* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Lec.2 Dr.Maysem M.Alwash Hypersensitivity Reaction s (cont.)
Anti-nuclear antibody wikipedia , lookup
Immunocontraception wikipedia , lookup
Lymphopoiesis wikipedia , lookup
Human leukocyte antigen wikipedia , lookup
Rheumatic fever wikipedia , lookup
Inflammation wikipedia , lookup
DNA vaccination wikipedia , lookup
Complement system wikipedia , lookup
Rheumatoid arthritis wikipedia , lookup
Monoclonal antibody wikipedia , lookup
Immune system wikipedia , lookup
Adaptive immune system wikipedia , lookup
Adoptive cell transfer wikipedia , lookup
Innate immune system wikipedia , lookup
Sjögren syndrome wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
Polyclonal B cell response wikipedia , lookup
Hygiene hypothesis wikipedia , lookup
Psychoneuroimmunology wikipedia , lookup
Immunosuppressive drug wikipedia , lookup
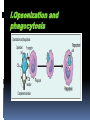
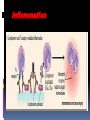
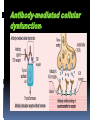
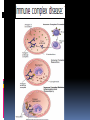
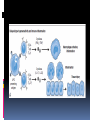
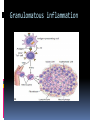
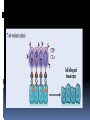
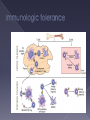
Hypersensitivity Reaction s (cont.): Lec.2 Dr.Maysem M.Alwash 2.Antibody-Mediated Diseases (Type II Hypersensitivity) is mediated by antibodies against endogenous antigens present on cell surfaces or in the extracellular matrix or adsorbed exogenous antigens (e.g., a drug metabolite). Subsequent pathology is a consequence of three mechanisms: i.Opsonization and phagocytosis ii.Inflammation ` iii. Antibody-mediated cellular dysfunction. i.Opsonization and phagocytosis Antibodies can coat (opsonize) cells, with or without complement proteins, and target these cells for phagocytosis by macrophages, . The result is depletion of the opsonized cells.e.g. Autoimmune hemolytic Anemia, Autoimmune thrombocytopenic purpura. i.Opsonization and phagocytosis ii. Inflammation Antibodies and immune complexes may deposit in tissues or blood vessels, and elicit an acute inflammatory reaction by activating complement, or by engaging Fc receptors of leukocytes. The inflammatory reaction causes tissue injury.e.g. Goodpasture syndrome and pemphigus vulgaris • Inflammation iii. Antibody-mediated cellular dysfunction. Antibodies can bind to cell surface receptors or essential molecules, and cause functional derangements either inhibition( e.g myasthenia Gravis), or unregulated activation( e.g. Graves disease ) without cell injury. Antibody-mediated cellular dysfunction. 3.Immune Complex Diseases (Type III Hypersensitivity): are caused by antibodies binding to antigens to form complexes that circulate and deposit in vascular beds and stimulate inflammation, typically as a consequence of complement activation. - The antigens in these complexes may be exogenous antigens, such as microbial proteins, or endogenous antigens, such as nucleoproteins Immune complex–mediated disease can be either systemic or local: A.Systemic Immune Complex Disease complexes are formed in the circulation and are deposited in several organs. E.g. -Acute serum sickness : inoculation of a large volume of exogenous antigen -Systemic lupus erythematosus. -polyarteritis nodosa (response to infectious agents) The pathogenesis of systemic immune complex disease can be divided into three phases: (1) formation of antigen– antibody complexes in the circulation . (2) deposition of the immune complexes in various tissues. (3) an inflammatory reaction in various sites throughout the body. - The antibody classes that induce such lesions are complement-fixing antibodies (i.e., IgG and IgM) .- Single large antigen exposures tend to induce acute, self-limited disease that resolves as the antigen is eliminated (e.g.,poststreptococcal glomerulonephritis) ; repeated or prolonged exposure leads to chronic, recurrent tissue injury (e.g.SLE ). -Histopathologic Lesions : Inflammation, necrotizing vasculitis (fibrinoid necrosis) B. Local Immune Complex Disease: -The complexes are formed and deposited in a specific site. Local immune complex disease is characterized by a localized tissue vasculitis and necrosis. A model of local immune complex diseases is the Arthus Reaction(Intracutaneous antigen injection in previously sensitized hosts carrying the appropriate circulating antibody). 