* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download and T cells
Anti-nuclear antibody wikipedia , lookup
Social immunity wikipedia , lookup
Duffy antigen system wikipedia , lookup
Lymphopoiesis wikipedia , lookup
Complement system wikipedia , lookup
Immunocontraception wikipedia , lookup
Hygiene hypothesis wikipedia , lookup
DNA vaccination wikipedia , lookup
Molecular mimicry wikipedia , lookup
Immune system wikipedia , lookup
Adoptive cell transfer wikipedia , lookup
Monoclonal antibody wikipedia , lookup
Psychoneuroimmunology wikipedia , lookup
Adaptive immune system wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
Innate immune system wikipedia , lookup
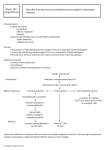
Innate Immunity Dr. Hani Masaadeh, MD, PhD Immunity: “Free from burden”. Ability of an organism to recognize and defend itself against specific pathogens or antigens. Immune Response: Third line of defense. Involves production of antibodies and generation of specialized lymphocytes against specific antigens. Antigen: Molecules from a pathogen or foreign organism that provoke a specific immune response. • immunity possessed by a group (as a species or race) that is present in an individual at birth prior to exposure to a pathogen or antigen and that includes components (as intact skin, salivary enzymes, neutrophils, natural killer cells, and complement) which provide an initial response against infection— called also natural immunity; compare ACQUIRED IMMUNITY, ACTIVE IMMUNITY, PASSIVE IMMUNITY Defensive mechanisms include : 1) Innate immunity (Natural or Non specific) 2) Acquired immunity (Adaptive or Specific) Cell-mediated immunity Humoral immunity Innate or Genetic Immunity: Immunity an organism is born with. • Genetically determined. • May be due to lack of receptors or other molecules required for infection. Acquired Immunity:Immunity that an organism develops during lifetime. • Not genetically determined. • May be acquired naturally or artificially. • Innate immunity is the first line of defense against infections. The cells and soluble molecules of innate immunity either exist in a fully functional state before encounter with microbes or are rapidly activated by microbes, faster than the development of adaptive immune responses • Innate immunity is present before any exposure to pathogens and is effective from the time of birth • • It involves nonspecific responses to pathogens • • Innate immunity consists of external barriers plus internal cellular and chemical defenses Components of Human Immune System • Innate immunity is the initial response to microbes that prevents, controls, or eliminates infection of the host by many microbes. • Innate immune mechanisms recognize the products of damaged and dead host cells and serve to eliminate these cells and to initiate the process of tissue repair. • Innate immunity to microbes stimulates adaptive immune responses and can influence the nature of the adaptive responses to make them optimally effective against different types of microbes. • The two major types of responses of the innate immune system that protect against microbes are inflammation and antiviral defense. • The innate immune system recognizes microbial products that are often essential for survival of the microbes • The innate immune system also recognizes endogenous molecules that are produced by or released from damaged and dying cells. These substances are called damageassociated molecular patterns (DAMPs) • The innate immune system uses several types of cellular receptors, present in different locations in cells, and soluble molecules in the blood and mucosal secretions to recognize PAMPs and DAMPs • The receptors of the innate immune system are encoded in the germline, whereas the receptors of adaptive immunity are generated by somatic recombination of receptor genes in the precursors of mature lymphocytes • The innate immune system does not react against normal, healthy cells and tissues. • Most cell types express pattern recognition receptors and therefore are capable of participating in innate immune responses. Phagocytes, including neutrophils and macrophages, and dendritic cells express the widest variety and greatest amount of these receptors • Toll-like Receptors • The Toll-like receptors (TLRs), an evolutionarily conserved family of pattern recognition receptors expressed on many cell types, recognize products of a wide variety of microbes. • Mammalian TLRs are involved in responses to a wide variety of molecules that are expressed by microbial but not by healthy mammalian cells. • TLRs are also involved in response to endogenous molecules whose expression or location indicates cell damage. • The structural basis of TLR specificities resides in the multiple extracellular leucine-rich modules of these