* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Pituitary Agents. Thyroid and Antithyroid Agents. Antidiabe
Survey
Document related concepts
Metabolic syndrome wikipedia , lookup
Hypothalamus wikipedia , lookup
Hypothyroidism wikipedia , lookup
Growth hormone therapy wikipedia , lookup
Hypoglycemia wikipedia , lookup
Hyperandrogenism wikipedia , lookup
Hyperthyroidism wikipedia , lookup
Graves' disease wikipedia , lookup
Insulin resistance wikipedia , lookup
Gestational diabetes wikipedia , lookup
Diabetes management wikipedia , lookup
Complications of diabetes mellitus wikipedia , lookup
Diabetic ketoacidosis wikipedia , lookup
Transcript
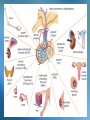
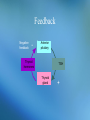
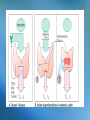
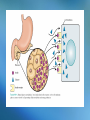
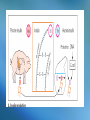
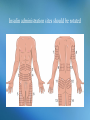
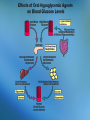
The Endocrine System • Consists of glands and other structures that produce hormones which are released into the circulatory system The Endocrine System • Consists of glands and other structures that produce hormones which are released into the circulatory system • Regulation is established through hormones affecting target tissue Regulation • Homeostatsis is achieved through feedback mechanisms • Negative feedback – negates change to bring levels back to normal Pituitary Gland • Regulates other endocrine glands as well as other body activities Different hormones, different signals Negative feedback - Anterior pituitary Thyroid hormones TSH Thyroid gland Negative feedback - Negative feedback + ADH Water absorption Negative feedback Insulin Liver, fat & muscle osmolality + Pancreas Glucose - Hypothalamus - + Parathyroids calcium PTH Bone, GIT & Kidney + Growth Hormone • Non-endocrine related disorders can also cause growth delay: – Intrauterine growth retardation, chromosomal defects, abnormal growth of cartilage or bone, poor nutrition, variety of systemic diseases Growth Hormone • Deficiency of endogenous growth hormone causes growth retardation • Growth delay may be caused by – Family growth patterns, genetic disorders, malnutrition, systemic or chronic illness, psychosocial stress, or a combination of these – Endocrine deficiency, or problems with thyroxine, cortisol, insulin, or GH Growth Hormone • Release of GH is stimulated by the release of GHRF secreted by the hypothalamus • GH is inhibited by – – – – – – Glucocorticoids Obesity Depression Progesterone Hypokalemia Altered thyroid function Drug List Synthetic Human Growth Hormones • somatrem (Protropin) • somatropin (Humatrope) Growth Hormone • The younger the patient at time of treatment the greater the height that may be achieved • Little response is seen after age 15-16 in boys and 14-15 in girls Thyroid Gland • Produces hormones (T3 and T4) that stimulate metabolic activity of body tissues • Hypothalamus and pituitary glands work together to release TSH • TSH stimulates T3 and T4 release Thyroid Hormone Feedback Loop • Thyroid hormones build up in the blood • Signals are sent to the hypothalamicpituitary axis that adequate levels have been met • TSH levels decrease Feedback Negative feedback - Anterior pituitary Thyroid hormones TSH Thyroid gland + Hypothyroidism • Production of thyroid hormones is below normal • Cretinism occurs in children at birth due to inadequate maternal iodine intake – Can cause mental retardation, thick tongue, lethargy, lack of response, short stature – can be corrected if treated Primary and secondary disorders Primary Thyroid disease Secondary Thyroid disease Hypothyroidism Symptoms • • • • • Apathy Constipation Decreased heart rate Depression Dry skin, nails, and scalp • Easy fatiguing • Enlarged thyroid • • • • • • Lowered voice pitch Myxedema Puffy face Reduced mental acuity Swelling of eyelids Tongue enlarged and thickened • Weight gain Causes of Hypothyroidism • Autoimmune destruction of the gland • Radioactive iodine therapy • Surgical removal of the gland Treatment for Hypothyroidism • Thyroid replacement therapy – Should not be used to treat obesity Drug List Agents for Hypothyroidism • levothyroxine, T4 (Levothroid, Levoxyl, Synthroid) • liothyronine, T3 (Cytomel) • liotrix (Thyrolar) • thyroid (Armour Thyroid) levothyroxine, T4 (Levothroid, Levoxyl, Synthroid) • Used for chronic therapy • Can be cardiotoxic • Alters protein binding of other drugs • Should not switch brands once stabilized levothyroxine Dispensing Issues Warning! • Can be cardiotoxic; report any of the following: – Chest pain, increased pulse, palpitations, heat intolerance, excessive sweating levothyroxine Dispensing Issues Warning! • Look-alike and Sound-alike Drugs: – levothyroxine (thyroid replacement) – levofloxacin (antibiotic) Hyperthyroidism • Excessive thyroid hormone • Most common cause is Grave’s disease • Other causes: – Excessive exogenous iodine – Thyroid nodules – Tumor in the pituitary causing overproduction of TSH Symptoms of Hypterthyroidism • • • • • • • • • Decreased menses Diarrhea Exophthalmos Flushing of the skin Heat intolerance Nervousness Perspiration Tachycardia Weight loss Drug List Agents for Hyperthyroidism • methimazole (Tapazole) • propylthiouracil, PTU • radioactive iodine, 131I Discussion What are the treatment options for hyperthyroidism? Discussion What are the treatment options for hyperthyroidism? Answer: in children: surgery and hormone replacement; adults: surgery or medications Diabetes/Hypoglycemic Agents • In the islets of Langerhans, in the pancreas, there are two primary specialized cells • Alpha Cells • Beta Cells Hypoglycemic Agents • In the islets of Langerhans, in the pancreas, there are two primary specialized cells • Alpha Cells – Produce glucagon and raise blood glucose levels • Beta Cells Hypoglycemic Agents • In the islets of Langerhans, in the pancreas, there are two primary specialized cells • Alpha Cells – Produce glucagon and raise blood glucose levels • Beta Cells – Produce insulin and lower blood glucose levels Insulin • Helps cells burn glucose for energy • Works with receptors for glucose uptake • Enhances transport and incorporation of amino acids into protein • Increases ion transport into tissues • Inhibits fat breakdown Diabetes • Caused by inadequate secretion or utilization of insulin • Leads to excessive blood glucose levels • Normal: 100 mg/dL Type I Diabetes • Occurs most commonly in children and young adults • Average age of diagnosis is 11 or 12 • Patients are insulin dependent and have no ability to produce insulin on their own • May be due to an autoimmune response • Type I accounts for 5-10% of diabetic population Type II Diabetes • Affect 80-90% of diabetics • Most patients are over 40 and more women than men are affected • Could be caused by insulin deficiency or insulin receptor resistance • Many of these patients are overweight and can treat their diabetes with weight loss Gestational Diabetes • • • • Occurs during pregnancy Increases risk of fetal morbidity and death Onset is during the 2nd and 3rd trimesters Can be treated with diet, exercise, and insulin • 30-40% of women with gestational diabetes will develop type II in 5-10 years Secondary Diabetes • Caused by medications – – – – – – Oral contraceptives Beta blockers Diuretics Calcium channel blockers Glucocorticoids phenytoin • May return to normal when drug is stopped Symptoms of Diabetes • • • • • • • • • • Frequent infections Glycosuria Hunger Increased urination and nocturia Numbness and tingling Slow wound healing Thirst Visual changes Vomiting Weight loss, easy fatigability, irritability, ketoacidosis Complications of Diabetes • Retinopathy leading to blindness • Neuropathy • Vascular problems can lead to inadequate healing which could lead to amputation • Dermatologic involvement • Nephropathy is the primary cause of endstage renal disease Lack of Insulin Activity • Diabetics cannot use glucose therefore their bodies metabolize fat • Gluconeogenesis is the formation of glucose from protein and fatty acids • Fatty acid is oxidized into ketones Ketones • Strong acids • Cause the body pH to drop • Excreted in the urine or eliminated through respiration • Causes a fruity acetone smell on the breath that can be mistaken for alcohol Treating Diabetes • Treatment consists of diet, exercise, and medications • Blood glucose monitoring must be done regularly throughout the day • Type II diabetics may be able to control the disease through diet and exercise alone Treatment for Type II 1. 