* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Accessary cells: in adaptive immunity are cells aid in the response
Survey
Document related concepts
Duffy antigen system wikipedia , lookup
DNA vaccination wikipedia , lookup
Immune system wikipedia , lookup
Lymphopoiesis wikipedia , lookup
Psychoneuroimmunology wikipedia , lookup
Monoclonal antibody wikipedia , lookup
Molecular mimicry wikipedia , lookup
Adaptive immune system wikipedia , lookup
Innate immune system wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
Immunosuppressive drug wikipedia , lookup
Transcript
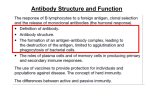
Accessary cells: in adaptive immunity are cells aid in the response but do not directly mediate specific antigen recognition; phagocytes, mast cells and natural killer cells (also called accessory effector cells) Acquired immune deficiency syndrome (AIDS): lost most of CD4 T cells due to virus infection Acute lymphoblastic leukemia: aggressive, undifferentiated form of lymphoid malignancy that is derived from a progenitor cell. Acute phase proteins: a series of proteins found in blood shortly after the onset of infection (eg, mannose-binding protein) Adaptive immune response (adaptive immunity): the response of antigen-specific lymphocytes to antigen, including the development of immunological memory. It is generated by clonal selection of lymphocytes (Acquired immune response) Adenosine deaminase deficiency: leads to the accumulation of toxic purine nucleosides and nucleotides, resulting in the death of most developing lymphocytes within the thymus, causing severe combined immunodeficiency Adhesion molecules: mediate the binding of one cell to other cells or to extracellular matrix proteins (integrins, selectins members of the immunoglobulin gene superfamily) Adjuvant: any substance that enhance the immune response to an antigen with which it is mixed. Adoptive immunity (adoptive transfer, adoptive immunization): immunity conferred on a naïve or irradiated recipient by transfer of lymphoid cells from an actively immunized donor Agglutination: clumping together of particles (eg. Antibody binding to antigens) Allelic exclusion: refers to the expression of immunoglobulin encoded by a single heavy-chain and a single light-chain immunoglobulin constant-region allele on the surface of B cells in heterozygous animals or people Allergens: antigens elicit hypersensitivity or allergic reaction Allergic asthma: constriction of the bronchial tree due to an allergic reaction to inhaled antigen Allergic reaction: a response to innocuous environment antigens or allergens due to pre-existing antibody or T cells (mostly the binding of allergen to IgE antibody on mast cells that causes asthma, hay fever, and others) Allergic rhinitis: an allergic reaction in the nasal mucosa (hay fever causes runny nose, sneezing and tears) Allergy: the symptomatic reaction to normal innocuous (non-toxic) environmental antigen. Results from interaction between antigen and antibody or T cells produced by earlier exposure to the same antigen Allogenic MHC molecules: Rejection of grafted tissues from unrelated donors usually results from T-cell responses to - - - expressed by the grafted tissues Anaphylactic shock (systematic anaphylaxis): allergic reaction to systemically administered antigen that causes circulatory collapse and suffocation due to tracheal swelling (binding of antigen to IgE antibody on connective tissue mast cells throughout the body, leading to the disseminated release of inflammatory mediators. Anergy: non-responsiveness to antigen Antibody: plasma proteins binding to antigens, neutralizing pathogens or prepare them for uptake and destruction by phagocytes (collectively called as Immunoglobulins) Antibody-dependent cell-mediated cytotoxicity (ADCC): Most ADCC is mediated by natural killer (NK) cells that have the Fc receptor FcRIII or CD16 on their surface Antibody repertoire: the total variety of antibodies that an individual can make Antigen: name arises from ability to Generate Antibodies. Immunogen: only those antigens that can induce antibody production (not bind to the antibody) Antigen:antibody complexes (immune complexes): non-covalently associated group Antigenic determinant (epitope): the portion of an antigenic molecule bound by a given antibody Antigenic drift (shift): point mutations of viral genes cause small differences in the structure of viral surface antigens. Influenza virus varies from year to year by this process, causing