* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Immune responses in viral infections
Survey
Document related concepts
Lymphopoiesis wikipedia , lookup
Sociality and disease transmission wikipedia , lookup
Hospital-acquired infection wikipedia , lookup
Herd immunity wikipedia , lookup
Monoclonal antibody wikipedia , lookup
Complement system wikipedia , lookup
DNA vaccination wikipedia , lookup
Social immunity wikipedia , lookup
Adoptive cell transfer wikipedia , lookup
Molecular mimicry wikipedia , lookup
Hygiene hypothesis wikipedia , lookup
Immune system wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
Polyclonal B cell response wikipedia , lookup
Adaptive immune system wikipedia , lookup
Immunosuppressive drug wikipedia , lookup
Transcript
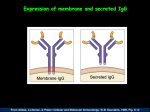
L.7 / 2016-2017 Microbiology/Immunology Asst.Prof.Dr. Ifad Kerim Al-Shibly Microbial immunity The immune system has developed to protect the host from pathogens and other foreign substances, self/non-self discrimination is one of the hallmarks of the immune system. Most pathogens can elicit both an antibody (humoral) and a cell-mediated response, both of which may contribute to ridding the host of the pathogen. However, for any particular pathogen one type of immune response whether antibody or a cellmediated immune response may be more important than the other type for the host to defend against the pathogen. Defense against infections is mediated by the early reactions of innate immunity and the later responses of adaptive immunity. The immune system is specialized to generate different effector mechanisms for different types of microbes. The survival and pathogenicity of pathogens in a host and so the outcome of infections is determined by the balance between host defenses and the ability of microbes to evade or resist immunity. Immune responses to microbes are themselves capable of causing tissue injury (Immunopathology). Antigenic mimicry is where a protein sequence of a foreign antigen is similar to a self-protein which results in unintentional cross reactivity of antibodies or T cell epitopes. This pathology can occur long after infectious agent has been eliminated (e.g. rheumatic fever after strept. infection). Immune responses in viral infections Viruses are obligatory intercellular pathogens that replicate within cells. They use the nucleic acid and protein synthetic machineries of the host cell. It can infect a variety of cell populations by utilizing normal cell surface molecules as receptors to enter cell. Infected cells use their major histocompatibility complex molecules to put pieces of the invading microbes on their surfaces, flagging down cytotoxic T lymphocytes to destroy the infected cells. ☺The primary defense against viruses is cell-mediated responses CMI, the cytotoxic T lymphocyte. Antibodies also can assist in the immune response by opsonizing and blocking viruses before they have a chance to enter cells. Innate immunity: 1. The principal mechanisms of innate immunity against viruses are inhibition of infection by interferons (INF). Interferons are antiviral proteins, or glycoproteins produced by several types of cells in response to viral infection: INFα by leucocytes, INFβ by fibroblast, and INFγ by natural killers (NK) cells. IFNs function to inhibit viral replication in both infected and uninfected cells. 2. NK cell –mediated killing of infected cells. NK cells are the host adaptation for killing class I MHC-negative virus infected cells. 1 L.7 / 2016-2017 Microbiology/Immunology Asst.Prof.Dr. Ifad Kerim Al-Shibly Adaptive immunity: 1. Because antibodies do not get into host cells, they are ineffective against intracellular pathogens. Antibodies opsonize and neutralize viruses and prevent infection. Block infectious virus early in course of infection (before entering cells) or after release from infected cells (prevents cell-to-cell spread). 2. CTLs recognize antigens from the virus that are displayed on the surface of the infected cell in association with MHC-I and kill the cell thereby preventing the spread of the infection to neighboring cells. In some latent viral infections (EBV, CMV), CTLs control but do not eradicate the infection; defective T cell immunity leads to reactivation of the virus (in HIV, immunosuppression caused by leukemia, treatment for graft rejection). Mechanisms of Immune Evasion by Viruses : 1. Antigenic variation (Influenza, HIV, rhinovirus). Viruses can alter their antigens, influenza viruses show changes in antigenicity(antigenic shifts and drifts). Because of antigenic variation, a virus may become resistant to immunity generated in the population by previous infection. 2. Inhibition of the class I MHC antigen processing pathway (e.g. CMV). 3. Different viruses use different mechanisms. 