* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download slides#5 - DENTISTRY 2012
Survey
Document related concepts
Complement system wikipedia , lookup
DNA vaccination wikipedia , lookup
Lymphopoiesis wikipedia , lookup
Monoclonal antibody wikipedia , lookup
Immune system wikipedia , lookup
Molecular mimicry wikipedia , lookup
Hygiene hypothesis wikipedia , lookup
Adoptive cell transfer wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
Immunosuppressive drug wikipedia , lookup
Adaptive immune system wikipedia , lookup
Sjögren syndrome wikipedia , lookup
Polyclonal B cell response wikipedia , lookup
Transcript
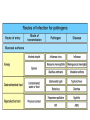
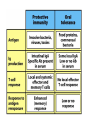
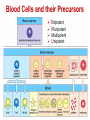
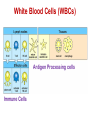
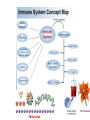
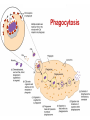
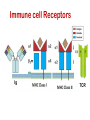
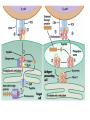
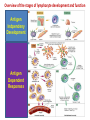
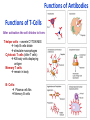
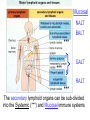
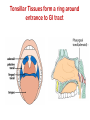
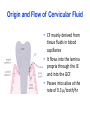
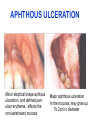
ORAL Immunology Faculty of Medicine/University Of Jordan April 9th 2015 Mohammed El-Khateeb Outline • The Origin of Immune Concept • Overview of Immunity to Microbes • Features & Components of Innate & Adaptive Immunity • Hallmarks of the Immune Response Self/Non-self Discrimination Memory Specificity Blood Cells and their Precursors Figure 1-3 part 1 of 4 Totipotent Pluripotent Multipotent Unipotent White Blood Cells (WBCs) Figure 1-3 part 4 of 4 Antigen Processing cells Immune Cells Molecules IMMUNE SYSTEM COMPNENTS Aaptive IS Innate IS • Organs: • Organs, – RES • Cell: Monocytes /Macrophages, PNL, Eosinophiles, Basophils, NK • Molecules: Acute phase proteins, interferone, interleukins , kimokines – Primary organs (Bone Marrow + Thymus) – Secondery organs ( LN, Spleen, MLAT) • Cells : B cells, T cells • Molecules: Igs, Lymphokine Cytokine The immune system Innate (non-specific) immunity Adaptive (specific) immunity Anatomic barriers (Skin,mucous membranes) Antigen specificity Physological barriers (temperature, pH) Immunological memory Phagocytic Barriers (cells that eat invaders) Inflammatory barriers (redness, swelling, heat and pain) Diversity Self/nonself recognition Innate and Adaptive Immunity INNATE IMMUNITY ACQUIRED • A summary of innate and acquired Rapid responses to a IMMUNITY Slower responses to immunity broad range of microbes specific microbes External defenses Invading microbes (pathogens) Internal defenses Skin Phagocytic cells Mucous membranes Antimicrobial proteins Secretions Inflammatory response Natural killer cells Humoral response (antibodies) Cell-mediated response (cytotoxic lymphocytes) Figure 2-2 part 2 of 2 Three-phase Response to2Initial Figure 2-1 part of 2 Infection 0 – 4 hours 4 - 96 hours Late > 96 hours RESPONSES • Activation of Complement • Activation of Acute Phase Proteins • Activate Phagocytosis C’ 13 Human Acute Phase Protein • Antiproteases α1-Protease inhibitor α1-Antichymotrypsin (ACT) Pancreatic secretory trypsin inhibitor Inter- α-trypsin inhibitor • Tranport proteins Ceroloplasmin Haptoglobin Hemopexin • Inflammatory response Phopholipase A2 Lipopolysaccharide-binding protein Interleukin-1-receptor antogonist Granulocyte colonystimulating factor • Others C-reactive protein Serum amyloid A Phagocytosis Phagocytosis 15 Immune cell Receptors Ig TCR Overview of the stages of lymphocyte development and function Antigen Indpendeny Development Antigen Dependent Responses 18 Functions of Antibodies Functions of T-Cells After activation the cell divides to form: T-helper cells – secrete CYTOKINES help B cells divide stimulate macrophages Cytotoxic T cells (killer T cells) Kill body cells displaying antigen Memory T cells remain in body B- Cells: Plasma cell Abs Memory B cells 19 Dynamics of Adaptive Immunity This chapter tries to integrate much of what we have already covered so we can better understand how the immune system protects from infection. • How infectious agents cause disease • The course of an adaptive immune response • Immunological memory Mucosal Immune System Introduction • Mucosal Defence • Mucosal Immune system Antigen - induced expansion of lymphoid tissue Lymphocyte homing Functional and phenotypic diversity Regulatory T cells Immunoglobulin IgA Immunity thru’ Vaccination COMPONENTS OF THE MUCOSAASSOCIATED LYMPHOID TISSUE • • • • • • • Gastrointestinal tract (GALT) Bronchial Tree (BALT) Nasopharyngeal area (NALT) Mammary gland Salivary and lacrimal glands Genitourinary organs Inner ear Mucosal NALT BALT *** # GALT *** # RALT *** The secondary lymphoid organs can be sub-divided into the Systemic (***) and Mucosal immune systems Tonsillar Tissues form a ring around entrance to GI tract Mucosal Immune System • Immune response – Induction & Expression within same system • Mucosal Lymphocytes – Remain within the mucosal immune system – Lymphocyte migration / homing / retention • Special T cells – CD8 α/β, γ/λ , and regulatory T cells – Th17 cells Produce IL-17 Examples of mucosal diseases- role for Th17 cells Gut: IBD – autoimmune diseases of the gut Vaginal mucosa:Th17 cells are protective against Neisseria gonnorrheae Lung: Th17 cells are protective against various pneumoniaes, TB, etc., promote airway hyperreactivity/allergy Mouth: Th17 cells promote Sjogren’s (autoimmune disease of salivary gland, tear ducts), but protective in oropharyngeal candidiasis (“thrush”) Mouth Contains organisms that survive mechanical removal by adhering to gums and teeth Excellent growth environment with water, nutrients, temperature, etc. Both aerobes and anaerobes present (biofilms) Streptococci, especially S. mutans attach to enamel by glycocalyx Contribute to formation of dental plaque, dental caries, gingivitis, and periodontal disease Mucosa • The intact oral mucosa is a barrier against infecting organisms. • Superficial squamous cells may be colonized with bacteria in the same way as squamous cells on the skin, • Intact bacteria can cross a damaged epithelial barrier. • The undamaged oral mucosa is permeable to a range of substances smaller than bacteria Oral mucosal secretions • • • • • • • • • Mucin Lysozyme Lactoferrin Salivary peroxidase Histatins PRPs Statherin Cystatins Epithelial cell derived antimicrobial peptides Saliva • Saliva is a dynamic barrier in the mouth, • • constantly flowing backwards to the oesophagus. Micro-organisms become entrapped and are carried via the oesophagus to the hydrochloric acid and pepsin of the stomach. Saliva also acts as an additional barrier to the penetration of materials into the oral mucosa. Saliva • Saliva contains a number of materials which afford non-specific protection to the individual. Lysozyme, a mucolytic enzyme: is capable of splitting sugars off the glycopeptides of the cell wall of many Grampositive bacteria, leading to their lysis. Lactoferrin, which reduces the amount of free iron available for bacterial metabolism, Unidentified basic polypeptides, which exert antimicrobial activity, Lactoperoxidase which can cross-link proteins and hence damage certain bacteria and viruses. Mucins : have some carbohydrate side chains in common with epithelial cells and competitively inhibit the binding of viruses to the epithelial cells Salivary constituents and their functions defensins defensins Mucins defensins Gingival Crevice • Since the gingival crevice may harbor micro-organisms and their products, the ability of the junctional epithelium to withstand penetration may be of considerable importance. • The junctional epithelium is apparently more permeable than other non-keratinized oral mucosa. • The flow of fluid is increased with gingival inflammation. • The major immunoglobulin classes are represented in gingival crevice fluid. Cellular Components The cells involved in the immune response in the mouth are widely distributed in the following sites, Submucosal tissue Gingiva, Salivary glands, Epithelium, Gingival crevice fluid, Tonsils, Extra oral lymph nodes, which drain lymph from the oral cavity Oral Tolerance • Oral tolerance is – A general immunosuppressive state in the oral mucosa to prevent reaction to harmless Ags such as commensals or foods – the generation of systemic immune unresponsiveness by feeding of antigen • Necessary to prevent excessive response to normal flora and food antigens Limitations to Oral Tolerance • Can be overcome with mucosal adjuvant (e.g. Cholera toxin) • Alter physical characteristics of antigen: antigen in micro-spheres that target PP • Feeding of attenuated enteric pathogen expressing the antigen (Salmonella) Oral Antigen Induces IgA • Ingestion of killed Streptococcus mutans • IgA antibody producing cells – Peripheral blood by day 7, peak day 10 – 12 • Secretory IgA antibodies – Saliva & Tears by 2 weeks, peak 3 weeks Natural development of sIgA At birth: no sIgA in saliva Predentate infants (16-28 wks): Detected against “1st wave” of strep. organisms: S. mitis, S. salivarius (Smith and Taubman, 1992) These organisms initially colonize mucosal surfaces No Abs to S. mutans detected Dentate children: Tooth eruption brings “2nd wave” of strep. organisms: S. sanguis, S. mutans Antibodies (Abs) against S. mutans observed in 1 yr old children Abs against: serotype specific carbohydrate, protein I/II, glucosyltransferase, glucans, teichoic acids w/i 10 yrs the child has IgA levels comparable to an adult (adult parotid saliva contains 30-160 g/ml IgA) sIgA Major