Antigenic variation (new antigens appeared and not recognized by antibody or T cells elicited in earlier infection Antigen presentation: display of antigen as peptide fragments bound to MHC molecules on the surface of a cell; T cells recognize antigen only when it is presented in this way Antigen processing: the degradation of proteins into peptides that can bind to MHC molecules for presentation to T cells Anti-immunoglobulin antibodies: antibodies to immunoglobulin constant domains, useful for detecting bound antibody molecules in immunoassays Antiserum (Antisera): the fluid component of clotted blood from an immune individual that contains antibodies against the molecule used for immunization. Aplastic anemia: a failure of bone marrow stem cells so that formation of all cellular elements of blood ceases; it can be treated by bone marrow transplantation Apoptosis (programmed cell death): a form of cell death in which the cell activates an internal death program (nuclear DNA degradation, nuclear degeneration and condensation, phagocytosis of cell residue) Arthus reaction: a skin reaction in which antigen is injected into the dermis and react with IgG Atopic allergy (atopy): a condition of increased susceptibility to immediate hypersensitivity usually mediated by IgE antibodies. Pathogens are said to be attenuated (weakened) when they will grow in their host and induce immunity without producing serious clinical diesea. Autograft: a graft of tissue from one site to another on the same individual Autoimmune response: an adaptive immune response directed at self antigens (eg. Autoimmune hemolytic anemia-red blood cell destruction; --thrombocytopenic purpura-platelet) B cells (B lymphocyte): B-1 B cell (CD5 B cell also called) and B-2 B cell (conventional B cell called), made up in the white pulp of spleen. B cell receptor (antigen receptor on B cell); Upon activation by antigen, B cells differentiate into cells producing antibody of same specificity as their initial receptor. Blood group antigens: surface molecules on RBC that are detectable with antibodies from other individuals. The major group antigens are called ABO and Rh (Rhesus). Incompatibility of cross-matching causes the destruction of RBC and releasing hemoglobin (toxicity). Bone marrow: the site of hematopoiesis, the generation of the cellular elements of blood; RBC, monocytes, polymorphonuclear leukocytes, and platelets. In addition, the site of B-cell development in mammals and the source of stem cells to give rise to T cells upon migration to the thymus. Booster immunization: is given after a primary immunization to increase the state of immunity. Bursa of Fabricius: an outpouching of the cloaca found in birds, aggregated epithelial tissue and lymphoid cells and the site of intense early B cell proliferation. It is required for B cell development in birds. An equivalent organ has not been detected in humans. Carriers: foreign proteins to which small, non-immunogenic antigen, or haptens, can be coupled to render the hapten immunogenic. Cell-mediated immunity (cell-mediated immune response): any adaptive immune resonse in which antigen specific T cells play the main role. It encompasses all adaptive immunity that can not be transferred to a naïve recipient with serum antibody, the definition of humoral immunity. Central lymphoid organs: sites of lymphocyte development. In humans, B lymphocytes development in bone marrow whereas T lymphocytes develop within the thymus from bone marrow derived progenitors. Chemokines: small cytokines that are involved in the migration and activation of phagocytic cells and lymphocytes. They play a central part in inflammation responses. Clonal selection theory: a central paradigm of adaptive immunity. It states that adaptive immune responses derive from individual antigen-specific lymphocytes that are self-tolerant. Clone: a population of cells all derived from a common progenitor. A cloned T-cell line is a continuously growing line of T cells derived from a single progenitor. Cloned T cell lines must be stimulated with antigen periodically to maintain growth. Clusters of differentiation (CD): groups of monoclonal antibodies that identify the same cellsurface molecule. The cell surface molecule is designated CD followed by a number (eg. CD1, CD2, etc.). Common lymphoid progenitors: stem cells which give rise to all lymphocytes. They derived from pluripotent hematopoietic stem cells Congenic strains of mice: genetically identical at all loci except