receptors, which bind directly to PAMPs or to adaptor molecules that bind the PAMPs. • TLRs are found on the cell surface and on intracellular membranes and are thus able to recognize microbes in different cellular locations • TLR recognition of microbial ligands results in the activation of several signaling pathways and ultimately transcription factors, which induce the expression of genes whose products are important for inflammatory and antiviral responses • RIG-like Receptors • RIG-like receptors (RLRs) are cytosolic sensors of viral RNA that respond to viral nucleic acids by inducing the production of the antiviral type I interferons. • • • • Other Cell-Associated Pattern Recognition Receptors Receptors for Carbohydrates Scavenger Receptors N-Formyl Met-Leu-Phe Receptors • • • • • CELLULAR COMPONENTS OF THE INNATE IMMUNE SYSTEM Epithelial Barriers Phagocytes Dendritic Cells Natural Killer Cells • Effector Functions of NK Cells • The effector functions of NK cells are to kill infected cells and to activate macrophages to destroy phagocytosed microbes • Mast Cells • Mast cells are present in the skin and mucosal epithelium and rapidly secrete proinflammatory cytokines and lipid mediators in response to infections and other stimuli. • THE INFLAMMATORY RESPONSE • The major way by which the innate immune system deals with infections and tissue injury is to stimulate acute inflammation, which is the accumulation of leukocytes, plasma proteins, and fluid derived from the blood at an extravascular tissue site of infection or injury. • Acute inflammation can develop in minutes to hours and last for days. Chronic inflammation is a process that takes over from acute inflammation if the infection is not eliminated or the tissue injury is prolonged. It usually involves recruitment and activation of monocytes and lymphocytes. • The Major Proinflammatory Cytokines TNF, IL-1, and IL-6 • One of the earliest responses of the innate immune system to infection and tissue damage is the secretion of cytokines by tissue cells, which is critical for the acute inflammatory response. Three of the most important proinflammatory cytokines of the innate immune system are TNF, IL-1and IL-6 • Tumor Necrosis Factor • Tumor necrosis factor (TNF) is a mediator of the acute inflammatory response to bacteria and other infectious microbes. • Interleukin-1 (IL-1) is also a mediator of the acute inflammatory response and has many similar actions as TNF. • Interleukin-6 • IL-6 is another important cytokine in acute inflammatory responses that has both local and systemic effects, including the induction of liver synthesis of a variety of other inflammatory mediators, the stimulation of neutrophil production in the bone marrow, and the differentiation of IL17–producing helper T cells. • Recruitment of large numbers of neutrophils, followed by monocytes, from blood into tissues typically occurs as part of the acute inflammatory response to infections and tissue injury. The cytokines TNF, IL-1, and IL-6 and chemokines, which are secreted in the local sites of infection or tissue injury. • Recruitment of Leukocytes to Sites of Infection • Phagocytosis and Killing of Microbes by Activated Phagocytes • Neutrophils and macrophages that are recruited into sites of infections ingest microbes into vesicles by the process of phagocytosis and destroy these microbes . • Neutrophils and macrophages express receptors that specifically recognize microbes, and binding of microbes to these receptors is the first step in phagocytosis. • Activated neutrophils and macrophages kill phagocytosed microbes by the action of microbicidal molecules in phagolysosomes • A complication of severe bacterial sepsis is a syndrome called septic shock • Acute inflammation may cause tissue injury because the effector mechanisms that phagocytes use to kill microbes are also highly toxic to host tissues. • THE ANTIVIRAL RESPONSE • The major way by which the innate immune system deals with viral infections is to induce the expression of type I interferons, whose most important action is to inhibit viral replication. • Type I interferons are a large family of structurally related cytokines that mediate the early innate immune response to viral infections • Type I interferons increase the cytotoxicity of NK cells and CD8+ . • Type I interferons upregulate expression of class I MHC molecules and thereby increase the probability that virally infected cells will be recognized and killed by CD8+ CTLs. External Defenses • Intact skin and mucous membranes • Form physical barriers that bar the entry of microorganisms and viruses • Certain cells of the mucous membranes produce mucus • A viscous fluid that traps microbes and other particles • In the trachea, ciliated epithelial cells • Sweep mucus and any entrapped