* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Beals syndrom
Gene therapy wikipedia , lookup
Neuronal ceroid lipofuscinosis wikipedia , lookup
Neocentromere wikipedia , lookup
Gene expression programming wikipedia , lookup
Artificial gene synthesis wikipedia , lookup
Oncogenomics wikipedia , lookup
Frameshift mutation wikipedia , lookup
X-inactivation wikipedia , lookup
Point mutation wikipedia , lookup
Designer baby wikipedia , lookup
Medical genetics wikipedia , lookup
Pectus excavatum wikipedia , lookup
Microevolution wikipedia , lookup
Genome (book) wikipedia , lookup
Down syndrome wikipedia , lookup
Saethre–Chotzen syndrome wikipedia , lookup
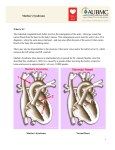
Team B Dr.Osama Mudhafar Pediatric History : Saad is a 9 month old , Saudi boy , He was admitted through the ER with history of coughing , S.O.B. and cyanosis . There was no history of fever , diarrhea , or constipation . No history of contact with patient with URTI. Cont.. He is known to have : Beals syndrom. chronic lung disease with recurrent chest infections. Past medical history : He is a product of FT , SVD ,born in MCH hospital with Bwt 2.9 kg , he was discharged with the mother in good general condition . At 40 days of life , he was admitted in our PMW with history of cough , S.O.B. and cyanosis . Then he was transferred to PICU for 28 days , intubated for 14 days and diagnosed as bronchiolitis . At 4 moths of age , he was admitted with a history of the same problem . Also at 5 months of age , he was admitted through the ER to PMW with chest infection .This admission he was admitted PICU but not intubated . Past surgical history : negative Vaccination : up to date Nutrition : on bottle feeding Developmental : he is 9 month and supporting head , and set with support and can roll on the bed and cannot set without support . He can hear and see normally . Review of system : unremarkable . Blood transfusion : he received PRBCs in first admission. Social history : they live in Jeddah , Kilo 3 , his father works in the airport and the mother is a housewife . Family history : There is no consanguinity , he is the first and the only child in the family .no family history of the same problem . There is FH of bronchial asthma . Physical Examination : General : he is conscious , alert and active . He looks dysmorphic with large ears , depressed nasal bridge , micrognathia , high arched palate , short neck , long and cylindrical fingers and toes . Vitally : stable , on 0.5 L O2 saturation is 95 % . Chest : intercostal ,subcostal and suprasternal recession , AE bilaterally and minimal crepitation . CVS : S1 + S2 + 0 Abdomen : soft , lax , liver is 2 cm BCM and no splenomegally . CNS : tone , normal reflexes and power . Extremities : long limbs , fingers and toes . Joint contractures especially in the knee and elbow joints , Ophthalmology : ? Irido coloboma , normal ocular movement , no lens sublaxation . Investigations : general : CBC : last WBC 18.6 Hb 11.4 Plt 509 U&E : normal . Ca , 2.38 PO4 2.8 ALP 40 Mg 0.88 Partial septic screen : -ve CXR : emphysematous changes CT chest : narrowing of the main bronchi , emphysematous changes. Sweat chloride test : 34 mEq Investigations : specific : Chromosomal analysis :has been done but the results are not in our hand Echo : mild TR and PFO , normal ventricular function and size . CT angio : -aortic root measures 22.5 mm in transverse diameter ( needs expert evaluation to decide aortic dilatation or not ) -ascending aorta measures 14.5 mm -descending, thoracic and abdominal aorta no evidence of dilatation . MRI brain : normal study . EEG : normal study . Beals Syndrome Team B Dr.Osama Mudhafar Pediatric medical Intern. Names : Beals syndrome Beals-Hecht syndrome; first described by Beals and Hecht in 1971 Congenital contractural arachnodactyly, (CCA); Arthrogryposis, distal, type 9. Definition: Congenital contractural arachnodactyly (CCA; Beals syndrome) is an autosomal dominantly inherited