one. Convertase: an enzymatic activity that converts a complement protein into its reactive form by cleaving it. Cyclophophamide and cyclosporin A: immunosuppressive drugs Cytokines: proteins made by cells that affect the behavior of other cells. Cytokines made by lymphocytes are often called lymphokines or interleukines (IL). Cytokines act on specific cytokine receptors on the cells they affect. Cytokine receptors signal via Janus kinases (JAK), tyrosine kinases that are activated by cytokine receptor aggregation. In, turns, these kinases phophorlate proteis known as STATs, for Signal Transducers and Activators of Transcription. These proteins are found in the cytosol normally, but move to the nucleus upon phosphorylation and activate a variety of genes. Cytotoxic T cells: T cells that can kill other cells (CD8 T cells generally). Host defense against cytosolic pathogens. Cytotoxins: proteins made by cytotoxic T cells (Perforins, granzymes or fragmentins). Delayed-type hypersensitivity: a form of cell-mediated immunity elicited by antigen in the skin. It is mediated by inflammatory CD4 T cells. Reaction appears hous to days after antigen is injected. Dendritic cells: also known as interdigitating reticular cells; found in T-cell arears of lymphoid tissues. Most potent stimulators of T-cell responses. Effector cells: lymphocytes that can mediate the removal of pathogens from the body without the need for further differentiation, as distinct from naïve lymphocytes, which must proliferate and differentiate before they can mediate effector functions, and memory cells which must differentiate and often proliferate before thay become effector cells. They are also called armed effector cells to indicate that they can be triggered to effector function by antigen binding alone. ELISA (enzyme-linked immunosorbent assay): serological assay in which bound antigen or antibody is detected by a linked enzyme that converts a colorless substrate into colored products. Embryonic stem (ES) cells: continuously growing cells that retain the ability to contribute to all lineages of cells in developing mouse embryos. ES cells can be genetically anipulated in tissue culture and then inserted into mouse blastocysts to generate mutant lines of mice; most often, genes are deleted in ES cells by homologous recombination and the mutant ES cells then used to generate gene knock-out mice. Endotoxin: bacterial toxins that are only released when the bacterial cell is damaged, as opposed to exotoxins which are secreted bacterial toxins. The most important endotoxin is lipopolysaccharide (LPS), a potent inducer of cytokine synthesis found in gram-negative bacteria. Epitope: a site on an antigen recognized by an antibody, also called antigenic determinants. Epstein-Barr virus (EBV): a hepes virus that selectively infects human B cells. Fas: another member of the TNF receptor gene family; it is expressed on certain target cells that are susceptible to killing by cells expressing the Fas ligand, a member of the TNFfamily of cytokines and cell surface molecules. Hapten: molecules that can bind antibody but cannot by themselves elicit an adaptive immune response. Haptens must be chemically linked to protein carriers to elicit antibody and T cell responses. Hemagglutinin: any substance that causes RBC to agglutinate. Hematopoiesis: generation of the cellular elements of blood (RBC, leukocytes, platelets). Histamine: a vasoactive amine stored in mast cell granules. Released by antigen binding to IgE on mast cells causes dilation of local blood vessels and smooth muscle contraction, producing some of the symptoms of immediate hypersensitivity reactions. Antihistamines are drugs that counter histamine actions. Immunoglobulins: IgM, IgG, IgD, IgA and IgE. Inducible NO synthase (iNOS): macrophage and many other cells have this enzyme. INOS is induced by many different stimuli to activate NO synthesis. A major mechanism of host resistance to intracellular infection in mice and probably in humans as well. Inflammation: a general term for the local accumulation of fluid, plasma proteins, and WBC that is initiated by physical injury, infection, or a local immune response. Inflammatory CD4 T cells (TH1): armed effector T cells that make the cytokines interferon-, and TNF upon recognition of antigen. The major function is the activation of macrophages. Interferons: IFN-, IFN- are produced by leukocytes and fibroblasts, respectively. IFN- is a product of inflammatory CD4 T cells, CD8T cells, and