* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Innate immunity
Herd immunity wikipedia , lookup
Monoclonal antibody wikipedia , lookup
Social immunity wikipedia , lookup
Hygiene hypothesis wikipedia , lookup
Molecular mimicry wikipedia , lookup
Lymphopoiesis wikipedia , lookup
Complement system wikipedia , lookup
Polyclonal B cell response wikipedia , lookup
Immune system wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
Adoptive cell transfer wikipedia , lookup
Adaptive immune system wikipedia , lookup
Psychoneuroimmunology wikipedia , lookup
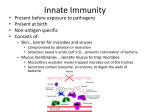
Welcome to the lecture series INTRODUCTION TO IMMUNOLOGY Valerio Izzi, Ph.D. 1 Key literature • Abbas et al. Cellular and molecular immunology. 7th Edition (2012) (Elsevier) • Abbas et al. Basic Immunology. Functions and disorders of the immune system. 3rd Edition (2011) (Saunders, Elsevier) • Kindt et al. Kuby Immunology. 6th Edition (2007) (Freeman) • Original research and review articles Questions? RAISE YOUR HANDS! (don’t be shy) Get in touch: [email protected] 2 Lesson 1: General view of the immune system, its components and the immune responses Immunology is a matter of SELF VS NON-SELF DISCRIMINATION Self: A unique set of molecules normally expressed by our cells (MHC) identifies every cell of our body as “normal, non harmful”. The immune system WILL NOT ATTACK CELLS IDENTIFIED AS SELF! Non-self: A wide set of molecules not normally expressed by our cells (ANTIGENS) identifies the cells which harbor them as “non-normal, potentially harmful”. The immune system WILL ATTACK CELLS IDENTIFIED AS NON-SELF! The outcome of self recognition is TOLERANCE. Errors in self recognition lead to AUTOIMMUNE DISEASES. The outcome of non-self recognition is SURVEILLANCE. Errors in non-self recognition lead to INFECTIOUS DISEASES and CANCER. 3 Introduction to immunology. Lesson 1 Tasks of the immune system As multicellular organisms “immersed” in a living environment, we are currently exposed to many possible threat to our integrity, including: • Bacteria • Viruses • Parasites • Fungi • Toxins • Environmental poisons • Transformed/neoplastic cells Immunity is defined as resistance to disease, specifically infectious disease. The collection of cells, tissues and molecules that mediate resistance to infections is called the immune system, and the coordinated reaction of these cells and molecules to infectious microbes is the immune response. The physiologic function of the immune system is to prevent infections and to eradicate established infections. 4 Introduction to immunology. Lesson 1 Cells and tissues of the immune system Leukocytes Cells (Each has a form and a specific function) phagocytes lymphocytes Tissues (Each made of equal cells) Organs (Each made of different tissues) Systems Primary where leukocytes develop Secondary where immune reactions take place (Each made of similar organs) Organism 5 Introduction to immunology. Lesson 1 Cells of the immune system – The phagocytes This group includes different types of cells, all of them originating from a common precursor (the MYELOID lineage precursor) and endowed with phagocytic (“eating”) activity. Those cells are: • The first cellular line of defense of the body • Aspecific and inborn – do not discriminate what kind of pathogen they’re dealing with • Needed for the proper activation of other, more specific cells (the lymphocytes) • Attack pathogens with oxidant molecules and enzymes, and “eat” them Monocyte Macrophage Neutrophil Basophil Eosinophil Mast cell Granulocytes 6 Introduction to immunology. Lesson 1 Cells of the immune system – Other myeloid cells This group includes cells with none or very poor phagocytic activity, or tissue-specific forms of the phagocytes found in specific locations of the body Megakaryocyte Platelets Erythroid cells Tissue-specific phagocytes: • Kupffer cells (Liver) • Alveolar macrophages (Lungs) • Langerhans cells (Skin) • Histiocytes (Blood vessels) • Dendritic cells (Lymph nodes) Red blood cells 7 Introduction to immunology. Lesson 1 Cells of the immune system – The lymphocytes This group includes different types of cells, all of them originating from a common precursor (the LYMPHOID lineage precursor) and endowed with specific