeworms • Parasites which inhabit the GI tract of the definitive host • May cause lesions in many different tissues in the intermediate host • Do not have their own digestive system • Life cycle often indirect but may also be direct Echinococcus granulosus Tapeworm tissue cysts Cysts in a baboon heart Hymenolepis (Rodentolepis) nana • A tapeworm of rodents and humans • Has a direct life cycle Nematodes--The “Roundworms” • Worms that are round in cross-section • Body structure contains a GI tract as well as reproductive organs • Both direct and indirect life cycles • May live in many tissues in both the intermediate and definitive hosts Ascarids • Common intestinal parasite of dogs, cats, swine and humans • Also called roundworms • Both direct and indirect life cycles • Infections in humans can result in visceral larval migrans or ocular larval migrans Toxacara canis life cycle Toxocara canis • Adults • Egg Dirofilaria immitis Heartworm • A nematode parasite that lives in the right side of the heart in dogs and occasionally cats • Life cycle of this parasite requires passage through mosquitoes • Infection can cause heart failure Heartworm life cycle Acanthocephalans • Thorny headed worms • Seen in pigs and nonhuman primates Arthropod parasites • Large group of external parasites that include – Insects – Ticks – Mites Arthropod parasites • In lab animal science most likely to see – Mites – Lice – Fleas Mites • Parasites in the arachnid family • Have eight legs in the adult stage • Live on the skin, sometimes deep in the hair follicle • May be zoonotic Sarcoptic mange mite • Sarcoptes scabiei with multiple subspecies • Infest a multitude of species • Infestation is also called “scabies” • Can cause intense pruritis • Infestation is worse if animal is immunosuppressed Sarcoptic mange in a dog Scabies in a person Prevention of Infectious Disease • In all cases it’s easier to prevent diseases than to treat them • Principles of prevention are simple and usually more cost-effective than treatment Principles of Prevention • • • • Purchase disease free animals Ship them correctly Receive them correctly Use proper practices to keep them disease free • Have detection methods in place • Have a plan for therapy if needed LATG Lecture Series Immunology Historical Background • In 1790’s, Edward Jenner observes that milkmaids who had contracted cowpox (vaccinia virus) were immune to smallpox – In 1797, Jenner inoculates a boy with material from a cowpox lesion, then intentionally infects him with smallpox – Luckily for the inoculated boy, Jenner’s reasoning was correct and the boy was immune Historical Background • Why did Jenner’s technique work? – Smallpox and vaccinia viruses are closely related, allowing cross-protective immune responses Historical Background • In 1870’s , Louis Pasteur accidentally discovers the concept of an attenuated vaccine while studying fowl cholera – Chickens infected with an old culture of fowl cholera bacteria, Pasteurella multocida, became sick but survived and became immune to lethal challenge with virulent bacteria – Attenuation = loss of virulence Historical Background • Pasteur extended the attenuation concept to other infectious diseases. – Sheep vaccinated with heat-treated anthrax bacillus were protected against challenge with live anthrax – Administers an attenuated rabies virus vaccine to a boy who had been bitten by a rabid dog. The Immune System • Immunity = ability to resist diseases caused by foreign infectious (contagious) agents. – – – – – Bacteria (e.g. streptococcus, E. coli) Viruses (e.g. influenza, HIV, polio) Parasites (e.g. protozoan and helminthic) Prions (e.g. “mad cow disease”, scrapie) Fungi (crytococcus, candida) • Some evidence for protection from proliferative diseases caused by cancer cells • Also involved with allergy, transplantation, autoimmunity, immunodeficiency, etc. Pathway to Infectious Disease Exposure Infection Disease Resolution No Infection No Disease Death Pathway to Infectious Disease • ExposureInfectionDiseaseDeath • Host Immunity - operates at two basic levels to restrict progression to disease and death. These are termed innate and adaptive immunity. • ExposureInfection (innate) • ExposureInfectionDisease (adaptive) • ExposureInfectionDiseaseDeath (adaptive) Innate vs. Adaptive Immunity • Innate – “nonspecific” and nonadaptive – Basic resistance mechanisms that an individual is