* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download 32_Metabolism of ammonia. Biosynthesis of urea and its disorders
Survey
Document related concepts
Evolution of metal ions in biological systems wikipedia , lookup
Adenosine triphosphate wikipedia , lookup
Microbial metabolism wikipedia , lookup
Biosynthesis wikipedia , lookup
Oxidative phosphorylation wikipedia , lookup
Glyceroneogenesis wikipedia , lookup
Amino acid synthesis wikipedia , lookup
Clinical neurochemistry wikipedia , lookup
Biochemistry wikipedia , lookup
Metabolomics wikipedia , lookup
Pharmacometabolomics wikipedia , lookup
Basal metabolic rate wikipedia , lookup
Transcript
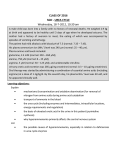
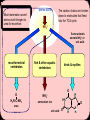
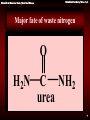
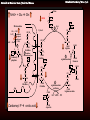
Metabolic & Molecular Basis of Inherited Disease Metabolic Disorders of Urea Cycle Metabolic Disorders of Urea Cycle Metabolic & Molecular Basis of Inherited Disease amino acids Most mammals convert amino-acid nitrogen to urea for excretion The carbon chains are broken down to molecules that feed into the TCA cycle. NH4+ Some animals excrete NH4+ or uric acid. most terrestrial vertebrates fish & other aquatic vertebrates birds & reptiles O O H2N-C-NH2 NH4+ ammonium ion H N HN urea uric acid O O N H N H Metabolic & Molecular Basis of Inherited Disease Metabolic Disorders of Urea Cycle Ammonia is a toxic substance to plants and animals (especially for brain) Normal concentration: 25-40 mol/l (0.4-0.7 mg/l) Ammonia must be removed from the organism Terrestrial vertebrates synthesize urea (excreted by the kidneys) ureotelic organisms Urea formation takes place in the liver Birds, reptiles synthesize uric acid Metabolic Disorders of Urea Cycle Metabolic & Molecular Basis of Inherited Disease Major fate of waste nitrogen O H 2N C NH2 urea 4 Metabolic & Molecular Basis of Inherited Disease Metabolic Disorders of Urea Cycle Why Urea? Non toxic Water soluble Combines two waste products into one molecule: CO2 NH3 5 Metabolic Disorders of Urea Cycle Metabolic & Molecular Basis of Inherited Disease Ammonia is highly toxic Main reason to form urea is to reduce levels of ammonia “Ammonia” often refers to (NH3 + NH4+) NH3 is really ammonia NH4+ is the ammonium ion pKa = 9.3 NH4+ NH3 + H+ 6 Metabolic & Molecular Basis of Inherited Disease Metabolic Disorders of Urea Cycle Hypotheses toxicity of ammonia A. The binding of ammonia in the synthesis of glutamate causes an outflow of α-ketoglutarate from the tricarboxylic acid cycle, with decreased formation of ATP energy and deteriorates the activity of cells. B. Ammonium ions NH4 + caused alkalization of blood plasma. This increases the affinity of hemoglobin for oxygen (Bohr effect), the hemoglobin does not release oxygen to the capillaries, resulting the cells hypoxia occurs. C. The accumulation of free NH4 + ion in the cytosol affects the membrane potential and intracellular enzymes work - it competes with ion pumps, Na + and K +. Metabolic & Molecular Basis of Inherited Disease Metabolic Disorders of Urea Cycle Hypotheses toxicity of ammonia D. The producing ammonia tramsform glutamic acid glutamine - an osmotically active substance. This leads to water retention in the cells and the swelling that causes swelling of tissues. In the case of nervous tissue it can cause brain swelling, coma and death. E. The use of α-ketoglutarate