* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download cells
DNA vaccination wikipedia , lookup
Complement system wikipedia , lookup
Lymphopoiesis wikipedia , lookup
Monoclonal antibody wikipedia , lookup
Immune system wikipedia , lookup
Psychoneuroimmunology wikipedia , lookup
Molecular mimicry wikipedia , lookup
Adaptive immune system wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
Immunosuppressive drug wikipedia , lookup
Adoptive cell transfer wikipedia , lookup
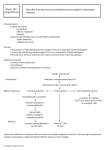
BIOL-723 Immunology 3(2-2) Theory: Comprehensive survey of immunology: cellular and humoral immunity, Inflammation and immune response. Physical and chemical procedures for isolation and characterization of antigens and immune factors. Immunogens and immunogenicity. Immunoglobins-structure, function, gene expression. Cell and organs associated with immune response. Lymphoid cells and markers, cellular cooperation, intracellular messengers, help suppression. The macrophages, immune deficiencies diseases, antigen antibody reactions, complement. Transplantation immunity and immunological tolerance, hypersensitivity and autoimmunity. Practical: Non-specific resistance, blood group determination- slide agglutination. Agglutination reactions-hemagglutination, milk ring test, outerlony test, Immuno-diffusion, immune electrophoresis, current immunoassay (ELISA, RIA, Complementation fixation). Books Recommended: 1. Khan, F. H. 2009. The Elements of Immunology. Pearson Education, London, UK. 2. Coico, R and Sunshine, G. 2009. Immunology: A short course. 6th Ed. Wiley-Blackwell, New York, USA. 3. Paul, W. E. 2008. Fundamental Immunology. Wolters Kluiwer/Lippincoll William & Wilkins, USA. Introduction: The word Immunology owes its origin to the Latin words • Immunitus and • Immunis which are not remotely related to present day immunology Initially in Rome, these words implied “exemption of an individual from service or duty” Later during the middle ages, it came to mean “the exemption of the church and its properties and personnel from civil control” It was Roman poet Marcus Annaeus Lucanus (AD 39-65) first applied the word immunes in the present day biological context Lucas described the resistance to snake bite of the Psylli tribe of North African in his poem Pharsalia Then in the 14th century, Colle used the word to describe his escape from a plague epidemic Although these terms; immunis, immunitas, immunes were used intermittently thereafter, the word immunology attained currency only in 19th century Following the rapid spread of Edward Jenner’s historic technique for small pox vaccination What he did? • He inoculated a young boy with pus from a lesion of a dairy maid who had cowpox, a relatively benign disease that is related to small pox • He than deliberately exposed the boy to small pox • This exposure failed to cause disease Since then , immunity came to be known as the ability of an individual to resist diseases The study of immune reaction was initially referred to as immunochemistry which was coined by Arrhenius, a noted Chemist and Nobel laureate Gradually the meaning of the word immunology evolved to mean an experimental discipline that manipulates the function of the immune system By the start of the 19th century, society as a whole was better prepared to accept and grow with the advancement of science in general and immunology in particular The Components of Immunity: The human body provides two levels of protection from infectious diseases; • Non-specific resistance or innate immunity and • Specific resistance or adaptive immunity Innate Immunity; The non-specific component of immunity also known as innate immunity Latin- innasci i.e. to be born in/inborn It is not directed against any particular pathogen but is a general defense mechanism as the human body must constantly defend itself from a variety of infectious microbes invasion Microbes are viruses, bacteria, fungi, protozoa and multi cellular parasites This defensive mechanism is active right from the time a child is born hence innate The specificity of innate immunity is relatively low as it lacks the ability to distinguish one microbe from another Innate immunity provides the early lines of defense against microbes while adaptive immunity against antigen occurs after five to six days of antigen exposure In general most pathogens encounter by a healthy individual are rapidly cleared within a few days of their entry in to the host body by the nonspecific defenses of the host This occurs much before the full force of the adaptive immune response unlashed The principal components of innate immunity are; • Mechanical and chemical barriers • Phagocytosis • Fever • Inflammation and • Acute phase proteins Mechanical Barriers; A mechanical and physical barrier refers to the various physical hindrances blocking the entry of the microbes into the host body Mechanical barriers include • The skin and • The mucous membrane These barriers act as the first line of defense against infection The Skin; • The skin consists of two distinct layers - the thinner outer epidermis and - the thicker inner dermis - Epidermis consists of several layers of tightly packed epithelial cells - The outer layer of epidermis coated with a tough protein called keratin that does not support viral replication or penetration by bacteria - The inner layer of dermis contains most of the skin’s living structures such as blood vessels, nerve endings, elastic fibers, sweat glands and sebaceous glands - The intact surface of the healthy epidermis provides an excellent defense against penetration by bacteria or viruses - Moreover, the epidermis of the skin is constantly shed off, resulting in the continual removal of any clinging pathogens - Any break in the integrity of the skin facilitates the entry of pathogen - The bacteria that are most likely to cause dermal infection under such conditions are those that infect hair follicles. For example Staphylococci - Some viruses such as Papillomoviruses – produce human warts, enter the skin at sites where cuts and abrasions have resulted in the loss of epithelial integrity - The skin is also penetrated by insect bites. For example mosquitoes, ticks, fleas and flies - Pathogen infected arthropods introduce the pathogen in to the host - Plasmodium, the