anti-microbial recognition activity. Those cells are: • The second cellular line of defense of the body • Specific and adaptive – they discriminate (at the finest molecular level) what kind of pathogen they’re dealing with • Needed for pathogen eradication and proper orchestration of the immune response • Attack pathogens with antibodies and lytic enzymes T-lymphocyte B-lymphocyte Natural Killer (NK) cell 8 Introduction to immunology. Lesson 1 Cells of the immune system – Other lymphoid cells This group includes cells which, though being similar to their common counterpart, have more specific or restricted activities and which are generally present in specific tissues only. gd T-lymphocytes • • B1-lymphocytes Recognize phosphoantigens Found predominantly in the intestinal tract and the skin • • NKT cells • Faster antibody production • No immunological memory • Found predominantly in the pleural and peritoneal cavities • Recognize glycolipidic antigens Fundamental for T-cells development Found predominantly in the mucosae and the thymus 9 Introduction to immunology. Lesson 1 Immune system organs – Primary and secondary Primary lymphoid organs are those where T- and B-lymphocytes develop. Those are: • The bone marrow, where T- and B-cells, as well as all myeloid cells, are born. All immune cells, apart from T-cells, also mature here. • The thymus, where immature T-cells (coming from the bone marrow) mature. Secondary lymphoid organs are those where lymphocytes get activated, and they are arranged as a series of filtering stations along the lymphatic transit. Those are: • Lymph nodes • Tonsils • Spleen • Peyer’s patches • Mucosa-associated lymphoid tissue (MALT) 10 Introduction to immunology. Lesson 1 Hematopoiesis – the production of all blood cells (white and red) in the bone marrow Hematopoietic stem cells Myeloid lineage Lymphoid lineage 11 Introduction to immunology. Lesson 1 Hematopoiesis – a stressful but necessary event for our survival The hematopoietic process is probably one of the most-demanding tasks for our body. It needs to: 1) be able to produce a steady number of red and white blood cells every day to supply oxygen and nutrients to every tissue, and to efficiently patrol the body; 2) be able to boost the production of red blood cells in case of low oxygen tensions and of leukocytes in case of infection; 3) be able to perform those actions for the whole life of an organism, by saving and keeping constant a certain amount of hematopoietic stem cells. It has been calculated that: • Approx. 1011-1012 cells are produced daily by the hematopoietic process • Hematopoietic stem cells replicate once each 48-50 weeks, meaning that they replicate 100 times in 80 years. 12 Introduction to immunology. Lesson 1 Immunity – innate/adaptive or humoral/cell-mediated? We already said that immunity is defined as resistance to infectious disease. There are two different ways to “approach” the study of immunological mechanisms, either by considering their specificity/ontogenetic derivation or their effector mechanisms. Specificity and ontogeny: innate and adaptive Effector mechanisms: humoral and cell-mediated Innate immunity is: • Aspecific • Faster • Parentally acquired • Equal for all human beings Humoral immunity is: • Mediated by macromolecules (antibodies, complement system, antimicrobial peptides) • Occurs in blood and mucosae • Effective against bacteria and toxins Adaptive immunity is: • Very specific • Slower • Somatically variable • Particular for each human being Cell-mediated immunity is: • Mediated by leukocytes • Occurs in almost every body district • Effective against bacteria, worms and viruses 13 Introduction to immunology. Lesson 1 Innate and adaptive immunity Abbas et al. 14 Introduction to immunology. Lesson 1 Innate immunity The innate immunity is our first line of defense, and relies on cellular and humoral mechanisms to actively match the invading pathogens as fast as possible. Its main targets are microbes and cells infected by microbes. The outcome of innate immunity is INFLAMMATION and activation of the ANTIVIRAL STATE. Recognition of microbes and infected cells occurs via: SIGNALS Pathogen-Associated Molecular Patterns (PAMP) Damage-Associated Molecular Patterns (DAMP) RECEPTORS Microbes TLRs, RIGs, NOD, Mannose receptor, Dectins, Scavenger receptors Phagocytes Damaged/ Infected cells Antibodies, complement system, antimicrobial peptides Mucosae and circulating 15 Introduction to immunology. Lesson 1 Innate immunity – PAMPs, DAMPs and PRRs Pathogen- Associated Molecular Patterns (PAMPs) are approx. 