born with (requires no prior experience) – First line of defense against invading pathogens – Acts within minutes to hours – Broadly recognizes certain features shared by various classes of microorganisms • bacterial cell walls • double-stranded RNA of some viruses Innate vs. Adaptive Immunity • Adaptive – Specifically recognize and selectively eliminate invading pathogens – Requires several days to a week for optimal induction the first time a pathogen is encountered (sometimes not fast enough!) – Backs-up the innate response against specific infectious agents, parasitic infections and neoplastic (cancer) transformations. – Mediated by lymphocytes (B and T cells) and antigen presenting cells (macrophages, dendritic cells and B cells) The Innate Immune Response • Anatomic (External) Barriers – Skin (mechanical barrier) – Mucous membranes (normal flora competes; mucus traps microorganisms and cilia propels them out of the body) • Physiological Barriers – Temperature (e.g. fever) – Low pH of stomach, skin – Chemical mediators (lysozyme, interferons, complement, fatty acids) – Species specific physiological differences The Innate Immune Response • Phagocytic Barriers – Phagocytic cells such as macrophages , neutrophils, Natural Killer cells engulf and destroy pathogens • Inflammatory Barriers – Vasodilation, increased vascular permeability – Production of inflammatory mediators such as Creactive protein, histamine, kinins • Species, sex, nutrition, fatigue, age, and genetic constitution are influencing factors. The Adaptive Immune Response • Specificity – Capacity to distinguish among various molecules (antigens) produced by pathogens – Mediated by antigen recognition molecules antibodies, T cell receptor, MHC • Diversity – Capacity to react with an almost limitless variety of antigens (>109 different antibodies can be produced) The Adaptive Immune Response • Memory – Ability to “remember” a previous encounter with an antigen – “Secondary” response is typically induced more quickly and is considerably more vigorous than the “primary” response – Immunological memory can be exploited by vaccination • Self/nonself recognition – Ability to respond to and eliminate foreign antigens without bringing harm to one’s own tissues The Adaptive Immune Response • Humoral immune response – the production and secretion of soluble antibody molecules that neutralize and/or destroy infectious agents • Cell-mediated immune response – the generation of active lymphocytes that work at close range to destroy infectious agents, parasites or other cells Defense Cells of the Adaptive Immune System • B Lymphocytes (B Cells) – Provide antibody-mediated immunity – Originate in the bone marrow in higher vertebrates and the bursa of Fabricius in birds – Develop into plasma cells that produce and secrete antibody Defense Cells of the Adaptive Immune System • T Lymphocytes (T Cells) – Develop in the thymus – Provide cell-mediated immunity – Serve as helper or regulator cells to B cells – Release lymphokines or cytokines that activate macrophages • Macrophages – Attack and destroy viral-infected cells and cancer cells – inhibit certain white blood cells from migrating away from areas in which they are needed Defense Cells of the Adaptive Immune System • Lymphocytes circulate from the bloodstream through the spleen, the lymph nodes, the thoracic duct and back into the bloodstream. Organs of the Immune System • Primary Lymphoid Organs – Thymus – Bone Marrow • Secondary or Peripheral Lymphoid Organs – Lymph Nodes (tissue) – Spleen (blood) – Gut-associated lymphoid tissue (Peyer’s patches) – Tonsils Antigen Processing for the Adaptive Immune Response • Recognition – self or nonself – requires interactions between a signal molecule and a receptor molecule • Processing – transmission of the received signal from the receptor to other molecules and cells – mediated by cytokines • Response Antigen Processing for the Adaptive Immune Response • Response – Organism responds with active immunity against nonself antigens – Humoral and/or cellular immunity depends on: • antigen’s chemical structure • living or dead organism • concentration • route of inoculation – Second response to the same antigen is quicker and stronger than the first (Anamnestic Response) Humoral Immune Response • Antibodies (Abs) – Also known as Immunoglobulins (Ig) – Produced by B lymphocytes – May be membrane bound or