and glutamate to neutralize the ammonia causes a decrease in the synthesis of γ-aminobutyric acid (GABA) inhibitory neurotransmitter of the nervous system. Metabolic Disorders of Urea Cycle Metabolic & Molecular Basis of Inherited Disease Ammonia rapidly equilibrates across membranes NH4+ NH4+ pKa = 9.3 NH3 NH3 Lipid Bilayer Metabolic Disorders of Urea Cycle AMMONIA METABOLISM Metabolic & Molecular Basis of Inherited Disease The ways of ammonia formation 1. Oxidative deamination of amino acids 2. Deamination of physiologically active amines and nitrogenous bases. 3. Absorption of ammonia from intestine (degradation of proteins by intestinal microorganisms results in the ammonia formation). 4. Hydrolytic deamination of AMP in the brain (enzyme – adenosine deaminase) Metabolic Disorders of Urea Cycle Metabolic & Molecular Basis of Inherited Disease Production of ammonia Amino acids -Keto acids -Ketoglutarate -Ketoglutarate Glutamate GDH Oxaloacetate Aspartate Other reactions NH+4 Urea cycle Urea Metabolic & Molecular Basis of Inherited Disease Metabolic Disorders of Urea Cycle Summary of sources of ammonia for urea cycle Metabolic & Molecular Basis of Inherited Disease Metabolic Disorders of Urea Cycle Peripheral Tissues Transport Nitrogen to the Liver Two ways of nitrogen transport from peripheral tissues (muscle) to the liver: 1. Alanine cycle. Glutamate is formed by transamination reactions Glutamate is not deaminated in peripheral tissues Metabolic & Molecular Basis of Inherited Disease Metabolic Disorders of Urea Cycle Nitrogen is then transferred to pyruvate to form alanine, which is released into the blood. The liver takes up the alanine and converts it back into pyruvate by transamination. The glutamate formed in the liver is deaminated and ammonia is utilized in urea cycle. Metabolic Disorders of Urea Cycle Metabolic & Molecular Basis of Inherited Disease Closer look at transport of waste N from peripheral tissue to liver via alanine and glutamine Waste N funnelled to pyruvate via transaminations Glucose – Alanine Cycle Net: N (muscle) Urea (liver) Metabolic & Molecular Basis of Inherited Disease Metabolic Disorders of Urea Cycle 2. Nitrogen can be transported as glutamine. Glutamine synthetase catalyzes the synthesis of glutamine from glutamate and NH4+ in an ATP-dependent reaction: Ammonia transport in the form of glutamine. Excess ammonia in tissues is added to glutamate to form glutamine, a process catalyzed by glutamine synthetase. After transport in the bloodstream, the glutamine enters the liver and NH4 is liberated in mitochondria by the enzyme glutaminase. Metabolic & Molecular Basis of Inherited Disease Metabolic Disorders of Urea Cycle Synthesis of Glutamine in Peripheral Tissue and Transport to the Liver 17 Metabolic & Molecular Basis of Inherited Disease Metabolic Disorders of Urea Cycle Metabolic & Molecular Basis of Inherited Disease Metabolic Disorders of Urea Cycle UREA FORMATION Metabolic Disorders of Urea Cycle Metabolic & Molecular Basis of Inherited Disease Overview Occurs primarily in liver; excreted by kidney Principal method for removing ammonia Hyperammonemia: Defects in urea cycle enzymes (CPS, OTC, etc.) Severe neurological defects in neonates Treatment: Stop protein intake Dialysis Increase ammonia excretion: Na benzoate, Na phenylbutyrate, L-arginine, L-citrulline Metabolic Disorders of Urea Cycle Metabolic & Molecular Basis of Inherited