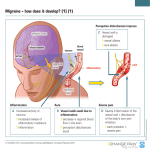
* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download The Genetics of Migraine
Gene desert wikipedia , lookup
Gene therapy of the human retina wikipedia , lookup
Biology and consumer behaviour wikipedia , lookup
Epigenetics of human development wikipedia , lookup
Human genetic variation wikipedia , lookup
X-inactivation wikipedia , lookup
Genome evolution wikipedia , lookup
History of genetic engineering wikipedia , lookup
Gene therapy wikipedia , lookup
Epigenetics of diabetes Type 2 wikipedia , lookup
Gene expression profiling wikipedia , lookup
Quantitative trait locus wikipedia , lookup
Nutriepigenomics wikipedia , lookup
Genetic engineering wikipedia , lookup
Pharmacogenomics wikipedia , lookup
Saethre–Chotzen syndrome wikipedia , lookup
Gene expression programming wikipedia , lookup
Heritability of IQ wikipedia , lookup
Artificial gene synthesis wikipedia , lookup
Oncogenomics wikipedia , lookup
Medical genetics wikipedia , lookup
Epigenetics of neurodegenerative diseases wikipedia , lookup
Neuronal ceroid lipofuscinosis wikipedia , lookup
Site-specific recombinase technology wikipedia , lookup
Frameshift mutation wikipedia , lookup
Population genetics wikipedia , lookup
Designer baby wikipedia , lookup
Public health genomics wikipedia , lookup
Point mutation wikipedia , lookup
Review Genetics of migraine The Genetics of Migraine Anne Ducros, Elisabeth Tournier-Lasserve, and Marie-Germaine Bousser The search for genes involved in the pathophysiology of migraine poses major difficulties. First, there is no objective diagnostic method to assess the status of the individuals studied. Second, migraine is a polygenic multifactorial disorder. Familial hemiplegic migraine (FHM) is the only known autosomal dominant subtype of migraine. In half the families with FHM who have been studied, there are mutations in the calcium-channel gene CACNA1A, located on chromosome 19. In other families, a locus has been mapped on chromosome 1. The role of these loci in typical migraine is still unknown. A susceptibility locus for migraine with aura has been located on chromosome 19 (but is distinct from CACNA1A) and a genome-wide linkage analysis has mapped a susceptibility locus on chromosome 4. Another locus for migraine may be on the X chromosome. Finally, many positive association studies have been published, but few have been replicated. Lancet Neurology 2002; 1: 285–93 Migraine is a primary headache disorder consisting of recurrent attacks of disabling pain that last from a few hours to a few days.1 Typically, patients with migraine are perfectly well between attacks. Migraine is very common, affecting about 15% of the western populations.2–5 The mechanisms of migraine are far from being completely understood. Familial aggregation has long been known and was even classically used as a diagnostic criterion. During the past 10 years, the genetics of migraine has become an important research topic with the major goal being the identification of susceptibility genes that may give clues to the mechanisms underlying this disorder and may help to develop new diagnostic and therapeutic strategies. Why is it so difficult to identify migraine genes? Genetic studies face difficulties directly related to some of the characteristic features of migraine. First, researchers must establish the clinical status of each person studied—ie, find out whether the individual is affected or not. In the absence AD is at the Headache Emergency Department, Lariboisière Hospital. AD and ETL are both at INSERM Unit EMI 99-21, Faculté de Médecine Lariboisière. MGB is at the Department of Neurology, Lariboisière Hospital, Paris, France. Correspondence: Dr Anne Ducros, Urgences Céphalées, Hôpital Lariboisière, 2 rue Ambroise Paré, 75475 Paris Cedex 10, France. Tel +33 1 4995 6537; fax +33 1 4995 2481; email [email protected] THE LANCET Neurology Vol 1 September 2002 of any biological or radiological marker, the diagnosis of migraine is purely clinical. The International Headache Society (IHS) classification (panel), published in 1988,1 IHS diagnosis criteria for migraine without aura, migraine with aura, and two varieties of migraine with aura (migraine with typical aura and FHM)1 Migraine without aura At least five attacks meeting the criteria below: Headache attacks lasting between 4 h and 72 h (untreated or unsuccessfully treated) Headache with at least two of the following characteristics: Unilateral location Pulsating quality Moderate or severe intensity Aggravation by walking up stairs or similar routine physical activity During headache at least one of the following: Nausea and/or vomiting Photophobia and phonophobia At least one of the following: History and physical and neurological examinations do not suggest a disorder causing secondary headaches History and physical and neurological examinations suggest a disorder causing secondary headaches, but it is ruled out by appropriate investigations Such a disorder is present, but migraine attacks do not occur for the first time in close temporal relation to the disorder Migraine with aura At least two attacks meeting the criteria below: At least three of the following four characteristics: One or more fully reversible aura symptoms indicating focal cerebral cortical and/or brain stem dysfunction At least one aura symptom that develops gradually over more than 4 min or two or more symptoms that occur in succession No aura symptom lasts more than 60 min; if more than one aura symptom is present, duration is proportionally increased Headache follows aura with a free interval of less than 60 mins (it may also begin before or simultaneously with the aura) At least one of the following: History and physical and neurological examinations do not suggest a disorder causing secondary headaches History and physical and neurological examinations suggest a disorder causing secondary headaches, but it is ruled out by appropriate investigations Such a disorder is present, but migraine attacks do not occur for the first time in close temporal relation to the disorder Migraine with typical aura Meets criteria for migraine with aura (above) including all four of the following criteria: Homonymous visual disturbances Unilateral paresthesias and/or numbness Unilateral weakness Aphasia or unclassifiable speech difficulty Familial hemiplegic migraine Meets criteria for migraine with aura The aura includes some degree of hemiparesis and may be prolonged At least one first-degree relative has identical attacks http://neurology.thelancet.com 285 For personal use. Only reproduce with permission from The Lancet Publishing Group. Review Genetics of migraine distinguishes different varieties of migraine, the two most frequent being migraine without aura and migraine with aura. Attacks of migraine without aura are characterised by moderate to severe head pain which is often unilateral, pulsating, and aggravated by routine physical activity (panel). The headache lasts from 4 h to 72 h and is associated with nausea, vomiting, photophobia, and phonophobia. Attacks of migraine with aura are characterised by transient neurological signs preceding or accompanying the headache phase. These “aura” symptoms develop gradually and last from a few minutes to up to an hour (panel). Visual symptoms, including the classical scintillating scotoma, are the most frequent, followed by sensory disturbances, speech difficulties, and, rarely, motor symptoms. Migraine is characterised by the repetition of such attacks in the absence of any underlying disorder causing secondary