103 different molecules which are normal components of viruses and bacteria (while our cells do not normally express them). They are mostly structural components of bacterial walls, or viral genomic elements. Their recognition by innate immunity ensures non-self discrimination and major damage of microbes. When cells get infected by microbes, they will eventually die by necrosis, releasing intracellular proteins. Those self nuclear/cytoplasmic proteins recognized by innate immunity are called Damage-Associated Molecular Patterns (DAMPs). Receptors for PAMPs and DAMPs are called Pattern Recognition Receptors (PRRs). 16 Introduction to immunology. Lesson 1 Innate immunity – PAMPs and DAMPs PAMPs Microbes Nucleic Acids Proteins Wall lipids Carbohydrates ssRNA Viruses dsRNA Viruses Non-meth. CpG Viruses, Bacteria Pilin Bacteria Flagellin Bacteria LPS Gram- bacteria LTA Gram+ bacteria Mannans Fungi Glucans Fungi, Bacteria All of these molecules are necessary for the normal functions and survival of microbes. Their recognition ensures wide coverage and a strong interference on microbial life cycle. DAMPs Stress proteins Crystals Nuclear proteins HSP Monosodium urate HMGB1 17 Introduction to immunology. Lesson 1 Innate immunity – PRRs Toll-like receptors (TLRs) are a family of receptors evolved from Drosophila’s Toll receptors. They exist as membrane-bound and cytosolic forms, and show the widest ability to recognize PAMPs. They also recognize DAMPs. In humans 9 TLRs are known (TLR 1-9). Their activation by intracellular or extracellular ligands determines transcriptional activation of: • antiviral genes (Type-I interferons) • cytokines genes • chemokines genes • adhesion molecules genes • co-stimulatory molecules • oxidative burst genes Abbas et al. 18 Introduction to immunology. Lesson 1 Innate immunity – PRRs NOD-like receptors (NLRs) are cytosolic receptors for PAMPs and DAMPs. More than 20 NLRs are known, but the best characterized are NOD1 and NOD2. NOD1 recognizes preferentially bacterial peptidoglycans, while NOD2 recognizes muramyl dipeptide from Gram+ and Grambacteria. NLRs activation leads to gene activation in a similar way to TLRs. NOD1 and NOD2 are especially important against Helicobacter pylori and defects in NOD2 might be involved in Chron’s disease. RIG-like receptors (RLRs) are cytosolic receptors for viral RNA (both ssRNA and dsRNA). Best characterized RLRs are RIG-I and MDA5, which recognize different viral nucleic acids. Once activated, they will lead to transcription of Type-I interferons and antiviral defenses activation. These include suppression of transcription factors needed for viral genes (like EIF2a), the synthesis of RNAse which degrade viral RNA and suppression of viral proteins assembly complexes. 19 Introduction to immunology. Lesson 1 Innate immunity – other PRRs Microbial carbohydrates are recognized by calcium-dependent Lectins (C-type Lectins). These include: • Mannose receptor (CD206), which recognizes D-mannose, L-fucose and N-acetyl-Dglucosamine. • Dectins, which recognize fungal b-glucan (dectin-1) and mannose-rich oligosaccharides (dectin-2). • Langherin (CD207), DC-SIGN, and others Other microbial PAMPs are recognized by: • Scavenger receptors (like SR-A and CD36). Initially identified as receptors for oxidized LDL (involved in atherosclerosis), they bind to bacterial polyanions (LPS, LTA, nucleic acids etc.). • N-FMLP receptors (like FPR and FPRL1). Those receptors bind to n-formylmethionine leucyl-phenylalanine, a sequence which characterizes all bacterial proteins but not human ones (apart from mitochondrial proteins). 