* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download transplantation
Transmission (medicine) wikipedia , lookup
Adaptive immune system wikipedia , lookup
Neglected tropical diseases wikipedia , lookup
Innate immune system wikipedia , lookup
Monoclonal antibody wikipedia , lookup
Kawasaki disease wikipedia , lookup
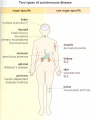
Adoptive cell transfer wikipedia , lookup
Multiple sclerosis signs and symptoms wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
Behçet's disease wikipedia , lookup
Polyclonal B cell response wikipedia , lookup
Graves' disease wikipedia , lookup
Pathophysiology of multiple sclerosis wikipedia , lookup
Anti-nuclear antibody wikipedia , lookup
Multiple sclerosis research wikipedia , lookup
Rheumatic fever wikipedia , lookup
Systemic scleroderma wikipedia , lookup
Globalization and disease wikipedia , lookup
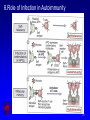
Neuromyelitis optica wikipedia , lookup
Germ theory of disease wikipedia , lookup
Ankylosing spondylitis wikipedia , lookup
Autoimmune encephalitis wikipedia , lookup
Psychoneuroimmunology wikipedia , lookup
Myasthenia gravis wikipedia , lookup
Immunosuppressive drug wikipedia , lookup
Hygiene hypothesis wikipedia , lookup
Systemic lupus erythematosus wikipedia , lookup
Molecular mimicry wikipedia , lookup
Rheumatoid arthritis wikipedia , lookup
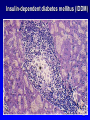
Bo Gao, Ph.D. Email: [email protected] Tel: 54237379 DEPARTMENT OF IMMUNOLOGY INSTITUTE FOR IMMUNOBIOLOGY 2010-07-02 1 Contents: Introduction Organ-Specific Autoimmune Diseases Systemic Autoimmune Diseases Mechanisms of Induction Treatment 2 Introduction 3 Autoimmunity Origins Horror autotoxicus: Literally, the horror of selftoxicity. A term coined by the German immunologist Paul Ehrlich (1854-1915) to describe the body's innate aversion to immunological self-destruction. Paul Ehrlich , Nobel Prize in 1908 for demonstrating production of antibody 4 Clone selection hypothesis Self-reactive lymphocyte were deleted during development Frank Burnet 1900--1990 Nobel Prize 1960 5 Definition of autoimmune disease Disease caused by failure of self-tolerance and subsequent immune responses against self antigens are called autoimmune diseases. 6 5 % to 7% adult affected. Two third women. More than 40 human diseases autoimmune in origin. 7 8 Organ-Specific Autoimmune Diseases Insulin-dependent diabetes mellitus Multiple sclerosis Myasthenia gravis Graves’s disease Hashimoto’ disease Goodpasture’s syndrome …… 9 Systemic Autoimmune Diseases 10 Systemic Autoimmune Diseases Systemic lupus Erythematosus (SLE) Rheumatoid arthritis (RA) Sjögren’s syndrome Scleroderma Dermatomyositis Mixed connective tissue disease (MCTD) ……. 11 Induction Theories for Autoimmune Disorders 12 1. Ag released from hidden location (by injury or infection) Intraocular antigens Sperm Post-traumatic uveitis Orchitis after vasectomy 13 2. Molecular mimicry (Cross-reactions) 14 Molecular mimicry Definition: Determinants of infectious agent mimic a host antigen and trigger self-reactive T-cell clones to attack host tissues. Examples: Rheumatic fever due to group A streptococcus SLE due to Epstein-Barr virus cross reactive with nuclear Sm antigen Lyme artrhritis due to Borrelia burgdorferi reactive with LFA-1 (lymphocyte function antigen-1) 15 Rheumatic fever is a classic example of molecular mimicry 16 3. Inappropriate expression of class II MHC “Wrong” cells induced to express MHC Class II antigen (and act as APCs) – IDDM, Hashimoto’s Additional signals, such as IFN-gamma IL-1 and TNF 17 4.Epitope spreading Definition: Initial response to one self determinant (one peptide) could expand to involve additional determinants on the same molecule as well as additional self-proteins. 18 It explains how a response to one cryptic epitope can mature into a full-blown autoimmune response . 19 5. Polyclonal B cell activation by CMV, EBV, and some G-negative bacteria - T-cell-independent - Large amounts of IgM produced 20 6.Role of Infection in Autoimmunity 21 7. Gene factors in autoimmunity Multiple sclerosis – particular alleles of HLA-DR (DRB1*1501, DRB5*0101) Systemic lupus – lack of C1q and C4 Genetically determined low expression of given self-antigen in the thymus Mutation (usually deletion) of autoimmune regulator-1 gene (AIRE-1) 22 Association between HLA and susceptibilit y to autoimmune disease 23 8.Estrogens and Autoimmunity 24 9.Other factors favoring autoimmunity Lymphocytes abnormalities Cytokine Imbalance (↑IL-2 in SLE) Disturbances of apoptosis ( Deficiencies in Fas, complement, CTLA-4) Toxins, Drugs, Chemicals (including food), UV, Stress 25 THERAPY OF AUTOIMMUNE DISEASES 26 Reduce symptoms Immunosuppression Corticosteroids, azathioprine, cyclophosamide Removal of thymus Plasmapheresis Short-term relief (Grave’s disease, RA, SLE) 27 Reduce inflammation TNF-alpha blockers (RA, Crohn’s dis., psoriasis) e.g., Enbrel, Remicade, Humira IL-1 receptor antagonist (RA) Ab’s against IL6R and IL-15R Statins, shown to lower CRP (RA, MS) 28 Block MHC with similar peptide or antibody Anti-CD4 Blockage of IL-12 activity 29 T cell vaccines (against activated Ag-specific T cells) Monoclonal antibodies against a variety of target antigens Oral induction of tolerance (MS) So far, efforts have been more successful in mice than humans 30 31 Insulin-dependent diabetes mellitus (IDDM) Disease in which the body does not produce enough insulin. It is a “ T cell” Disease. T cells attack and destroy pancreatic beta cells. 