Disease Overview Key reaction: hydrolysis of arginine Arginine + H2O ==> urea + ornithine arginase Resynthesis of Arginine Metabolic & Molecular Basis of Inherited Disease Metabolic Disorders of Urea Cycle Blood Urea Nitrogen Normal range: 7-18 mg/dL Elevated in amino acid catabolism Glutamate N-acetylglutamate CPS-1 activation Elevated in renal insufficiency Decreased in hepatic failure Metabolic Disorders of Urea Cycle Metabolic & Molecular Basis of Inherited Disease Urine urea NH2 C O Mitochondrion CO2 + NH4+ carbamoyl 2 ATP phosphate synthetase I (CPSI) 2ADP + Pi 1 O H2N C O P O- CH2 H C NH2 Ornithine 2 ornithine NH2 Pi H2O C NH CH2 NH CH2NH2 CH2 transcarbamoylase Carbamoyl O phosphate 5 Cytosol COOH O NH2 NH2 C O CH2 NH CH2 CH2 H C NH2 COOH Citrulline CH2 CH2 CH2NH2 CH2 H C NH2 COOH COOH CH2 Arginine H C NH2 COOH 4 argininosuccinase Ornithine NH2 C O HC CH COOH Fumarate COOH NH CH2 NH C CH2 NH CH2 NH CH2 CH2 H C NH2 3 argininosuccinate synthetase COOH Citrulline COOH H2N C H CH CH2 COOH CH2 H C NH2 COOH Argininosuccinate ATP AMP + PPi CH2 COOH Aspartate 23 Metabolic & Molecular Basis of Inherited Disease THE UREA CYCLE Metabolic Disorders of Urea Cycle Urea cycle - a cyclic pathway of urea synthesis first postulated by H.Krebs The sources of nitrogen atoms in urea molecule: - aspartate; - NH4+. Carbon atom comes from CO2. Metabolic Disorders of Urea Cycle Metabolic & Molecular Basis of Inherited Disease HCO3- 2 ATP 2 ADP + Pi The urea cycle O O H2N-C-O-P-OO- NH4+ ornithine NH3+ Pi H2N-CH2CH2CH2CH-CO2- O H2N-C-NH2 cytosol carbamoyl phosphate mitochondria citrulline + NH3 O H2N-C-NH-CH2CH2CH2CH-CO2- CO2- Asp -O C-CH CH-NH + 2 2 3 ATP AMP + PPi urea H2O CO2- NH2+ NH3+ -O C-CH CH-NH-C-NH-CH CH CH CH-CO 2 2 2 2 2 2 argininosuccinate arginine NH3+ NH2+ H2N-C-NH-CH2CH2CH2CH-CO2- -O 2C-CH=CH-CO2 - fumarate Metabolic Disorders of Urea Cycle Metabolic & Molecular Basis of Inherited Disease Incorporation of ammonia into urea begins with formation of carbamoyl phosphate O O H2N-C-O-P-Ocarbamoyl Ophosphate 2 ADP + Pi NH4+ + HCO32 ATP This occurs in the mitochondrial matrix. Carbamoyl-phosphate synthetase-1 catalyzes the reaction in three steps, using two molecules of ATP: HCO3ATP (1) ADP O O HO-C-O-P-OONH4+ (2) carbamate O H2N-C-O- Pi carbonicphosphoric acid anhydride ATP ADP (3) O O H2N-C-O-P-OO- Metabolic Disorders of Urea Cycle Metabolic & Molecular Basis of Inherited Disease Carbamoyl phosphate reacts with ornithine to form citrulline O O H2N-C-O-P-OO- carbamoyl phosphate Pi NH3+ +H N-CH CH CH CH-CO 3 2 2 2 2 ornithine NH3+ O H2N-C-NH-CH2CH2CH2CH-CO2+ H+ citrulline This step also occurs in the mitochondrial matrix. Metabolic Disorders of Urea Cycle Metabolic & Molecular Basis of Inherited Disease Combination of citrulline with aspartate to form argininosuccinate is driven by breakdown of ATP to AMP CO2-O C-CH CH-NH + 2 2 3 aspartate NH3+ O H2N-C-NH-CH2CH2CH2CH-CO2- ATP citrulline AMP + PPi + H2O argininosuccinate CO2- NH2+ NH3+ -O C-CH CH-NH-C-NH-CH CH CH CH-CO 2 2 2 2 2 2 This reaction occurs only in the cytosol, so citrulline first must leave the mitochondria. A transporter exchanges ornithine for citrulline plus a proton across the mitochondrial inner membrane. Metabolic Disorders of Urea Cycle Metabolic & Molecular Basis of Inherited Disease Argininosuccinate splits into arginine and fumarate CO2- NH2+ NH3+ -O C-CH CH-NH-C-NH-CH CH CH CH-CO 2 2 2 2 2 2 argininosuccinate -O 