* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Lecture 3 – intro to ANS drugs – cholinergic
Pharmacognosy wikipedia , lookup
5-HT3 antagonist wikipedia , lookup
Discovery and development of beta-blockers wikipedia , lookup
NMDA receptor wikipedia , lookup
5-HT2C receptor agonist wikipedia , lookup
Drug interaction wikipedia , lookup
Toxicodynamics wikipedia , lookup
Discovery and development of angiotensin receptor blockers wikipedia , lookup
Norepinephrine wikipedia , lookup
Cannabinoid receptor antagonist wikipedia , lookup
NK1 receptor antagonist wikipedia , lookup
Nicotinic agonist wikipedia , lookup
Neuropsychopharmacology wikipedia , lookup
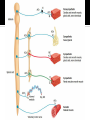
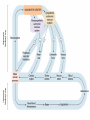
Lecture 3 Autonomic nervous system Sympathetic Parasympathetic Nerve impulses and synapses Axon terminal Synapse Receptors on the effector organ Basic arrangement of nerves: CNS nerve ganglion nerve effector organ Preganglionic and postganglionic nerves ▪ Preganglionic parasympathetic and preganglionic sympathetic ▪ Postganglionic para and postganglionic sympa Preganglionic Postganglionic Parasympa Acetylcholine (long) Acetylcholine (short) Sympa Acetylcholine (short) Noradrenaline or dopamine (long) Ganglionic receptor Effector receptor Parasympa = Cholinoceptors or cholinergic receptors Nicotinic receptor Muscarinic receptor Sympa = Adrenoceptors or adrenergic receptors Nicotinic receptor Muscarinic, Adrenaline, noradrenaline or dopamine receptors 5 key features of neurotransmitter function, which can be targets for pharmacotherapy Synthesis Storage Release Termination of action Receptor effects Acetylcholine (Ach) Produced in the nerve axon body and stored in the axon terminal Synthesized from acetyl-CoA + choline (via enzyme choline acetyltransferase or ChAT) ▪ Acetyl CoA comes from the mitochondria (Krebs) ▪ Choline is absorbed by the nerve cell from outside thru a transporter called choline transporter (CHT) ▪ Blocked by a research drug called Hemicholiniums Once synthesized, Ach is transported to vesicles by a vessicle associated transporter (VAT) ▪ Blocked by a research drug called vesamicol Acetylcholine (Ach) Release of neurotransmitter is dependent on calcium entry into the nerve axon ▪ Once an action potential (nerve impulse) reaches the terminal end of the axon, calcium channels open. ▪ This promotes vesicles to merge with the axonal membrane to release contents into the synapse ▪ Release can be blocked by botolinum toxin Acetylcholine (Ach) Once released, Ach binds with cholinoceptors on the effector organ = effect Ach is then deactivated by AChe (acetylcholinesterase) ▪ Very rapidly ▪ Split into acetate and choline ▪ Choline is then recycled back into the nerve axon Noradrenaline or Norepinephrine Synthesis ▪ Starts as a tyrosine molecule, eventually modified into dopa dopamine norepinephrine epinephrine ▪ Conversion of tyr to dopa inhibited by drug metyrosine Storage ▪ Stored in vesicles via transporter VMAT (vesicular monoamine transporter) ▪ Blocked by drug reserpine = depletion of adrenergic stores Noradrenaline or Norepinephrine Release ▪ Similar to cholinergic release = nerve impulse stimulates opening of Ca++ channels Termination of action ▪ 2 processes: ▪ Simple diffusion away from the receptor site (with eventual metabolism in the plasma or liver) ▪ Reuptake into the nerve terminal by NET (norepinephrine transporter) Blocked by drugs such as cocaine and tricyclic antidepressants (TCAs) = increased neurotransmitter activity in the synapse NANC or nanadrenergic, noncholinergic neurons Some parts of the ANS does not follow the usual