* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download document
Immunocontraception wikipedia , lookup
Major histocompatibility complex wikipedia , lookup
Duffy antigen system wikipedia , lookup
DNA vaccination wikipedia , lookup
Psychoneuroimmunology wikipedia , lookup
Lymphopoiesis wikipedia , lookup
Immune system wikipedia , lookup
Innate immune system wikipedia , lookup
Monoclonal antibody wikipedia , lookup
Molecular mimicry wikipedia , lookup
Adaptive immune system wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
Immunosuppressive drug wikipedia , lookup
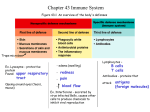
Objectives 8 A. Characteristics of Immune Responses Every immune response has these characteristics: 1. It is antigen specific 2. It is systemic in scope 3. It has memory Red: defects in innate immunity Green: defects in specific immunity Yellow both systems intact Objective 9 Cell Mediated and Humoral Immunity There are two interacting mechanisms in the immune response: Cells Involved Humoral Immunity (Antibody Mediated) B lymphocytes and their descendants (plasma cells) Mechanism plasma cells secrete antibodies into body fluids antibody is transported in body fluids to the site of infection antibodies form complexes with antigens and may activate complement, neutralize the antigen or immobilize the antigen by precipitation or agglutination C. Definitions Neutralization: the antibody combines with the antigen and blocks an active site, preventing antigen binding to receptors on tissue cells Agglutination: antibodies are divalent (have more than one binding site); they can bind to more than one antigen at a time, forming cross linked clumps of antigen/antibody complexes Precipitation: same as agglutination, but the antigen is a soluble molecule; clumping causes the soluble antigen to fall out of solution Cell Mediated Immunity Cells Involved Mechanism T lymphocytes T lymphocytes travel directly to the site of infection and act directly to lyse the invader or indirectly by secreting chemicals which activate other immune mechanisms Objective 10 1. Cells of the Adaptive IS Antigen Presenting Cells: include dendritic cells, macrophages. B lymphocytes APCs engulf antigens and present fragments of the engulfed antigens to B cells and/or T cells 2. B Lymphocytes and T Lymphocytes a. Maturation: Subsets of B Lymphocytes and T Lymphocytes: B Lymphocytes Differentiate in bone marrow where they acquire surface antibody (B cell receptor) They then travel to lymph nodes and other lymphoid tissues Self reactive B cells are deleted in bone marrow or are inactivated in peripheral lymphoid tissues (anergy) Activation leads to mitosis and the production of plasma cells (which secrete antibody) and memory cells Plasma Cell: antibody secreting cell that is a descendant of an activated B lymphocyte Memory Cell descendant of a B lymphocyte that is programmed to respond quickly to the same subsequent encounters with the same antigen T Lymphocyte: lymphocyte that has differentiated in the thymus gland where it acquires a T cell receptor (TCR) It later travels to lymph nodes and other lymphoid tissues T cells must acquire two properties while in the thymus gland: 1. Must be able to bind to MHC class 1 antigens found on the surfaces of nucleated body cells (positive selection) 2. Must not react to self antigens bound to MHC class 1 molecules on the surface of nucleated body cells T cells that fail to meet these criteria are removed from the pool of developing T cells via apoptosis T Cell Subsets: Helper T Cells: Specific Glycoprotein: Activating Cell CD 4 APC presentation of antigen requires MHC class II antigen and processed antigen Generally, they activate macrophages, attract WBCs, assist in B cell and T cell activation and stimulate B cell and T cell divsion TH1 subset TH2 subset Is involved in stimulating inflammation, activating macrophages and promoting cytotoxic T cell activation Is involved in eosinophil recruitment ; stimulates B cell division and antibody production activation Cytotoxic T Cells Specific Glycoprotein: CD8 Activating Cell: APC presentation of antigen Functions: Directly attack and kill body cells infected with virus or other intracellular parasites, cancer cells and transplanted tissue cells Cytoxic T cells kill their targets by: 1. Inducing apoptosis 2. Releasing cytokines Regulatory T Cells Specific glycoprotein: CD8 Regulate the immune response by releasing inhibitory cytokines (IL 10, transforming growth factor , interferon) Gamma Delta T Cells Activation: unknown Function(s) Located mostly within epithelium recognize markers expressed by stressed or damaged cells Objective 11 Antigens (Immunogens) A. (Immunogens) antigens are substances which evoke immune responses typically, antigens are: 