* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Bronchial Asthma: Pathophysiologic Concepts
Psychedelic therapy wikipedia , lookup
Discovery and development of angiotensin receptor blockers wikipedia , lookup
Polysubstance dependence wikipedia , lookup
Discovery and development of beta-blockers wikipedia , lookup
Pharmacokinetics wikipedia , lookup
NMDA receptor wikipedia , lookup
Drug design wikipedia , lookup
Toxicodynamics wikipedia , lookup
Pharmacognosy wikipedia , lookup
NK1 receptor antagonist wikipedia , lookup
5-HT2C receptor agonist wikipedia , lookup
Drug discovery wikipedia , lookup
Prescription drug prices in the United States wikipedia , lookup
Pharmacogenomics wikipedia , lookup
Pharmaceutical industry wikipedia , lookup
Prescription costs wikipedia , lookup
Cannabinoid receptor antagonist wikipedia , lookup
Drug interaction wikipedia , lookup
Nicotinic agonist wikipedia , lookup
Psychopharmacology wikipedia , lookup
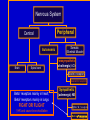
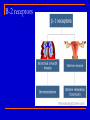
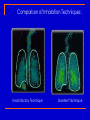
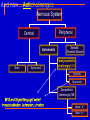
Pulmonary Disorders Pharmacologic Interventions Wanda Lovitz, APRN Obstructive Pulmonary Disease An “Umbrella Term” Asthma Emphysema Chronic Bronchitis GENERIC NAME albuterol TRADE NAME Proventil ROUTE CLASSIFICATION Short-term beta² agonist SABA Inhaled Q4-6H (bronchodilator) salmeterol Serevent diskus Long-acting beta² agonist LABA Inhaled Q12H (bronchodilator) ipratropium Atrovent Anti-cholingergic Short acting anti-cholingergic Inhaled Q4-6H tiotropium Spiriva Anti-cholingeric Long acting anti-cholingergic Inhaled once daily theophylline Theodur Methylxanthine (brochodilator) PO beclomethasone Beclovent Glucocorticoid (steroid) Inhaled Q4-6H triamincolone Azmacort Glucocorticord (steroid) Inhaled Q4-6H prednisone Prednisone Glucocorticoid (steroid) PO varying dose sc fluticasone AND salmeterol Advair Corticosteroid + a LABA) Inhaled BID *NOT a rescue inh *INDICATED for Asth montelukast Singulair (children) Leukotriene modifier PO daily Leukotriene modifier Inhaled Obstructive Pulmonary Disease: Pharmacology Two 1. 2. Major Groups of Drugs Bronchodilators PREVENT/TREAT bronchoconstriction Anti-inflammatory agents PREVENT/TREAT inflammation ↓ inflammation will ALSO ↓ bronchoconstriction by: ↓ mucosal edema ↓ mucous secretion ↓ hyper-reactivity to various stimuli Nervous System Peripheral Central Autonomic Brain Spinal cord Somatic (Skeletal Muscle) Parasympathetic (cholinergic) ACh Nicotinic receptors Muscarinic receptors Beta¹ receptors mainly in heart; Beta² receptors mainly in lungs FIGHT OR FLIGHT ↑ HR and cause bronchodilation Sympathetic (adrenergic) NE Alpha ¹ & ² receptors Beta ¹ & ² receptors Question: If you were giving BOTH a bronchodilator and an antiinflammatory to the client, which would you give first? What is a “beta agonist”??? Beta agonists are SYMPATHOMIMETIC drugs They “mimic” the action of the SNS ”fight or flight” Bronchodilation Beta Agonist Turn the SNS ON!! Ideally have“SELECTIVE” activation of beta2-adrengeric receptors B2 agonist activate receptors in smooth muscle of the lungs B2 agonist also: suppress the release of histamine increase ciliary motility Pharmacodynamics: Receptors Receptor Theory of Drug Action RECEPTORS are PROTEINS located on surfaces of cell membranes Are special CHEMICALS in the body that drugs interact with to produce effects (hormones, neurotransmitter, other molecules) When drug molecules bind with receptor molecules → result in a →INITIATES DRUG-RECEPTOR COMPLEX which