* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Lesson 11Adaptive Immunity“Specific Immunity”
Psychoneuroimmunology wikipedia , lookup
Immune system wikipedia , lookup
Lymphopoiesis wikipedia , lookup
Molecular mimicry wikipedia , lookup
Monoclonal antibody wikipedia , lookup
Innate immune system wikipedia , lookup
Adaptive immune system wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
Adoptive cell transfer wikipedia , lookup
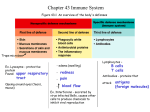
Lesson 11 Adaptive Immunity “Specific Immunity” March 31,2015 Immunity Review • Innate Immunity: defenses against any pathogen – Skin – Phagocytes – Inflammation – Fever • Adaptive Immunity: induced resistance to a specific pathogen – Humoral (antibodies) – Cell-mediated Figure 17.20 The dual nature of the adaptive immune system. Humoral (antibody-mediated) immune system Cellular (cell-mediated) immune system Control of freely circulating pathogens Control of intracellular pathogens Intracellular antigens are expressed on the surface of an APC, a cell infected by a virus, a bacterium, or a parasite. Extracellular antigens A B cell binds to the antigen for which it is specific. A Tdependent B cell requires cooperation with a T helper (TH) cell. T cell Cytokines activate T helper (TH) cell. Cytokines activate macrophage. Cytokines Cytokines A T cell binds to MHC– antigen complexes on the surface of the infected cell, activating the T cell (with its cytokine receptors). B cell The B cell, often with stimulation by cytokines from a TH cell, differentiates into a plasma cell. Some B cells become memory cells. Cytokines from the TH cell transform B cells into antibody-producing plasma cells. Cytotoxic T lymphocyte Plasma cell Plasma cells proliferate and produce antibodies against the antigen. Activation of macrophage (enhanced phagocytic activity). TH cell Memory cell Some T and B cells differentiate into memory cells that respond rapidly to any secondary encounter with an antigen. Lysed target cell The CD8+T cell becomes a cytotoxic T lymphocyte (CTL) able to induce apoptosis of the target cell. Dual Nature of Adaptive Immunity • Main components of Adaptive Immunity are T cells and B cells • The fetal liver serves as the source of both T and B cells early in development and in bone marrow in adulthood – T cells develop in thymus in adults – B cells develop in the red bone marrow in adults Figure 17.8 Differentiation of T cells and B cells. Stem cells develop in bone marrow or in fetal liver Stem cell (diverges into two cell lines) Red bone marrow of adults Thymus Differentiate to B cells in adult red bone marrow Differentiate to T cells in thymus B cell T cell Migrate to lymphoid tissue such as spleen, but especially lymph nodes Dual Nature of Adaptive Immunity • Humoral Immunity – Due to antibodies – B cells mature in the bone marrow • Name derived from chickens: bursa of Fabricius – Bursa is an organ found in chickens that when removed results in the abrogation in antibody production Dual Nature of Adaptive Immunity • Cellular Immunity – Due to T cell activation – T cells mature in the thymus 1. 2. 3. Stimulate the production macrophages and other phagocytes Activate B-cells into becoming plasma cells Activate Cytotoxic T-Lymphocytes The Nature of Antigens • Antigen (Ag): a substance that causes the body to produce specific antibodies or sensitized T cells “foreign molecules” – Microbial cell wall components, proteins, capsules, flagella, toxins, viral coats – Non-microbial agents such as blood cell surface molecules can serve as antigens • Organ rejection – Antibodies (Ab) interact with epitopes, or antigenic determinants which are specific regions on the antigen – Hapten: antigens that are too small to stimulate a immune response. Require carrier molecules Figure 17.1 Epitopes (antigenic determinants). Antibody A Epitopes (antigenic determinants) on antigen Antigens: components of cell wall Binding sites Bacterial cell Antibody B Figure 17.2 Haptens. Hapten molecules Carrier molecule Hapten-carrier conjugate The Nature of Antibodies • Globular proteins called Immunoglobulins • Antigen-binding sites (ABS) are parts of the antibody that binds the epitope • Valence refers to the number of antigen binding sites on an antibody – Two binding sites are bivalent (most common) – One binding site is monovalent Figure 