32 Insulin-dependent diabetes mellitus (IDDM) 33 Insulin-dependent diabetes mellitus (IDDM) 34 Multiple Sclerosis Myelin sheath of nerves targeted CNS attacked by inflammatory lesions Starts in 20-40 yr. old people Characterized by weakness, paralysis and ocular symptoms MS patients can have autoantibodies and/or self reactive T cells which are responsible for the demyelination 35 Myasthenia Gravis Disease marked by progressive weakness and loss of muscle control Classified as a “B cell” Disease Autoantibodies against nicotinic acetylcholine receptors Eventually destroys it 36 Myasthenia Gravis 37 Graves’s disease Autoantibody mimics TSH, leads to constant thyroid stimulation 38 Hashimoto’s thyroiditis Th1 cells and autoantibodies specific for thyroid Ag’s infiltration of thyroid by L, M, and PC’s hypothyroidism Chronic inflammation and enlargement 39 Normal thyroid gland 40 Hashimoto’s thyroiditis 41 Hashimoto’s thyroiditis (From Robbins Basic Pathology ,2003) 42 Goodpasture’s syndrome Antibodies to membrane antigens in kidney and alveoli in lungs Specificity – part of type IV collagen Complement activation, cell damage, inflammation 43 The anti-basement membrane antibody in Goodpasture’s syndrome forms an even layer on the glomerular basement membrane. 44 Systemic Lupus Erythematosus (SLE) Typical patient: young woman with butterfly rash Symptoms unpredictable (relapsing/remitting) Multisystem (skin, kidneys, joints, heart) 45 Systemic Lupus Erythematosus (SLE) Etiology • Autoantibodies! • Antinuclear Ab present in all patients with SLE... but found in other autoimmune diseases too 46 Systemic Lupus Erythematosus (SLE) What’s so bad about having these autoantibodies? They cause tissue injury! Form immune complexes Cause destruction, phagocytosis of cells Multisystem effects: Kidney (renal failure) Skin (“butterfly rash”) CNS (focal neurologic deficits) Joints (arthritis) Heart (pericarditis, endocarditis) 47 Systemic Lupus Erythematosus (SLE) prognosis Variable! Some have few symptoms, rare patients die within months. Most patients: relapses/remissions over many years. Acute flare-ups controlled with steroids 80% 10-year survival Most common cause of death: renal failure 48 Systemic Lupus Erythematosus (SLE) Lupus nephritis. There are two focal necrotizing lesions at 11 and 49 2 o’clock. (H&E stain.) (Dr. Helmut Rennke) Slide 7.24 Systemic Lupus Erythematosus (SLE) Lupus nephritis, diffuse proliferative type. Note the marked increase in 50 throughout the glomerulus. (H&E stain.) (Dr. Helmut Rennke) Slide cellularity 7.25 Immunofluorescence micrograph stained with fluorescent anti-IgG from a patient with diffuse proliferative lupus nephritis. One complete glomerulus and part of another one are seen. Note the 51 mesangial and capillary wall deposits of IgG. Slide 7.26 Lupus nephritis showing a glomerulus with several “wire loop” lesions representing extensive subendothelial deposits of immune complexes. (Periodic acid-Schiff [PAS] stain.) 52 Slide 7.28 Systemic lupus erythematosus involving the skin. A, An H&Estained section shows liquefactive degeneration of the basal layer of the epidermis and edema at the dermoepidermal junction. B, An immunofluorescence micrograph stained for IgG reveals deposits of immunoglobulin along the dermoepidermal junction. Slide 7.29 53 Rheumatoid Arthritis Symmetric, mostly small-joint arthritis Systemic symptoms (skin, heart, vessels, lungs) Rheumatoid factor Cytokines (especially TNF) cause damage 54 Rheumatoid Arthritis Etiology Circulating IgM antibody Directed against patient’s OWN IgG! Forms IgM-IgG immune complexes, which deposit in joints and cause badness Present in 80% of patients 55 Rheumatoid Arthritis Etiology T cells release cytokines: activate macrophages (causing destruction) cause B cells to make antibodies against joint Most important of these cytokines: TNF Cytokines cause inflammation and tissue damage 56 Rheumatoid Arthritis Joint disease Mainly small joints (hands), but also knees, elbows, shoulders Symmetric; characteristic hand features Chronic synovitis with pannus formation: synovial cell proliferation inflammation granulation tissue 57 Rheumatoid Arthritis Systemic disease Weakness, malaise, fever Vasculitis Pleuritis, pericarditis Lung fibrosis Eye changes Rheumatoid nodules on forearms 58 Rheumatoid Arthritis prognosis Variable! A few patients stabilize Most patients have chronic course with progressive joint destruction and disability Lifespan shortened by 10-15 years 59