physiochemical reactions that STIMULATE/activate OR INHIBIT normal cellular function agonistic (stimulates) antagonistic (inhibits) Receptor – “ON” or “OFF” Drug binds to a receptor and either The light switch is either “ON” or it is “OFF” • MIMICS or BLOCKS the normal physiological activity controlled by the receptor Receptor Theory of Drug Action: Antagonist Antagonist A drug that produces its action not by stimulating receptors but by PREVENTING OTHER, natural substances from stimulating receptors Examples: ranitidine (Zantac) = H² ANTAGONISTBLOCKS release of gastric acid diphenhydramine (Benadryl) = H¹ ANTAGONIST- BLOCKS action of histamine propranolol (Inderal) = beta¹ adrenergic ANTAGONIST – BLOCKS action of epinephrine Adrenergic/Sympathetic Beta Receptors Beta receptors are a type of adrenergic receptor B1 receptors mostly in heart and kidney activation causes increase in HR and and increase release of renin (↑ B/P) B2 receptors mostly in lungs and uterus Inderal – beta 1 receptor antagonist – blocks actions of epinephrine activation causes BRONCHODILATION and uterine relaxation B3 receptors mostly in adipose tissue Activation of beta receptors triggers an adrenergic response or MIMICS the SNS think ‘fight or flight” ADRENERGIC uses ADRENALIN increased in HR and force, vasodilation of lungs, smooth muscle contraction….body is ready to FLEE! Autonomic Nervous System Which one dominates? B-2 receptors Bronchodilators: Classifications 1. Beta-agonists 2. Anti-cholinergics 3. Methylxanthines Beta-agonists: 3 Classifications Other names: ADRENERGIC agents or SYMPATHOMIMETICS: mimic SNS Nonselective ADRENERGIC (Stimulate alpha, beta¹ & beta²) Nonselective BETA-ADRENERGIC drugs drugs (Stimulate beta¹ & beta²) Selective BETA drugs (Stimulate ONLY beta² receptors) Cause relaxation of bronchioles For a beta-agonist to dilate the airways of lungs, it must stimulate beta²-adrenergic receptors located throughout the lungs Beta-agonists (remember agonists enhance the response) MOA: If stimulate beta¹ receptors: (these receptors are located mostly in the heart) ↑ rate/force of ventricular contraction (may be an adverse effect when given for bronchodilation) If stimulate alpha receptors (mostly in heart): ↑ vasoconstriction (what we do not want!) If stimulate beta²-adrenergic receptors (mostly in lungs): RELAXATION OF SMOOTH MUSCLE IN BRONCHI/BRONCHIOLES Beta Agonists: Methods of deliver Orally – not used as often Most often by INHALATION MDI (metered dose inhaler) DPI (dry powder inhaler) Nebulizer (med in a solution and delivered with high flow oxygen to make a mist) Short acting vs long acting inhalation Most inhaled B2 agonist are short-acting (SABA) Duration =Q4-6H A commonly RX ‘LONG ACTING INHALED B2 AGONIST’ (LABA): Salmetrol /Serevent Diskus Duration – 12H Can you identify these? Comparison of Inhalation Techniques: Unsatisfactory Technique Excellent Technique Beta-agonists Indications for Use: Treatment of bronchial asthma, bronchitis, emphysema Adverse Effects: SELECTIVE beta² agonists → ALPHA-BETA agonists → MOST ADVERSE EFFECTS- because they are NONSELECTIVELY stimulating cardiacreceptors as well as lung receptors Minimal; tremors Insomnia, restlessness, anorexia, CARDIAC STIMULATION, tremor, vascular headache Nonselective beta-agonists → limited to beta-adrenergic effects/cardiac constriction effects CARDIAC STIMULATION, tremor, ANGINAL PAIN, vascular headache We like the SELECTIVE BETA 2 AGONISTS they work where we want them to work for COPD……the LUNGS!! Beta-agonists: Common Drugs albuterol /Proventil ** Short-acting