2C-CH=CH-CO2 fumarate - NH3+ NH2+ H2N-C-NH-CH2CH2CH2CH-CO2arginine This reaction occurs in the cytosol. Metabolic Disorders of Urea Cycle Metabolic & Molecular Basis of Inherited Disease Hydrolysis of arginine releases urea and regenerates ornithine NH3+ NH2+ H2N-C-NH-CH2CH2CH2CH-CO2arginine H2O O H2N-C-NH2 urea NH3+ H2N-CH2-CH2-CH2-CH-CO2H+ ornithine This reaction occurs in the cytosol. To continue the cycle, ornithine must return to a mitochondrion. Metabolic Disorders of Urea Cycle Metabolic & Molecular Basis of Inherited Disease HCO3- 2 ATP 2 ADP + Pi carbamoyl O O phosphate H2N-C-O-P-OOPi NH4+ NH3+ O H2N-C-NH-CH2CH2CH2CH-CO2- ornithine O H2N-C-NH2 urea citrulline ATP 2 Pi PPi + AMP CO2-O C-CH CH-NH + 2 2 3 Asp H2O CO2- NH2+ NH3+ -O C-CH CH-NH-C-NH-CH CH CH CH-CO 2 2 2 2 2 2 argininosuccinate Formation of urea consumes 4 phosphate anhydride bonds Metabolic Disorders of Urea Cycle Metabolic & Molecular Basis of Inherited Disease Input-Output 1. NH4+ + CO2 + 2 ATP carbamoyl phosphate + 2 ADP + Pi 2. carbamoyl phosphate + ornithine citrulline + Pi 3. citrulline + aspartate + ATP argininosuccinate + AMP + PPi 4. AMP + ATP 2 ADP 5. PPi + ATP 2 ADP 6. argininosuccinate arginine + fumarate 7. arginine + H2O urea + ornithine SUM: NH4+ + CO2 + 4 ATP + aspartate urea + fumarate + 4 ADP + 4 Pi Metabolic Disorders of Urea Cycle Metabolic & Molecular Basis of Inherited Disease The aspartate consumed in the urea cycle can be regenerated from the fumarate that is produced 2 ATP HCO3+ NH4+ 2 ADP + Pi carbamoyl phosphate Pi -keto acids amino acids aspartateoxaloacetate aminotransferase ornithine citrulline Urea cycle urea ATP AMP + PPi arginine oxaloacetate aspartate malate dehydrogenase argininosuccinate NADH malate NAD+ fumarate H2O This process also uses both cytosolic and mitochondrial enzymes Metabolic Disorders of Urea Cycle Metabolic & Molecular Basis of Inherited Disease Oxidation of malate in mitochondria generates ATP 2 ATP 2 e- to O2 via NADH dehydrogenase generates ~ 2.5 ATP 2 ADP + Pi HCO3+ NH4+ carbamoyl phosphate oxaloacetate mitochondrion NAD Pi aspartate ornithine citrulline ATP glutamate -ketoglutarate -ketoglutarate citrulline ornithine NADH malate glutamate aspartate urea AMP + PPi arginine argininosuccinate amino acids -ketoacids malate cytosol fumarate H2O NADH, and oxaloacetate can’t cross the mitochondrial inner membrane, but there are transporters for malate, aspartate, glutamate and -ketoglutarate. NAD+ Metabolic & Molecular Basis of Inherited Disease Metabolic Disorders of Urea Cycle Transport systems in the mitochondrial inner membrane exchange aspartate for glutamate and a-ketoglutarate for malate mitochondrion aspartate- aspartatecytosol glutamate- + H+ glutamate- + H+ -ketoglutarate -ketoglutarate malate malate Because the Asp/Glu transporter also moves a proton across the membrane, it can be driven by an electrochemical potential gradient. Mutations in this transporter have been linked to autism. Metabolic Disorders of Urea Cycle Metabolic & Molecular Basis of Inherited Disease Alpha--ketoglutarate/malate and aspartate/glutamate transporters also participate in oxidation of cytosolic NADH mitochondrion NADH NAD+ 2 e- to electrontransport chain oxaloacetate aspartate aspartate glutamate glutamate -ketoglutarate -ketoglutarate oxaloacetate cytosol NADH NAD+ glycolysis malate malate Metabolic Disorders of Urea Cycle Metabolic & Molecular Basis of Inherited