causative agent of malaria, is introduced in to the human body by mosquito bites - Similarly, viruses such as human Papillomaviruses, Myxomavirus and Flaviviruses are introduced in the host by arthropod vector during feeding Mucous Membrane; • The regions of the body that are not protected by intact skin are lined by the mucous membrane • The gastrointestinal tract, respiratory tract, urogenital tract and conjunctiva (inner eyelid and parts of eyeball) - all are lined by the mucous membrane • The mucous membrane protects the human body in several ways • In the respiratory tract, goblet cells secret mucous that entraps dust and microbes and is propelled by the action of ciliated epithelial cells, thereby clearing foreign material from the respiratory tract • The mucous membrane of the gastrointestinal tract offers the same protection • Some mechanical factors that assist in protecting the mucous membrane include - The lavaging (process of washing out an organ of the body) action of physiological fluids. For example tears, saliva - that assist in flushing microbes from the body - The trapping action of mucous-coated hair in the anterior chambers of the nose - The expulsive effects of coughing and sneezing, which protect the respiratory and gastrointestinal tracts and - The cool temperature of the upper respiratory tract which inhibits replication by many viruses • However, the protection provided by the mucous membrane against pathogenic invasion is not enough • The mere ingestion of typhoid bacilli or tubercle bacilli or picornaviruses is sufficient numbers will lead to penetration of gastrointestinal mucosa • A similar penetration of the conjunctiva by Leptospira or adenoviruses and of the respiratory tract by Pneumococci or Rhinoviruses (Rhino is from Greek word rhin indicating nose or nasal- The common cold virus is example of rhinovirus), can occur following a heavy exposure to these pathogens Chemical Barriers; • Mechanical barriers alone do not account for the remarkable resistance provided by the innate defense mechanism to pathogenic invasion • Host body has several chemical/physiological barriers that contribute to innate immunity • These include - Acidic gastric secretions - Low pH of the skin - Lysozyme - Gastric and duodenal enzymes • - Antibodies and inhibitors - Interferones - Complement proteins - Antimicrobial peptides Acid Gastric Secretions; - The physiological environment in the stomach appears to be extremely inhospitable/not friendly to invading pathogens - Why? - The secretion of hydrochloric acid by gastric parietal cells maintains the pH of the stomach at 2.0 - This kills most microorganisms except some resistance ones such as Hepatitis A virus Picornaviruses and Typhoid bacilli • Low pH of the Skin; - Sebum secreted by the sebaceous glands present in the dermis contains organic acids • • - These organic acids maintain the pH of the skin in the range of 3-5 - This low pH inhibits or retards the growth of most microorganisms present on the surface of the skin Lysozyme; - It is a hydrolytic enzyme present in all mucous secretions including tears, saliva and nasal secretion - It can lyse Gram-positive bacteria by cleaving the peptidoglycan layer found in the bacterial cell wall Gastric and Duodenal Enzymes; - A large array of enzymes including proteases and lipases digests a variety of structural and metabolic chemical components of pathogens - For example - Rhinoviruses are easily inactivated by gastric acids - However, in rare cases, the infectivity of the pathogen is increased by acidity - For example – the infectivity of Coronavirus is enhanced by an acid environment • • • Antibodies and Inhibitors; - The mucous secreted by gastric and intestinal cells usually contains antibodies IgA molecules as well as non-specific inhibitors of viral infections - For example sialic acid found in mucous, inhibits the attachment of influenza virus particles to cells - Antibodies (IgA) are also found in tears and saliva - Secretary IgA protects the body surface against invading pathogenic microbes Interferons; - This name refers to a group of proteins produced by virus-infected cells that induce a generalized antiviral state in neighbouring uninfected cells - These proteins also augment innate immunity Complement Proteins; - These are a group of serum proteins that circulate in an inactive state in the plasma - A variety of specific and non-specific mechanisms activate these proteins • The activated forms of these proteins damage the invading pathogen Antimicrobial Peptides; - All insects and mammals including human secrete a number of antimicrobial peptides such as defensins for protection - The human body is protected by 1 μm thick bioflim of defensins - That protects the external surface of the body from microbial assault Fig 1.1 Roitt 6th Ed/Fig 1.5 Roitt 7th Ed Fig 1.2 Khan 2009 Phagocytosis: Phgocytosis of invading microorganisms is another important innate defense mechanism Phagocytosis can be defined as ligand-induced uptake of particular material of 150-200 nm diameter or more This basically includes large particles such as cell debris and microbial cells When bacteria or other invading parasites penetrate the skin or the mucous membrane, phagocytes such as • Neutrophils • Blood monocytes and • Tissue macrophages surge towards the site of infection These phagocytes engulf the bacteria to form a large intracellular vesicle containing bacteria. These are called phagosome Fig 1.3 Khan 2009 Phagocytosis is non-specific and is different from specific receptormediated endocytosis wherein extracellular molecules are ingested after they bind to specific receptor Phagocytosis is also different from pinocytosis – the mechanism by which cells take up fluids and dissolved solutes from the surrounding medium Phagocytes must be selective of cells and material they phagocytose Otherwise normal cellular structures would be ingested The occurrence of phagocytosis depends on the following factors: - Presence of strong electrical charge - Presence of antibodies and complement components on the cell surface - Surface of the particle Fever; Fever is the condition of an abnormally high body temperature, accompanied by increased pulse rate and dry skin It provides non-specific defense against disease Fever is physiological response to