beta² agonist (SABA): onset minutes Inhalation RESCUE DRUG! Delivery method: MDI or nebulizer → FIRST LINE of treatment for acute asthma attack! PO → Proventil Repetabs; Proventil Syrup used for long-term moderate to severe asthma; not to be used for exacerbations albuterol/Proventil Inhaler: Treatment Of Choice For ACUTE Asthma Attack Proventil is a RESCUE drug! Use of more than one canister per month indicates inadequate control of asthma & need for initiating or intensifying anti-inflammatory therapy 200 ACTUATIONS per cannister Regularly scheduled daily use is NOT recommended * Also for PREVENTION of EIA (exercise induced asthma) And now....Anticholinergics Nervous System Peripheral Central Autonomic Brain Spinal cord Somatic (Skeletal Muscle) Parasympathetic (cholinergic) ACh Nicotinic Muscarinic REST and Digest-things get ‘wetter’ increase salivation, lacrimation, urination Sympathetic (adrenergic) NE Alpha ¹ & ² Beta ¹ & ² Parasymphathetic Cholinergic Receptors Cholinergic receptors- certain type of cells that respond to a specific neurotransmitter called acetylcholine Due to their location and reaction to acetylcholine, the cholinergic receptors control responses that occur in the heart, intestine, prostate, bladder Giving ANTI-cholinergic agents results in Turning off cholinergic response (PNS) and turning on SNS SNS dominates = bronchodilation Thus increasing perfusion to heart, lungs, and brain Lungs Heart Anticholinergics are also used to treat OPD Action is also BRONCHODILATION, but by a different mechanism than the Beta Blockers Eye Action Sites of Anti-cholinergics Exocrine glands Bladder GI tract Anti-cholinergics: Side Effects Blockade of cholinergic receptors Anti-cholinergic Effect “Can’t see, can’t pee, can’t spit, can’t poop!” Anti-cholinergics (anti = blocking of the receptors: antagonist drugs) MOA: Blocks the action of ACETYLCHOLINE in bronchial smooth muscle when given by inhalation → keeps those MUSCLES around the large airways from tightening = BRONCHODILATION but by a different mechanism than Beta blockers which works on the BRONCHIOLES. Indications for Use: Used prophylactically/maintenance of emphysema & bronchitis Action is SLOW and PROLONGED NOT a RESCUE inhaler Treatment of asthma (off label) Anti-cholinergics ADVERSE EFFECTS: Dry mouth, visual difficulities,GI distress, constipation,urinary retention, anxiety d/t blocking those cholinergic receptors COMMON DRUGS: Works SYNERGISTICALLY with beta agonists may be given concomitantly (1+1=3) Combivent (inhalation) also known as Duoneb Atrovent ** (qid) ipratropium bromide / A product that contains both albuterol & ipratropium tiotropium bromide (SPIRIVA) (Feb, 2004)* First once-daily maintenance therapy for COPD ** Prototype And finally......Methylxanthines MOA: Bronchodilation 2 smooth muscle relaxation Also stimulate CNS & CVS (esp. heart) Indications for Use: SECOND-LINE agent may be added in severe OPD (all 3) ADVERSE EFFECTS: TOXICITY: N/V/D, insomnia, H/A, tachycardia, dysrrhythmias, seizures (especially in elderly) Methylxanthines Common Drugs: theophylline TheoDur, ** PO, IV or rectal Take with food Caffeine may ↑ side effects Smoking → ↓ absorption NARROW THERAPEUTIC INDEX DRUG! Maintain serum level 5-15 mcg/ml **PROTOTYPE Anti-inflammatory Agents: Classifications Corticosteroids/Glucocorticoids Leukotriene Modifiers Mast cell stabilizers Effect of Cortisol on the Body NATURAL CORTISOL has important effects in the body, including regulation of: Protein, carbohydrate, lipid and nucleic acid metabolism Inflammation and immune response