found in serum, the fluid portion of blood – Bind to specific sites on antigens or infectious organisms – IgA, IgM, IgG, IgE, IgD Humoral Immune Response • Antibodies – Symmetrical molecule, 2 heavy and 2 light chains – Composed of polypeptides (protein) and carbohydrates – Antigen combining or binding site reacts with antigen – Antibodies + Complement - lyse (cause to break apart) bacteria and infected cells Immunoglobulins • IgG – Most abundant serum Ab – Only Ig that crosses placenta, conferring immunity to the fetus – Also transferred in the colostrum (first milk) after birth – Associated with secondary anamnestic response Immunoglobulins • IgM – Second most abundant Ig – First Ig produced by fetus – First produced in primary immune response to an antigen – IgM titer (concentration) drops as IgG rises – May be on membrane of B cells Immunoglobulins • IgA – Found in mucus secretions of the intestines, lungs, nose and urogenital tract – Also found in tears, bile, saliva and milk (colostrum) – Helps protect body surfaces from invasion by bacteria and viruses – Common Mucosal Immune System Immunoglobulins • IgE – Found in very low concentrations – Levels increase during parasitic infections and other allergic reactions – Attaches to mast cells and basophils which release chemicals like histamine that produce inflammation and cause tissue damage – Over response with IgE associated with hypersensitivity reactions such as hay fever, food and skin sensitivities, other allergies and asthma Immunoglobulins • IgD – Not much known – Sometimes found with IgM on membranes of B cells – may be involved in the recognition process and in the activation of B cells Humoral Immune Response • Primary Immune Response – Lag Phase – Log Phase – Plateau Phase – Decline Phase Humoral Immune Response • Secondary or Anamnestic Immune Response – Response to the same antigen is more rapid and the antibody levels rise higher and last longer than in Primary response – Peaks 2-3 weeks later – Gradual decline over weeks or months – Additional boosters result in stronger anamnestic responses Cell-mediated Immune Response • Mediated by long-lived T cells originating in the thymus • T cells stimulated by an antigen divide into memory cells and killer cells (cytotoxic T lymphocytes, CTL’s) • Lymphocyte blastogenesis - the production of new lymphocytes Types of Immunization • Passive Immunization – Transfer of Abs from an immune animal to a nonimmune animal – Develops immediately after transfer – Temporary immunity, Ab degrades over several weeks – Examples - Abs in colostrum, Abs crossing placenta, antiserum injections Types of Immunization • Active Acquired Immunity – Produced by an animal in its own body in response to exposure to a foreign antigen – Develops slowly after exposure to antigen – Longer, stronger protection than Passive Immunization, especially with periodic reexposure – Memory Types of Immunization • Vaccines – Live, attenuated whole organism vaccines stimulate the best immune response but have the risk of disease transmission (oral polio, measles, rabies, vaccinia) – Dead organism vaccines are more stable in storage, have no risk of disease and suppress contaminating organisms – Adjuvants mixed with vaccines enhance the immune response by prolonging the presence of antigen in the tissue Transplantation of Organs • Histocompatiblity of donor and recipient determines success • Identical twins and inbred animals Diseases of the Immune System • Autoimmune Disease – An organism’s immune system mistakenly recognizes self as nonself – Immune response attacks its own tissues – Autoimmune hemolytic anemia - red blood cells destroyed leading to severe anemia – Multiple Sclerosis - myelin sheath protecting nerves Diseases of the Immune System • Immunodeficiency Disease – Primary immunodeficiency disease • innate error of metabolism or inherited genetic disease • Athymic nude mouse - lack T cells – Secondary immunodeficiency disease • more common than primary immunodeficiency disease • Caused by infectious disease, cancer, aging, poor nutrition, immune suppressing drugs • FeLV, HIV Diseases of the Immune System • Chronic Immune Complex Disease – Chronic infections produce a prolonged elevation of soluble antigens in the blood – Immune complex formed between antigen and bound antibody and deposited in tissues, particularly the kidneys (immune complex glomerulonephritis)