infection Many proteins and breakdown products of proteins, toxins and lipopolysaccharides, particularly from Gram-negative bacteria, released by microbes can affect the endothelial cells of the hypothalamus to raise the body temperature from its “set point” of 36.5oC Such substances that increase the body temperature are called pyrogens Gram-positive bacteria release a class of very potent endotoxins called endogenous pyrogens Just few nanograms of endogenous pyrogens can cause very high fever This class of molecules is released when either the bacteria or its breakdown product bind to macrophages and neutrophils These cells then release several cytokines like IL-1β, TNF-α and IL-6 that act on the hypothalamus to produce fever Fever is beneficial to the host because it inhibits the growth of temperature sensitive pathogen It also increased cell metabolism encourages rapid tissue repair and phagocytosis Fig 1.4 Khan 2009 Inflammation; It is the reaction of living tissue to either an injury or an infection It is characterized by • Heat • Redness • Swelling • Pain It is non-specific response of the body to injury The tissue injury could be caused by either mechanical agents such as • Cuts or pinprick Chemical agents such as • bee venom, acid or alkali Physical agents such as • Heat or ultraviolet radiation and Besides these infectious agents such as • Bacteria or other pathogens can also induce inflammation The process of inflammation may be initiated by a variety of tissue products such as: • Histamine • Bradykinin • Serotonin and • Prostaglandins released by a numbers of cells such as - Mast cells and - Basophils found in most tissues The mediators released by damaged cells Chemicals released by invading microorganisms Products of the complement system and Reaction products of blood clotting system also trigger the process of inflammation Many of these substance strongly activate macrophages and other cells of the phagocytic system However, the inflammatory response occurs in several different stages Fig 1.5 Khan 2009 Attack by Tissue Macrophages • Macrophages already present in the tissues: - The alveolar macrophages in lungs - Histocytes in subcutaneous tissue - Kupffer cells in liver - Microgalia in brain Fig 1.5 Roitt 6th Ed/ Fig 1.2 Roitt 7th Ed • However, initially tissue macrophages are present in small numbers • In the case of inflammation, these macrophages immediately proceed towards the injury site to begin their phagocytic actions • Therefore, they serve as first line of defense • The next step in inflammation is the redirection of blood phagocytes towards the lesion site • This is facilitated by vasodilation of blood vessels and capillaries at the site of injury • The increase in diameter of blood vessels is brought about by chemical mediators like - Histamine and - Bradykinins • These mediators bind to the receptors on nearby capillaries and vessels, causing vasodilation • The engorged capillaries are responsible for increased blood accumulation and the redness of the inflamed tissue -erythema • The increased permeability of the capillaries permits the influx of fluid from the engorged capillaries in to the site of irritation or injury • The accumulation of fluid at the site of irritation results in tissue swelling –oedema Margination and Diapedesis • The products release from inflamed area also cause phagocytes now mainly neutrophils to move towards the inflamed area • A process facilitated by vasodilation of the cells to the capillary walls • This process is called margination • The adhered phagocytes then pass from the blood vessels in to tissue spaces through the spaces between capillary endothelial cells • This process is called diapedesis • Once in the tissue spaces, the phagocytes migrate towards the injured tissue • Once phagocytes engulf the invading bacteria and the necrotic tissue, many phagocytes eventually die • However, some enzymes may leak out in to the extracellular environment from the neutrophils before the phagosome closes • This process termed sloppy eating and damages healthy cells • After a few days, a cavity containing - necrotic tissue - dead bacteria and - dead phagocytes is formed at the site of inflammation • This fluid mixture is often called pus. This pus formation continue until all infection is suppressed • The blood clotting system also activated in the inflamed region which results in the deposition of insoluble strands of fibrin • • This seals off the injured area from rest of the body, thereby preventing the spread of infection • This pus enclosed in a wall of fibrin, usually forms an opening on the surface of the body, from where it empties out • The fibrin clot dissolves, tissue repair occurs and scar tissue is formed Acute Phase Proteins; These are a group of heterogeneous proteins that are important in the innate defense against microorganisms mostly bacteria and protozoa and in Limiting the damage caused by infection, trauma, malignancy and other diseases to tissues In response to tissue insult, cells circulating in the blood such as • Macrophages and • Neutrophils secrete a variety of cytokines that stimulate the liver to produce acute phase proteins • Important acute phase proteins include - C-reactive complement protein (CRP) - Mannose binding metal protein (MBP) - Binding proteins and - Protease inhibitors Acute phase proteins function by • stimulating phagocytosis acting as opsonins - such as an antibody or a complement fragment that binds on an antigen surface and promotes phagocytosis • activating the complement system and clumping the invading microbes All these help in the non-specific removal of pathogens CRPs have aesthetically designed pentagonal structure to clump bacteria (Pneumococci) that bear C proteins on their surface CRPs are present in primitive invertebrates MBP binds to the mannose residue of glycolipids present on the surface of protozoan and microbial cells and activate the complement system Complement components that act as acute-phase proteins act as opsonins as well These complement proteins coat the invading microbes making them susceptible to phagocytosis Table 1.1 Khan 2009 In addition to soluble molecules of the innate immune system, an increasing number of cell-surface receptors present on a variety of cells in the human body also provides a