* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download A newborn mammal has no opportunity to develop protective
Survey
Document related concepts
Immune system wikipedia , lookup
Lymphopoiesis wikipedia , lookup
Psychoneuroimmunology wikipedia , lookup
Immunocontraception wikipedia , lookup
Anti-nuclear antibody wikipedia , lookup
Molecular mimicry wikipedia , lookup
Innate immune system wikipedia , lookup
Adaptive immune system wikipedia , lookup
Adoptive cell transfer wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
Polyclonal B cell response wikipedia , lookup
Transcript
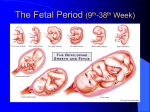
A newborn mammal has no opportunity to develop protective antibodies on its own, unless, as happens very rarely, it was infected while in the uterus. Yet it is born into an environment similar to its mother's, which contains all the potential microbial invaders to which she is exposed. Although the fetus possesses the components of innate immunity, it has few or none of its mother's lymphocytes. The placenta generally prevents the maternal lymphocytes from crossing into the uterus, where they would recognize the fetal tissues as foreign antigens and cause a reaction similar to the rejection of an incompatible organ transplant. What is transferred across the placenta in many species is a fair sample of the mother's antibodies. How this happens depends on the structure of the placenta, which varies among species. In humans maternal IgG antibodies—but not those of the other immunoglobulin classes—are transported across the placenta into the fetal bloodstream throughout the second two-thirds of pregnancy. In many rodents a similar transfer occurs, but primarily across the yolk sac. Maternal immunity, Passive immunity Immunity in a neonate provided by IgG antibodies from the mother passing across the placenta to the fetus; MI is immunoprotective for up to 6 month . Maternal antibody, an antibody transmitted from mother to fetus via the placenta. Such antibodies can provide immunity for the fetus and the newborn for up to 6 months after birth. They may also cause hemolytic anemia in newborns in cases of Rh or ABO blood group incompatibility between mother and child. Human colostrum is also rich in IgA, with the concentration highest immediately after birth. After a newborn has received its supply of maternal antibodies, it is as fully protected as its mother. This means, of course, that if the mother has not developed immunity to a particular pathogen, the newborn will likewise be unprotected. For this reason, a physician may recommend that a prospective mother receive immunizations against tetanus and certain other disorders. (The active immunization of pregnant women against certain viral diseases, such as rubella [German measles], must be avoided, however, because the immunizing agent can cross the placenta and produce severe fetal complications.) As important as the passively transferred maternal antibodies are, their effects are only temporary. The maternal antibodies in the blood become diluted as the animal grows; moreover, they gradually succumb to normal metabolic breakdown. Because the active development of acquired immunity is a slow and gradual process, young mammals actually become more susceptible to infection during their early stages of growth than they are immediately after birth. Occasionally the transfer of maternal antibodies during fetal life can have harmful consequences. A well-known example of this is erythroblastosis fetalis, or hemolytic disease of the newborn, a disorder in which maternal antibodies destroy the child's red blood cells during late pregnancy and shortly after birth. The most severe form of erythroblastosis fetalis is Rh hemolytic disease, which develops when: The fetus is Rh-positive; that is, its red blood cells carry an antigen known as the Rh factor. The mother is Rh-negative, which is to say her red blood cells lack the Rh factor. The mother's immune system has been previously activated against the Rh antigen; this usually is the result of exposure to fetal cells during the birth of an earlier Rh-positive baby or a transfusion of Rh-positive blood. Rh hemolytic disease can be prevented by giving the mother injections of anti-Rh antibody shortly after the birth of an Rhpositive child. This antibody destroys any Rh-positive fetal cells in the maternal circulation, thereby preventing the activation of the mother's immune system should she conceive another Rhpositive fetus. In addition to their importance in cooperating with B cells that secrete specific antibodies, T cells have important, separate roles in protecting against antigens that have escaped or bypassed antibody defenses. Immunologists have long recognized that antibodies do not necessarily protect against viral infections, because many viruses can spread directly from cell to cell and thus avoid encountering antibodies in the bloodstream. One major change that occurs as the body ages is a process termed "thymic involution." The thymus, located above the heart behind the breast bone, is the organ where T cells mature. Age-related changes in cell mediated immunity :1- As humans age, the thymus naturally atrophies. The volume of thymic tissue in a 60-year-old adult is less that 5% that of a newborn, and it is postulated that if humans lived to be more than 120, the thymus would disappear altogether. Although T cells are produced continuously throughout life, over time this progressive decay of the thymus causes a sharp decrease in the number and type of T cells produced. It is not known why the thymus deteriorates in this fashion. 2- A marked difference has been observed between young and old subjects in the subpopulations of naive and memory T cells. In newborns, the ratio of naive to memory T cells is quite high; in adults the ratio is reversed because most of the naive T cells have been exposed to antigen, and hence converted to memory cells. The elderly have almost no naive T cells at all, since as the thymus progressively deteriorates with age, fewer T cells are produced, and the naive T cell subpopulation is not replenished. 3- Another defect of T cell activation among the elderly is characterized by a decrease in calcium. Calcium is a vital element that is absolutely crucial for many biochemical reactions, including signal transduction. 4- Decreased amounts of calcium can also inhibit production of cytokines, proteins responsible for coordinating the interaction with antigen and amplifying the immune response. 5- Age-related genetic alterations occur within T cells as well. References :,Updated March 1999 , The Immunology of AgingDeborah B. Whitman 2012 Encyclopædia Britannica http://www.britannica.com/nobelprize/article-215587 Mosby's Medical Dictionary, 8th edition. McGraw-Hill Concise Dictionary of Modern Medicine. © 2002 by The McGraw-Hill Companies