microbes upward, m preventing the microbes from entering the10lungs Figure 43.3 • Secretions of the skin and mucous membranes • Provide an environment that is often hostile to microbes • Secretions from the skin • Give the skin a pH between 3 and 5, which is acidic enough to prevent colonization of many microbes • Also include proteins such as lysozyme, an enzyme that digests the cell walls of many bacteria • Phagocytes, types of white blood cells • Ingest invading microorganisms • Initiate the inflammatory response • Macrophages, a specific type of phagocyte • Can be found migrating through the body • Can be found in various organs of the lymphatic system Types of Acquired Immunity I. Naturally Acquired Immunity: Obtained in the course of daily life. A. Naturally Acquired Active Immunity: • Antigens or pathogens enter body naturally. • Body generates an immune response to antigens. • Immunity may be lifelong (chickenpox or mumps) or temporary (influenza or intestinal infections). B. Naturally Acquired Passive Immunity: • Antibodies pass from mother to fetus via placenta or breast feeding (colostrum). • No immune response to antigens. • Immunity is usually short-lived (weeks to months). • Protection until child’s immune system develops. Types of Acquired Immunity (Continued) II. Artificially Acquired Immunity: Obtained by receiving a vaccine or immune serum. 1. Artificially Acquired Active Immunity: • Antigens are introduced in vaccines (immunization). • Body generates an immune response to antigens. • Immunity can be lifelong (oral polio vaccine) or temporary (tetanus toxoid). 2. Artificially Acquired Passive Immunity: • Preformed antibodies (antiserum) are introduced into body by injection. • Snake antivenom injection from horses or rabbits. • Immunity is short lived (half life three weeks). • Host immune system does not respond to antigens. Aquired (specific) immunity * The acquired immune response is more specialized than innate immune response * The acquired immune response involves a combination of two mechanisms : 1) Humoral immune response 2) cell mediated immune response * They interact with one another to destroy foreign body (microorganisms, infected cells, tumor cells) Aquired (specific) immunity Two mechanisms 1) Humoral immune response: - Antibodies are produced by B-lymphocytes - These have the ability to recognize and bind specifically to antigen that induced their formation 2) The cell mediated immune response (CMI) - It is mediated by certain types of T-lymphocytes - T-lymphocytes recognize foreign material by means of surface receptors - T-lymphocytes attack and destroy foreign material directly or through release of soluble mediators i.e. cytokines Characters Of Acquired Immune Response 1) Highly specific for the invading organism 2) Discrimination between “self and “non self” molecules The response only occurs to “non self” molecules 3) Diversity: - It can respond to millions of different antigens - Lymphoctes population consists of many different clones (one cell and its progny) - Each clone express an antigen receptor and responds only to one antigenic epitope Mechanism Of Acquired Immune Response Acquired immune response is initiated by: * Recognition of the antigen by specific lymphocytes * Activation of these specific lymphocytes * Proliferation and differentiation into effector cells; -The effector cells eliminate the antigen -Return of homeostasis and development of memory cells * Memory cells evoke a more rapid and long response on re-exposure to same antigen Acquired Or Adaptive Immunity I- Passive acquired immunity a-Naturally passive acquired immunity Antibodies are passed through placenta to the fetus b- Artificially passive acquired immunity The injection of alredy prepared antibodies, such as gamma globulin (short-term immunization) II- Active acquired immunity a-Natural active acquired immunity : - Following clinical or subclinical infections - measles or mumps, in which immunity is long lasting b- Artificial active acquired immunity : - Following vaccination with live or killed infectious agents or their products Mechanism of Humoral immunity * Antibodies induce resistance through: 1) Antitoxin neutralize bacterial toxins (diphtheria,tetanus) Antitoxin are developed actively as a result of: a- Previous infection b- Artificial immunization c- Transferred passively as antiserum * Neutralization of toxin with antitoxin prevents a combination with tissue cells Mechanism of Humoral immunity 2) Antibodies attach to the surface of bacteria and a- act as opsonins and enhance phagocytosisd b- prevent the adherence of microorganisms to their target cells, e.g. IgA in the gut c- Activate the complement and lead to bacterial lysis d- Clump bacteria (agglutination) leading to phagocytosis Vaccination * Vaccination