classification May use a combination of adrenergic and cholinergic receptors and transmitters May use other substances (ex. nitric oxide, cholecystokinin, enkephalins, serotonin, somatostatin, etc.) ANS = sympa and parasympa Multifactorial and multilevel interactions Ex. blood pressure or mean arterial pressure (MAP) ▪ MAP = CO x TPR ▪ CO = SV x HR SV = Venous return = blood volume = affected by oral intake and kidneys ▪ TPR = arterial diameters ▪ Give norepinephrine (a potent vasoconstrictor) in small doses = promote vasoconstriction and slightly increased HR increase BP ▪ But the TPR will induce the parasympa to HR (via vagus nerve and baroreceptors in the carotid body) ▪ Therefore = there will be an BP with a corresponding HR, despite the direct action of NE to the heart Historically, plant derivatives, muscarine (mushroom Amanita muscaria) and nicotine (tobacco), were applied or ingested, which produced parasympathetic effects. Receptors were termed muscarinic or nicotinic Usually has a diffuse action (due to wide spread presence of cholinergic receptors) Selectivity of action may be achieved via: ▪ Modifying the drug for specific receptors ▪ Modifying route of administration = ex. eye drops Type of receptor Location Muscarinic Nicotinic G protein-linked (stimulates 2nd messenger system) Nerves, CNS, heart, smooth muscle, glands Ion channel Skeletal muscle (NMJ), CNS Preganglionic nerves Receptor Type M1 M2 (Cardiac M2) Location Nerves Heart, nerves, smooth muscle M3 M4 M5 Glands, smooth muscle, endothelium CNS CNS NM NN Skeletal muscle (NMJ) CNS, postganglionic cell body, dendrites Direct acting agents bind to and activate muscarinic or nicotinic receptors Acetylcholine, methacholine, carbachol, bethanechol Indirect acting agents inhibit acetylcholinesterase Neostigmine, carbaryl, physostigmine, edrophonium Pharmacokinetics Permanently charged = hydrophilic ▪ Poorly absorbed into the CNS Rapidly metabolized by Ach-ase (AChe) ▪ Ach = very rapidly metabolized ▪ Need to give a very large amount and injected very quickly to produce an effect ▪ Modified drugs are more resistant to Ach-ase metabolism, and therefore longer duration of action ▪ Methacholine < Carbachol < Bethanechol Pharmacodynamics MOA: ▪ activates muscarinic receptors on effector organ ▪ Inhibits release of neurotransmitters on nerve terminals with muscarinic receptors ▪ In effect, promote parasympa activity and inhibit sympa activity ▪ Muscarinic receptors activate the 2nd messenger cascade (ex. IP3 and DAG cascade) ▪ Nicotinic receptors opens up Na+ and K+ channels causing depolarization of the nerve cell or NMJ, producing contraction of the muscle Pharmacodynamics ▪ Special activity at nicotinic receptors during prolonged exposure to agonists ▪ Prolonged agonist occupancy of the nicotinic receptor will eventually stop its activity (ex. the muscle initially contracts then relaxes despite exposure to the agonist) ▪ Continued presence of the nicotinic agonist prevents electrical recovery of the postjunctional membrane = “depolarizing blockade” (receptor becomes insensitive to more agonist concentrations) ▪ Receptor eventually becomes desensitized to agonist and is becomes more difficult to be reversed (useful in muscle relaxant drugs = ex. succinylcholine) Choline Ester Acetylcholine chloride Methacholine Carbachol Bethanechol Susceptibility to cholinesterase ++++ Muscarinic Nicotinic action action +++ +++ + Negligible Negligible ++++ ++ ++ None +++ None Organ System Effects Eye ▪ Pupillary constriction and accomodation Cardiovascular system ▪ Reduction in peripheral vascular resistance ▪ Decreased HR Respiratory system ▪ Bronchoconstriction and increased glandular activity Organ System Effects Gastrointestinal ▪ Increase secretory and motor activity of the gut Genitourinary ▪ Promote voiding Secretory glands ▪ Stimulate sweat, lacrimal, nasopharyngeal glands Organ System Effects Central Nervous System ▪ Muscarinic receptors = ▪ role in cognition, learning ▪ hunger ▪ Nicotinic receptors = ▪ release of other transmitters (ex. glumatate, serotonin, GABA, etc) ▪ Chronic exposure can lead to desensitization and greater release of dopamine in the mesolimbic system Contributes to the mild alerting and addictive qualities of cigarette smoking Organ Response Eye Iris muscle (pupils) Contraction (miosis) Ciliary muscle Accomodation (near vision) Heart Organ Response Lungs Bronchial muscle constriction Bronchial glands stimulation GI Tract SA node rate (chrontropy) Motility Increase Atria inotropy Sphincters Relax AV node conduction velocity (dromotropy) Secretion Stimulation Ventricles Mild inotropy Blood vessels Salivary glands Dilation (EDRF) Constriciton (at very high doses) Stimulate Urinary bladder Detrusor muscle Trigone & sphincter Sweat glands Contract Relax Stimulate Act by inhibiting acetylcholinesterase = increasing or prolonging Ach activity on the synapse 3 groups Alcohols with quaternary ammonium group ▪ Edrophonium Carbamic acid esters with quaternary or tertiary ammonium groups ▪ Carbamates (Ex. neostigmine, pyridostigmine, physostigmine) Organic derivatives of phosphoric acid ▪ Organophosphates (ex. echothiophate) and thiophosphates (malathion) Pharmacokinetics Carbamates ▪ Generally hydrophilic, and therefore poor absorption in lungs and gut and skin Organophosphates ▪ Generally hydrophilic, but more lipid soluble than carbamates = better absorbed in skin, gut and lungs ▪ Potentially more dangerous to humans, but can kill more insects ▪ Relatively shorter half-life in the environment than carbamates Pharmacokinetics Thiophosphates ▪ More lipid soluble = better drug absorption ▪ Must be activated in the body to produce an effect ▪ Easily metabolized into inactive products among birds and mammals, but not in insects and fishes ▪ Makes it potentially more safe to humans. Pharmacodynamics MOA: Inhibits Ach-ase Alcohols ▪ Reversibly bind with Ach-ase, preventing binding with Ach. ▪ Effect is of short duration (5-15min) Carbamates ▪ Covalently bonds with Ach-ase. = longer duration (30min6hours) Organophosphates ▪ Phosphorylates with Ach-ase = extremely stable bond = (duration, ≥100hours) Uses Alcohols Edrophonium Carbamates Neostigmine Pyridostigmine Physostigmine Organophosphates Echothiophate Myasthenia gravis, ileus, arrythmias Approximate duration of action 1-15min Myasthenia gravis MG Glaucoma 0.5-2 hours 3-6 hours 0.5-2 hours Glaucoma 100 hours Organ System Effects CNS ▪ Produce mild alertness Eye, respiratory tract, GIT, urinary ▪ Similar to cholinergic drug effects Cardiovascular system ▪ Can increase activity on both para and sympa ganglia ▪ Heart = negative chronotropic, dromotropic and inotropic effects ▪ Blood vessels lack cholinergic innervation. sympathetic response vascular constriction increase in blood pressure ▪ NET effect = HR, CO, TPR = BP ▪ At toxic doses, there will be severe bradycardia = hypotension Organ System Effects Neuromuscular Junction (NMJ) ▪ At low doses = intensify action of Ach at the NMJ = increase muscular contractions. May help treat muscle weakness in myasthenia gravis ▪ Moderate doses = may produce fasciculations of the muscle unit (ex. tonic-like seizure) ▪ High doses = prolonged relaxation (neuromuscular depolarizing blockade, as in succinylcholine) Treatment