1. Large, complex molecules 2. Natural or man-made substances 3. Are non-self B. A complete antigen has two properties: Immunogenicity can activate B cells and/or T cells Reactivity can react with activated T cells or antibodies Immunogenicity Reactivity An incomplete antigen (hapten) is a molecule that is too small by itself to be immunogenic; it can become immunogenic if it attaches to a larger carrier protein and becomes part of a larger complex Antigenic determinants (epitopes): the portions of the antigen that are actually immunogenic Objective 12 The Humoral Response To Antigen Objective 13 Immunity can be innate or acquired through exposure to antigens: Active Immunity generated when an individuals B cells encounter antigen and manufacture antibodies as part of an immune response (IR); long lasting protection is generated Passive Immunity generated when an individual receives antibodies produced by another organism (human or animal donor); shorter duration because no memory is generated Acquired Immunity Naturally Acquired Immunity immunity that is acquired as a result of a natural process (eg, infection, placental transfer of antibody) Artificially Acquired Immunity immunity that is acquired when the antigen is introduced as part of a clinical process (eg., vaccination) Acquired Immunity specifically obtained through the transfer of serum from one individual to another individual is order to fight a disease is an example of: Immunity that is passive and artificial Objective 14 Antibodies (Immunoglobulins) Antibodies (immuoglobulins) are glycoproteins secrted by plasma cells. They are located in interstitial fluid, plasma (gamma globulins) and in body secretions Antibody Structure Four polypeptide chains (two heavy, two light) Chains are held together by covalent disulfide bonds (S=S) each heavy and light chain has two functional areas: Variable region Constant region consists of highly variable amino acid sequences and forms the basis of antigen specificity; antigen binds here more conserved amino acid sequences, which define the 5 antibody classes: IgA, IgD, IgE, IgG, IgM each class has its own effector functions B. Antibody Classes: Class IgD IgM IgG Generalized Location(s) Structure Attached to B cell surfaces Function(s) B cell activation First antibody released during a primary infection; potent agglutinator; activates compliment Pentamer is found in IF and plasma Monomer is attached Monomer is involved in B cell to B cell surfaces activation Plasma and IF Effective against bacteria, extracellular viruses and toxins; activates complement and crosses the placenta IgA Body Secretions protects body surfaces and prevents the attachment of pathogens IgE Attached to mast cell and basophil surfaces Triggers the release of histamine and other mediators of inflammation during allergic reactions B cell receptors are IgM early in the primary response and IgD afterwards Objective 15 The Cell Mediated Response Objective 16 MHC Major histocompatibility (MHC) antigens are self antigens that are tolerated by the host, but not by other genetically different individuals. There are two classes of MHC surface markers. MHC Class I: Location: All cells except RBCs Recognized by: CD8 T cells Function activate cytotoxic T cells if body cells are infected with intracellular parasites such as viruses, if body cells become malignant, or by non-self antigens (eg, transplants) MHC Class I antigens allow activated cytotoxic T cells to interact with the target cell How MHC Class I and Endogenous Peptides are displayed on all cells (except RBCs) Note: TAP (transporter associated with antigen processing) MHC Class II: Location: Dendritic cells, macrophages, B cells Recognized by: CD 4 cells Function present antigens to helper T cells How MHC Class II and peptide derived from extracellular antigen is displayed on an APC surface The MHC Class I antigens of a donor will stimulate a recipient to reject a transplanted tissue causing tissue incompatibility; it is the class I proteins that are typed and matched prior to transfusion autograft : tissue is grafted from an individual back to himself isograft : tissue is transplanted between genetically identical individuals allograft xenograft : tissue is transplanted between two members of the same species (not genetically identical) : tissue is transplanted from a member of one species to a member of another species A young female soccer player tears her ACL during practice and decides to have it replaced with a graft. She is given several surgical options – decide which category each graft below falls in to: a. A porcine) pig derived ligament (Z-lig) xenograft b. A section of the patient’s own patellar tendon: autoograft c. A section of hamstring from a cadaver (not a relative): allograft