prevents and control such diseases as cholera, rabies, poliomyelitis, diphtheria, tetanus, measles, and typhoid fever * Vaccines can be: a- prophylactic (e.g. to prevent the effects of a future infection by any natural or "wild" pathogen b- Therapeupic (e.g. vaccines against cancer are also being investigated) Vaccination Vaccination: *Producing immunity against pathogens (viruses and bacteria) by the introduction of live, killed, or altered antigens that stimulate the body to produce antibodies against more dangerous forms *Vaccines work with the immune system's ability to recognize and destroy foreign proteins (antigens) Vaccination Immunization of young children and adolescents: - Hepatitis B (HepB) and Hepatitis A (HepA) - Diphtheria, tetanus and pertussis (whooping cough) given together as DTaP (formerly DTP) - Haemophilus influenzae b (Hib) - Poliomyelitis (IPV) - Measles, Mumps, and Rubella, given together as MMR - Chicken pox (Var) - Neisseria meningitidis (meningococcal meningitis) Cells Of Immune Response Cells involved in specific immune mechanisms are: I) Hematopoitic leucocytes 1- Lymphoid * T-lymphocytes: - Antigen specific cells carrying CD3 complex, CD4, CD8 - Dominant blood lymphocytes (70%) - Produce cytokines - Activation of other cells (Th CD4) - Suppressors for others (Ts CD8) Cells Of Immune Response * B-lymphocytes: - Antigen specific cells with surface receptor - Less common lymphocytes (20%) - Responsible for antibody production * NK, K cells: - Not antigen specific - Carry Fc receptors , NK-target cell receptor Cells of Immune Response (cont.) 2- Monocytic myeloid a- Monocyte-tissue macrophages: . Non specific . Carry Fc receptors . Phagocytic . Antigen processing and presenting cells . Produce cytokines b- Neutrophils: . Non specific . Carrying Fc, complement molecules Cells of Immune Response (cont.) c- Eosinophils: . Non specific . Carrying Fc receptor . Produce allergic mediators d- Basophils and Mast cells: . Non specifc . Carrying Fc receptors . Produce allergic mediators Humoral Immunity (Continued) Clonal Selection • Clonal Selection: B cells (and T cells) that encounter stimulating antigen will proliferate into a large group of cells. • Why don’t we produce antibodies against our own antigens? We have developed tolerance to them. • Clonal Deletion: B and T cells that react against self antigens appear to be destroyed during fetal development. Process is poorly understood. Consequences of Antigen-Antibody Binding Antigen-Antibody Complex: Formed when an antibody binds to an antigen it recognizes. Affinity: A measure of binding strength. 1. Agglutination: Antibodies cause antigens (microbes) to clump together. • IgM (decavalent) is more effective that IgG (bivalent). • Hemagglutination: Agglutination of red blood cells. Used to determine ABO blood types and to detect influenza and measles viruses. 2. Opsonization: Antigen (microbe) is covered with antibodies that enhances its ingestion and lysis by phagocytic cells. Humoral Immunity (Continued) 3. Neutralization: IgG inactivates viruses by binding to their surface and neutralize toxins by blocking their active sites. 4. Antibody-dependent cell-mediated cytotoxicity: Used to destroy large organisms (e.g.: worms). Target organism is coated with antibodies and bombarded with chemicals from nonspecific immune cells. 5. Complement Activation: Both IgG and IgM trigger the complement system which results in cell lysis and inflammation. Immunological Memory Antibody Titer: The amount of antibody in the serum. Pattern of Antibody Levels During Infection Primary Response: • After initial exposure to antigen, no antibodies are found in serum for several days. • A gradual increase in titer, first of IgM and then of IgG is observed. • Most B cells become plasma cells, but some B cells become long living memory cells. • Gradual decline of antibodies follows. Immunological Memory (Continued) Secondary Response: • Subsequent exposure to the same antigen displays a faster and more intense antibody response. • Increased antibody response is due to the existence of memory cells, which rapidly produce plasma cells upon antigen stimulation. Duality of Immune System (Continued) II. Cell Mediated Immunity • Involves specialized set of lymphocytes called T cells that recognize foreign antigens on the surface of cells, organisms, or tissues: • Helper T cells • Cytotoxic T cells • T cells regulate proliferation and activity of other cells of the immune system: B cells, macrophages, neutrophils, etc. • Defense against: • Bacteria and viruses that are inside host cells and are inaccessible to antibodies. • Fungi, protozoa, and helminths • Cancer cells • Transplanted tissue T Cells and Cell Mediated Immunity Antigens that stimulate this response are mainly intracellular. Requires