20 Introduction to immunology. Lesson 1 The innate immunity in action – a 3 step process STEP 1 Epithelia: - Physical barrier - Defensive molecules Abbas et al. STEP 2 STEP 3 Circulating defenses: - Natural antibodies - The Complement system Cellular defenses: - Phagocytes - NK cells 21 Introduction to immunology. Lesson 1 The innate immunity in action – anatomical barriers Epithelia play a big role in the very first match with invading pathogens. As most of the microbes enter the body via the skin, the respiratory and the gastrointestinal tract, these epithelia evolved specific strategies to counteract pathogens, like: • Expression of sialomucins on the external side of the plasma membrane, which electrostatically repel bacterial walls • Production of antimicrobial peptides (like defensins and cathelicidins), which both directly attack the microbes and help their recognition by innate immunity cells • Hosting of intraepithelial lymphocytes. While some of them are “classical” ab Tcells, many are gd T-cells, which are particularly good at recognizing bacterial phospholipids. They can directly attack microbes and stimulate phagocyte responses. Abbas et al. 22 Introduction to immunology. Lesson 1 The innate immunity in action – circulating defenses Once microbes enter the blood flow or the extracellular fluids, they get in contact with the humoral effector mechanisms of the innate immunity: natural antibodies, the complement system and the pentraxins/collectins/ficolins family members. Natural antibodies belong to the pentameric IgM class. They are mainly produced by B1 lymphocytes in a spontaneous way which does not require any presence of the pathogen. These natural antibodies recognize PAMPs and DAMPs, especially carbohydrates, lipids and lipoproteins. The AB0 blood group system depends on the presence of natural antibodies. Once bound to microbes, they activate the complement and stimulate phagocyte response to eradicate the threat. 23 Introduction to immunology. Lesson 1 The innate immunity in action – circulating defenses The complement system is a network of many (> 20) soluble and membrane-bound proteins which are normally present in the blood flow in the form of inactive precursors (pro-enzymes). The term complement (C) was used to refer to a heat-instable serum component which was able to lyse bacteria when incubated at 37oC, but lost when incubated at 56oC for 30 minutes (antibodies are thermo stable!). • • Jules Bordet • • • The complement system is activated by microbial macromolecules or by antibodies bound to them. There are 3 complement activation pathways. Complement activation proceeds through sequential cleavage and activation of circulating inactive forms of C proteins. Once cleaved, those precursors become active and acquire proteolytic activity. The final stages of complement activation lead to formation of MAC (Membrane Attack Complex), which is a canal (similar to acquaporins) structure allowing water to enter into the microbes and kill them by osmotic lysis. Microbes bound to complement fragments can be more-easily recognized and killed by phagocytes Self cells, but not microbes, express proteins which inhibit complement activation. 24 Introduction to immunology. Lesson 1 The innate immunity in action – complement activation C3 has a spontaneous cleavage turnover in body fluids, so it can directly recognize microbes. The classical and lectins pathway provide specificity to complement activation Abbas et al. 25 Introduction to immunology. Lesson 1 The innate immunity in action – complement activation Abbas et al. 26 Introduction to immunology. Lesson 1 The innate immunity in action – other functions of the complement The complement system provides a fast and reliable way to directly attack microbes, but it is also connected to the cells of the innate immunity thanks to COMPLEMENT RECEPTORS (CR): • CR1 (or CD35) promotes the phagocytosis of microbes bound to C3b and C4b. It is expressed by almost all immune cells, in which determines activation, but also by red blood cells. This provides a mean for the elimination of microbes by hemocatheresis. • CR2 (or CD21) promotes the activation of B-cells and antibody production. It’s also expressed by specific epithelial cells and is involved in Epstein-Barr virus pathogenesis. • CR3 (or CD11b/Mac-1) binds a fragment deriving from C3b (iC3b) and is a strong promoter of phagocytes’ activation. • CR4 (or CD11c) belongs to the same family of CR3 and has similar functions, even though is more restricted to specific cell subtypes (like dendritic cells) • CR5 (or CRIg) binds to C3b and iC3b and is expressed only by liver’s Kupffer cells. It is mostly involved in the direct elimination of circulating microbes by hemocatheresis. 