headaches. According to the IHS criteria, at least five attacks of migraine without aura or two attacks of migraine with aura are required to classify a person as affected. Recurrent migraine attacks may be part of the clinical range of several organic cerebral disorders such as arteriovenous malformations,6 mitochondrial encephalopathies (including mitochondrial encephalopathy with lactic acidosis and stroke-like episodes [MELAS]),7,8 antiphospholipid antibody disease,9 and some cerebral arteriopathies including cerebral autosomal dominant arteriopathy with subcortical infarcts and leucoencephalopathy (CADASIL).10,11 Moreover, a migrainous attack may be triggered by various acute vascular events such as cervical-artery dissection, cerebral-venous thrombosis, or cerebral infarction. In patients affected by such disorders, migraine attacks are symptomatic of the underlying problem. However, symptomatic migraine attacks are often difficult to distinguish from those of a primary migraine disorder. Are the mechanisms of symptomatic migraine attacks different from those of primary migraine attacks? Or is it just that patients with these organic cerebral disorders have a lower threshold for developing migraine attacks? As described above, the IHS classification distinguishes different types of migraine. Migraine without aura is more common than migraine with aura in the general population (6–10% vs 3–6%). Some patients have attacks of only one type—with or without aura—but about a third experience both types of attacks during their life. We do not yet know whether migraine with and without aura are two clinical forms of the same disease, or whether they represent two distinct disorders. There are also other less common types of migraine. Several genetic studies have focused on familial hemiplegic migraine (FHM), a rare type of migraine with aura, because it is the only form in which a monogenic mendelian mode of inheritance has been clearly established.12,13 A typical attack is characterised by unilateral motor weakness associated with at least one other aura symptom such as sensory disturbances within the zone of motor deficit, visual symptoms, or aphasia.13–16 Bilateral motor and sensory symptoms are reported by about a quarter of patients.16,17 The aura phase lasts for 1–2 h and is followed by a migrainous headache. The mean age at onset is lower (at about 11 years) than in other types of 286 migraine.16,18,19 Moreover, severe attacks of confusion or even coma with prolonged hemiplegia, fever, and meningismus are reported by a third of the patients with FHM at least once in their life.16,20–23 Finally, some patients may have permanent neurological signs between attacks, mostly nystagmus and ataxia.15,16,22,24 These features have led to the distinction between families with pure hemiplegic migraine (80%) and those with hemiplegic migraine and cerebellar symptoms (20%), in which at least one family member has nystagmus or ataxia.13,25,26 FHM is characterised by large clinical variability in the severity and frequency of attacks among individuals belonging to different families but also within the same family.13,15,16 Besides familial cases, some sporadic cases of hemiplegic migraine with cerebellar symptoms have also been reported.16,27 Whether FHM has the same pathophysiological mechanisms as other types of migraine with aura is not known. Classification of individuals as “affected” or “unaffected” for genetic studies does not reflect the important clinical heterogeneity of migraine. Indeed, the frequency and severity of attacks show much variability from one patient to another. Let us consider, for example, a family in which the 40-year-old daughter has had one or two severe attacks of migraine without aura with intractable headache and vomiting every month, lasting 3 days at a time, since the age of 12. The 65-year-old mother has had only two mild and short attacks of migraine with visual aura in her fifties. The daughter is affected by migraine without aura and the mother by migraine with aura, but do they suffer from the same disorder? Finally, several other factors have to be taken into account in genetic studies of migraine. The high prevalence of migraine (8–25% of the population)2,3 could lead, purely by chance, to a significant part of the observed familial aggregation. Women are twice as likely to be affected as men, which also has to be taken into account in segregation studies.4,5 Is migraine a genetic condition? In addition to genetic factors, familial aggregation of a pathological disorder may be due to environmental factors and may also, as previously mentioned, occur purely by chance in very common diseases. A major step in the study of migraine genetics was thus to show the existence of genetic factors by the means of genetic epidemiological surveys.28 Twin studies have been used to assess the respective roles of genetic and environmental factors. These studies are based on the comparison of concordance rates between monozygotic and dizygotic twins. All twin studies done so far show that migraine has a genetic component in addition to environmental factors.29–36 The most recent of these studies was the only one that was carried out in a large population and used the IHS diagnosis criteria. In this Danish twin study including 1013 monozygotic and 1667 dizygotic twin-pairs, the pairwise concordance rate was significantly higher among monozygotic than dizygotic twin pairs for migraine without aura (28 vs 18%, p<0·05)34 and for migraine with aura (34 vs 12%, p<0·001).36 THE LANCET Neurology Vol 1 September 2002 http://neurology.thelancet.com For personal use. Only reproduce with permission from The Lancet Publishing Group. Review Genetics of migraine Family studies provide information about the effect of genetic factors and the potential mode of inheritance. Many studies have produced controversial results owing to methodological biases such as the lack of homogeneous diagnostic criteria before 1988, the lack of separation between migraine without aura and migraine with aura, the use of a questionnaire instead of direct interview of the probands, the lack of a direct interview of the relatives, and the selection of probands from specialised centres.37–41 However, all of these studies concluded that genetic factors are implicated in migraine. The proportion of familial cases was estimated to be between 34% and 90%, and all possible transmission patterns were proposed, apart from X-linked inheritance. Two family studies addressing all methodological concerns have been published. Russell and Olesen42 studied the relative risk of migraine without aura and migraine with aura in all first-degree relatives and spouses of 44 probands selected out of 4000 representative individuals from the general Danish population. Compared with the general population, first-degree relatives of probands with migraine without aura had a relative risk of 1·86 (95% CI 1·56 to 2·16) of migraine without aura and first-degree relatives of probands with migraine with aura had a relative risk of 3·79 (95% CI 3·21 to 4·38) of migraine with aura.42 Stewart and colleagues43 undertook a population-based study in Maryland (USA) to analyse the relative risk of migraine without aura and migraine with aura in all first-degree relatives of 73 migrainous probands and 72 matched controls. Compared with controls, first-degree relatives of probands with migraine had a relative risk of 1·50. However, this increase in risk was not statistically significant (95% CI 0·94 to 2·40) and no difference was observed when migraine without aura and