Disease Well Fed State a.a.'s Asp a.a.'s KAs KG NH+ Glu 4 urea cycle fumarate urea CO2 + H2O OAA Mal malate Net: 2 NH4+ + CO2 + 4 ATP urea + 4 ADP + 4 Pi Metabolic Disorders of Urea Cycle Metabolic & Molecular Basis of Inherited Disease Fasted State ala Asp ala pyr KG Gluconeogenesis NH+ Glu 4 urea cycle fumarate urea OAA malate OAA 2 ala + CO2 1 urea + 1 glucose Glucose Metabolic Disorders of Urea Cycle Metabolic & Molecular Basis of Inherited Disease Balancing the levels of ammonia and aspartate for entry into urea cycle (a) NH3 in excess (b) Aspartate in excess NH3 NH3 -Ketoglutarate NADH NAD Glutamate dehydrogenase NADH NAD Glutamate Glutamate dehydrogenase Glutamate Aspartate transaminase Oxaloacetate Aspartate transaminase Oxaloacetate Aspartate Citrulline Carbamoyl phosphate Citrulline Carbamoyl phosphate Urea Cycle Urea Urea Cycle Urea -Ketoglutarate Aspartate Metabolic Disorders of Urea Cycle Metabolic & Molecular Basis of Inherited Disease The urea cycle is regulated in two ways 1. Allosteric activation of carbamoylphosphate synthetase-1 by N-acetylglutamate CO2+H N 3 C H CO2+ acetyl-CoA CH3CO-NH C H N-acetylglutamate CH2 Glu CH2 CH2 CoA-SH CO2- CH2 CO2- In mammals, N-acetylGlu appears to play only a regulatory role. Carbamoylphosphate synthetase-1 is completely inactive in its absence. A genetic deficiency in the enzyme that forms N-acetylGlu 2 ATP can cause a lethal defect in the urea cycle. NH4+ + HCO3- 2 ADP + Pi carbamoylphosphate O O H2N-C-O-P-OO- 2. A high-protein diet or starvation leads to increased synthesis of all five enzymes used in the urea cycle, including carbamoylphosphate synthetase-1. Expression of the enzyme that synthesizes N-acetylglutamate also increases. Metabolic Disorders of Urea Cycle The Linkage between Urea Cycle, Citric Acid Cycle and Transamination of Oxaloacetate Metabolic & Molecular Basis of Inherited Disease Fumarate formed in urea cycle enters citric acid cycle and is converted to oxaloacetate. Fates of oxaloacetate: (1) transamination to aspartate, (2) conversion into glucose, (3) condensation with acetyl CoA to form citrate, (4) conversion into pyruvate. Metabolic Disorders of Urea Cycle Metabolic & Molecular Basis of Inherited Disease Diagnostic significance of the determination of urea in urine. 25-30 g/day of urea is excreted in normal conditions. The increase of urea in urine occurs in high fever, malignant anemia, poisoning by phosphorus, intensive decomposition of protein in organism. The decrease of urea in urine occurs in liver diseases, kidney unsufficiency, acidosis. 28 April 2017 Total slide : 50 42 Metabolic & Molecular Basis of Inherited Disease Metabolic Disorders of Urea Cycle Urea Cycle Disorders Deficiency of any of the five enzymes in the urea cycle results in the accumulation of ammonia and leads to encephalopathy. Episodes of encephalopathy and associated systems are unpredictable and, if untreated, are lethal or produce devastating neurologic sequelae in long-term survivors. Although these disorders do not produce liver disease, the consequences of hyperammonemia resemble those seen in patients with hepatic failure or in a transient interference with the urea cycle, as seen in some forms of organic acidemias. Investigate for hyperammonemia in any infant or child with altered mental status Metabolic & Molecular Basis of Inherited Disease Metabolic Disorders of Urea Cycle The urea cycle Asterisk = N-acetyl