17.3ab The structure of a typical antibody molecule. Antigenbinding site Fc (stem) region Hinge region Antibody molecule Epitope (antigenic determinant) Antigenbinding site Enlarged antigen-binding site bound to an epitope Antigen IgG Antibodies • • • • Monomer 80% of serum antibodies Fixes complement Found in blood, lymph, and intestine • Cross placenta (passive immunity) • Enhance phagocytosis; neutralize toxins and viruses; protect fetus and newborn • Half-life = 23 days IgM Antibodies • Pentamer • 5–10% of serum antibodies • Fixes complement • In blood, in lymph, and on B cells • Agglutinate microbes; first Ab produced in response to infection • Half-life = 5 days Disulfide Bond J-Chain IgA Antibodies • Dimer • 10–15% of serum antibodies • In secretions • Mucosal protection • Secretory Component protects Ab from degradation • Most abundant antibody in the body • Half-life = 6 days J-Chain Secretory Component IgD Antibodies • Monomer • 0.2% of serum antibodies • In blood, in lymph, and on B cells • On B cells, initiate adaptive response • Half-life = 3 days IgE Antibodies • Monomer • 0.002% of serum antibodies • On mast cells, on basophils, and in blood • Allergic reactions; lysis of parasitic worms • Attracts complement and phagocytic cells • Half-life = 2 days Activation of B Cells • B-cells, when activated, become either plasma cells (Ab producers) or memory cells (responsible for enhanced secondary response) • B-cells are capable of producing multiple Abs (IgM, IgG, IgA) with the same antigenic determinants (class switching) • Major histocompatibility complex (MHC) expressed on mammalian cells are responsible for antigenic determinants – Molecules containing glycoproteins – Found on Antigen-presenting cells (APC) and lymphocytes – Presents antigen on the surface of the B cell • T-dependent antigens – Ag presented with (self) MHC to TH cell • Distinguishes (self) from antigen to prevent antibody production against host cells – Lupus, Type I diabetes, and rheumatoid arthritis – TH cell produces cytokines that activate the B cell • T-independent antigens – Antigens stimulate B cells directly to make Abs – Antigens are characterized by repeating subunits that bind multiple B cell receptors • Polysaccharides • Lipopolysaccharides Figure 17.4 Activation of B cells to produce antibodies. Extracellular antigens Ag fragment MHC class II with Ag fragment MHC class II with Ag fragment displayed on surface Antibodies B cell B cell B cell Immunoglobulin receptors coating B cell surface Immunoglobulin receptors on B cell surface recognize and attach to antigen, which is then internalized and processed. Within the B cell a fragment of the antigen combines with MHC class II. TH cell Plasma cell Cytokines MHC class II–antigenfragment complex is displayed on B cell surface. Receptor on the T helper cell (TH) recognizes complex of MHC class II and antigen fragment and is activated— producing cytokines, which activate the B cell. The TH cell has been previously activated by an antigen displayed on a dendritic cell (see Figure 17.10). B cell is activated by cytokines and begins clonal expansion. Some of the progeny become antibodyproducing plasma cells. Figure 17.6 T-independent antigens. Polysaccharide (T-independent antigen) Epitopes B cell receptors Figure 17.5 Clonal selection and differentiation of B cells. Stem cell Stem cells differentiate into mature B cells, each bearing surface immunoglobulins against a specific antigen. Antigen B cells I II III IV B cell III complexes with its specific antigen and proliferates. Memory cells Some B cells proliferate into long-lived memory cells, which at a later date can be stimulated to become antibodyproducing plasma cells. See Figure 17.17. Other B cells proliferate into antibody-producing plasma cells. Plasma cells Plasma cells secrete antibodies into circulation. Antigens in circulation now attached to circulating antibodies Cardiovascular system Activation of B Cells • Clonal Deletion eliminates harmful B cells – MHC molecules that contain self-antigens – Process in which the immune system does not attack an antigen is called immune tolerance • Gestational immune tolerance protects a baby from the immune system of the parent – Produces cytokines to inhibit immune system detection (neurokinin B) – Do not contain receptors that bind cytotoxic Tcells Antigen-Antibody Binding • Affinity—is the strength of a bond b/w antigen and antibody – Antibodies recognize the shape of an antigen – Better the fit b/w the antigen’s shape and Ab the stronger the affinity – Abs are highly specific (discern minor differences in antigens) Results of Antigen–Antibody Binding 1. 