* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Membrane Receptors for Antigen
Complement system wikipedia , lookup
Immunocontraception wikipedia , lookup
Lymphopoiesis wikipedia , lookup
Gluten immunochemistry wikipedia , lookup
Human leukocyte antigen wikipedia , lookup
Monoclonal antibody wikipedia , lookup
Psychoneuroimmunology wikipedia , lookup
Immune system wikipedia , lookup
Innate immune system wikipedia , lookup
Duffy antigen system wikipedia , lookup
DNA vaccination wikipedia , lookup
Immunosuppressive drug wikipedia , lookup
X-linked severe combined immunodeficiency wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
Molecular mimicry wikipedia , lookup
Adaptive immune system wikipedia , lookup
Adoptive cell transfer wikipedia , lookup
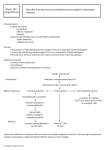
How Cells of the Immune System “See” and Respond to Antigen Immunoglobulin Class I MHC Membrane Receptors for Antigen • B-cell surface Receptor (BCR) – anchored Immunoglobulin • T-cell receptor (TCR) • Major Histocompatiblility Complex (MHC) – Class I molecules – Class II molecules • NK receptors B and T Lymphocytes • B-cells make Immunoglobulin – both secreted and on the surface • T-cells are lymphocytes that play a key role in the humoral (Ig) immune response, and also carry out their own recognition functions (cytotoxic lymphocytes) • T-cells have receptors that are similar to Ig molecules in several respects … Similarity of Ig and TCRs : • The TCR has two polypeptide chains, a and b that together form the antigen-combining site (just as Ig has the H and L chains) • The TCR chains each have two domains, a C and V, with folded structure that is similar to the C and V domains in the Fab arms of Ig. Ig and TCRs are similar: • The TCR has two polypeptide chains, a and b that together form the antigen-combining site (just as Ig has the H and L chains) • The TCR chains each have two domains, a C and V, with folded structure that is similar to the C and V domains in the Fab arms of Ig. • The antigen-combining region of the TCR are made up of 6 CDRs, three from each chain. CDRs on both the Ig and TCR variable regions Immunoglobulin Fab, H+L (one chain) T-cell receptor, a and b chains Ig and TCRs are similar: • The TCR has two polypeptide chains, a and b that together form the antigen-combining site (just as Ig has the H and L chains) • The TCR chains each have two domains, a C and V, with folded structure that is similar to the C and V domains in the Fab arms of Ig. • The antigen-combining region of the TCR are made up of 6 CDRs, three from each chain. • The high degree of variability in the variable regions (and CDRs) is mainly due to recombination in the DNA of developing T-cells in which one of several V, J and (in the b subunit) D regions are joined to create millions of different possible combinations. Gene rearrangements in different combinations of V, D and J segments provide for a huge number of different TCRs Although there are these interesting similarities between the B-cell receptor (Ig) and the TCR, there is one really key difference: While the B-cell receptor can recognize antigen alone, T-cell receptors recognize and antigen only when it is in the context of a Class I or Class II MHC molecule. What is a MHC molecule, you ask? Well…. The Major Histocompatiblity Complex, or MHC • BCRs (surface Igs) and TCRs both recognize a variety of chemical structures, but B-cells (as with the Igs they secrete) can “see” antigens in isolation • T cells recognize antigens when they are associated with normal cells -- they recognize “foreign” in the context of “self” • The “self” they see are molecules of the Major Histocompatilbity Complex, or MHC • They are called “histocompatiblity” antigens because they were first recognized as provoking graft rejection, because they seen as “not self” by T-cells, and an immune response is elicited • If you can find an individual with a similar (or better yet, identical) set of MHC antigens, they will be seen as “self” and not rejected There are two kinds of MHC Molecule: Class I and Class II • Class I molecules are expressed in nearly every cell type in the body – The TCRs of Cytotoxic lymphocytes see viral and tumor antigens when they show up on normal cells: foreign Ags “ in the context of Class I molecules “ • Class II molecules are expressed only on cells of the immune system, mostly macrophages and B cells – When these cells take in Ag, some of it is put back out on the cell surface with a Class II molecule – a way of focusing attention on this unusual bit, and encouraging an immune response. Class I Class II Both types of molecules have two polypeptides, and a domain structure similar to that of Ig and TCR, especially in those domains that are closest to the membrane Class I MHC molecules • Expressed on nearly all cells of the animal, though are more abundant on some cells than others • In humans