connective tissue disorder that shares phenotypical features with Marfan syndrome (MFS). Beals syndrome has distinct features however, and is caused by a mutation in the fibrillin-2 gene (FBN2) in 5q23, while Marfan syndrome is caused by mutations in fibrillin-1 Epidemiology The incidence of Beals $ is unknown Prevalence is difficult to estimate considering the overlap in phenotype with Marfan $. Etiology Beals $ is an autosomal dominantly inherited single gene disorder . caused by a mutation in FBN2 gene on chromosome 5q23 . Dysmorphic Terms : Camptodactyly : is permanent contraction in the joints . Arachnodactyly : is long webbed fingers or toes ( spider like ) Dolichostenomelia : the limbs are disproportionally long compared with the trunk . Clinical Description at birth with clenched position of hands (fist-like), their ears having a crumpled irregular superior helix and prominent antihelix and root of helix . (may become milder with age) fingers are long and there is elongation of phalanges on X-rays. (Arachnodactyly) Pectus carinatum Clinical Description ( cont..) Striae. highly arched palate Contractures of varying degrees at birth mainly involving the large joints, are present in all affected children. Elbows, knees and fingers are most commonly involved. The contractures may be mild and tend to reduce in severity, but residual camptodactyly always remains present . Clinical Description ( cont..) cardiovascular involvement ( CHD , Mitral valve prolapse ,aortic arch dilation ) Ophthalmologic abnormalities (heterotopia, Ectopia lentis is very rare. blue sclerae and glaucomatous optic disc cupping, and partial coloboma of the lens, mild cataract, abnormal cilliary body and glaucoma were reported ) Clinical Description ( cont..) mentally normal Delay in the motor development is common (due to contractures ) Dislocation of joints, especially patellae scoliosis and sometimes kyphoscoliosis Lethal form of Beals $ : A single report described a mother and daughter with classic and severe lethal Beals . cardiac abnormalities as septal defects, interrupted aortic arch single umbilical artery duodenal atresia, esophageal atresia, and intestinal malrotation Differential diagnosis: Beals $ Muta. FBN 2 chrom 5q23 Marfan $ FBN 1 chrom 15q21 share Marfanoid habitus , arachnodactyly , camptodactyly , dolichostenomelia , scoliosis and kyphoscoliosis . knee dislocations , high arched palate , they also overlap in ( CVS , ophth , respiratory,joints..) features . Respir Pectus carinatum or exavatum Spont. Pneumothorax Dura - Dural ectasia(dilat.) CVS MR Aortic dilat.(<2SD) M prolapse, AR Aortic dilat(>2SD) Aortic dissection Dysrhythmia Joints Contracturs and hyperlaxity . ophth Partial coloboma , mild glucoma&cataract Micrognathia , crumbled ears. Lens dislocation , retinal detachment , ectopia lentis Why Beals and Marfan shares clinical features ? The overlap in clinical features has a molecular basis. Beals and MFS result from mutations in two homologous genes, FBN2 and FBN1, which are highly similar but distinct genes situated in 5q23-31 and 15q15-21.3 chromosome, respectively Beals Vs Marfan Now it is proven that the original patient first described by Dr. Antoine Marfan in 1898 has been stated to have Beals, rather than MFS !!! Is there a relationship between Beals & Respiratory diseases ? The answer will be in part II Management : Is symptomatic For contractures: physiotherapy and/or surgery . For CHD : echo, CT angio and F/U Ophthalmologic evaluation is recommended Genetic counseling is recommended There is no evidence of shortened lifespan. Individuals with Beals are to live normal lives unless complicated with cardiac problems or severe deformity of the vertebrae.. Antenatal diagnosis Molecular antenatal diagnosis: is possible if indicated and desired by the parents after appropriate genetic counseling. Ultrasound imaging: may be used to demonstrate joint contractures and hypokinesia in suspected cases. Thank You….