salivary glands produce 70% of total salivary sIgA 30% comes from minor salivary glands sIgA system is what we attempt to manipulate to prevent dental caries and certain microbial infections 3 X as much IgA is produced/day than IgG ~2/3 of IgA produced is sIgA Primary function to prevent microbial adherence (serum) Bacterial IgA-specific proteases found in S. sanguis; periodontal pathogens. Secretory IgA - Production • IgA in blood is monomeric, >90% IgA1 • Secretory IgA ♦ polymeric, IgA1 upper respiratory & GI tract IgA2 in ♦ ♦ ♦ ♦ colon & rectum Induction by antigen in Peyer’s patches Production by IgA plasma cells in lamina propria J chain polymerisation of IgA Binds polymeric Ig-receptor for trans-epithelial transport, cleaved to release secretory IgA Secretory IgA - Function • Specificity ♦ 2 – 5% reacts with specific Ag after immunisation ♦ Commensal flora? Dietary antigens? • Resists proteolysis • Inhibits microbial adherence • Neutralisation of viruses, toxins (cholera) • Activates complement (alternative pathway) • Antigen exclusion • Modulation of enzyme activity Possible Causes of Immunologically Mediated Mucosal Damage • • • • • • • • Antigens: Local microbial flora or food Accumulation of cirvulating antigen B cell mitogens: Microorganisms and food Mitogenic complement split products Blastogenic factors from locally activated T and B cells Lymphostimulatory factors from macrophages and neutophils Altered autologous IgG-Immune complexes Endogenous tissue antigens cross-reacting with microbial componenets IgA Multiple Properties Adopted to GI Tract • Relatively resistant to proteolytic effect (IgA2>IgA1) • Poor activator of complement • Inhibits: – Bacterial adhesion – Macromolecule absorption – Inflammatory affects of other immunoglobulins • Neutralizes Viruses and Toxins • Enhances nonspecific defense mechanisms – Lectofernin – Lactoperoxidase • Mediate antibody dependent cytotoxicity (ADCC) Origin and Flow of Cervicular Fluid • CF mainly derived from tissue fluids in blood capillaries • It flows into the lamina propria through the JE and into the GCF • Passes into saliva at the rate of 0.3 /tooth/hr SPECIFIC ORAL DISEASES • Dental Carries • Peridontal Disease • Aphthous Ulceration • Oral menifestations of Systemic Immunological Diseases Mutans streptococci Group of strep species most closely associated with caries of smooth surfaces, pits, fissures 6 serotypes of ms that are associated with man S. mutans serotype C, predominant group associated with enamel surfaces; 80-87% of cases in U.S. Swedish kids; smooth surface caries, 36% presence of serotype c, 54% serotype d/g Specific immunity against DCs Caries correlated with sIgA titers and serum IgM to S. mutans. Elevation in titer is due to exposure Are these antibodies protective?? Association between sIgA antibodies and resistance to dental infection by S. mutans has still to be convincingly demonstrated. Serum Abs to Strp. mutans in Man DMF: Index of decayed, missing or filled tooth Active: High DMF group with one or more carious lesion Reduction of Caries in Monkey Model • Immunization against dental caries in Monkey • Subcutaneous immunization with S. mutans MO or purified Ag. • Both gave the same reduction in dental caries GENETIC FACTORS • Respond to low dose of S. mutans Ag (SA I/II) 1-10ng, positive for HLA-DRw6 • Needs 1000ng/ml negative for HLA-DRw6 • High Ab level to S mutans Subjects Low carries subjects SA I/II Ag HLA Ab Level Caries prone low Dose 1-10ng High Dose 1000ng DRw6 Positive DRw6 Negative High Low Stages of Periodontal Disease Some Types of Oral Ulcerations May Mimics RAS Recurrent aphthous stomatitis ♦ Behcet’s Syndrome ♦ Clinical Neuropenia ♦ Coeliac disease ♦ Iron deficiency ♦ Folate deficiency ♦ Ulcerative colitis Do not Usually Mimics RAS ♦ ♦ ♦ ♦ ♦ ♦ ♦ ♦ Pemphigus Mucus membrane pemphigoid Erythema multiforme Erosive lichen planus Chron’s disease Wagner’s granuloma Carcinoma Leukemia APHTHOUS ULCERATION Minor eleptical shape aphtous ulceration, and defined periulcer erythema, effects the non-keratinized mucosa Major aphthous ulceration In the mucosa, may grow up To 2cm in diameter Oral Manifestations of Systemic Immunological Diseases GI DISEASE Coeliac Disease Crohn’s Disease Ulcerative Colitis Food Allergy and Oral Disease Oral Manifestations of Systemic Immunological Diseases DERMATOLOGICAL DISEASES Lichen Planus Pemphigus Benign Mucous Membrane Pemphigoid (BMMP) Erythema Multiforme Oral Manifestations of Systemic Immunological Diseases CONNECTIVE TISSUE DISEASES Sjogren’s Syndrome Wagners’s Granulomatosis Malignant Midline Granuloma (Stewart’s Granuloma) Conclusion • Mucosal Immune system ◙ Antigen - induced expansion of lymphoid tissue ◙ Lymphocyte homing ◙ Functional and phenotypic diversity ◙ Regulatory T cells ◙ Immunoglobulin IgA