major defense against invading pathogens The receptors are called pattern-recognition receptors (PRR) Fig 1.6 Khan 2009 PRRs comprise a group of proteins that are used by cells of immune system to identify conserved molecules common to pathogens Though they do not have the absolute specificity of lymphocytes, they have evolved to recognize molecular patterns associated with different types of pathogens These structures on microbes called pathogen-associated molecular pattern (PAMP) Examples of PAMPs include bacterial molecules such as • Peptidoglycanes • teichoic acid • Lipopolysaccharide • flagellins and • viral double-stranded RNA PRR include • Toll receptors - bind to lipopolysaccharide and bacterial lipoprotein among others • CD14 - binds lipopolysaccharides • Mannose receptors- specific for mannose and fucose and • Scavenger receptors – bind lipids/carbohydrates, lipopolysaccharide and lipteichoic acid These receptors have been identified on • Macrophages • B cells and • Dendrite cells Table 1.2 Khan 2009 Adaptive Immunity : In contrast to innate immunity, adaptive immunity is a more evolved and specific defense mechanism The characteristics of adaptive immunity are • Exquisite antigenic specificity and • The ability to “remember” different types of antigens Adaptive immunity is activated only against • Invading foreign material and • Never against its own molecules except in autoimmune diseases Therefore, it has the ability to distinguish between self and non-self Because it can differentiate between a variety of • Different antigens • Invading pathogens and self antigens and induce different levels/types of immune response Therefore, adaptive immunity is also called as specific/acquired immunity But adaptive immunity is not independent of innate immunity Adaptive and innate immunity cooperate to produce a more • Effective • Evolved and • Vast defense mechanism against infectious agents. For example; Phagocytes, a crucial part of innate defense generate “signals” that stimulate specific immune response In turn, this facilitates the participation of the specific immune system in the destruction and elimination of pathogens The adaptive immune system produces various soluble factors that • stimulate and • increase the effectiveness of innate immune response For example, some T cells synthesize and secrete soluble factors that increase the ability of macrophages to kill the microbes they engulfed Thus both the adaptive and innate immune responses make up an • integrated and interactive system of host defense that provides an • effective and formidable barrier to infection Some important characteristics of the innate and adaptive system Table 1.3 Khan 2009 Cells of Immune System; An effective immune response is mediated by a variety of cells including • neutrophils • Lymphocytes • natural killer (NK) cells • eosinophils • basophils and • antigen-presenting cells Fig 1.1 Roitt 7th Ed The two main groups of cells are • Lymphocytes and • Antigen presenting cells Lymphocytes are mainly responsible for initiating adaptive immune response in human body • All lymphocytes are produced in bone marrow stem cells by a process called haematopoeisis • Two major populations of lymphocytes are: - T lymphocytes – develop in the thymus and - B lymphocytes – develop in bone marrow B Lymphocytes; • B lymphocytes as mentioned earlier originate in the bone marrow where they continue to differentiate and mature • Each B lymphocyte is programmed to encode a unique antigenbinding receptor on its membrane • This B-cell receptor is actually a membrane bound antibody molecule Fig 1.7 Khan 2009 • When a naïve B cell that has not been previously encountered antigen, comes in contact with an antigen via its membrane-bound antibody • It multiplies and differentiates in two types of cells - plasma cells and - memory cells • Plasma cells lack B-cell receptors • But they produce large numbers of soluble molecules –antibodies • B-cell receptors and antibodies differ only at their C terminal • B-cell receptors have an additional transmembrane segment at their Cterminal that anchors them to the cell membrane • Antibody molecule is a large, polyfunctional glycoprotein found in blood and other tissue fluids • Plasma cells have few days life • Memory B-cells have a longer life-sometimes up to 20 years • In human B-cells last for several months • Memory cells express some membrane-bound antibody molecule like their parent naïve cells • Memory cells are functionally in active unless they are stimulated by the same antigen again T Lymphocytes; • As mentioned they are produced in the bone marrow but they migrate to the thymus to mature • During maturation, each T cell acquire a specific receptor on its membrane termed as the T-cell receptor Fig 1.7 Khan 2009 • A T-cell receptor does not recognize soluble antigens • It recognizes antigens only when they are associated with a protein complex called major histocompatibility complex (MHC) • What are MHCs? • These are diverse transmembrane glycoproteins present on a variety of cells • These molecules present the antigens to the cells of the immune system • MHC molecules are named because they were first identified as “antigens” responsible for the • - acceptance or - rejection of tissue grafts i.e. histocompatibility Three classes of MHC proteins: i. Class I MHC molecules are expressed on nearly all nucleated cells and present antigenic determinants to a specific class of effector T cells ii. Class II MHC molecules are expressed only on antigenpresenting cells and present antigen to the other class of effector T cells iii. Class III MHC molecules are of diverse types and are directly or indirectly involve in the immune response • There are several different groups of T cells i. One group interacts with antigen-class II MHC molecule complex, gets activated and start secreting cytokines – called T helper (TH) cells. They activate B cells via cytokines and help them to divide, differentiate and secrete antibody molecules ii. Another group of T cells is responsible for the destruction of - virus-infected host cells - intracellular pathogens harboring host cells - tumor cells and - cells of a foreign tissue graft are called cytotoxic T (Tcyt) cell and recognize an antigen when it is associated with class I MHC molecules - As pointed