Distribution and excretion of water and solutes Secretion of adrenocorticotrophic hormone (ACTH) from the pituitary gland. Corticosteroids Most potent & effective antiinflammatory medication currently available INDICATION: as prophylaxis NOT used to gain immediate control of an ongoing acute attack Corticosteroids MOA: (anti-inflammatory action) 1. SUPPRESS INFLAMMATION in airways by: ↓ movement of fluid/protein into tissues ↓ migration/function of neutrophils/eosinophils ↓ synthesis of histamine in mast cells ↓ production of pro-inflammatory substances 2. ↑ NUMBER/SENSITIVITY of beta² adrenergic RECEPTORS to bronchodilators Corticosteroids: methods of delivery SYSTEMIC STEROIDS work in the same way as natural cortisol, and are prescribed for a large number of serious diseases They are called "SYSTEMIC" steroids if taken by mouth or given by injection as opposed to TOPICAL CORTICOSTEROIDS which are applied directly to INHALED CORTICOSTEROIDS which are inhaled via a the skin or nebulizer or MDI Corticosteroids Indications for Use: INHALED form: CORNERSTONE OF ASTHMA THERAPY (long-term control) (Not typically indicated for tx of COPD) Advantage → limited to topical site of action → the lungs SYSTEMIC (IV or PO) form: Used to gain prompt control of asthma when initiating long-term therapy Early stages of COPD → unlikely to need; however, may need short-course therapy for episodes of respiratory distress (PO/IV) End-stage COPD → often become “steroid-dependent” Corticosteroids: Asthma Used regularly to prevent symptoms, i.e. as “PREVENTOR drug” (even if asymptomatic) Used for maintenance therapy (not acute attacks) ADVERSE EFFECTS: Inhalation Limited 2 route (sore throat, dry mouth, infection) Teach client to rinse mouth after each administration to ↓ potential for fungal infections (ie, candidiasis*) of the mouth Use of SPACER also decreases med deposit in mouth Corticosteroids Common Drugs: Inhalation (Meter-Dose Inhaler) ( beclomethasone dipropionate Beclovent triamcinolone acetonide (Azmacort) ) ** SYSTEMIC (PO/IV) prednisone (Prednisone) hydrocortisone (Solu-Cortef) methylprednisolone (Solu-Medrol) Take with food Follow dosing schedule exactly 3-10 day course of treatment (Lehne – “acute” use) PROTOTYPE ** Most common SE of inhaled corticosteroids Oropharyngeal candidiasis “thrush” Prevention: Rinse and spit Treatment: Anti-fungal agent Systemic Steroids: Short term vs Long term Treatment for less than ONE MONTH is considered SHORT TERM treatment Majority of SE seen with LONG TERM SYSTEMIC steroids Steroid treatment continuing for more than 3 MONTHS is regarded as LONG TERM SIDE EFFECTS OF SYSTEMIC CORTICOSTERIODS (will be in covered in more detail in the stress lecture Skin problems (infection, easy bruisng, thinning, acne) Sleep disturbance Increased appetite Weight gain Psychological effects, including ACUTE PARONIA INCREASED OR DECREASED ENERGY Reduction of your own cortisol production Osteoporosis (thinning of the bones) Redistribution of body fat:(moon face, buffalo hump, truncal obesity = CUSHING’S SYNDROME Increased suseptibility to internal infections (TB) Peptic Ulcers Combination Drug: ADVAIR Advair – Diskus and MDI Is a combination of fluticasone (corticosteroid) AND salmeterol (LABA) Caution: BLACK BOX WARNING! Indication: Is a PREVENTOR DRUG Approved for treatment of asthma in patients 4 years and older. NOT approved for emphysema and bronchitis IS NOT A RESUCE DRUG! Indicated for MODERATE TO SEVERE ASTHMA Advair: Black Box Warning WARNING: ASTHMA-RELATED DEATH Long-acting beta2-adrenergic agonists (LABAs), such