migraine with aura were analysed separately. When the researchers considered only the 26 probands with important disability due to migraine, they found a 2·17-fold significantly increased risk of migraine in first-degree relatives (95% CI 1·22 to 3·87).43 With regard to the mode of inheritance, the results of a large Danish population-based segregation analysis, including 126 families with migraine without aura and 127 families with migraine with aura, showed that both types of migraine have a non-mendelian multifactorial mode of inheritance.44 Analysis of the Danish twin-study data also favoured a model combining additive genetic and environmental factors.34–36 In addition, analysis of 31 families with a high risk of migraine without aura also suggested multifactorial inheritance.45 Together, these data indicate that both migraine without aura and migraine with aura are complex diseases caused by a combination of genetic and environmental factors. Several studies have suggested that genetic factors may be more important in migraine with aura than in migraine without.35,36,42 The possible number of genetic susceptibility loci is unknown. FHM is the only monogenic variety of migraine.12,13 Strategies in the quest for migraine genes In non-mendelian diseases, the identification of diseasecausing mutations can be achieved by different methods. In THE LANCET Neurology Vol 1 September 2002 families, linkage analysis to candidate genes or markers can be used to map a susceptibility locus, followed by detection of the pathogenetic mutation and positional cloning. Modelfree or non-parametric linkage analyses have to be used in migraine because classic parametric linkage analyses require the definition of a precise genetic model, and such a definition is inaccurate in non-mendelian disorders. Association studies, which do not have such difficult methodological considerations, can be performed in homogeneous populations.46 These studies compare the frequency of alleles of a polymorphic genetic marker between patients and healthy controls. In the absence of methodological shortcomings, a significant difference means that the polymorphism is located within the susceptibility gene or is in linkage disequilibrium with the susceptibility gene. However, association studies do not provide any indication of the normal function of the tested gene or of its abnormal function in the pathophysiology of the disease being studied.46 By contrast, genetics provides powerful tools for the identification of genes causing mendelian disorders. Several research teams have thus focused their efforts on the localisation and identification of the genes involved in FHM, since these genes may also be good candidates for the much more frequent migraine types, migraine with aura and migraine without aura. Genetic heterogeneity of FHM FHM is genetically heterogeneous.12,14,25,26,47–49 Joutel and coworkers47 localised the first gene on the short arm of chromosome 19 in 1993. In 1996, Ophoff and colleagues12 identified this gene as CACNA1A, which encodes the ␣1A subunit of the neuronal P/Q type voltage-gated calcium-ion channel. CACNA1A is implicated in about 50% of families with FHM and in all families with FHM and permanent cerebellar symptoms.14–16,25,26 In 1997, a second gene was mapped to chromosome 1q; significant linkage with markers located on 1q31 was found in a large American family48 and significant linkage to more centromeric markers located at 1q21-q23 was found in three French families.49 From present evidence, we do not know whether one gene or two distinct genes for FHM are located on chromosome 1q. The chromosome 1 locus is implicated in a few families (10–20%) of those affected by pure FHM.49 Finally, 30–40% of families show no linkage to these first two loci, which suggests the existence of at least one other FHM gene.49 CACNA1A, ␣1A subunit, and P/Q-type channels CACNA1A, the only known FHM gene, encodes the main subunit of the P/Q type voltage-gated calcium channel.12 These channels are large multimeric proteins located within the cell membrane; in the centre is a pore that opens in response to membrane depolarisation, letting calcium ions flow into the cell.50,51 In neurons, they have a major role in the control of neuronal excitability and neurotransmitter release. Each channel is formed by a main ␣1 subunit associated with four auxiliary subunits (␣2, , ␥, and ␦).50,51 The ␣1 subunit forms the ionic pore that includes the structures that bring about voltage sensitivity and ionic http://neurology.thelancet.com 287 For personal use. Only reproduce with permission from The Lancet Publishing Group. Review R195K R192Q S218L Genetics of migraine V1457L V714A K1336E R583Q T666M D715E V1696I Y1385C R1668W L1682P W1684R I1811L CACNA1A mutations causing FHM. A schematic structure of the ␣1A pore-forming subunit of the P/Q type voltage-gated calcium channels is shown. This subunit is located in the neuronal membrane and contains four repeat domains. Each domain includes six membrane-spanning segments (S1 to S6) and a so-called P-loop between the fifth and sixth segments. The four S4 segments form the voltage sensor of the channel, the four S5 and S6 segments build the ionic pore, and the four P-loops line the inner part of this pore. Positions of the 15 mis-sense mutations identified in FHM are indicated. Mutations causing pure hemiplegic migraine are represented by red circles and mutations causing hemiplegic migraine with permanent cerebellar symptoms are represented by green stars. selectivity. All ␣1 subunits have the same structure (figure). There are at least ten genes (CACNA1A, B, C, D, E, F, G, H, I, and S) coding for distinct ␣1 subunits.50–52 Depending on the ␣1 subunit type, a calcium channel has distinct pharmacological and kinetic properties generating different types of calcium currents: L, N, P/Q, R, or T.50,51,53 The ␣1A subunit is the main subunit of P/Q type neuronal calcium channels, which are expressed in central neurons and in peripheral neurons at the neuromuscular junction.50,54 As a result of alternative splicing, ␣1A subunits can generate two distinct types of calcium currents: the slow inactivating P-type currents that are the major calcium currents in cerebellar Purkinje cells, and the fast inactivating Q-type currents that play a major part in the control of neurotransmitter release.55 CACNA1A is a large gene containing 47 exons.12 Exon 47 contains a polymorphic CAG repeat, which is predicted to code for a polyglutamine stretch in a subset of the known human transcripts.56 Thus far, 15 CACNA1A mutations have been identified in 31 families with FHM (24 affected by FHM with cerebellar symptoms and seven by pure FHM) and in two sporadic cases affected by hemiplegic migraine with cerebellar symptoms (table 1).12,16,19,27,57–63 Five of these mutations are recurrent—ie, they have been detected in two or more unrelated families.12,16,19,57,59,60,62,63 The commonest mutation, T666M, has been detected in 12 unrelated families and in one sporadic case.12,16,59,60,63 All 15 mutations are missense mutations, causing a substitution of one amino acid of the 2550 that constitute the predicted protein. The mutations are located in important functional domains of the subunit, near the ionic pore or within the voltage sensor (figure). Nine of the 15 mutations, including the five recurrent ones, are associated with hemiplegic migraine with cerebellar symptoms. Different CACNA1A mutations have been identified in two other autosomal dominant neurological disorders: episodic ataxia type 2 (EA2)12 and spinocerebellar