out earlier that T cell recognize antigens only when they are presented in association with MHC molecules - The receptor that recognizes an antigen-MHC complex is present on the cell membrane of T cells and it called Tcell receptor (TCR) Antigen-Presenting Cells; • Any cell that is capable of processing and presenting antigens to the cells of the immune system may be called as antigen-presenting cell • But this term is used only for those cells that display antigen associated with class II MHC molecules • These antigen presenting cells present antigens to TH cells • Antigen-presenting cells include - dendritic cells (interdigitating) - macrophages and - B lymphocytes Fig 1.8 Khan 2009 • Antigen presenting cells take up antigens either by - endocytosis or - phagocytosis • The internalized antigen is then degraded and processed • Small peptides derived from antigen processing are then displayed on the surface of the antigen-presenting cells in association with class II MHC molecules • This antigen-class II MHC complex is recognized by TH cells • This binding with TH cell also activates antigen-presenting cells • Which produces signal molecules (cytokines) that lead to the activation of the TH cell which further augment the immune response Natural Killer Cells; • NK cells play an important role in immune surveillance and innate immunity • These large granular cell are called natural killer cells • Because they have natural “instinct” to kill tumor or virus infected cells without prior immunization • It is believed that NK cells recognize cells that have lost class I MHC molecules from their surface • Many surface changes occur on tumor cell and some virus-infected cells including loss of class I MHC molecules • NK cells recognize and damage these class I-MHC-negative cells very effectively Eosinophils; • These are specialized group of leukocytes that are weak phagocytes exhibiting chemotaxis • These are produced in large numbers in individuals with parasitic infections • Sometimes when a parasite is too big to be phagocytosed such as schistosomes or flatworms • They attached themselves to these parasites and release their intracellular granular contents that contain several toxic proteins to kill the parasite Basophiles and Mast Cells; • Basophiles circulating in the blood are very similar though not identical to the large mast cells • Which are located outside many blood capillaries mainly in tissues • Both these cells have stored granules that contain a variety of molecules capable of triggering inflammation upon their release • These mediators are released when the cells are activated • Basophiles and mast cells have bound antibody (IgE) molecules on their surface • These binding and cross linking of these antibody molecules by an allergen stimulates the release of pharmacologically active granules that are stored in basophile/mast cells • These granules elicit symptoms to an allergic reaction when released inside the host body Mononuclear Phagocytes; • The mononuclear phagocyte system comprise blood monocytes and tissue macrophages (histocytes) • Monocytes are incompletely differentiated cells that circulate in blood • These are referred to as macrophages when they migrate through blood vessels and are sequestered in to the surrounding organs and connective tissues • These are derived from the myeloid lineage of bone marrow stem cells • These cells are also very effective at presenting antigens to T lymphocytes Fig from Science ? Neutrophils; • It is another important short lived phagocyte that has a multilobed nucleus and often referred as polymorphonuclear neutrophil (PMN) • Neutrophils express Fc receptors for antibodies –receptor that binds to the Fc region of the antibody and • Receptors for complement proteins that help to phagocytose the opsonized bacteria Fig 10.13 Glick 3rd Ed • These cells are also involved in inflammation and migrate from blood vessels into inflamed tissue in response to chemical signals received from lesion site • But these will die after phagocyting 5-20 bacteria – probably by the action of variety of lytic enzymes released near the neutrophils during phagocytosis • Thus neutrophils are short lived cells Antigen and Antigen Recognition: • An antigen can be defined as any macromolecule which is capable of inducing B cells to produce specific antibody molecules • Now its usage is broadened to include any molecule that can be specifically recognized by either B cells or T cells or both • Antigen is not recognized as a whole by either B or T lymphocytes • Instead, each lymphocyte receptor/antibody binds to a small or restricted part of the antigen called antigenic determinant i.e. the region that determines antigenicity or epitope • A particular antigen can have several different antigenic determinants on its surface or the same antigenic determinant may be repeated several times Fig 9.2 Glick 3rd Ed • B cell receptors, antibody molecules and T cell receptors are specific for a particular antigenic determinant rather that the whole antigen • B lymphocytes express on their surface, antibody molecule that can recognize only a specific antigen • T lymphocytes which is responsible for cell-mediated immunity, express receptors that recognize short peptide sequences only when these sequences are associated with MHC molecules present on surface of the cell • Thus humoral immunity recognizes various foreign proteins, polysaccharides, lipids, toxins and lipopolysaccharides released by invading pathogens in to the blood stream • In contrast, cell-mediated immunity recognizes antigenic determinants displaced on self-cells and altered self-cells by MHC molecules like tumor cells or virus infected cells MHC and Antigen Presentation: • The major histocompatibility complex (MHC) consists of approximately 15 different genes • Most of them highly polymorphic – over 500 different alleles of MHC have been identified • Initially, these gens were identified as their gene products – proteins and were responsible for the acceptance or rejection of tissue grafts – histocompatible. For example: • If two mice had the same MHC alleles like identical twins, the tissue graft was accepted • However, the same graft was rapidly rejected if the two mice were of different strains • MHC proteins are membrane bound glycoproteins and can