glutamate synthetase; 1 = carbamyl phosphate synthetase; 2 = ornithine transcarbamylase; 3 = argininosuccinate synthetase; 4 = argininosuccinate lyase; 5 = arginase Metabolic Disorders of Urea Cycle Metabolic & Molecular Basis of Inherited Disease UREA CYCLE DISORDERS Disorder Deficient Enzyme Inheritance Pattern Carbamyl phosphate synthetase deficiency Carbamyl phosphate synthetase Autosomal recessive Ornithine transcarbamylase deficiency Ornithine transcarbamylase X-linked Citrullinemia Argininosuccinate synthetase Autosomal recessive Argininosuccinate lyase Autosomal recessive Arginase Autosomal recessive Argininosuccinic aciduria Argininemia Metabolic & Molecular Basis of Inherited Disease Metabolic Disorders of Urea Cycle Case The patient is a full-term newborn boy from a normal vaginal delivery. The pregnancy was uncomplicated. At 36 hours the baby became lethargic, irritable, and was hyperventilating. Over the next 24 hours lethargy increased and progressed to coma requiring mechanical ventilation. Hemodialysis was started at 5 days. Patient died at one week of age. Laboratory Results At 36 hours arterial blood pH was 7.50 (7.35-7.45), carbon dioxide was 25 torr (35-45), and blood urea nitrogen was 2 mg/dl (5-20). Sepsis workup was negative. On day 5 plasma ammonium was 1800 :mol/l (<35). Plasma glutamine was 1500 :mol/l (550-650),arginine was below normal, and citrulline undetectable. Orotic acid in the urine was extremely elevated. Family History Two of the mother’s four brothers had died shortly after birth. Cause of death was given as encephalitis. Biochemical Basis of Disorder , same as.. Diagnosis: ornithine transcarbamoylase deficiency Metabolic & Molecular Basis of Inherited Disease Metabolic Disorders of Urea Cycle Biochemical explanations for ornithine transcarbamoylase deficiency Low BUN Low blood arginine Undetectable blood citrulline Elevated blood ammonia Elevated blood glutamine Elevated orotic acid Metabolic Disorders of Urea Cycle Metabolic & Molecular Basis of Inherited Disease Urine NH4+ + Glu Gln urea NH2 C O Mitochondrion CO2 + NH4+ carbamoyl 2 ATP phosphate synthetase I (CPSI) ADP + Pi 1 O H2N C O P O- CH2 H C NH2 Ornithine 2 ornithine NH2 phosphate C NH CH2 NH CH2 CH2 CH2NH2 CH2 CH2 NH CH2 CH2 H C NH2 COOH Citrulline H C NH2 Arginine H C NH2 COOH 4 argininosuccinase Ornithine NH2 C O HC CH COOH Fumarate COOH NH CH2 NH C CH2 NH CH2 NH CH2 CH2 H C NH2 3 argininosuccinate synthetase COOH Citrulline COOH H2N C H Carbamoyl P orotic acid COOH COOH CH2 C O Pi H2O CH2NH2 CH2 transcarbamoylase Carbamoyl O 5 Cytosol COOH O NH2 NH2 CH2 COOH Aspartate CH2 H C NH2 COOH Argininosuccinate ATP AMP + PPi CH CH2 COOH Metabolic & Molecular Basis of Inherited Disease Metabolic Disorders of Urea Cycle Carbamoyl P synthetase deficiency Metabolic Disorders of Urea Cycle Metabolic & Molecular Basis of Inherited Disease Urine NH4+ + Glu Gln urea NH2 C O Mitochondrion CO2 + NH4+ carbamoyl 2 ATP phosphate synthetase I (CPSI) ADP + Pi 1 O Cytosol CH2 H C NH2 Ornithine H2N C O P O- 2 ornithine transcarbamoylase Carbamoyl O NH2 phosphate C NH CH2 NH CH2 CH2 CH2NH2 CH2 CH2 NH CH2 CH2 H C NH2 COOH Citrulline H C NH2 Arginine H C NH2 COOH 4 argininosuccinase Ornithine NH2 C O HC CH COOH Fumarate COOH NH CH2 NH C CH2 NH CH2 NH CH2 CH2 H C NH2 3 argininosuccinate synthetase COOH Citrulline COOH H2N C H CH2 Carbamoyl P orotic acid COOH COOH CH2 C O Pi 5 H2O CH2NH2 CH2 COOH O NH2 