4. Production of immune modulators. Some viruses produce molecules that inhibit innate and adaptive immunity. EBV produces a protein that is homologous to IL-10 and may function to inhibit CMI. Soluble cytokine receptors may act as “decoys” and block actions of cytokines (poxviruses). 5. Infection of immune cells (HIV infect CD4 T cells). Immune responses in bacterial infections Intracellular Bacteria: Intercellular bacteria have the ability to survive and even replicate within phagocytes where they are inaccessible to circulating antibodies, for example, Mycobacterium tuberculosis, the causative agent of tuberculosis. Elimination of intracellular bacteria requires immune responses that are very different from the responses against extracellular bacteria. By living inside a host cell they avoid many effective host immune strategies (antibodies, phagocytosis, and complement). However these bacteria need to have strategies to escape lysosomes. Some intracellular bacteria choose to escape from the endosome and replicate in cytoplasm like viruses. Others stay in protected endosome and alter it in order to prevent fusion with lysosome. 2 L.7 / 2016-2017 Microbiology/Immunology Asst.Prof.Dr. Ifad Kerim Al-Shibly Innate immunity: The major defensive and protective immunological response against intracellular bacteria is CMI. During the innate immune response to intracellular bacteria phagocytes ingest and attempt to destroy it. Phagocytosis occurs initially by ٭neutrophils and later by ٭macrophages, intracellular bacteria are resistant to degradation within phagocytes. ٭NK cells function by two means direct killing of infected cells and by activating of macrophages through the production of IFN-γ. Adaptive immunity: 1. Cell-mediated immune response (CMI): is the major specific immune response against intracellular bacteria. Helper and cytotoxic T cells cooperate in cell-mediated immunity against intracellular microbes. There are two types of cell-mediated reactions: killing of phagocytosed intracellular bacteria as a result of macrophage activation by ٭Th1 cell – derived cytokines, and lysis of infected cells by ٭CTLs. Th1 cells, is the primary defense against intracellular bacteria that live within vesicles (phagosomes). Th1 cells recognize antigen from the bacteria that are expressed on the surface of infected antigen presenting cells in association with MHC-II and release cytokines that activate these cell. Th1 cytokines IFN-γ, TNF-α activate macrophages. Once activated, they can then kill the pathogen. Activated macrophages kill phagocytosed microbes by producing microbicidal reactive oxygen intermediates, nitric oxide and lysosomal enzymes. The same activated helper T cells, if present in the vicinity of cytotoxic T cells, provide cytokine signals (IL-2) that stimulate cytotoxic T cells to proliferate. Activation of cytotoxic T cells leads to their proliferation and differentiation into effector cytotoxic T cells capable of cytolytic functions. The most specific feature of cytotoxic cell differentiation is the development of membrane bound cytoplasmic granules that contain proteins, including perforins and granzymes. CTLs also express a membrane protein called Fas ligand (FasL), which binds to its target protein Fas that is expressed in many cell types. The production of perforines and granzymes, and the interaction of Fas-FasL results in apoptosis and death of the target cell. 2. Antibodies (AMI) /Th2 cytokines help with protection from reinfection but may be less effective for elimination. Mechanisms of Immune Evasion by Intracellular Bacteria: Intracellular bacteria’s ability to resist elimination by phagocytes is an important mechanism for survival and evasion of the immune response. Some intracellular bacteria do this by inhibiting phagolysosome fusion, while others produce hemolysin that blocks bacterial killing in macrophages. 3 L.7 / 2016-2017 Microbiology/Immunology Asst.Prof.Dr. Ifad Kerim Al-Shibly Extracellular Bacteria : Extracellular bacteria are capable of replicating outside of the host cells. They are fast replicating to avoid elimination. They cause disease by two principle mechanisms: 1.They induce inflammation. 2. Many of these bacteria produce toxins (endotoxins and exotoxins). The immune responses against extracellular bacteria are aimed at eliminating the bacteria and at neutralizing the effects of their toxins. Innate immunity: 1. Phagocytosis by macrophages and neutrophils. 2. Complement activation and inflammation. Complement activation leads to phagocytosis and lysis. Gram positive bacteria contain peptidoglycan that activate alternative complement cascade, complement components induce inflammation. Adaptive immunity: 1. Humoral immunity (AMI) is the principle specific immune response against extracellular bacteria. Strong IgM responses are caused by polysaccharides. Antibodies IgM and IgG against bacteria surface antigens and toxins stimulate three types of effector mechanisms: opsonization, toxin neutralization, and complement fixation. 