2. 3. 4. Agglutination Opsonization Activation of complement Antibody-dependent cell-mediated cytotoxicity 5. Neutralization Figure 17.7 The results of antigen–antibody binding. PROCTECTIVE MECHANISM OF Activation of complement BINDING ANTIBODIES (see also Figure 18.5) (see also Figure 16.9) TO ANTIGENS Causes inflammation and Reduces number of infectious units to cell lysis be dealt with Complement Agglutination Bacteria Bacterium Lysis Antibody-dependent cell-mediated cytotoxicity Opsonization (see also Figure 16.9) (see also Figure 17.16) Antibodies attached to target cell cause destruction by macrophages, eosinophils, and NK cells Coating antigen with antibody enhances phagocytosis Phagocyte Eosinophil Epitopes Large target cell (parasite) Neutralization (see also Figure 18.9) Blocks adhesion of bacteria and viruses to mucosa Virus Bacterium Blocks attachment of toxin Toxin Perforin and lytic enzymes T Cells and Cellular Immunity • T cells are derived from stem cells of bone marrow • These stem cells migrate to the thymus where they mature into T cells – Thymic selection eliminates many immature T cells • Similar to clonal deletion of B cells. Weed out cells that would otherwise attack “self” • Mainly responsible for clearance of intracellular bacteria Table 17.2 Principal Cells That Function in Cell-Mediated Immunity T Cells and Cellular Immunity • T cells require antigen-presenting cells (APCs) to become activated • T cells respond to Ag by T-cell receptors (TCRs) – Similar to antibodies on the surface of B cells • Pathogens entering the gastrointestinal or respiratory tracts pass through: – M (microfold) cells over – Peyer’s patches (secondary lymphoid organs), which contain APCs • T cells are characterized by glycoproteins on surface – CD4—bind to MHC II molecules (found on lymphocytes) – CD8—bind to MHC I molecules (present on all nucleated cells) Figure 17.9 M cells. (a) M cell on Peyer’s patch. Note the tips of the closely packed microvilli on the surrounding epithelial cells. Antigen M cell Microvilli on epithelial cell TH cell Pocket B cells Macrophage Epithelial cell (b) M cells facilitate contact between the antigens passing through the intestinal tract and cells of the body’s immune system. T Cell Classification • Certain glycoproteins on the surface of T cells help distinguish different classes of T cells – Clusters of Differentiation (CD) – Responsible for the adhesion of T cells to receptors – Cells containing CD4 are called CD4+ cells and cells containing CD8 are called CD8+ cells T Helper Cells • CD4+ or TH cells – TCRs recognize Ags and MHC II on APC – TLRs are a costimulatory signal on APC and TH – TH cells produce cytokines and differentiate into: • • • • • TH1cells TH2 cells TH17 cells TFH cells Memory cells T Helper Cells – TH1 produce IFN-gwhich activates cells related to cell-mediated immunity, macrophages, and Abs – TH2 activate eosinophils and B cells to produce IgE – TH17 stimulate the innate immune system – TFH stimulate B cells to produce plasma cells and are involved in class switching Figure 17.11 Lineage of effector T helper cell classes and pathogens targeted. Antibodies TH1 cells B cell TH2 cells TH17 cells Recruits neutrophils; provides protection against extracellular bacteria and fungi TH17 cells Cell-mediated immunity; control of intracellular pathogens, delayed hypersensitivity reactions (page 535); stimulates macrophages. TH cell IL-17 IL-4 IFN-g TH1 cells TH2 cells Fungi Extracellular bacteria Neutrophil Macrophage Mast cell Basophil Eosinophil Intracellular bacteria and protozoa Important in allergic responses, especially by production of IgE Stimulates activity of eosinophils to control extracellular parasites such as helminths (see ADCC, page 495). Helminth Figure 17.10 Activation of CD4+T helper cells. An APC encounters and ingests a microorganism. The antigen is enzymatically processed into short peptides, which combine with MHC class II molecules and are displayed on the surface of the APC. A receptor (TCR) on the surface