ataxia type 6 (SCA6).56 EA2, like FHM, is a paroxysmal neurological disorder causing recurrent attacks of major instability with lack of coordination. Attacks are often provoked by exercise or emotion and last between 15 min and a few hours. Acetazolamide is effective in preventing attacks in most patients. During attack-free intervals, clinical examination commonly discloses permanent cerebellar signs (nystagmus and/or ataxia). Most of the mutations identified in patients with EA2 are predicted to result in a truncation of the putative protein.12,64,65 SCA6 is a progressive cerebellar disease Table 1. CACNA1A mutations identified in FHM Mutation S218L R583Q D715E Y1385C Reference 62 57 16 12 60 16 63 16 16 27 R1668W L1682P W1684R I1811L 16 61 16 12 Family (or case) 2 families 1 family 3 families 1 family 1 family 9 families 1 family 1 sporadic case 1 family 1 sporadic case (de novo mutation) 1 family 1 family 1 family 2 families R192Q R195K V714A K1336E V1457L R1668W V1696I 12 16 12 16 58 16 16 1 family 1 family 1 family 1 family 1 family 1 family 1 family T666M 288 Exon 5 13 Nucleotide change TCG→TTG CGA→CAA ␣1A subunit domain IS4-S5 IIS4 Cerebellar symptoms + + 16 ACG→ATG II P loop + 17 26 GAC→GAG TAC→TGC IIS6 IIIS5 + + 32 32 32 36 CGG→TGG CTN→CCN TGG→CGG ATC→CTC IVS4 IVS4 IVS4-S5 IVS6 + + + + 4 4 17 25 27 32 33 CGA→CAA AGG→AAG GTG→GCG AAA→GAA GTG→TTG CGG→TGG GTC→ATC IS4 IS4 IIS6 IIIS3-S4 III P loop IVS4 IVS5 - THE LANCET Neurology Vol 1 September 2002 http://neurology.thelancet.com For personal use. Only reproduce with permission from The Lancet Publishing Group. Review Genetics of migraine characterised by an adult-onset statokinetic ataxia caused by small expansions of the CAG repeat contained within exon 47 of CACNA1A.56,66 Consequences of CACNA1A mutations Several methods can be used to understand the mechanisms leading from the different CACNA1A mutations to the observed phenotypes. Seven CACNA1A mutations causing FHM have been studied electrophysiologically by comparison of the calcium currents between cells expressing the wild-type gene and cells expressing the mutant gene.67–69 All the mutations modify the density and the gating properties of P/Q-type currents. FHM mutations are thus “gain of function” mutations with the abnormal protein producing altered calcium currents. No difference was observed between the mutations causing pure FHM and the mutations causing FHM with cerebellar symptoms. However, the conditions in vitro are unlikely to reflect the complexity of the situation in vivo. On the other hand, EA2 mutations are “loss of function” mutations with the mutated protein incapable of generating any current when expressed in heterologous cells.70,71 Knockout mice that do not carry the Cacna1a gene are born with a severe ataxia and die within a few days.72 Mice carrying different mutations within Cacna1a display distinct phenotypes called tottering,73 leaner,73 or rocker,74 which are characterised by various paroxysmal manifestations (absence epilepsy and motor attacks) and are in all cases associated with a permanent cerebellar ataxia of variable severity. Tottering mice show abnormal control of acetylcholine release at the neuromuscular junction.54 Moreover, the different mutants display several anatomical abnormalities, including abnormal arborisation of Purkinje cells, abnormal migration of granular cells, and abnormalities of the locus coeruleus.73,74 These abnormalities suggest that P/Q-type channels may be implicated not only in the control of neurotransmitter release but also in neuronal development. Genotype–phenotype correlations in FHM FHM is characterised by striking clinical variability. Age at onset, frequency, duration, and features of attacks may vary from one patient to another, even among affected members from a given family who all carry the same mutation in the same gene.16,19 This variability suggests complex interactions between the consequences of the mutation and environmental factors or modifying genetic factors. Several studies have shown that the various FHM genotypes have a role in producing this clinical variability. In a study of five families, the clinical features of 46 patients from three families with linkage to chromosome 19 were compared with those of 20 patients from two unlinked families.15 Patients from the families with chromosome 19 linkage had a higher frequency of attacks with loss of consciousness (39% vs 15%) and head-trauma triggered attacks (70% vs 40%) than unlinked families.15 In a study of 17 families, the clinical and genetic features of FHM were THE LANCET Neurology Vol 1 September 2002 compared between three groups of families: ten with linkage to chromosome 19 (94 patients), three with linkage to chromosome 1 (24 patients), and four unlinked families (24 patients).75 Two major differences were shown: first, the penetrance of FHM was lower in chromosome-1-linked families than in the other group and second, permanent cerebellar symptoms were present in a subset of chromosome-19-linked families and absent in all the other family groups.75 The detailed clinical analysis of a large series of 117 individuals with CACNA1A mutations causing FHM has allowed better delineation of the clinical range of this type of migraine with aura.16 FHM caused by CACNA1A mutations is characterised by a high penetrance of hemiplegic migraine attacks (86%), in which the motor aura is always associated with sensory, language, or visual aura symptoms. However, in contrast to other varieties of migraine with aura in which visual symptoms are present in about 99% of patients, a quarter of patients with FHM do not have visual symptoms.76 FHM is also characterised by the frequency of bilateral motor signs during aura (about 30% of patients), severe attacks with impairment of consciousness (30% of patients), an early age at onset (close to 11 years), and by the importance of minor head trauma as a triggering factor. Finally, permanent cerebellar signs are found in about 80% of patients with mutations belonging to families who have hemiplegic migraine with cerebellar symptoms. Altogether, these characteristics suggest that FHM due to CACNA1A mutations is a very unusual variety of migraine with aura. In addition, striking correlations have been found between the genotype and phenotype. The frequency of symptoms was studied in 85 patients with the three most frequent mutations linked to FHM with cerebellar signs: T666M (55 patients), R583Q (16 patients), and D715E (14 patients).16 Patients with the T666M mutation had the highest penetrance of hemiplegic migraine (98%), severe attacks with coma (50%), and nystagmus (86%). Patients with the R583Q mutation had the highest penetrance of gait ataxia (81%) in the absence of any nystagmus, and those with the D715E mutation had the lowest penetrance of hemiplegic migraine attacks (64%).16 The various studies of CACNA1A mutations in FHM have provided several important insights. First, the mutations causing FHM with cerebellar symptoms are distinct from those causing pure FHM, and all recurrent mutations cause FHM with cerebellar symptoms.16,19 This genotype–phenotype correlation strongly suggests that mutations causing FHM with cerebellar symptoms have particular pathogenetic consequences in cerebellar neurons, whereas mutations causing pure FHM do not have such deleterious effects. Second, other important genotype–phenotype correlations have been demonstrated, suggesting that the existence of distinct CACNA1A mutations may explain, at least partly, the clinical variability of FHM.16,19 Finally, mutations have been