constant presence of antigen to remain effective. Unlike humoral immunity, cell mediated immunity is not transferred to the fetus. Cytokines: Chemical messengers of immune cells. • Over 100 have been identified. • Stimulate and/or regulate immune responses. • Interleukins: Communication between WBCs. • Interferons: Protect against viral infections. • Chemokines: Attract WBCs to infected areas. T Cells and Cell Mediated Immunity Types of T cells 1. T Helper (TH) Cells: Central role in immune response. • Most are CD4+ • Recognize antigen on the surface of antigen presenting cells (e.g.: macrophage). • Activate macrophages • Induce formation of cytotoxic T cells • Stimulate B cells to produce antibodies. Types of T cells (Continued) 2. Cytotoxic T (Tc) Cells: Destroy target cells. • Most are CD4 negative (CD4 -). • Recognize antigens on the surface of all cells: • Kill host cells that are infected with viruses or bacteria. • Recognize and kill cancer cells. • Recognize and destroy transplanted tissue. • Release protein called perforin which forms a pore in target cell, causing lysis of infected cells. • Undergo apoptosis when stimulating antigen is gone. Types of T cells (Continued) 3. Delayed Hypersensitivity T (TD) Cells: Mostly T helper and a few cytotoxic T cells that are involved in some allergic reactions (poison ivy) and rejection of transplanted tissue. 4. T Suppressor (Ts) Cells: May shut down immune response. Nonspecific Cellular Components 1. Activated Macrophages: Stimulated phagocytes. • Stimulated by ingestion of antigen • Larger and more effective phagocytes. • Enhanced ability to eliminate intracellular bacteria, virus-infected and cancerous cells. 2. Natural Killer (NK) Cells: • Lymphocytes that destroy virus infected and tumor cells. • Not specific. Don’t require antigen stimulation. • Not phagocytic, but must contact cell in order to lyse it. Relationship Between Cell-Mediated and Humoral Immunity 1. Antibody Production T-Dependent Antigens: • • • • Antibody production requires assistance from T helper cells. A macrophage cells ingest antigen and presents it to TH cell. TH cell stimulates B cells specific for antigen to become plasma cells. Antigens are mainly proteins on viruses, bacteria, foreign red blood cells, and hapten-carrier molecules. T-Independent Antigens: • Antibody production does not require assistance from T cells. • Antigens are mainly polysaccharides or lipopolysaccharides with repeating subunits (bacterial capsules). • Weaker immune response than for T-dependent antigens. Relationship Between Cell-Mediated and Humoral Immunity 2. Antibody Dependent Cell Mediated Cytotoxicity • Target cell is covered with antibodies, leaving Fc portion sticking outwards. • Natural killer and other nonspecific cells that have receptors for Fc region are stimulated to kill targeted cells. • Target organism is lysed by substances secreted by attacking cells. • Used to destroy large organisms that cannot be phagocytosed. • Humoral and cell-mediated immunity defend against different types of threats • Acquired immunity includes two branches • The humoral immune response involves the activation and clonal selection of B cells, resulting in the production of secreted antibodies • The cell-mediated immune response involves the activation and clonal selection of cytotoxic T cells • Serum: Fluid that remains after blood has clotted and cells have been removed. • Antiserum: Serum containing antibodies to a specific antigen(s). Obtained from injecting an animal (horse, rabbit, goat) with antigen (snake venom, botulism or diphtheria toxin). • Serology: The study of reactions between antibodies and antigens. • Gamma Globulins: Fraction of serum that contains most of the antibodies. • Serum Sickness: Disease caused by multiple injections of antiserum. Immune response to foreign proteins. May cause fever, kidney problems, and joint pain. Rare today. • Antibodies are circulating proteins that are produced in vertebrates in response to exposure to foreign structures known as antigens. • The substances that generated or were recognized by antibodies were then called antigens • Antibodies can exist in two forms: membrane-bound antibodies on the surface of B lymphocytes function as receptors for antigen, and secreted antibodies that reside in the circulation, tissues, and mucosal sites neutralize toxins, prevent the entry and spread of pathogens, and eliminate microbes. • B lymphocytes are the only cells that synthesize antibody molecules. • Structural Features of Antibody Variable Regions • Most of the sequence differences and variability among different antibodies are confined to three short stretches in the V region of the heavy chain and to three stretches in the V region of the light chain. These diverse stretches are known as hypervariable