of the CD4+T helper cell (TH cell) binds to the MHC–antigen complex. If this includes a Toll-like receptor, the APC is stimulated to secrete a costimulatory molecule. These two signals activate the TH cell, which produces cytokines. TH cell receptor (TCR) APC (dendritic cell) The cytokines cause the TH cell (which recognizes a dendritic cell that is producing costimulatory molecules) to become activated. T helper cell Antigen Microorganism carrying antigens Antigen fragment (short peptides) Complex of MHC class II molecule and antigen fragment Cytokines Costimulatory molecule, (required to activate T cells that have not previously encountered antigen) T Cytotoxic Cells • CD8+ or TC cells • Target cells are self-cells carrying endogenous antigens • Activated into cytotoxic T lymphocytes (CTLs) – CTLs recognize Ag + MHC I – Induce apoptosis in target cell • CTL releases perforin and granzymes Figure 17.12 Killing of virus-infected target cell by cytotoxic T lymphocyte. Processed antigen presented with MHC class I Processed antigen T cell receptors Infected target cell is lysed MHC class I Virus-infected cell (example of endogenous antigen) A normal cell will not trigger a response by a cytotoxic T lymphocyte (CTL), but a virus-infected cell (shown here) or a cancer cell produces abnormal endogenous antigens. CTL Virus-infected cell Cytotoxic T lymphocyte (CTL) The abnormal antigen is presented on the cell surface in association with MHC class I molecules. CD8+T cells with receptors for the antigen are transformed into CTLs. The CTL induces destruction of the virus-infected cell by apoptosis. Figure 17.13 Apoptosis. T Regulatory Cells • Treg cells CD4 and CD25 on surface • Suppress T cells against self Antigen-Presenting Cells • Digest antigen • Ag fragments on APC surface with MHC – B cells – Dendritic Cells – Activated Macrophages Figure 17.14 A dendritic cell. Figure 17.15 Activated macrophages. Activated macrophages Resting (inactive) macrophage Natural Killer (NK) Cells • Granular leukocytes destroy cells that don’t express MHC I • Kill virus-infected and tumor cells • Attacks parasites ADCC • Antibody-dependent cell-mediated cytotoxicity Figure 17.16a Antibody-dependent cell-mediated cytotoxicity (ADCC). KEY Macrophage Cytotoxic cytokines Lytic enzymes Perforin enzymes Eosinophil Extracellular damage Fc region Large parasite Epitope Antibody (a) Organisms, such as many parasites, that are too large for ingestion by phagocytic cells must be attacked externally. Figure 17.16b Antibody-dependent cell-mediated cytotoxicity (ADCC). Eosinophils Fluke Eosinophils adhering to the larval stage of a parasitic fluke. Cytokines • Chemical messengers – Allows for communication between cells • Overproduction leads to cytokine storm Cytokines Cytokine Representative Activity Interleukin-1 (IL-1) Stimulates TH cells in presence of antigens; attracts phagocytes Interleukin-2 (IL-2) Proliferation of antigen-stimulated CD4+ T helper cells, proliferation and differentiation of B cells; activation of CD8+ T cells and NK cells Interleukin-12 (IL-12) Inhibits humoral immunity; activates TH1 cellular immunity Cytokines Cytokine Representative Activity Chemokines Induce the migration of leukocytes TNF-α Promotes inflammation Hematopoietic cytokines Influence differentiation of blood stem cells IFN- and IFN- Response to viral infection; interfere with protein synthesis IFN-g Stimulates macrophage activity Immunological Memory • Antibody titer is the amount of Ab in serum • Primary response occurs after initial contact with Ag • Secondary (memory) response occurs after second exposure Figure 17.17 The primary and secondary immune responses to an antigen. IgG Antibody titer in serum IgM Initial exposure to antigen Time (days) Second exposure to antigen Types of Adaptive Immunity • Naturally acquired active immunity – Resulting from infection • Naturally acquired passive immunity – Transplacental or via colostrum • Artificially acquired active immunity – Injection of Ag (vaccination) • Artificially acquired passive immunity – Injection of Ab Terminology of Adaptive Immunity • Serology: the study of reactions between antibodies and antigens • Antiserum: the generic term for serum because it contains Ab • Globulins: serum proteins • Immunoglobulins: antibodies • Gamma (g) globulin: serum fraction containing Ab