27 Introduction to immunology. Lesson 1 The innate immunity in action – cellular immunity Cellular defenses belonging to the innate immunity involve all myeloid cells and some specific lymphoid cell types. Myeloid Lymphoid Phagocytes Phagocytosis and RESPIRATORY BURST CYTOKINES and CHEMOKINES Mast cells BIOGENIC AMINES NK cells and gd T-cells CYTOLYTIC MECHANISMS B1 cells NATURAL ANTIBODIES BIOGENIC AMINES 28 Introduction to immunology. Lesson 1 The innate immunity in action – phagocytosis and the respiratory burst Elsevier 2005 29 Introduction to immunology. Lesson 1 The innate immunity in action – phagocytosis and the respiratory burst Once the microbe is engulfed, the phagosome (phagocytic vesicle) fuses with the lysosome. Its acidification activates the pro-enzymes that it contains and allows microbial degradation. • Elastase and Cathepsin-G. Wide-spectrum proteases able to degrade many bacterial proteins. Elastase is a serin-protease while Cathepsin-G is chymotripsin-like protease. Those enzymes are activated by the low pH and by radicals. In the phagolysosome, the respiratory burst occurs. This is the most powerful antimicrobial mechanism of the phagocytes. It involves both the consumption of oxygen and specific aminoacids to produce toxic compounds. • Reactive oxygen species (ROS) include H2O2, O2.-, O. and are generated by the NADPH oxidase. Those compounds are able to destroy/destabilize all major classes of biomolecules, and thus destroy bacterial walls, membranes and genomes. Deficit of NADPH oxidase is responsible for the chronic granulomatous disease (CGD), a very severe deficiency of the innate immunity. • The inducible nitric oxide synthase (iNOS) catalyzes the conversion of arginine to citrulline. During this process, nitric oxide is formed. In the phagolysosome, NO interacts with H2O2 and O2.- to form peroxynitrite (ONOO-) which is extremely toxic as the ROS. 30 Introduction to immunology. Lesson 1 The innate immunity in action – biogenic amines and prostanoids Phagocytes and mast cells secrete immunomodulatory compounds upon their activation, including amines and prostanoids. Histamine is produced via decarboxylation of histidine. Once released, it will determine: • Vasoconstriction of the major arteries • Vasodilatation of arterioles • Contraction of endothelial cells with increased permeability of the capillaries and venulae. This facilitates the immune cells to penetrate in the site of infection (leukocyte extravasation). Histamine is responsible for itching at inflamed sites (think of mosquitos bites) 31 Introduction to immunology. Lesson 1 The innate immunity in action – biogenic amines and prostanoids Phagocytes and mast cells secrete immunomodulatory compounds upon their activation, including amines and prostanoids. Prostanoids are produced from arachidonic acid by the cyclooxygenase (COX) enzymes (target of NSAIDS). Prostaglandins (PGs), leukotrienes (LTs) and thromboxanes (TXs) have different systemic and local effects, but they generally either: • Stimulate inflammation and leukocyte extravasation (LTs, and TXs and some PGs) • Suppress local inflammation (PGs like PGE2) 32 Introduction to immunology. Lesson 1 The innate immunity in action – lymphoid cells Microbes can be recognized and killed by lymphoid cells too. Involved in this process are mainly NK cells, NKT cells and gd T-cells. Recognition can be either direct or mediated by antibodies. DIRECT F1000 2011 MEDIATED Nature 2003 33 Introduction to immunology. Lesson 1 The innate immunity in action – ADCC NK cells can also directly recognize microbes if they are covered by antibodies (opsonized). Abbas et al. When antibodies bound to a microbe (or a damaged cell) are recognized by the NK cell through their antibody receptor (FcgRIII), activation will occur even if the cells express suppressive stimuli. Note that opsonization works the same way to aid phagocytes with microbes recognition and engulfment. 34 Introduction to immunology. Lesson 1 The innate immunity in action – Inflammation The 5 symptoms of inflammation: • Tumor (swelling) • Rubor (redness) • Calor (heat) • Dolor (pain) • Functio laesa (functional damage) Consequences of immune system activation! 