4 . Cell–Mediated (Type IV) Hypersensitivity : T cell–mediated (type IV) hypersensitivity is mediated by antigen specific T lymphocytes and includes delayed-type hypersensitivity (CD4+ T) cells and T cell–mediated cytotoxicity (CD8+ T) cells. A-Reactions of CD4+ T cells : delayed-type hypersensitivity and immune inflammation : This response is largely mediated by helper CD4+ T cells and can be of two major types; responses associated with TH1 CD4+ T cells are predominated by macrophages, while those driven by TH 17 cells are characterized by a greater neutrophil infiltration. The classic delayed-type hypersensitivity (DTH) response is the tuberculin reaction to intracutaneous injection of purified protein derivative (PPD) derived from the tubercle bacillus. Prior tuberculosis infection results in circulating PPDresponsive memory CD4+T cells; subsequent PPD injection into such an individual leads to the recruitment and activation of these cells beginning at 6 to 8 hours and peaking at 24 to 72 hours (the delayed in DTH). Granulomatous inflammation occurs when persistent or nondegradable antigens (e.g., foreign bodies) lead to chronic macrophage activation manifesting as large epithelioid cells; nodules of these activated cells are called granulomas. Granulomatous inflammation Contact dermatitis; multiple sclerosis; type 1 diabetes; tuberculosis are examples of a DTH response B-Reactions of CD8+ T cells: cell-mediated cytotoxicity: Class I MHC molecules bind to intracellular peptide antigens and present the peptides to CD8+ T lymphocytes, stimulating the differentiation of these T cells into effector cells called cytotoxic T- cell( CTLs) . CTLs play a critical role in resistance to virus infections and some tumors and allograft rejection AUTOIMMUNE DISEASES Autoimmunity: Immune reactions to self antigens Autoimmune diseases range from those in which specific immune responses are directed against one particular organ or cell type and result in localized tissue damage, to multisystem diseases characterized by lesions in many organs and associated with multiple autoantibodies or T cell–mediated reactions against numerous self antigens. In many of the systemic diseases that are caused by immune complexes and autoantibodies, the lesions affect principally the connective tissue and blood vessels of the various organs involved. Therefore, these diseases are often referred to as “collagen vascular” or “connective tissue” disorders, even though the immunologic reactions are not specifically directed against constituents of connective tissue or blood vessels. Normal persons are unresponsive (tolerant) to their own (self) antigens, and autoimmunity results from a failure of self-tolerance. - Self tolerance: refers to a lack of immune responsiveness one’s own tissue antigens. Central Tolerance : This refers to the process by which T and B cells that recognize self antigens are either killed (negative selection) or rendered harmless during their maturation in central (generative) lymphoid organs (i.e., in the thymus for T cells and in the bone marrow for B cells). Peripheral Tolerance Self reactive cells that escape central regulatory mechanisms can be removed or inactivated in the periphery through one of the following pathways: 1.Anergy: This term refers to functional inactivation (rather than death) of lymphocytes induced by encounter with antigens under certain conditions. 2. suppression by regulatory T lymphocytes, 3. Activation-induced cell death ( apoptosis). Mechanisms of Autoimmunity: It is believed that the breakdown of self-tolerance and development of autoimmunity result from a combination of inherited susceptibility genes, which influence lymphocyte tolerance, and environmental factors, such as infections or tissue injury, that alter the display of self antigens -Autoimmune diseases have a tendency to run in families. -Several autoimmune diseases are linked with the HLA locus, especially class II alleles (HLA-DR, -DQ) e.g. - Rheumatoid arthritis and HLA DRB1 -Ankylosing spondylitis and HLA- B*27 -many genetic polymorphisms in ( non - HLA Genes) are associated with different autoimmune diseases. e.g. PTPN-22 gene and type I diabetes and rheumatoid arthritis. Microbes may induce autoimmune reactions by several mechanisms: -Viruses and other microbes may share cross-reacting epitopes with self antigens,This phenomenon is called molecular mimicry. . • Microbial infections with resultant tissue necrosis and inflammation can expose self-antigens and activate APCs and lymphocytes in the tissues. Autoimmune diseases are , more common in women than in men. Thank you