be grouped in to two major classes and important ones . These are members immunoglobulin super family as they contain Ig-like domain: • - Class I and - Class II (Though there is also Class III) With somewhat different structure and functions Fig 1.9 Khan 2009 Processing of Endogenous Antigens; • Antigens located in the cytosol of the cells are degraded by proteases of the proteasome complex • Two common examples of endogenous antigens are: - viral proteins synthesized inside virus-infected cells and - unique proteins synthesized by cancerous cells • These proteins are degraded in to 8-15 residue long fragments that are suitable for binding to the groove of class I MHC molecules • These peptides that are generated in the cytosol, are transported in to the lumen of the endoplasmic reticulum (ER) by a peptide transporter called transporter of antigenic peptide (TAP) located in the membrane of the ER Fig 1.10 Khan 2009 Processing of Exogenous Antigens; • Exogenous antigens are produced/present outside the host cell and enter the cells via - phagocytosis or - endocytosis • Antigen presenting cells such as macrophages ingest and degrade antigens in the endosomal or lysosomal compartment by acid proteases • The peptides generated within the lysosome are 13-18 residues long, slightly longer than those generated by proteasomes • These 13-18 residue peptides then fuse with the endocytic vesicle containing class II MHC molecules • The antigenic peptide binds to the cleft within the class II MHC molecule and this complex then moves to the cell membrane where it is displayed • Since only antigen presenting cells predominantly display class II MHC molecules, the presentation of exogenous antigens is limited to these cells • TH cells recognize antigen only when it is associated with class II MHC molecules • Thus are said to be class-II-MHC-restricted • Therefore TH cells are activated primarily by exogenous (extracellular) antigens such as - bacterial toxins or - those that are part of bacterial cell walls Types of Immune Response: The specific immune response normally stimulated when the host is exposed to invading microbes over a period of time This form of immunity called active immunity In which the immune system of the host plays an active role in responding to the foreign antigen However, specific immunity can also be conferred upon an individual by transferring cells or serum from specially immunized individuals or animals This form of immunity is called passive immunity This makes the recipient individual immune to a particular antigen or pathogen without even being exposed to it Passive immunization is usually used against those pathogens or toxins which act so rapidly and in most cases lethally that the affected individual is unable to mount an active and effective immune response Immune response can also be classified as antibody-mediated or cellmediated depending on which effector arm of the immune system is stimulated Antibody-Mediated Immunity; Antibody-mediated immunity is mediated by B cells and antibodies These antibodies react with • Pathogens like bacteria and viruses • Soluble antigens • Toxins and • Foreign cells within the body Antibodies function • by binding to pathogens or toxins • neutralizing them and • facilitating their elimination Pathogens and foreign cells coated with antibodies • can be killed by proteins of the complement system • Can be readily ingested by phagocyte Fig 1.11 Khan 2009 Toxins are neutralized by antitoxin antibodies Antibody-mediated immunity is commonly called humoral immunity as it is centered around antibodies which are found primarily in the blood Blood was one of the four humors formerly thought to constitute the body Cell-mediated Immunity; Cells of the immune system are directly involved in conferring cellmediated immunity The effector T lymphocytes that are generated during cell-mediated immunity are TH cells and Tcyt Tcyt lymphocytes play a key role in killing • virus infected cells • Transplanted cells and • Tumor cells While TH cells can activate various phagocytic cells enabling them to • Phagocytose and kill microbes effectively TH cells also activate humoral response simultaneously Thus while antibody-mediated immunity is the principal defense mechanism against • Toxins • Bacteria • Viruses or • foreign cells in the blood stream Cell-mediated immunity is primarily directed against intracellular microbes such as • Viruses and some bacteria that survive and proliferate inside host cells where they are inaccessible to circulating antibodies Activation of the Immune Response: There are two arms of the immune response • Humoral response mediated by B cells and antibodies and • Cell-mediated response effected by T cells Humoral Response; Antigen specific recognition by lymphocytes induces two major changes in lymphocytes • Proliferation and • Differentiation The initial development of antigen-specific clones of lymphocytes occurs before a lymphocyte ever encounters an antigen As B cells mature in the bone marrow, random gene shuffling occurs in the gene segment that code for antibody molecules Ultimately each mature B cell possesses a single active gene for each light and heavy chain Therefore the B cells produce and display one type of antibody i.e. antibody of single specificity on its membrane But different cells in a population of B lymphocytes undergo different genome rearrangements leading to the production of different antibody molecules by B cells There are about 105 antibody molecules displayed on a given B cell, all having the same specificity Each B lymphocyte and its clone show a distinct specificity for a particular antigenic determinant The number of antigenic determinants that can be recognized by the human B cell repertoire is estimated to be 109 to 1011 This huge diversity in the population of mature B cells is subsequently reduced by a screening process that eliminates any B cell that recognizes self antigens This selection process ensures that antibodies that react with self-antigens are not produced Similarly T cell maturation involves rearrangements of a series of gene segments that encode T-cell receptor Each T lymphocyte expresses about 105 receptors on its surface and the number of antigenic specificities recognized by T cell receptors of the entire human immune