35 Introduction to immunology. Lesson 1 The innate immunity in action – Inflammation Inflammation is the normal, second line of defense of our body against pathogens. It is defined as acute inflammation when it proceeds normally and resolves spontaneously. It will eventually turn to chronic inflammation, a pathological process leading to tissue destruction, if the stimulus (microbial invasion) cannot be resolved by the immune cells. The clinical signs of inflammation depend on the release of soluble immune mediators, including amines, prostanoids, cytokines and chemokines. cytokines chemokines direct regulation of immune processes coordinated regulation of surrounding, non-immune cells chemotactic factors for immune cells 36 Introduction to immunology. Lesson 1 The innate immunity in action – cytokines Cytokines can: • Stimulate the functions of phagocytes and lymphocytes, empowering their antimicrobial activity. • Stimulate the proliferation of leukocytes, to empower body defenses. • Stimulate lymphocytes differentiation, ensuring specific immunity to be effective. • Stimulate multiple organs functions, to cooperate with leukocytes activity. • Suppress immune functions, to end the reaction and restore the normal functions of the body. Abbas et al. 37 Introduction to immunology. Lesson 1 The innate immunity in action – cytokines Abbas et al. 38 Introduction to immunology. Lesson 1 The innate immunity in action – chemokines Chemokines are generally divided into: • CC chemokines (b-chemokines), if they have two adjacent cysteines at the C-terminus • CXC chemokines (a-chemokines), if the two N-terminal cysteines are separated by another residue (X) 39 Introduction to immunology. Lesson 1 The innate immunity in action – activation of anti-viral state The anti-viral state is a coordinated set of events occurring mostly in a paracrine way to prevent viruses dissemination and further infection. It is considered as an ancillary mechanism, as the major defense against viruses requires lymphocytes (adaptive immunity). It is mediated by Type-I interferons, which are produced when viral PAMPs activate PRRs. Type-I interferons IFN-a (9 different types) IFN-b (1 type) Segregation of lymphocytes in the lymph nodes, where they will “learn” what type of virus is infecting Potentiation of NK cells Th1 differentiation of T-cells Increased MHC-I expression Adaptive immunity ACTIVATION OF THE ANTIVIRAL STATE Innate (passive) immunity 40 Introduction to immunology. Lesson 1 The innate immunity in action – activation of anti-viral state The so-called antiviral state is a passive defense, which prevents viruses to replicate in cells which have been targeted by Type-I IFN. But, it does not kill infected cells. The need for Adaptive immunity Abbas et al. 41 Introduction to immunology. Lesson 1 Inflammation switch-off – feedback mechanisms Involving powerful cells (phagocytes, NK cells, etc.) armed with aggressive enzymes and toxic products (lytic enzymes, vasoactive molecules, ROS, NO, etc.), inflammation always damage the tissues. It is therefore necessary that it ends as soon as the microbial invasion is resolved. Interleukin-10 (IL-10) is the prototypical anti-inflammatory cytokine. Its production is triggered by inflammatory stimuli, but starts after the synthesis of inflammatory cytokines like TNF, IL-1, IL-12 etc. Once secreted, it switches off the transcription of inflammatory cytokines genes. IL-1 functions are suppressed by a soluble antagonist which binds to the same receptor as IL-1 but which has no biological functions, called IL-1 receptor antagonist (IL-1ra), produced by phagocytes. There is also a Type-II receptor for IL-1 which is a decoy receptor with no activity (scavenger of IL-1). Inflammatory stimuli induce the expression of autophagy genes (Atg). Autophagy is the process of a cell which degrades (eat) its own organelles. By “eating” organelles where PRRs or cytokines are stored, a cell diminishes its ability to activate during inflammation. Several suppressor of cytokines transduction pathways (SOCS, Suppressors Of Cytokine Signaling) are induced by inflammatory stimuli and shut down pro-inflammatory cytokine signals. 42