for Diseases of the eye (Glaucoma) Gastrointestinal and urinary tract (motility problems, postoperative atony, neurogenic bladder) Neuromuscular junction (myasthenia gravis) Alzheimer’s disease Excess of parasympathetic effects Nausea, vomiting, diarrhea, urinary urgency, salivation, cutaneous vasodilation, bronchial constriction, seizures, coma, death Nicotine overdose Fatal dose is 40mg, or 1 drop of the pure liquid (in essence is the amount in 2 cigarettes) ▪ Destroyed by heat, and exhaled Chronic smoking = behavioral therapy, nicotine patch, nasal spray or inhaler ▪ New drug Varenicline = prevents release of dopamine in the thalamus = reduce the rewarding/addicting sensation ▪ Side effects = nausea, insomnia, anxiety, depression, suicidal ideation Pesticide/Insecticide overdose (organophosphates) “Muscarinic excess” = miosis, salivation, sweating, bronchial constriction, vomiting, diarrhea, convulsions, coma, muscle and respiratory depression Treatment = atropine Used during warfare = “nerve gas” Also called parasympatholytic Cholinoceptor antagonists Nicotinic antagonists ▪ Ganglion blockers = little clinical significance (because of its very broad effects) ▪ NMJ blockers = muscle relaxants Muscarinic antagonists ▪ Atropine = basic drug ▪ Synthetic drugs = developed for more specific and less toxic effects ▪ Tertiary = 3rd generation (pirenzepine, dicyclomine, trpicamide, benztropine) ▪ Quaternary = 4th generation (propantheline, glycopyrrolate, tiotropium) Atropine Found from the plant Atropa belladona (“deadly nightshade”) Generally well absorbed ▪ Tertiary drugs enter the CNS readily (more lipid soluble) ▪ Quaternary drugs less lipid soluble (less absorbed in the GUT and CNS) = more peripheral activity Elimination: 2 phases ▪ Rapid phase = t½ 2 hours ▪ Slow phase = t½ 13 hours ▪ Excreted mainly in the urine Atropine MOA = reversible blockade of cholinomimetic actions at muscarinic receptors (may be overcome by large doses of Ach) Inverse agonists = stop the muscarinic receptor from being active Organ System Effects CNS ▪ Mild CNS effect ▪ Treatment for tremors in Parkinson’s disease ▪ Due to relative excess of cholinergic activity (due to decreased dopamine activity in the brain) Eye ▪ Used by ophthalmologists to examine the eye ▪ Mydriasis (pupil dilation) Organ System Effects Cardiovascular ▪ Stimulates SA node = tachycardia ▪ Shortens AV node conduction = tachycardia ▪ Blood vessels have minimal innervations from parasympa = mild effect on BP ▪ NET effect = HR but normal BP Respiratory ▪ Mild bronchodilation and reduce bronchial secretions ▪ Useful during inhalational anesthetics Organ System Effects Gastrointestinal ▪ Decrease salivary, stomach and intestinal secretions ▪ Decreased peristalsis = prolonged GI time Genitourinary ▪ Relaxes urinary bladder = slows voiding Sweat glands ▪ Decreases sweating = may affect temperature regulation, called atropine fever Parkinson’s disease (in combination with dopamine drugs) Motion sickness Due to cholinergic activation of vestibular nerves (ear) Scopolamine best used to treat motion sickness For eye exam Preparation for pre-operative patients who will need inhalational anesthetics Asthma Ipratropium = bronchodilation and decreased secretions Reversing bradycardia Acute myocardial infarction and resuscitation Gastrointestinal Peptic ulcer disease, diarrhea Antidote for nerve gas and organophosphate poisoning and some types of mushroom poisoning Hyperhydrosis (excessive sweating) Symptoms: dry mouth, mydriasis, tachycardia, hot and flushed skin, agitation and delirium “dry as a bone, blind as a bat, red as a beet, mad as a hatter”