natural killer cells. Interleukin (IL): a generic term of cytokines produced by leukocytes. More general term is Cytokine. Kupffer cells: phagocytes lining the hepatic sinusoids. They remove debris and dying cells from the blood, but are not known to elicit immune responses. Langerhans’ cells: phagocytic dendritic cells found in the epidermis. Leukocyte: WBC Leukocytosis: In acute infection, increased number of leukocytes. Lymphatic system: the system of lymphoid channels that drains fluid from the periphery via the thoracic duct to the blood, including the lymph nodes, Peyers patches, and other organized lymphoid elements apart from the spleen, which communicates directly with the blood. Lymphatic vessels (lymphatics): thin-walled vessels that carry lymph, the extracellular fluid that accumulates in tissues, back through the lymph nodes to the thoracic duct. Lymph node: secondary lymphoid organs where adaptive immune responses are initiated. Lymphoblast: lymphocyte that has enlarged and increased its rate of RNA and protein syntheses. Lymphoid organs: thymus and bone marrow. The secondary ones lymph nodes, spleen, and mucosal-associated lymphoid tissues (tonsils, and Peyer’s patch) where adaptive immune responses initiatied. Lymphotoxin (LT, TNF-): a cytokine secreted by inflammatory CD4 T cells, and cytotoxic to some cells. Lymphotoxin (LT, TNF-): cytokine secreted by inflammatory CD4T cells, which is directly cytotoxic for some cells. Macroglobulin: high molecular weight globulin like IgM. Macrophage: large mononuclear phagocytic cells in early non-adaptive phases of host defense. They are migratory cells deriving from bone marrow precursors and are found in most tissues of the body. Resting macrophage does not destroy intracellular bacteria unless the macrophage is activated by a T cell. Macrophage chemoattractant and activating protein is a chemokine. Major Histocompatibility Complex (MHC): a cluster of genes on human chromosome 6 or mouse chromosom 7 that encode the MHC molecules. Class I and –II are available. Mast cell: large cells found in connective tissues throughout the body. Most abundantly in the submucosal tissues and the dermis. They contain large granules that store a variety of mediator molecules including the vasoactive amine histamine. Mast cell play a crucial role in allergic reactions. Monoclonal antibodies: antibodies produced by a single clone of B lymphocytes. Monocytes: WBC with a bean-shaped, a precursor to macrophages. Mucin: highly glycosylated cell-surface proteins. Mucin-like molecules are bound by L-selectin in lymphocyte stimulatory loci. Multiple sclerosis: a neurological disease characterized by focal demyelination in the CNS, lymphatic infiltration into brain. An autoimmune disease. Myelopoiesis: production of monocytes and polymorphonuclear leukocytes in bone marrow. Naïve lymphocytes: lymphocytes that have never encountered their specific antigen and thus have never responded to it, as distinct from memory or effector lymphocytes. All lymphocytes leaving the central lymphoid organs are naïve lymphocytes, those from the thymus being naïve T cells and those from bone marrow being naïve B cells. Natural Killer cells (NK cells): non-T, and non-B lymphocytes, usually having granular morphology, that kill certain tumor cells. Necrosis: the death of cells or tissues due to chemical and physical injury, as opposed to apoptosis, which is a biologically programmed form of cell death. Neutralize: antibody inhibits the infectivity of virus or toxicity of a toxin. Neutrophils (neutrophilic polymorphonuclear leukocytes): a major class of WBC in human peripheral blood. Phagocytes. Opsonization: the alteration of the surface of a pathogen or other particle so that it can be ingested by phagocytes. Antibody and complement opsonize extracellular bacteria for destruction by neutrophils and macrophages. Pathogenic microorganisms (pathogens): infective microorganisms. Pentadecacatechol: natural substance derived from poisonous ivy plant leave, causes the cell mediated immunity associated with allergy to poison ivy. Peripheral blood mononuclear cells: lymphocytes and monocytes isolated from peripheral blood. Peripheral lymphoid organs: lymph nodes, spleen, and mucosal-associated lymphoid tissue where immune responses are induced, as opposed to the central lymphoid organs where lymphocytes develop. Peyer’s patch: aggregates of lymphocytes along the small intestine, especially the ileum. Phagocytic cells (phagocytes): macrophages or