2. Cellular immunity: Th2 cytokines important for B cell activation. Th1 CKs have some role for activating macrophages. Mechanisms of Immune Evasion by Extracellular Bacteria: 1. IgA specific proteases (e.g. niesseria). 2. Antigenic variation: genetic variation of the surface antigen to evade specific immunity (e.g. pilli variation in salmonella). 3. Polysaccharide capsule gives resistance to phagocytosis. 4. Molecular mimicry: Pertussis toxin mimic selectins and can block selectin activity and leukocyte recruitment to site of infection. 5. The capsule contain one or more sialic acid residues that inhibit complement activation by the alternative pathway. Immune responses in fungal infections Fungi are eukaryotes that tend to cause serious infections primarily in individuals with impaired immunity. Innate Immunity: The principal mediator of innate immunity against fungi is the ٭neutrophils and ٭macrophages. They liberate fungicidal substances, by the production of toxic molecules through oxygen-dependent mechanisms - nitric oxide, reactive oxygen 4 L.7 / 2016-2017 Microbiology/Immunology Asst.Prof.Dr. Ifad Kerim Al-Shibly intermediates (ROIs), and reactive nitrogen intermediates (RNIs) forming the respiratory burst. Fungi have developed evasion mechanisms to inhibit the respiratory burst through the production of specific scavengers of oxidative killing by phagocytes- catalase, mannitol and melanin. The oxygen-independent mechanisms consist of degranulation and release of neutrophil cationic peptides, lysozyme, antimicrobial peptides- defensins, arachidonic acid and iron sequestration. The phagocytes also secrete cytokines and chemokines which are involved in the protective immune response in order to phagocytose fungi for intracellular killing. Adaptive immunity: Cell-mediated specific immunity is the major defense against fungal infections. Fungi that are present intercellularly in macrophages are eliminated by the same cellular mechanisms that are effective against intracellular bacteria (see above). CMI activated by Th1 cells are the major mechanisms of adaptive immunity against fungal infection. Generally Th1 response is protective to the host during fungal infection, while Th2 response is detrimental. Immune responses in parasitic infections In infectious disease terminology, “parasitic infection” refers to infection with animal parasites, such as protozoa, helminthes, and ectoparasites. Humans are only part of the complex life cycle of parasites. Innate Immunity: Protozoa and helminthic parasites that enter the blood stream or tissue are often able to survive and replicate because they are resistant to host innate immune responses. Parasites in humane host are usually resistant to complement. Macrophages can phagocytose protozoa, but the tegument of helminthic parasites makes them resistant to the cytocidal effects of both neutrophils and macrophages. Adaptive immunity: Different parasites elicit quite distinct specific immune responses. CMI is the principal defense against protozoa that survive within macrophages. Protozoa that replicate inside cells and lyse host cells stimulate specific ٭CTL responses, similar to cytopathic viruses. ٭Th2 cells also play a vital role in immunity to helminthic infections since they induce inflammatory reactions that are dominated by eosinophils and mast cells. Th2 cells, secrete IL-4 and IL-5. IL-4 stimulates the production of helminthic-specific IgE antibodies, which opsonize the helminthes. IL5 activates eosinophils, which bind to IgE coated on helminthes (type of ADCC). Eosinophil granules contain major basic protein and eosinophil cationic protein; these 5 L.7 / 2016-2017 Microbiology/Immunology Asst.Prof.Dr. Ifad Kerim Al-Shibly proteins are toxic to several parasites. Degranulation of these contents by ADCC leads to death of the helminth. Mechanisms of Immune Evasion by Parasites: 1. Some parasites survive and replicate inside cells. 2. Antigen masking is an effective form of immune response evasion by parasites. Some parasites develop cysts shedding their antigenic coats e.g. Entameoba histolytica that are resistant to immune responses. 3. Parasites can develop a tegument that is resistant to damage by antibodies and complement or CTLs. Parasites become resistant to immune system during their residence in the host, schistosoma larva travel to the lungs of infected host and develop a thick tegument to resist the action of CTLs and complement system. 4. Antigenic variation: parasites change their surface Ag during their life cycle in the infected host: e.g. Plasmodium. 5. Inhibition of host immune response by induction of T cells anergy (in ability to response), e.g. filarial infection. Thank you 6