as salmeterol, one of the active ingredients in ADVAIR HFA, increase the risk of asthma-related death. Should only be prescribed for moderate to severe asthma. Patient teaching a MUST! Not a rescue drug Leukotriene Modifiers Fairly new class of asthma medication; first in over 20 years Leukotrienes Cause inflammation, bronchoconstriction, & mucous production MOA of leukotriene modifiers: Anti-inflammatory action PREVENTS leukotrienes from attaching to receptors (block inflammation) by: (1) inhibiting enzymes (2) inhibiting proteins or (3) blocking receptors Leukotriene Modifiers INDICATIONS FOR USE: PREVENTOR DRUG: Oral prophylaxis & chronic treatment of asthma in adults & children 6 years old NOT MEANT FOR ACUTE ASTHMA ATTACKS!! ADVERSE EFFECTS: Headache, dyspepsia, nausea, dizziness, insomnia Leukotriene Modifiers Common drugs (oral): zafirlukast /Accolate** - for adults montelukast/ Singulair** – once daily dose for children Improvement seen ≈ 1 week **PROTOTYPE Mast Cell Stabilizers Common drugs: cromolyn (Intal)** – first agent developed MOA: (anti-inflammatory action) Stabilize membranes of mast cells & prevent release of bronchoconstrictive/ inflammatory substances when mast cells are confronted with allergens/other stimuli they release mediators of inflammation Indications for Use: PREVENTOR DRUG Used for prophylaxis of acute asthma attacks in clients with chronic asthma (prior to exercise or known allergen) Mast Cell Stabilizers Use may allow ↓ dosage of bronchodilators & corticosteroids Use 15-20 min prior to known trigger PROPHYLAXIS USE ONLY! exercise, pollutants, etc. Adverse Effects: Very safe drug Occ cough, sore throat, bronchospasm Two Categories of Medications Used to Prevent & Treat OPD, (Particularly Asthma) 1. Long-term control medications AKA: Long-term preventive Controller Maintenance 2. Quick-relief (RESCUE) medications AKA: Reliever Acute rescue OPD Medications: Routes of Administration Two routes: 1. Inhaled “aerosols” Major advantages: Higher concentrations can be delivered more effectively to airways Systemic adverse effects are avoided or minimized Onset of inhaled bronchodilators < oral bronchodilators (5-15 minutes) ‘Rinse & spit’ following inhalation 2. Systemic Oral or parenteral Inhaled Medications: A Variety of Devices Metered-dose inhaler (MDI) Actuation during a slow, deep inhalation (3-5 secs) Followed by 10-second breath-holding; Wait one minute between each puff Do bronchodilator BEFORE anti-inflammatory agent Open-mouth technique (1-2 inches) vs. closed-mouth technique Population: > 5 years Inhaled Medications: A Variety of Devices Breath-actuated MDI Slow inhalation (3-5 secs) - followed by 10-second breathholding 400 inhalations/cannister Indicated for clients unable to coordinate inhalation and actuation cannot be used with spacer/holding chamber devices Population: > 5 years “Maxair Autohaler” Inhaled Medications: A Variety of Devices Spacer/holding chamber Slow (3-5 secs) inhalation or tidal breathing immediately following actuation Easier to use than MDI alone Recommended for anyone using MDI! Population: > 4 years, 4 years with face mask Inhaled Medications: A Variety of Devices Nebulizer Slow tidal breathing with occasional deep breaths tightly fitting face mask for those unable to use mouthpiece Less dependent on client coordination/cooperation DELIVERY METHOD OF CHOICE for cromolyn in children & for high-dose beta² agonists/anticholinergics in MODERATE-TO- SEVERE EXACERBATIONS IN ALL CLIENTS Moving on Drugs to treat Tuberculosis Drugs to KNOW: Drugs to Treat TB