* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download The Immune System - Hatzalah of Miami-Dade
Survey
Document related concepts
Rheumatic fever wikipedia , lookup
Inflammation wikipedia , lookup
Lymphopoiesis wikipedia , lookup
DNA vaccination wikipedia , lookup
Rheumatoid arthritis wikipedia , lookup
Monoclonal antibody wikipedia , lookup
Immune system wikipedia , lookup
Molecular mimicry wikipedia , lookup
Adaptive immune system wikipedia , lookup
Adoptive cell transfer wikipedia , lookup
Autoimmunity wikipedia , lookup
Polyclonal B cell response wikipedia , lookup
Sjögren syndrome wikipedia , lookup
Hygiene hypothesis wikipedia , lookup
Innate immune system wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
Transcript
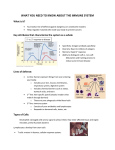
Disorders of the Immune System Disorders of Immune System • Defenses against infection • Immune system disorders – Autoimmune diseases – Immunodeficiency Defenses Against Infection • Barriers (non-specific) – Skin – Mechanical removal (coughing, vomiting, diarrhea, skin sloughing) – Normal flora – Antimicrobial secretions • Inflammation (non-specific) • Immunity (specific) Immune Response • • • • Natural vs. Acquired Active vs. Passive Primary vs. Secondary Humoral vs. Cell-Mediated Humoral Immunity • B Lymphocytes (Plasma Cells) – Produced in bone marrow – Make antibodies (immunoglobulins) Antibodies • Protein molecules produced by B-cells • Specific shapes allow binding to specific molecules (antigens) • Allow body to respond defensively to presence of specific potential threats Antibody Types • • • • • IgG IgM IgA IgD IgE IgG • Most common antibody type • Only antibody that crosses placenta • Prime mediator of secondary immune response • Principal defender against bacteria, viruses, and toxins IgM • Macroglobulin • Confined to bloodstream • First antibody to appear in response to presence of antigen • Agent of primary immune response IgA • Secretory antibody • Found in saliva, tears, respiratory secretions, GI tract secretions • Frontline bacterial, viral defense IgD • • • • Role not fully understood Low serum levels High concentrations on B-cells May act as receptors that trigger production of other antibodies IgE • • • • Very low serum levels Primarily bound to mast cells in tissues Controls allergic response Prevents parasitic infections Antigen-antibody binding initiates reactions that: • • • • Neutralize bacterial toxins Neutralize viruses Promote phagocytosis Activate components of inflammatory response Cell-Mediated Immunity • T Lymphocytes – Originate in bone marrow – Altered by passage through thymus – Responsible for mediation of cellular immunity T Lymphocyte Types • • • • Helper cells (T4 cells) Cytotoxic cells (Killer T cells) Suppressor cells Memory cells Helper T-Cells • Master “on-switch” of immune system • Recognize antigens • Secrete lymphokines that activate all other immune system cells • Stimulate B-cells to begin antibody production Cytotoxic (Killer) T-Cells • Respond to presence of antigens and lymphokines produced by T-4 cells • Seek out, bind to, and destroy: – Cells infected by viruses – Some tumor cells – Cells of tissue transplants • Can deliver lethal hits on multiple cells in sequence Suppressor T-Cells • Produce lymphokines that inhibit proliferation of B and T cells • Downregulate or dampen immune response Memory T-Cells • Have previously encountered specific antigens • Respond in enhanced fashion on subsequent exposures • Induce secondary immune response Inflammation • Occurs in vascularized tissue • Nonspecific response to injury • Response is same regardless of agent that initiates it Inflammation: Physiology • Triggered by cellular injury • Injury activates mast cells • Mast cells release chemical mediators: – – – – Histamine Heparin Leukotrienes (SRS-A) Eosinophil chemotactic factor Inflammation: Pathology • Mediators cause: – Vasodilation (redness, heat) – Vascular permeability (swelling) – White cell movement to and infiltration of affected area (pus) – Nerve ending stimulation (pain) “Dolor, Calor, Tumor, Rubor” Inflammation: Purposes • Confines injurious agents • Increases blood cell, plasma movement to injured areas • Enhances immune response • Destroys injurious agents • Promotes healing Inflammation: Cellular Components • Neutrophils – – – – Phagocytic cells Engulf foreign material/organisms Arrive early Short-lived Inflammation: Cellular Components • Macrophages – – – – – – Phagocytic cells Engulf foreign material/organisms Arrive later Long-lived Transfer antigens back to T4 cells Help initiate immune response to specific agents Inflammation: Cellular Components • Eosinophils – Secrete caustic proteins – Dissolve surface membranes of parasites Disorders of Immunity Autoimmune Disease • Clinical disorder produced by an immune response to a normal tissue component of a patient’s body Autoimmune Diseases • • • • • • Hyperthyroidism Primary myxedema Type I diabetes Addison’s disease Multiple sclerosis Myasthenia gravis Autoimmune Diseases • • • • • Rheumatic fever Crohn’s disease Ulcerative colitis Rheumatoid arthritis Systemic lupus erythematosis Systemic Lupus Erythematosis • • • • • Primarily occurs in 20- to 40-year old females Also in children and older adults 90% of patients are female Autoimmune reaction to host DNA Mortality after diagnosis averages 5% per year Systemic Lupus Erythematosis • Signs/Symptoms – Facial rash/skin rash triggered by sunlight exposure – Oral/nasopharyngeal ulcers – Fever – Arthritis Systemic Lupus Erythematosis • Signs/Symptoms – Serositis (pleurisy, pericarditis) – Renal injury/failure – CNS involvement with seizures/psychosis – Peripheral vasculitis/gangrene – Hemolytic anemia Systemic Lupus Erythematosis • Chronic management – Anti-inflammatory drugs • Aspirin • Ibuprofen • Corticosteroids – Avoidance of emotional stress, physical fatigue, excessive sun exposure Disorders of Immunity Immunodeficiency Diseases Immunodeficiency Diseases • Congenital • Acquired Immunodeficiency Diseases: Congenital • B cell deficiency – Agammaglobulinemia – Hypogammaglobulinemia Immunodeficiency Diseases: Congenital • T cell deficiency • IgA deficiency • Severe combined immune deficiency syndrome (B and T cell deficiency) Immunodeficiency Diseases: Acquired • • • • • Nutritional deficiency Iatrogenic (drugs, radiation) Trauma (prolonged hypoperfusion) Stress Infection (AIDS)