NH2 COOH Aspartate CH2 H C NH2 COOH Argininosuccinate ATP AMP + PPi CH CH2 COOH Metabolic Disorders of Urea Cycle Metabolic & Molecular Basis of Inherited Disease Autism is a neurodevelopmental genetic disorder Deficits in verbal & nonverbal communication and social interactions Repetitive or stereotyped behaviors Incidence ~1 per 1000 people (possibly higher) Strong evidence for heritability Polygenic - between 5 & 10 genes may be involved Single-nucleotide polymorphisms (SNPs) in the gene for a mitochondrial, Ca2+-dependent Asp/Glu exchanger increase the risk by a factor of 3 to 4. This is the main form of the Asp/Glu exchanger that is expressed in the brain. Mutations in the gene impair the urea cycle. N. Ramoz et al., Am. J. Psychiatry 161: 662 (2004) L. Palmieri et al., EMBO J. 20: 5060 (2001) Metabolic & Molecular Basis of Inherited Disease Metabolic Disorders of Urea Cycle Urea Cycle Disorders (Diagnosis) Cultured skin fibroblasts may be desirable if prenatal diagnosis is considered in future pregnancies. Carbamyl phosphate synthetase I and ornithine transcarbamylase (OTC) are not expressed in cultured fibroblasts. The enzymatic diagnosis of CPSD and OTCD requires liver biopsy. Biopsy should be done when establishing the diagnosis of the first case in a family. Metabolic & Molecular Basis of Inherited Disease Metabolic Disorders of Urea Cycle Urea Cycle Disorders (Treatment) Once hyperammonemia is demonstrated in an infant, protein-containing feedings should be discontinued immediately, appropriate supportive care, (mechanical ventilation) Maximal calories should be provided in the form of intravenous glucose and lipids in an effort to reduce catabolism. Plans should be immediately made to initiate hemodialysis in infants who are encephalopathic and have plasma ammonia levels over 10 times the upper limit of normal. Metabolic & Molecular Basis of Inherited Disease Metabolic Disorders of Urea Cycle Urea Cycle Disorders (Treatment) Maintenance therapy dietary protein restriction+supplementation with citrulline or arginine+ the use of drugs The primary drug now used( provides an alternate pathway for waste nitrogen excretion) for maintenance therapy in patients with urea cycle disorders is sodium phenylbutyrate (Buphenyl). The drug is typically administered four times a day in a dose of 0.4 to 0.6 g/kg/day. It is supplied as a powder, which can be mixed with food or formula, or as a tablet. Metabolic & Molecular Basis of Inherited Disease Metabolic Disorders of Urea Cycle Urea Cycle Disorders (Treatment) Liver transplantation for Severe neonatal OTC and CPS deficiency. Liver failure and cirrhosis in ASL deficiency. Failed medical-pharmacologic treatment. Pretransplant care by aggressively managing intercurrent hyperammonemia, vaccinations and prophylaxis are given against infectious appropriate caloric intake Gene replacement Metabolic Disorders of Urea Cycle Metabolic & Molecular Basis of Inherited Disease Genetic deficiencies in some of the urea-cycle enzymes can be treated pharmacologically benzoate CO2- CO2- ATP + CoA-SH AMP + PPi ATP + CoA-SH AMP + PPi O S-CoA S-CoA benzoyl-CoA O glycine CoA-SH hippurate (benzoylglycine) phenylacetate phenylacetyl-CoA glutamine CoA-SH O N H H N CO2- CO2- phenylacetylglutamine O O NH2 The amide products of these reactions (hippurate and phenylacetylglutamine) are excreted in the urine. Replenishing the Gly or Gln removes ammonia.