detected in two sporadic cases, including a de novo mutation; thus, sporadic hemiplegic migraine is due to CACNA1A mutations in at least some cases.16,27 http://neurology.thelancet.com 289 For personal use. Only reproduce with permission from The Lancet Publishing Group. Review Genetics of migraine Are FHM genes implicated in migraine without aura and/or migraine with aura? CACNA1A is the first gene for which an involvement in a subtype of migraine has been demonstrated. CACNA1A and the other FHM genes represent good candidate genes for migraine with aura and migraine without aura. Indeed, several clinical features support the hypothesis that migraine without aura and migraine with aura could also be neurological channelopathies, the main factor being paroxysmal presentation with attacks lasting a few hours to a few days. Several groups have tried to implicate CACNA1A or other ion channel genes indirectly in migraine with aura and migraine without aura. Subtle subclinical cerebellar abnormalities have been discovered by the analysis of hand reaching movements in patients with migraine.77 This impairment was more pronounced in patients with aura than those without. By means of single-fibre electromyography, subclinical abnormalities of neuromuscular transmission have been shown in a subset of patients with migraine with aura.78,79 Single-endplate abnormalities were significantly more frequent in a group of patients affected by migraine with prolonged aura than in a group of healthy volunteers.80 These studies do not show that CACNA1A is involved in migraine without aura or migraine with aura, but they do provide important information about the existence of mild subclinical permanent neurological abnormalities in a subgroup of patients with migraine that could be used as objective markers to constitute homogeneous groups of patients for genetic studies. The involvement of CACNA1A in the more frequent types of migraine has been analysed by linkage and association studies with contradictory results.81–88 None of the positive studies provided a direct analysis of the CACNA1A gene to detect pathogenetic mutations. As a consequence, these studies showed only that a susceptibility locus for migraine with or without aura might be located nearby or within the 19p13 region, without direct evidence that CACNA1A was the susceptibility gene. Nyholt and coworkers82 published a linkage study in a large family affected by migraine with aura showing positive linkage results with 19p13 markers. Subsequently, the same group reported that sequencing of the 47 exons of CACNA1A in two patients from this family did not reveal any mutations.87 In a second step, they conducted a linkage analysis in 82 pedigrees and a large case-control association study but did not detect any linkage or association between CACNA1A polymorphisms and migraine in these groups.87 Jones and colleagues88 analysed families affected by migraine with aura for cosegregation of the disease with six chromosome-19p13 markers. Positive lod scores were obtained by use of multipoint model-free linkage analysis as well as a dominant affected-only model with all six tested markers. The maximum lod score (model-free lod=4·28) was obtained close to marker D19S592, which is located about 10 cM telomeric to CACNA1A. This study reinforces the positive results previously obtained by several groups and is consistent with the presence of a susceptibility locus for migraine on 19p close to, but distinct from, the CACNA1A gene.81–83 290 On the basis of these studies, CACNA1A is most likely not a major susceptibility gene for migraine with aura and migraine without aura. Some explanations for this conclusion are as follows. First, as discussed above, FHM resulting from CACNA1A mutations differs from typical migraine in its unusual genetic and clinical features, including a high penetrance of hemiplegic migraine attacks and a frequent association with permanent clinically obvious cerebellar symptoms.16 Second, CACNA1A is implicated in less than 40% of families with pure FHM.14,16,25,26,48,49,58,75 The genes causing pure FHM (ie, without cerebellar signs) may be better candidate genes for migraine with aura and migraine without aura. However, none of the previously cited studies have definitively ruled out the possibility that CACNA1A may contribute to migraine with aura, at least in a small subset of patients and families. Three of the 16 families with migraine with aura studied by Jones and colleagues88 had higher lod scores with markers from the CACNA1A locus than with markers located telomeric to CACNA1A. These families may therefore show linkage to CACNA1A. Further data are needed to clarify the relations between CACNA1A and migraine with aura.88 Genes encoding ion-channel subunits are major candidates for other FHM genes and remain good candidates for migraine with aura and migraine without aura. The chromosome 1q FHM gene (or genes) remains unidentified. Moreover, nothing is known about the involvement of the chromosome 1q FHM locus in migraine with aura and migraine without aura, and a third FHM gene has yet to be mapped. Are other loci or genes implicated in migraine with or without aura? Nyholt and colleagues89,90 have analysed X-chromosome markers in three large Australian pedigrees. They found positive non-parametric lod scores with Xq24–28 markers in two of these families.89,90 According to these researchers, this locus may be involved in the higher female prevalence of this disorder. Further studies, including a much larger panel of families, are necessary to confirm the role of an X-chromosome locus in migraine susceptibility. As previously discussed, Jones and colleagues88 have shown that chromosome 19p13 contains a susceptibility locus for migraine with aura that seems to be distinct from the FHM locus. Subsequently, the same group found a significant association between migraine and five different single-nucleotide polymorphisms within the insulin receptor gene (INSR) located on 19p13.91 This association was found in two large case-control populations collected independently, including a total of 827 cases and 765 controls. Positive association was mainly accounted for by the results obtained in patients with migraine with aura and in one of the two populations. The five single-nucleotidepolymorphism alleles associated with migraine had no effect on INSR transcription, translation, protein expression, and INSR-mediated functions.91 This study did not exclude the possibility that the five polymorphisms in INSR could be in linkage disequilibrium with another gene close to INSR. The nature of INSR gene involvement in migraine remains to be THE LANCET Neurology Vol 1 September 2002 http://neurology.thelancet.com For personal use. Only reproduce with permission from The Lancet Publishing Group. Review Genetics of migraine elucidated and present evidence does not allow us to consider INSR as a migraine gene. Recently Wessman and colleagues92 published the first genome-wide linkage analysis in migraine with aura, which led to the mapping of a susceptibility locus on chromosome 4q24.92 This large study included 50 Finnish families with vertical transmission of migraine with aura consistent with dominant inheritance. The Finnish population is genetically homogeneous owing to a small number of founders. The researchers analysed only families affected by migraine with aura because of data suggesting that genetic factors may be more important in migraine with aura than in migraine without aura. Moreover, only individuals affected by migraine with aura were