system is of the order of 1015 This enormous repertoire of T cells is diminished through selection process in the thymus that ensures that any T cell capable of reacting with self antigen is eliminated The antigen selects a specific pre-existing clone by binding to the membrane-bound receptor i.e. mature B cell or T cell leading to a proliferation of cells with a given antigenic specificity In this process an antigen binds to a particular T or B cell and stimulates it to divide repeatedly into a clone of cells, each with antigenic specificity identical to that of the original parent cell- clonal selection These antigen stimulated clones start differentiating into effector plasma cells and memory cells Memory B cells appear to have a longer lifespan than the naïve lymphocytes from which they arise Though antigens bind and stimulate membrane receptors of B cells very rapidly, antibody levels in plasma start to increase after a week of antigen exposure What could be the possible reasons for this? This could be due to: - time required for expansion of clone of B lymphocytes in to plasma cells - time required for TH cell-induced B-cell proliferation and differentiation This initial and slightly delayed immune response that occurs after the initial antigen exposure - primary response It peaks in approximately 14 days, when it shows highest antibody concentration and then slowly starts to decline as plasma cells produces after initial antigen exposure begins to die Subsequent contact with the same antigen elicits a faster, stronger and sustained immune response with s shorter lag period of one to two days and results in much higher antibody levels - secondary response This is due the presence of large number of memory cells generated after the first antigenic exposure The increased antibody levels in secondary immune response is primarily due to the fact that there are more memory B cells than naïve B cells that can be stimulated The short lag period is due to the fact that memory B cells respond to antigen more quickly as compared to naïve B cells As memory cells are stimulated, they again divide to produce a progeny of memory cells and antibody-secreting plasma cells and consequently antibody level rise between 100 and 1,000 fold The memory cells continue to live for weeks, months or even years while plasma cells die after few days Selective Activation of B Cells and Generation of Humoral Response; Typically B cells make antibodies in two forms: • Secretary and • Membrane bound A membrane bound antibody, called a B-cell receptor, is attached to the cell surface by a transmembrane tail present at the C terminal of its Fc region This leaves the combining site on Fab region free to bind antigens The binding of antigens to these antibody molecules on the surface of B cell triggers its activation and proliferation Antigen binding cross-links membrane-bound antibody molecules resulting in their internalization of receptor-mediated endocytosis After endocytosis, the antigen is partially digested / processed The resulting peptides are combined with class II MHC or class I MHC molecules on their membrane The antigen-class II MHC complex is recognized by specific TH cells The stimulated TH cells secrete a variety of cytokines that stimulate various stages of B-cell division and differentiation These cytokines expand the population of the B cells specific for the invading antigen This increased population of B cells then differentiates in to antibody-secreting plasma cells and memory cells Fig 1.12 Khan 2009 Cell-Mediated Response; Cell mediated immunity which is centered on T lymphocytes, respond to cells infected with pathogens such as • viruses and • bacteria As pointed out earlier that T lymphocytes recognize short peptide sequences only when these peptides sequences are associated with MHC molecules and displayed on the cell surface This peptide-MHC complex acts as a signpost that is recognized by T lymphocytes The recognition of an antigen-MHC complex by a mature, specific T lymphocyte activates these lymphocytes Activated lymphocytes undergo proliferatrion and differentiation in to various types of effector (TH and Tcyt) and memory T cells Memory T cells have longer half life than naïve T cells and are more easily activated than naïve cells Short lived effector cells perform either helper or cytotoxic functions For example Tcyt cell binds to antigenic peptides that are associated with class I MHC molecules on the membrane of the altered self cell The self-cell can be altered by a viral or bacterial infection or by tumor Tcyt cell mediates the specific killing of these altered cells Fig 1.13 Khan 2009 The cytokines secreted by specific TH cell stimulate proliferation and differentiation of T cells forming memory Tcyt cells TH cells are stimulated upon binding to antigen-class II MHC complex present on antigen presenting cells This activation of TH cells causes rapid proliferation and differentiation in to effector TH cells and memory TH cells This clonally expanded population of antigen-specific TH cells is actively engaged in stimulating B and T lymphocytes, thereby generating effective humoral and cell-mediated responses Apart from stimulating B and T lymphocytes, the cytokines secreted by TH cells also activates non-specific effector cells that play different roles in cell-mediated response These cells which include macrophages, neutrophils and NK cells play a significant role in phagocytosing pathogens or lysing virusinfected cells or tumor cells non-specifically These phagocytes and NK cells serve as the non-specific effector arm of cell-mediated immunity A specific class of TH cells is the delayed type hypersensitivity cells (TDTH) which are usually helper T cell of TH1 type These cells are involved in a specific type of hypersensitivity reaction called delayed-type hypersensitivity This is a form of cell-mediated immune reaction and is designed as a primary defense against intracellular bacteria that may survive within phagolysosomes or in the cytosol of the host cell such as monocyte However, if the antigen is not cleared from the system, prolonged delayed-type hypersensitivity response can become destructive to the host as the intense inflammatory response that ensues can damage blood vessels and cause extensive tissue necrosis