segments Antibodies are Produced by B Lymphocytes Antibodies are Proteins that Recognize Specific Antigens Antibodies Proteins that recognize and bind to a particular antigen with very high specificity. Made in response to exposure to the antigen. One virus or microbe may have several antigenic determinant sites, to which different antibodies may bind. Each antibody has at least two identical sites that bind antigen: Antigen binding sites. Valence of an antibody: Number of antigen binding sites. Most are bivalent. Belong to a group of serum proteins called immunoglobulins (Igs). Antibody Structure Monomer: A flexible Y-shaped molecule with four protein chains: • 2 identical light chains • 2 identical heavy chains Variable Regions: Two sections at the end of Y’s arms. Contain the antigen binding sites (Fab). Identical on the same antibody, but vary from one antibody to another. Constant Regions: Stem of monomer and lower parts of Y arms. Fc region: Stem of monomer only. Important because they can bind to complement or cells. Properties of Immunoglobulins Property IgG Heavy chain symbol γ α µ ε δ Molecular weight 150 KDa 170-400 KDa 900 KDa 190 KDa 180 KDa Percentage in serum 75 % 15 % 10 % 0.004 % % 0.2 Complement fixation Yes No Yes No No Transplacental passage Yes No No No No Opsonization Yes No No No No IgA IgM IgE IgD Primary and Secondary antibody response Secondary response to Ag Amount of antibodies in serum Primary response to Ag 1 2 3 4 5 6 Time (months) 1st injection of Ag 2nd injection of Ag Immunoglobulin Classes I. IgG Structure: Monomer Percentage serum antibodies: 80% Location: Blood, lymph, intestine Half-life in serum: 23 days Complement Fixation: Yes Placental Transfer: Yes Known Functions: Enhances phagocytosis, neutralizes toxins and viruses, protects fetus and newborn. Immunoglobulin Classes II. IgM Structure: Pentamer Percentage serum antibodies: 5-10% Location: Blood, lymph, B cell surface (monomer) Half-life in serum: 5 days Complement Fixation: Yes Placental Transfer: No Known Functions: First antibodies produced during an infection. Effective against microbes and agglutinating antigens. Immunoglobulin Classes III. IgA Structure: Dimer Percentage serum antibodies: 10-15% Location: Secretions (tears, saliva, intestine, milk), blood and lymph. Half-life in serum: 6 days Complement Fixation: No Placental Transfer: No Known Functions: Localized protection of mucosal surfaces. Provides immunity to infant digestive tract Immunoglobulin Classes IV. IgD Structure: Monomer Percentage serum antibodies: 0.2% Location: B-cell surface, blood, and lymph Half-life in serum: 3 days Complement Fixation: No Placental Transfer: No Known Functions: In serum function is unknown. On B cell surface, initiate immune response. Immunoglobulin Classes V. IgE Structure: Monomer Percentage serum antibodies: 0.002% Location: Bound to mast cells and basophils throughout body. Blood. Half-life in serum: 2 days Complement Fixation: No Placental Transfer: No Known Functions: Allergic reactions. Possibly lysis of worms. Antibodies Antibodies Immunoglobulin G (IgG) • Most abundant class (80%-85%) • Transported across the placenta • Four classes • IgG1, IgG2, IgG3, and IgG4 Immunoglobulin A (IgA) • Two classes • IgA1 molecules are found predominantly in the blood • IgA2 molecules are found predominantly in normal body secretions • IgAs found in body secretions are dimers anchored by a J chain and a “secretory” piece • Secretory piece may function to protect IgAs against enzyme degradation Immunoglobulin M (IgM) • Largest of the immunoglobulins • Pentamer stabilized by a J chain • First antibody produced during the primary response to an antigen • Synthesized during fetal life Immunoglobulin D (IgD) • • • • Limited information on IgD function Low concentration in the blood Located primarily on the surface of developing B lymphocytes Function as one type of B cell antigen receptor Immunoglobulin E (IgE) • Least concentrated of the immunoglobulin classes in the circulation • Mediator of many common allergic responses • Defender against parasites IgE Function • Provides protection from large parasites • Initiates an inflammatory reaction to attract eosinophils • When produced against innocuous environmental antigens, they are a common cause of allergies • Fc portions of IgEs are bound to mast cells Primary and Secondary Responses • Primary response • Initial exposure • Latent period or lag phase • B cell differentiation is occurring • After 5 to 7 days, an IgM antibody for a specific antigen is detected • An IgG response equal or slightly less follows the IgM response Primary and Secondary Responses • Secondary response • More rapid • Larger amounts of antibody are produced • Rapidity is due to the presence of memory cells that do not have to