considered to avoid heterogeneity and eventual phenocopies that might have been introduced by inclusion of migraine without aura. Statistically significant linkage was found with the marker D4S1647 by parametric two-point linkage analysis on the assumption of a dominant mode of transmission, as well as multipoint parametric and non-parametric analyses.92 The chromosome 4q24 locus was the only one to give significant linkage results in this panel of families. In addition, non-significant nominal evidence of linkage (ie, positive lod scores <3, p>0·001) was found with other markers, including markers on 19p13.2, 1q42.2, and Xp (but not Xq). The 19p13 marker that gave a positive lod score is located telomeric to CACNA1A, and the 1q42 marker that gave a positive lod score is located telomeric to both FHM loci (1q21–23 and 1q31). The results of this study strongly suggest a susceptibility locus for migraine with aura on 4q24. Lea and colleagues93 recently published a linkage study in a large family affected by typical migraine. They reported significant linkage using a chromosome 1q31 marker located within the locus for FHM. These researchers also conducted a linkage analysis of 82 pedigrees and a case-control association study, which produced positive linkage results (maximum lod score of 1·24, p=0·008) and significant association results (p=0·010). These observations will need to be confirmed by other researchers but they reinforce the hypothesis that pure FHM genes may be good candidates for migraine with or without aura. Finally, many association studies have been performed in migraine.94 Positive associations have been found between migraine and polymorphisms within genes encoding the dopamine D2 receptor,95,96 the human serotonin transporter,97,98 catechol-O-methyltransferase,99 endothelin type A,100 dopamine -hydroxylase,101 and 5,10-methylenetetrahydrofolate reductase.102 These various candidate polymorphisms have been chosen on the basis of the Search strategy and selection criteria aura Migraine subtype FHM with cerebellar symptoms Pure FHM Pure FHM Migraine with aura Chromosome 19p13 19p13 1q21–23 1q31 19p13.2 Migraine with aura Migraine with aura 4q24 Xq Gene CACNA1A CACNA1A Unknown Distinct from CACNA1A? INSR? Unknown Unknown hypothesis that the genes containing them encode proteins that are thought to be involved in migraine. However, further studies are needed to find out whether the alleles associated with migraine have any biological effect. Moreover, most of these studies are single reports and await replication. Summary Migraine is a complex polygenic multifactorial disorder in which genetic factors interact with environmental factors. Several studies have suggested that genetic factors may be more important in migraine with aura than in migraine without aura. The number of different susceptibility loci and genes is still unknown (table 2). FHM, which is the only known monogenic variety of migraine, is caused by mutations in the calcium channel gene CACNA1A located on chromosome 19p13 in about 50% of families. In those families, FHM is thus a neuronal channelopathy. However, CACNA1A is most likely not a major susceptibility gene for the other types of migraine. Other FHM genes, responsible for pure FHM, may be better candidate genes for migraine with aura and migraine without aura. Recent data suggest that a susceptibility locus for migraine with aura is located on 19p13, telomeric to CACNA1A. Another susceptibility locus for migraine with aura has been mapped on 4q24 by a genome-wide linkage analysis in 50 Finnish families. Finally, a migraine susceptibility locus may reside on Xq. Several associations have been found between polymorphisms within various candidate genes and migraine, but the significance of these findings is still unclear. Future objectives in migraine genetics are: to identify other FHM genes and to analyse their role in migraine with aura and migraine without aura; to identify the susceptibility gene or genes for migraine with aura located within the 19p13 locus and to find out whether CACNA1A is implicated; and to replicate the 4q24 significant linkage results in migraine with aura in a non-Finnish population and identify the underlying susceptibility gene. Authors’ contributions Data for this review were identified by searches of Medline and references from relevant articles using the search terms “migraine”, “hemiplegic migraine”, “familial”, “genetics”, “association study”, “polymorphism”, “linkage”, “gene”, and “calcium channel”. Many articles were also identified through searches of the extensive files of the authors. Abstracts were included only when they related directly to previous published work. In addition to papers published in English, a few papers published in French were reviewed. THE LANCET Neurology Vol 1 September 2002 Table 2. Susceptibility loci identified in FHM and in migraine with AD wrote this review with assistance from MGB. ETL and MGB critically evaluated the review at its various stages. Conflict of interest We have no conflict of interest. Role of the funding source The authors are supported by the Assistance Publique des Hopitaux de Paris and by INSERM. No funding body had a role in the preparation of the review or in the decision to submit it for publication. http://neurology.thelancet.com 291 For personal use. Only reproduce with permission from The Lancet Publishing Group. Review Genetics of migraine References 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 Headache Classification Committee of the International Headache Society. Classification and diagnostic criteria for headache disorders, cranial neuralgias and facial pain. Cephalalgia 1988; 8: 1–96. Henry P, Michel P, Brochet B, Dartigues JF, Tison S, Salamon R. A nationwide survey of migraine in France: prevalence and clinical features in adults. Cephalalgia 1992; 12: 229–37. Stewart WF, Lipton RB, Celentano DD, Reed ML. Prevalence of migraine headache in the United States: relation to age, income, race, and other sociodemographic factors. JAMA 1992; 267: 64–9. Lipton RB, Silberstein SD, Stewart WF. An update on the epidemiology of migraine. Headache 1994; 34: 319–28. Lipton RB, Stewart WF, Diamond S, Diamond ML, Reed M. Prevalence and burden of migraine in the United States: data from the American Migraine Study II. Headache 2001; 41: 646–57. Bruyn GW. Intracranial arteriovenous malformation and migraine. Cephalalgia 1984; 4: 191–207. Pavlakis SG, Phillips PC, DiMauro S, De Vivo DC, Rowland LP. Mitochondrial myopathy, encephalopathy, lactic acidosis, and strokelike episodes: a distinctive clinical syndrome. Ann Neurol 1984; 16: 481–88. Montagna P, Gallassi R, Medori R, et al. MELAS syndrome: characteristic migrainous and epileptic features and maternal transmission. Neurology 1988; 38: 751–54. Cervera R, Piette JC, Font J, et al. Antiphospholipid syndrome: clinical and immunologic manifestations and patterns of disease expression in a cohort of 1,000 patients. Arthritis Rheum 2002; 46: 1019–27. Verin M, Rolland Y, Landgraf F, et al. New phenotype of the cerebral autosomal dominant arteriopathy mapped to chromosome 19: migraine as the prominent clinical feature. J Neurol Neurosurg Psychiatry 1995; 59: 579–85. Chabriat H, Vahedi K, Iba-Zizen MT, et al. Clinical spectrum of CADASIL: a study of 7 families. Lancet 1995; 346: 934–39. Ophoff RA, Terwindt GM, Vergouwe MN, et al. Familial hemiplegic migraine and episodic ataxia type-2 are caused by mutations in the Ca2+ channel gene CACNL1A4. Cell 1996; 87: 543–52. Ducros A, Campbell JK. Familial hemiplegic migraine. In: Olesen J, Tfelt-Hansen P, Welch KMA, eds. The headaches, 2nd edn. New York: LippincottRaven, 2000: 501–05. Ahmed MA, Reid E, Cooke A, Arngrimsson R, Tolmie JL, Stephenson JB. Familial hemiplegic migraine in the west of Scotland: a clinical and genetic study of seven families. J Neurol Neurosurg Psychiatry 1996; 61: 616–20. Terwindt GM, Ophoff RA, Haan J, Frants RR, Ferrari MD. Familial hemiplegic migraine: a clinical comparison of families linked and unlinked to chromosome 19. Cephalalgia 1996; 16: 153–55. Ducros A, Denier C, Joutel A, et al. The clinical spectrum of familial hemiplegic migraine associated with mutations in a neuronal calcium channel. N Engl J Med 2001; 345: 17–24. Haan J, Terwindt GM, Ophoff RA, et al. Is familial hemiplegic migraine a hereditary form of basilar migraine? Cephalalgia 1995; 15: 477–81. Haan J, Terwindt GM, Bos PL, Ophoff RA, Frants RR, Ferrari MD. Familial hemiplegic migraine in The Netherlands. Clin Neurol Neurosurg 1994; 96: 244–49. Terwindt GM, Ophoff RA, Haan J, et al. Variable clinical expression of mutations in the P/Q-type calcium channel gene in familial hemiplegic migraine. Neurology 1998; 50: 1105–10. Fitzsimons RB, Wolfenden WH. Migraine coma: meningitic migraine with cerebral oedema associated with a new form of autosomal dominant cerebellar ataxia. Brain 1985; 108: 555–77. Munte TF, Muller-Vahl H. Familial migraine coma: a case study. J Neurol 1990; 237: 59–61. Elliott MA, Peroutka SJ, Welch S, May EF. Familial hemiplegic migraine, nystagmus, and cerebellar atrophy. Ann Neurol 1996; 39: 100–06. Echenne B, Ducros A, Rivier F, et al. Recurrent episodes of coma: an unusual phenotype of familial hemiplegic migraine with linkage to chromosome 1. Neuropediatrics 1999; 30: 214–17. Young GF, Leon-Barth CA, Green J. Familial hemiplegic migraine, retinal degeneration, deafness, and nystagmus. Arch Neurol 1970; 23: 201–09. Joutel A, Ducros A, Vahedi K, et al. Genetic heterogeneity of familial hemiplegic migraine. Am J Hum Genet 1994; 55: 1166–72. Ophoff RA, van Eijk R, Sandkuijl LA, et al. Genetic 292 27 28 29 30 31 32 33 34 35 36 37 38 39 40 41 42 43 44 45 46 47 48 49 50 51 52 53 54 55 heterogeneity of familial hemiplegic migraine. Genomics 1994; 22: 21–26. Vahedi K, Denier C, Ducros A, et al. CACNA1A gene de novo mutation causing hemiplegic migraine, coma, and cerebellar atrophy. Neurology 2000; 55: 1040–42. Russell MB, Olesen J. The genetics of migraine without aura and migraine with aura. Cephalalgia 1993; 13: 245–48. Ziegler DK, Hassanein RS, Harris D, Stewart R. Headache in a non-clinic twin population. Headache 1975; 14: 213–18. Lucas RN. Migraine in twins. J Psychosom Res 1977; 21: 147–56. Honkasalo ML, Kaprio J, Winter T, Heikkila K, Sillanpaa M, Koskenvuo M. Migraine and concomitant symptoms among 8167 adult twin pairs. Headache 1995; 35: 70–78. Larsson B, Bille B, Pedersen NL. Genetic influence in headaches: a Swedish twin study. Headache 1995; 35: 513–19. Ziegler DK, Hur YM, Bouchard TJ Jr, Hassanein RS, Barter R. Migraine in twins raised together and apart. Headache 1998; 38: 417–22. Gervil M, Ulrich V, Kyvik KO, Olesen J, Russell MB. Migraine without aura: a population-based twin study. Ann Neurol 1999; 46: 606–11. Gervil M, Ulrich V, Kaprio J, Olesen J, Russell MB. The relative role of genetic and environmental factors in migraine without aura. Neurology 1999; 53: 995–99. Ulrich V, Gervil M, Kyvik KO, Olesen J, Russell MB. Evidence of a genetic factor in migraine with aura: a population-based Danish twin study. Ann Neurol 1999; 45: 242–46. Waters WE. Migraine: intelligence, social class, and familial prevalence. BMJ 1971; 2: 77–81. Steiner TJ, Guha P, Capildeo R, Rose FC. Migraine in patients attending a migraine clinic: an analysis by computer of age, sex and family history. Headache 1980; 20: 190–95. Baier WK. Genetics of migraine and migraine accompagnee: a study of eighty-one children and their families. Neuropediatrics 1985; 16: 84–91. Mochi M, Sangiorgi S, Cortelli P, et al. Testing models for genetic determination in migraine. Cephalalgia 1993; 13: 389–94. Bille B. A 40-year follow-up of school children with migraine. Cephalalgia 1997; 17: 488–91. Russell MB, Olesen J. Increased familial risk and evidence of genetic factor in migraine. BMJ 1995; 311: 541–44. Stewart WF, Staffa J, Lipton RB, Ottman R. Familial risk of migraine: a population-based study. Ann Neurol 1997; 41: 166–72. Russell MB, Iselius L, Olesen J. Inheritance of migraine investigated by complex segregation analysis. Hum Genet 1995; 96: 726–30. Ulrich V, Russell MB, Ostergaard S, Olesen J. Analysis of 31 families with an apparently autosomal-dominant transmission of migraine with aura in the nuclear family. Am J Med Genet 1997; 74: 395–97. Gambaro G, Anglani F, D’Angelo A. Association studies of genetic polymorphisms and complex disease. Lancet 2000; 355: 308–11. Joutel A, Bousser MG, Biousse V, et al. A gene for familial hemiplegic migraine maps to chromosome 19. Nat Genet 1993; 5: 40–45. Gardner K, Barmada MM, Ptacek LJ, Hoffman EP. A new locus for hemiplegic migraine maps to chromosome 1q31. Neurology 1997; 49: 1231–8. Ducros A, Joutel A, Vahedi K, et al. Mapping of a second locus for familial hemiplegic migraine to 1q21-q23 and evidence of further heterogeneity. Ann Neurol 1997; 42: 885–90. De Waard M, Gurnett CA, Campbell KP. Structural and functional diversity of voltage-activated calcium channels. In: Narahashi T, ed. Ion channels. New York: Plenum Press, 1996: 41–87. Moreno Davila H. Molecular and functional diversity of voltage-gated calcium channels. Ann N Y Acad Sci 1999; 868: 102–17. Lacinova L, Klugbauer N, Hofmann F. Low voltage activated calcium channels: from genes to function. Gen Physiol Biophys 2000; 19: 121–36. Perez-Reyes E. Three for T: molecular analysis of the low voltage-activated calcium channel family. Cell Mol Life Sci 1999; 56: 660–69. Plomp JJ, Vergouwe MN, Van den Maagdenberg AM, Ferrari MD, Frants RR, Molenaar PC. Abnormal transmitter release at neuromuscular junctions of mice carrying the tottering alpha(1A) Ca(2+) channel mutation. Brain 2000; 123: 463–71. Bourinet E, Soong TW, Sutton K, et al. Splicing of 56 57 58 59 60 61 62 63 64 65 66 67 68 69 70 71 72 73 74 75 76 77 78 alpha 1A subunit gene generates phenotypic variants of P- and Q-type calcium channels. Nat Neurosci 1999; 2: 407–15. Zhuchenko O, Bailey J, Bonnen P, et al. Autosomal dominant cerebellar ataxia (SCA6) associated with small polyglutamine expansions in the alpha 1Avoltage-dependent calcium channel. Nat Genet 1997; 15: 62–69. Battistini S, Stenirri S, Piatti M, et al. A new CACNA1A gene mutation in acetazolamideresponsive familial hemiplegic migraine and ataxia. Neurology 1999; 53: 38–43. Carrera P, Piatti M, Stenirri S, et al. Genetic heterogeneity in Italian families with familial hemiplegic migraine. Neurology 1999; 53: 26–33. Ducros A, Denier C, Joutel A, et al. Recurrence of the T666M calcium channel CACNA1A gene mutation in familial hemiplegic migraine with progressive cerebellar ataxia. Am J Hum Genet 1999; 64: 89–98. Friend KL, Crimmins D, Phan TG, et al. Detection of a novel missense mutation and second recurrent mutation in the CACNA1A gene in individuals with EA-2 and FHM. Hum Genet 1999; 105: 261–65. Gardner K, Bernal O, Keegan M, et al. A new mutation in the chr19p calcium channel gene CACNL1A4 causing hemiplegic migraine with ataxia. Neurology 1999; 52 (suppl 2): A115. Kors EE, Terwindt GM, Vermeulen FL, et al. Delayed cerebral edema and fatal coma after minor head trauma: role of the CACNA1A calcium channel subunit gene and relationship with familial hemiplegic