there are three main genes, located on Chromosome 6, called HLA-A, HLA-B and HLA-C (HLA stands for Human Leukocyte Antigen – they were originally called antigens because animals make antibodies against MHC molecules from different individual) • These genes are polymorphic, meaning that are many different alleles (or versions) of each gene in the human population. Class I MHC proteins The TCRs of Cytotoxic lymphocytes see viral and tumor antigens when they show up on normal cells: foreign Ags “in the context of Class I molecule” (CD8 is also involved) Class II MHC molecules • Expressed on cells of the immune system, mainly macrophages and B-cells • In humans there are three main genes, located on Chromosome 6, called HLA-D – there are many genes, each with several alleles • These are also important to match in tissue transplantation, especially if lymphocytes are transplanted. • MHC Class II molecules are important in achieving good Antibody responses to antigen T-cell help in Antibody generation Class II molecules are important in the humoral immune response because they present antigen to T cells that enhance the immune response • Foreign antigens are engulfed by macrophages, non-specifically • The macrophage partially degrade the antigen, and pieces are bound to Class II molecules in the internal membrane system of the cell • These are put out on the surface: Antigen is presented in the context of Class II MHC molecules • The TCR on CD4+ T cells can now “see the foreign antigen – it is in the context of the Class II molecule (which CD4 helps to bind) • The T-cell is activated…. The interaction stimulates both the T-cell and the macrophage: • T-cell – Stimulated to secrete IL-2 • stimulates the T-cell to proliferate -- expansion of clones that can see this antigen • Macrophage – stimulated to release IL-1 • further stimulates the T-cell • recruits other immune cells (inflammatory response) Antigen can also be presented by B-cells • Antigen can be bound to the Ig (BCR) on the surface of ‘virgin” B cells • Binding causes endocytosis, and “processing” (partial digestion) of the antigen. • Fragments of antigen bound to Class II molecules are put out to the surface • Antigen + Class II engages T-cells • The T-cell clones that can see this antigen are expanded, and secrete cytokines (IL-4 and IL-5) that stimulate the B-cells to proliferate and differentiate into plasma cells. Besides being just interesting, this explains why some molecules can be good antigens and yet not be immunogenic … • To elicit a good Ab response, a molecule must be able to be presented to T-cells • If it is not big enough to bind to the Class II molecule and the T-cell receptor at the same time, it may fail to recruit T-cell help • The B-cells that will recognize it may be activated, but without the help, the response will be poor. • Small molecules, including peptides, need to be attached to carrier molecules in order to elicit a good responses. Practical Issues in Ab Production (some may make more sense now that we have looked at T-cell help) • • • • • Purity and Integrity of Antigen Form of antigen Animals Adjuvant Route of injection, dose etc Antigen • How pure should it be? … – For polyclonals, purified is best. – If you can “clean it up” in the serum, you do not need to start with a pure Ag – Antigen-affinity column – Adsorb “out” other antibodies – For monoclonals it is less of an issue (more unwanted clones, but if you can screen them out….) Antigen, other considerations • Native or denatured antigen (SDS-PAGE gel slices) – but if denatured, you may not get as many “native” epitopes • Peptides – Need carrier protein (T-cell help). – Abs raised to peptides may not recognize native molecule well Depends on how much information you have • Particulate Ags tend to work well because they are easily phagocytized (for Ag presentation) Animals • Species considerations: – Size/cost – Phylogenetic distance (not good to use mouse for Abs to a mouse Ab. Chickens are sometimes used for this reason. – Useful Ig properties, such as IgY (birds) or Ig (llamas) – Monoclonals are usually mouse, unless phylogenetic distance is needed. (Also mice are more limited in the varriety of Class II molecules they have b/c they are inbred, but outbred strains are available ) • Several animals are generally done to provide more heterogeneity in Class II options • (empirically animals differ in their response, so do >1 Injections • Adjuvant – An emulsion of mineral oil/water (Freund’s) that will hold the Ag in place long enough for macrophages to get there – May contain an irritant to cause local inflammation (“Complete” adjuvant) to recruit cells of immune response • Route of injection, does per injection and period of time between boosts – depend on the animal, whether adjuvant is used, the nature of the antigen, and experience (empirical) … people base their practices on history