isoniazide/INH pyrizinamide/PZD rifampin/Rifadin ethambutol/Myambutol Streptomycin Pharmacological Treatment of TB 1. PERSONS WITH ACTIVE TB At least 6 months of tx with multiple agents Multiple drug regimens for 6-12 months Treatment may last up to 24 months…especially with multi-drug resistant TB 2. PERSONS WITH CLOSE CONTACT TO CASES OF ACTIVE TB and persons with positive PPD but no active disease (prophylactic treatment) SINGLE DRUG REGIMEN: INH FOR 6- 9 MONTHS American Thoracic Society: 3 Principles On Which Treatment For TB Are Based 1. Regimens must include MULTIPLE DRUGS to which the organisms are susceptible 2. The drugs must be taken REGULARLY 3. Drug therapy must continue for a sufficient time to provide safest/most effective therapy in shortest possible period Antitubercular Agents: 5 First-Line Primary Agents isoniazid (INH) * rifampin (Rifadin) ** pyrazinamide (PZA) ** ethambutol (Myambutol) ** Streptomycin ** * Prototype ** Know adverse effects of drug isoniazid (INH)* Mainstay of treatment of TB MOA: Inhibits cell wall synthesis of mycobacterium depletes pyridoxine (B6) (needed for cell to multiply) SE/Adverse Reactions: Hepatoxicity Peripheral neuropathy Tx for neuropathy may include: pyridoxine (Vitamin B6) q day * PROTOTYPE Why would a patient receiving INH therapy take vitamin B6? Vitamin B6 (pyridoxine) is needed for nerve conduction and the synthesis of neurotransmitters A decrease in B6 levels can result in nerve damage Nerve damage can cause “peripheral neuropathy” Peripheral" means nerves further out from the center of the body, distant from the brain and spinal cord."Neuro" means nerves."Pathy" means abnormal) Neuropathic symptoms: Pain, burning, numbness, pins and needles sensation isoniazid (INH) Prophylaxis use alone 6 months – 1 year Active TB use with 1 – 2 other drugs – minimum 6 months and up to 2 years for resistant TB Monitor liver function tests (LFT’s) rifampin (Rifadin) MOA: Inhibits protein synthesis (cell cannot divide) SE/Adverse Reactions: Induces hepatic microsomal enzymes & accelerates metabolism of numerous drugs MONITOR LFTS AND ASSESS FOR JAUNDICE AND ENLARGED LIVER ½ life/therapeutic effects of some drugs Causes harmless redorange discoloration of body fluids pyrazinamide (PZA) Used WITH other antibtubercular agents in treatment of clinical TB MOA: Unknown ? inhibits lipid synthesis ? SE/Adverse Reactions: Hepatoxicity (Check LFT’s) ethambutol (Myambutol) MOA: Inhibits protein synthesis of mycobacterium cell wall SE/Adverse Reactions: Optic neuritis (infection of the optic nerve) visual acuity & ability to differentiate red from green reversible with discontinuation of drug therapy streptomycin Aminoglycoside ANTIBIOTIC 1944 – first TB drug Used today WITH COMBINATIONS ONLY 2° drug toxicities: Hepatoxicity Otoxicity Nephrotoxcity Given parenterally (IM) MOA: Inhibits protein synthesis TB: Sample Drug Plan Drug-susceptibility tests performed Once test results available, meds adjusted accordingly Active disease? Will feel better in 2-3 weeks Culture may take 2-12 weeks Before results are known, client is started on 4-drug regimen (’s possibility of resistant organisms): isoniazid rifampin pyrazinamide ethambutol or streptomycin What is DOT Therapy? Direct Observation Therapy (DOT) Advocated by the World Health Organization (WHO) Form of treatment that requires that another person actually watch the client as the prescribed drugs are taken Can ↑ compliance to near 100% Can be conducted with regimens given once daily, 2 times weekly, or 3 times weekly THE END OF THE ROAD FOR TODAY!