migraine. Ann Neurol 2001; 49: 753–60. Takahashi T, Igarashi S, Kimura T, et al. Japanese cases of familial hemiplegic migraine with cerebellar ataxia carrying a T666M mutation in the CACNA1A gene. J Neurol Neurosurg Psychiatry 2002; 72: 676–77. Yue Q, Jen JC, Thwe MM, Nelson SF, Baloh RW. De novo mutation in CACNA1A caused acetazolamideresponsive episodic ataxia. Am J Med Genet 1998; 77: 298–301. Denier C, Ducros A, Vahedi K, et al. High prevalence of CACNA1A truncations and broader clinical spectrum in episodic ataxia type 2. Neurology 1999; 52: 1816–21. Geschwind DH, Perlman S, Figueroa KP, Karrim J, Baloh RW, Pulst SM. Spinocerebellar ataxia type 6: frequency of the mutation and genotype- phenotype correlations. Neurology 1997; 49: 1247–51. Kraus RL, Sinnegger MJ, Glossmann H, Hering S, Striessnig J. Familial hemiplegic migraine mutations change alpha1A Ca2+ channel kinetics. J Biol Chem 1998; 273: 5586–90. Hans M, Luvisetto S, Williams ME, et al. Functional consequences of mutations in the human alpha1A calcium channel subunit linked to familial hemiplegic migraine. J Neurosci 1999; 19: 1610–19. Kraus RL, Sinnegger MJ, Koschak A, et al. Three new familial hemiplegic migraine mutants affect P/Q-type Ca(2+) channel kinetics. J Biol Chem 2000; 275: 9239–43. Guida S, Trettel F, Pagnutti S, et al. Complete loss of P/Q calcium channel activity caused by a CACNA1A missense mutation carried by patients with episodic ataxia type 2. Am J Hum Genet 2001; 68: 759–64. Jen J, Wan J, Graves M, et al. Loss-of-function EA2 mutations are associated with impaired neuromuscular transmission. Neurology 2001; 57: 1843–48. Jun K, Piedras-Renteria ES, Smith SM, et al. Ablation of P/Q-type Ca(2+) channel currents, altered synaptic transmission, and progressive ataxia in mice lacking the alpha(1A)- subunit. Proc Natl Acad Sci USA 1999; 96: 15245–50. Fletcher CF, Lutz CM, O’Sullivan TN, et al. Absence epilepsy in tottering mutant mice is associated with calcium channel defects. Cell 1996; 87: 607–17. Zwingman TA, Neumann PE, Noebels JL, Herrup K. Rocker is a new variant of the voltage-dependent calcium channel gene Cacna1a. J Neurosci 2001; 21: 1169–78. Ducros A, Joutel A, Vahedi K, Bousser MG, Tournier-Lasserve E. Genotype-phenotype correlations in familial hemiplegic migraine. In: Olesen J, Bousser MG, eds. Genetics of headache disorders (frontiers in headache research). New York: Lippincott-Raven, 2000: 123–28. Russell MB, Olesen J. A nosographic analysis of the migraine aura in a general population. Brain 1996; 119: 355-61. Sandor PS, Mascia A, Seidel L, de Pasqua V, Schoenen J. Subclinical cerebellar impairment in the common types of migraine: a three-dimensional analysis of reaching movements. Ann Neurol 2001; 49: 668–72. Ambrosini A, de Noordhout AM, Alagona G, THE LANCET Neurology Vol 1 September 2002 http://neurology.thelancet.com For personal use. Only reproduce with permission from The Lancet Publishing Group. Review Genetics of migraine 79 80 81 82 83 84 85 86 Dalpozzo F, Schoenen J. Impairment of neuromuscular transmission in a subgroup of migraine patients. Neurosci Lett 1999; 276: 201–03. Ambrosini A, Maertens de Noordhout A, Schoenen J. Neuromuscular transmission in migraine: a single-fiber EMG study in clinical subgroups. Neurology 2001; 56: 1038–43. Ambrosini A, de Noordhout AM, Schoenen J. Neuromuscular transmission in migraine patients with prolonged aura. Acta Neurol Belg 2001; 101: 166–70. May A, Ophoff RA, Terwindt GM, et al. Familial hemiplegic migraine locus on 19p13 is involved in the common forms of migraine with and without aura. Hum Genet 1995; 96: 604–08. Nyholt DR, Lea RA, Goadsby PJ, Brimage PJ, Griffiths LR. Familial typical migraine: linkage to chromosome 19p13 and evidence for genetic heterogeneity. Neurology 1998; 50: 1428–32. Terwindt GM, Ophoff RA, van Eijk R, et al. Involvement of the CACNA1A gene containing region on 19p13 in migraine with and without aura. Neurology 2001; 56: 1028–32. Hovatta I, Kallela M, Farkkila M, Peltonen L. Familial migraine: exclusion of the susceptibility gene from the reported locus of familial hemiplegic migraine on 19p. Genomics 1994; 23: 707–09. Monari L, Mochi M, Valentino ML, et al. Searching for migraine genes: exclusion of 290 cM out of the whole human genome. Ital J Neurol Sci 1997; 18: 277–82. Wieser T, Evers S, Gräber S, Günther M, Ziers S, Deufel T. Familial migraine: exclusion of common forms of migraine in four German pedigrees from 87 88 89 90 91 92 93 94 THE LANCET Neurology Vol 1 September 2002 the familial hemiplegic migraine region and the CACNL1A4 gene on chromosome 19p13. In: Olesen J, Bousser MG, eds. Genetics of headache disorders (frontiers in headache research). New York: Lippincott-Raven, 2000: 151–56. Lea RA, Curtain RP, Hutchins C, Brimage PJ, Griffiths LR. Investigation of the CACNA1A gene as a candidate for typical migraine susceptibility. Am J Med Genet 2001; 105: 707–12. Jones KW, Ehm MG, Pericak-Vance MA, Haines JL, Boyd PR, Peroutka SJ. Migraine with aura susceptibility locus on chromosome 19p13 is distinct from the familial hemiplegic migraine locus. Genomics 2001; 78: 150–54. Nyholt DR, Dawkins JL, Brimage PJ, Goadsby PJ, Nicholson GA, Griffiths LR. Evidence for an X-linked genetic component in familial typical migraine. Hum Mol Genet 1998; 7: 459–63. Nyholt DR, Curtain RP, Griffiths LR. Familial typical migraine: significant linkage and localization of a gene to Xq24-28. Hum Genet 2000; 107: 18–23. McCarthy LC, Hosford DA, Riley JH, et al. Singlenucleotide polymorphism alleles in the insulin receptor gene are associated with typical migraine. Genomics 2001; 78: 135–49. Wessman M, Kallela M, Kaunisto MA, et al. A susceptibility locus for migraine with aura, on chromosome 4q24. Am J Hum Genet 2002; 70: 652–62. Lea RA, Shepherd AG, Curtain RP, et al. A typical migraine susceptibility region localizes to chromosome 1q31. Neurogenetics 2002; 4: 17–22. Montagna P. Molecular genetics of migraine headaches: a review. Cephalalgia 2000; 20: 3–14. http://neurology.thelancet.com 95 Peroutka SJ, Wilhoit T, Jones K. Clinical susceptibility to migraine with aura is modified by dopamine D2 receptor (DRD2) NcoI alleles. Neurology 1997; 49: 201–06. 96 Del Zompo M, Cherchi A, Palmas MA, et al. Association between dopamine receptor genes and migraine without aura in a Sardinian sample. Neurology 1998; 51: 781–86. 97 Ogilvie AD, Russell MB, Dhall P, et al. Altered allelic distributions of the serotonin transporter gene in migraine without aura and migraine with aura. Cephalalgia 1998; 18: 23–26. 98 Yilmaz M, Erdal ME, Herken H, Cataloluk O, Barlas O, Bayazit YA. Significance of serotonin transporter gene polymorphism in migraine. J Neurol Sci 2001; 186: 27–30. 99 Emin Erdal M, Herken H, Yilmaz M, Bayazit YA. Significance of the catechol-O-methyltransferase gene polymorphism in migraine. Brain Res Mol Brain Res 2001; 94: 193–96. 100 Tzourio C, El Amrani M, Poirier O, Nicaud V, Bousser MG, Alperovitch A. Association between migraine and endothelin type A receptor (ETA -231 A/G) gene polymorphism. Neurology 2001; 56: 1273–77. 101 Lea RA, Dohy A, Jordan K, Quinlan S, Brimage PJ, Griffiths LR. Evidence for allelic association of the dopamine beta-hydroxylase gene (DBH) with susceptibility to typical migraine. Neurogenetics 2000; 3: 35–40. 102 Kowa H, Yasui K, Takeshima T, Urakami K, Sakai F, Nakashima K. The homozygous C677T mutation in the methylenetetrahydrofolate reductase gene is a genetic risk factor for migraine. Am J Med Genet 2000; 96: 762–64. 293 For personal use. Only reproduce with permission from The Lancet Publishing Group.