neutrophils. Phospholipase C-: a key enzyme in signal transduction, activated by protein tyrosine kinase. It cleaves inositol phopholipid into insitol triphosphate and diacylglycerol. Plasma: the fluid component of blood containing water, electrolytes, and the plasma proteins. Plasmablast: a B cell in a lymph node. Plasma cells: terminally differentiated B lymphocytes. The main antibody-secreting cells of the body. They are found in the medulla of the lymph nodes, in splenic red pulp, and bone marrow. Malignant plasma cells form multiple tumors in bone marrow and are called multiple myeloma. Platelets: small cell fragments, and crucial for blood clotting, and derived from megakaryocytes. Polymerase chain reaction (PCR): amplifying a specific sequence in DNA (by pairs of reciprocally oriented primers). Polymorphism: literally means existing in a variety of different shapes. Genetic - - - is variability at a gene locus where the variants occur at a frequency of greater than 1 %. Polymorphonuclear leukocytes: WBC with multi-lobed nuclei and cytoplasmic granules. There are 3 types of - - - leukocytes, the neutrophils, the eosinophils, basophils. Primary immune response: the adaptive immune response to an initial exposure to antigen. Primary immunization, also known as priming, generates both the primary immune response and immunological memory. Professional antigen-presenting cells (APCs): cells that normally initiate the response of naïve T cells to antigen. Only dendritic cells, macrophages, and B cells have this capacity. Progenitors: more differentiated progeny of stem cells that give rise to distinct subsets of mature blood cells and tht lack the self-renewal capacity of true stem cells. Proto-oncogenes: cellular genes that regulate growth control. When mutated or aberrantly expressed, they can contribute to malignant transformation of cells leading to cancer. Provirus: the DNA form of retrovirus when it is integrated into the host cell genome, it can remain transcriptionally inactive for a long period of time. Radioimmunoassay (RIA): antigen or antibody is labeled with radioactivity. An unlabeled antigen or antibody is attached to a solid support like a plastic surface, and the fraction of the labeled antibody or antigen retained on the surface is determined in order to measure binding. Recombination activating genes: RAG-1 and RAG-2 encode the proteins of RAG-1 and –2 that are critical to receptor gene rearrangement. Rapamycin: an immunosuppressive drug, blocks cytokine action. Recessive lethal gene: a gene that is needed for the human or animal to develop to adulthood; when both copies are defective, the human or animal dies in utero or early after birth. Recombination signal sequences (RSS): short stretches of DNA that flank the gene segments that are rearranged to generate a V-region exon. Reverse transcriptase: an essential component of retroviruses, as it translates of the RNA genome into DNA prior to its integration into host cell DNA. CDNA (complementary DNA) is formed by this enzymatic action. Rhesus (Rh blood group antigen): a RBC membrane antigen, is also detectable on the cells of rhesus monkeys. Rheumatoid arthritis: a common inflammatory joint disease that is probably due to an autoimmune response, accompanied by the production of rheumatoid factor, an IgM antiIgG antibody that may also be produced in normal immune response. SDS-PAGE: the common abbreviation for polyacrylamide gel electrophoresis of proteins dissolved in the detergent sodium dodecyl sulfate. This is widely used to characterize protein sizes. Sepsis: infection of the bloodstream. Infection of the blood with Gram-negative bacteria triggers septic shock through the release of the cytokine TNF-. Spleen: red pulp-removing senescent blood cells and a white pulp of lymphoid cells TNF-: tumor necrosis factor, a cytokine that is produced by macrophages and T cells and which has multiple functions in the immune response. TNF- is called lymphotoxin. Transgenesis: foreign genes can be placed in the mouse genome by this mean. This generates transgenic mice. Tyrosine kinase: an enzyme specifically phosphorylates tyrosine residue in proteins. It is critical in T- and B-cell activation. Vesicles: small membrane-bounded compartments within the cytosol. Virion; virus particles, Viruses. Western blotting: detecting proteins in a mixture using labeled antibodies, after the proteins have been separated, usually by gel electrophoresis, and transferred by blotting to nitrocellulose.