Immune Disorders: The immune system, complete with its innate and specific immunity, is almost a flawless asset, protecting the body against pathogenic invasion and cancer However, there are several occasions when the immune system misdirects itself causing a disease or other undesirable consequences The immune system can be compromised in one of the following three ways: • autoimmunity • immunodeficiency and • hypersensitivity Autoimmunity; Normally the immune system recognize all foreign antigens and reacts against them The immune system does not attack to its own cells and molecules So in actual immune system is tolerant towards the self Sometimes this tolerance mechanism breaks down leading to the production of auto antibodies and auto reactive T cells that cause tissue damage and induce pathogenesis As a result the body mounts an immune response against itself and This is when autoimmune disease occurs Examples: - Multiple sclerosis in which antibodies / T cells are formed against components of the myelin sheath of the nerve cells. This immunological attack interferes with the conduction of nerve impulse causing severe and progressive neurological damage - Rheumatoid arthritis is characterized by the attack of B and T lymphocytes on the joints due to a series of inflammatory responses. The destruction of cartilage and bone occurs which causes pain and finally results in the immobilization of joints - Garves’ disease is characterized by an immune response against the thyroid-stimulating hormone (TSH) receptors present on thyroid cells. The binding of antibodies of TSH receptors causes continual stimulation of these receptors resulting in hyperthyroidism - Thyroiditis develops from an immune attack against one or more proteins of the thyroid cells. The destruction of the thyroid gland leads to hypothyroidism - Others include insulin dependent diabetes mellitus, systemic lupus erythematosus (SLE) and pernicious anemia Immunodeficiency; There are following four elements of immune system that function together to protect the body; - T cells, B cells, phagocytes and complements If any of these elements is defective since birth i.e. primary immunodeficiency or become defective subsequently i.e. secondary or acquired deficiency, the individual may not be able to fight infections properly Examples of primary immunodeficiency include - Complement deficiencies - DiGeorge syndrome (defective T cell development) and - Neutropenia (few neutrophils) Example is acquired immuno- deficiency syndrome (AIDS) caused by the human immunodeficiency virus (HIV) - a retrovirus Hypersensitivity; It is an abnormal state of heightened immune response that damage the normal tissues of the host body In other words hypersensitivity is the outcome of the over reaction of the immune system The antigen, here referred to as allergen could be anything i.e. from pathogens to pollen grains to innocuous food molecules Hypersensitivity reactions cause substantial damage to unsuspecting individual Examples include - Atopy (allergy to environmental allergens) - Anaphylaxis and - Serum sickness At times, the immune system acts normally yet inconveniences the individual Examples are: - Blood transfusion and - Graft rejection In case of blood transfusion and organ grafting from incompatible or mismatched donors, the ordinary immune reaction that ensues can lead to life threatening consequences Therefore it is very important to carefully match donor and recipient blood in blood transfusion or tissue in tissue grafting to avoid rejection However, these problems are a small price to pay for the constant and vast protection provided by the immune system Evolution of Immunity: The vertebrate immune system probably evolved from the primitive cellsurface molecules that were involved in cell-cell interaction The duplication and divergence of this primordial recognition system led to the development of an immune system that resembled the T lymphocyte system It seems plausible that the B-lymphocyte system and antibodies arose from this recognition system, librated from the constraint of interaction with the MHC proteins It is wrongly assumes that the presence of a defense mechanism against pathogen invasion is limited only to vertebrate Though occurrence of antibodies, B cells and T cells are limited to vertebrates alone, it would be a mistake to assume that even a non-adaptive immunity i.e. innate immunity does not occur in invertebrates A rich variety of mechanisms that can distinguish self from non-self antigens and provide a non-specific barrier to the entry of pathogens has evolved Table 1.4 Khan 2009 The non-specific barrier of invertebrates includes mucous that surrounds the body of coelenterates and annelids The presence of a tough exoskeleton, such as shell forms a mechanical barrier in the case of arthropods, echinoderms and mollusks Other barriers include plasma gelation in arthropods (akin to vertebrate blood coagulations) at the site of injury to prevent the fatal loss of body fluids and phagocytosis by leukocytes (different from mammalian leukocytes) facilitated by lectins (akin to antibody) that coat the foreign invader If the pathogens to be phagocytosed are too large or too many in number, they are encapsulated (as in arthropods) in a multi cellular aggregate Sequestered organisms are killed by lysosomal enzymes, lysosomes, reactive oxygen species and reactive nitrogen species released by surrounding invertebrate leukocytes The body fluids of invertebrates contain various factors that have strong antibacterial and antimicrobial activity. These include: • agglutinins • Lysozymes • Non-lysozyme bactericidins • Lysosomal enzymes and antimicrobial proteins Antibacterial / antimicrobial proteins found in insects such as moths, flies and bees can be induces with in few hours of an antigen injection One such factor i.e. Cecropin A found in silk moths shows approximately 40 % homology with immunoglobulin domain and could represent a primitive form of immunoglobulin Surprisingly plant which diverged from vertebrates at least a billion years ago also respond to invading pathogens by producing a wide variety of antimicrobial peptides and non-peptide organic molecules that kill the pathogen This chapter provides a bird’s eye view of important components of the immune system