differentiate • IgM is produced in similar quantities to the primary response, but IgG is produced in considerably greater numbers Antibody Response After Exposure to Antigen Antigens Most are proteins or large polysaccharides from a foreign organism. • Microbes: Capsules, cell walls, toxins, viral capsids, flagella, etc. • Nonmicrobes: Pollen, egg white , red blood cell surface molecules, serum proteins, and surface molecules from transplanted tissue. Lipids and nucleic acids are only antigenic when combined with proteins or polysaccharides. Molecular weight of 10,000 or higher. • Hapten: Small foreign molecule that is not antigenic. Must be coupled to a carrier molecule to be antigenic. Once antibodies are formed they will recognize hapten. Part I Antigen and its characteristics I. Definition of antigen Antigen: Those substances that can induce a specific immune response and specifically bind products of immune response in vitro or in vivo. . Antigen . Tolerogen . Allergen II. Characteristics of Ag 1. Immunogenicity The ability of antigen which can stimulate the immune system of individual to induce a specific immune response. 2. Immunoreactivity The ability of antigen which can combine with corresponding Ab or sensitized T lymphocyte. III. Structure of antigen hapten and carrier Hapten: Only possess immunoreactivity Carrier: Enhance the immunogenicity of hapten • Immunogens :possess both characteristics Hapten +carrier complete antigen(immunogens) Part II Factors of affecting immunogenicity of antigen I. Factors related to antigen 1. Foreignness According to Burnet clone selection theory , foreignness means substances that never contact with lymphocytes in embryo period. (2) Chemical composition and structure Protein>polysaccharides, nucleic acids, lipids (Protein containing aromatic amino acid,such as tyrosine) (3) Physical nature Polymer > Monomer Cycle molecule >linear molecule Particulate Ag> soluble Ag II. Factors related to host 1. Genetic backround (Species, Individual) 2. Age,Sex and healthy condition II. Common antigen and cross reaction 1. Common antigen Different antigens which possess the same or similar epitopes are called common antigen. 2. Mechanism of cross reaction ----Existence of common Ag determinant Because there are some common antigen determinants existing in different microbes, so the antiserum against one kind of microbe can also react with another microbe,this called cross reaction. 3. Significance: In clinic, existence of cross reaction may lead to wrong diganosis. Part IV Classification of Ag I. According to immunogenicity of antigens: Antigen Hapten II. According to the dependence of T cells when Ags induce humoral immune response TD-Ag (thymus dependent Ag ) TI-Ag (thymus independent Ag) 1.TD-Ag (thymus dependent Ag ) TD-Ag can stimulate B cell to produce Ab with the help of T cell Most of TD-Ag are protein Have many kinds of determinants Can induce HI and CMI Stimulate B cell to produce :IgG, IgM, IgA Have immune memory 2. TI-Ag (thymus independent Ag) TI-Ag can stimulate B cells to produce Ab without the help of T cell Most are polysaccharide Have more same or repeat determinants Only induce B cell to produce IgM Can not induce CMI No immune memory III. According to source of antigen Xenoantigen Alloantigen Autoantigen Heterophile antigens(Forssman antigen) The common antigen existing different species. Part V Important antigens in medicine I. Pathogens and their products 1. Pathogens:such as bacteria et al. Surface antigen: “Vi” Ag Somatic Ag: “O” Ag Flagellar Ag: “H” Ag Pillus Ag 2. Exotoxin and toxoid (1) Exotoxin Produced by G+ bacteria Strong antigenicity and pathogenicity (2) Toxoid Under suitable conditions, exotoxin loss its toxicity without affecting its antigenicity, then the exotoxin turned into toxoid Antitoxin: The antibody produced by exotoxin or toxoid stimulation was called antitoxin. ABO system Blood type A B AB O antigen on RBC A B A,B - antibody in serum anti-B anti-A anti-A, anti-B • Recipient-donor combinations • Can be fatal or safe Table 43.1 • Another red blood cell antigen, the Rh factor • Creates difficulties when an Rh-negative mother carries successive Rhpositive fetuses Allergies • Allergies are exaggerated (hypersensitive) responses • To certain antigens called allergens • In localized allergies such as hay fever • IgE antibodies produced after first exposure to an allergen attach to receptors on mast cells • The next time the allergen enters the body • It binds to mast cell–associated IgE molecules • The mast cells then release histamine and other mediators • That cause vascular changes and typical symptoms • An acute allergic response sometimes leads to anaphylactic shock • A whole-body, life-threatening reaction that can occur within seconds of exposure to an allergen Thanks