2. 3. 4. 5. Lifestyle changes Oral monotherapy Combination oral therapy Oral drug plus insulin Insulin only General Treatment Guidelines • Attention to diet • Blood pressure control • Compliance with medications • Control of hyperlipidemia • Daily foot inspections • Increased physical activity • Recognizing hypoglycemia • Blood glucose testing • Monitoring in the Dr’s office • Patient education • Prompt treatment of infections • Setting goals Drug List Drug for Lower Extremity Diabetic Ulcers • becaplermin gel (Regranex) Insulin • Administered subcutaneously due to degradation in the GI tract • Different types of insulin have different onset of action times and duration of action times Insulin Duration of Action Type Duration of Action Humalog, Novolog Regular 1 hr (works in 15 mins and gone in about an hour) 5-6 hours (onset – 30 mins) NPH 10-16 hours Lente 12-18 hours Lantus 24 hours mixed Quick onset, longer duration Insulin Dispensing Issues Warning! • It is very easy to grab the wrong insulin in the refrigerator • Always double-check yourself • They look exactly alike Insulin administration sites should be rotated Hypoglycemia • Blood glucose levels of <70 mg/dL • Can be caused by – – – – Skipping meals Too much exercise Poor medication regimen Certain drugs Signs & Symptoms of Hypoglycemia • • • • • Confusion Double vision Headache Hunger Numbness and tingling in mouth and lips • • • • • • Nervousness Palpitations Sweating Thirst Visual disturbances Weakness Drug List Human Insulins • • • • • NPH isophane insulin (Humulin N) insulin aspart (NovoLog) insulin glargine (Lantus) insulin lispro (Humalog) regular insulin (Humulin R) insulin lispro (Humalog) • Rapid-onset insulin • Can be injected immediately before or after meals • May be used with a pump insulin aspart (NovoLog) • Rapid-acting insulin analog • Each dose should be administered before meals • May be used with a pump insulin glargine (Lantus) • Synthetic long-acting insulin • Absorbed slowly and works over a 24-hour time period • Works similarly to physiologic insulin release Drug List Human Insulins Mixtures • insulin aspart w/ protamine-insulin aspart (NovoLog Mix 70/30) • insulin lispro w/ protamine-insulin lispro (Humalog Mix 75/25) • insulin with zinc (lente) (Humulin L) • NPH-regular insulin (Humulin 70/30) Drug List Oral Hypoglycemic Agents First- Generation Sulfonylureas • chlorpropamide (Diabinese) • tolbutamide Drug List Oral Hypoglycemic Agents Second-Generation Sulfonylureas • glimepiride (Amaryl) • glipizide (Glucotrol, Glucotrol XL) • glyburide (DiaBeta, Glynase, Micronase) glipizide (Glucotrol, Glucotrol XL) • Taken with breakfast • Promotes insulin release from beta cells • Increases insulin sensitivity glipizide Dispensing Issues Warning! • Look-Alike and Sound-Alike Drugs – Glucotrol – Glucotrol XL glipizide Dispensing Issues Warning! • Look-Alike and Sound-Alike Drugs – glipizide (Glucotrol, Glucotrol XL) – glyburide (DiaBeta, Glynase, Micronase) Drug List Oral Hypoglycemic Agents Enzyme inhibitors: • acarbose (Precose) • miglitol (Glyset) Biguanide: • metformin (Glucophage, Riomet) metformin (Glucophage, Riomet) • Decreases intestinal absorption of glucose and improves insulin sensitivity • Has an effect on serum lipid levels • Best candidates are overweight diabetics with high lipid profile Drug List Oral Hypoglycemic Agents Glitazones/Thiazolidinediones • pioglitazone (Actos) • rosiglitazone (Avandia) pioglitazone (Actos) • Depends on the presence of insulin • Liver enzymes should be carefully monitored • May be taken without regard to food rosiglitazone (Avandia) • Increases insulin sensitivity in muscle and adipose tissue • Can be taken without regard to food Drug List Oral Hypoglycemic Agents Meglitinides • nateglinide (Starlix) • repaglinide (Prandin) Drug List Oral Hypoglycemic Agents Combinations • glipizide-metformin (Metaglip) • glyburide-metformin (Glucovance) • rosiglitazone-metformin (Avandamet) Discussion What does a diabetic have to be concerned with in relation to diet? Discussion What does a diabetic have to be concerned with in relation to diet? Answer: Eating at the same time everyday; to limit sugar intake by reading package labels