* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download POTASSIUM BALANCE
Cell membrane wikipedia , lookup
Extracellular matrix wikipedia , lookup
Tissue engineering wikipedia , lookup
Cytokinesis wikipedia , lookup
Cellular differentiation wikipedia , lookup
Membrane potential wikipedia , lookup
Endomembrane system wikipedia , lookup
Cell culture wikipedia , lookup
Cell encapsulation wikipedia , lookup
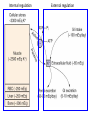
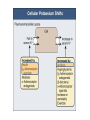
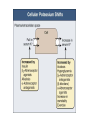
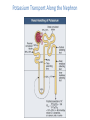
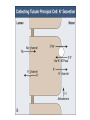
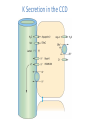
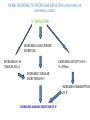
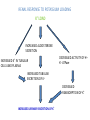
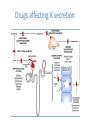
POTASSIUM BALANCE Ronen L, MD NEPHROLOGY AND HYPERTENSION SERVICES HADASSAH UNIVERSITY HOSPITAL Internal regulation External regulation Role of Insulin and β-adrenergics on the Distribution of K Shift of K Out of cells in Metabolic Acidosis Monocarboxylic acids enter the cells in an electorneutral fashion. Therefore they do not cause a change in cell voltage. H load of inorganic acid is titrated by HCO3 in the ECF→ ↓ cell voltage→ K shifts out of cell Potassium Transport Along the Nephron K Secretion in the CCD Factors Affecting Potassium Secretion From the Tubular Cell to the Lumen • K+ concentration gradient across the luminal membrane • Electrical gradient across the tubular cell • K+ permeability of the luminal membrane Effects of aldosterone actions in principal cells • Increases the permeability of the luminal membrane to Na by increasing the number of open ENaC→ increases electrical gradient across the tubular cell • Increases the permeability of the luminal membrane to K by increasing the number of open K channels • Enhances the activity of the Na-KATPase at the basolateral membrane→ increases cell K concentration Regulation of Potassium Secretion- Serum Potassium Concentration • Direct effects: enhances Na+-K+-ATPase activity, increases luminal permeability to K+ and Na+. • Indirect effect: increases aldosterone secretion. Regulation of Potassium Secretion- Distal Flow Rate • Increase in distal flow rate enhances K+ secretion. • It dilutes K+ secreted from the tubular cells to the lumen, and by doing so increases the K+ CONCENTRATION GRADIENT. • High flow rate also delivers more Na+ to the distal tubule, more Na+ is reabsorbed, and the gradient across the tubular cells rises, promoting K+ SECRETION. RENAL RESPONSE TO POTASSIUM DEPLETION (LOW INTAKE OR NON RENAL LOSSES) K+ DEPLETION DECREASED ALDOSTERONE SECRETION DECREASED K+ IN TUBULAR CELLS INCREASED ACTIVITY OF H+K+-ATPase DECREASED TUBULAR EXCRETION OF K+ INCREASED REABSORPTION OF K+ DECREASED URINARY EXCRETION OF K+ RENAL RESPONSE TO POTASSIUM LOADING K+ LOAD INCREASED ALDOSTERONE SECRETION K+ INCREASED IN TUBULAR CELLS AND PLASMA DECREASED ACTIVITY OF H+K+-ATPase INCREASED TUBULAR EXCRETION OF K+ DECREASED REABSORPTION OF K+ INCREASED URINARY EXCRETION OF K+ HYPOKALEMIA • DECREASED NET INTAKE • INCREASED ENTRY INTO CELLS • INCREASED GASTROINTESTINAL LOSSES • INCREASED URINARY LOSSES • INCREASED SWEAT LOSSES • DIALYSIS • POTASSIUM DEPLETION WITHOUT HYPOKALEMIA Major causes of hypokalemia Decrease potassium intake Increased entry into cells An elevation in extracellular pH Increased availability of insulin Elevated β-adrenergic activity- stress or administration of beta agonists Hypokalemic periodic paralysis Marked increase in blood cell production Hypothermia Major causes of hypokalemia Increased gastrointestinal losses Diarrhea* Lower GI losses due to villous ademoma, VIPoma * Laxative abuse * usu. Decreased intake and volume depletion leading to increased aldosterone contribute Major causes of hypokalemia Increased urinary losses Diuretics Primary mineralocorticoid excess Loss of gastric secretions Nonreabsorbable anions Renal tubular acidosis Salt-wasting nephropathies - including Bartter's or Gitelman's syndrome Liddle’s syndrome Amphotericin B Hypomagnesemia Polyuria Causes of Mineralocorticoid Excess • PRIMARY HYPERALDOSTRONISM A. Adenoma B. Hyperplasia C. Carcinoma • CUSHING DISEASE • LIDDLE’S SYNDROME • CHRONIC INGESTION OF EXOGENOUS MINERALOCORTICOID • HYPERRENINISM A. Renal artery stenosis B. Renin secreting tumor • HYPERSECRETION OF DEOXYCORTICOSTERONE OR OTHER MINERALOCORTICOID • LICORICE or CABENOXOLONE INGESTION- inhibits 11b-hydroxysteroid dehydrogenase which converts cortisol to cortisone • APPARENT MINERALOCORTICOID EXCESS Liddle’s syndrome • Autosomal dominant. Characterized by activating mutation in collecting duct Na+ channel with enhanced sodium reabsorption. Low renin, low aldosterone levels. • The clinical picture mimics primary hyperaldosteronism: hypertension, hypokalemia and alkalosis Barrter’s and Gitelman’s syndromes • Impairment in one of the transporters involved in sodium chloride reabsorption in the loop of Henle (Bartter’s) and distal tubule (Gitelman’s) • The tubular defects in sodium chloride transport are almost identical to that seen with chronic ingestion of a loop diuretic (mimicking Bartter syndrome) or a thiazide diuretic (mimicking Gitelman syndrome). – Impaired sodium chloride reabsorption leads to mild volume depletion and activation of the renin-angiotensinaldosterone system. – The combination of secondary hyperaldosteronism and increased distal flow and sodium delivery enhances potassium and hydrogen secretion at the secretory sites in the connecting tubules and collecting tubules, leading to hypokalemia and metabolic alkalosis Barrter’s syndrome • Bartter syndrome is an autosomal recessive disorder that often presents in childhood and may be associated with the following clinical features: Growth and mental retardation Hypokalemia Metabolic alkalosis Polyuria and polydipsia due to decreased urinary concentrating ability Normal to increased urinary calcium excretion Normal or mildly decreased serum magnesium concentration Gitelman’s syndrome • Gitelman syndrome is an autosomal recessive disorder that presents with hypokalemia, metabolic alkalosis, hypomagnesemia, hypocalciuria, and normal blood pressure • Manifestations include:: Cramps of the arms and legs, due at least in part to hypokalemia and hypomagnesemia Fatigue, which may be severe polyuria and nocturia Collecting duct Na HCO3 proximal convuluted tubule Hypokalemia– Sympatology • Muscle weakness or paralysis • Cardiac arrhythmias • Rhabdomyolysis • Renal dysFx Impaired concentration ability Increased ammonia production Impaired urinary acidification Increased bicarbonate reabsorption Renal insufficiency Hypokalemia– ECG • ST depression • Decreases amplitude of T wave • Increased amplitude of U wave • Prolongation of PR interval • Widening of the QRS complex Hypokalemia- diagnosis ANAMNESIS PHYSICAL EXAMINATION URINARY K+ EXCRETION ACID BASE STATUS Hypokalemia– Treatment • • KCl: the most common supplement ADVANTAGES: 1. correction of alkalosis, 2. remains extracellular, and corrects membrane potential more effectively. Hypokalemia– Treatment • KCL CAN BE GIVEN ORALY OR I.V. • ORALLY- CAN BE GIVEN IN LARGE DOSES BUT CAN CAUSE GASTRIC ULCERS. • I.V SHOULD BE GIVEN VERY SLOWLY UP TO 10-20 mEq/hr, AND AT LOW CONCENTRATION, UP TO 40-60 mEq/L. Hypokalemia– Treatment • CONTINUE MONITORING K+ PLASMA LEVELS. • CONTINUE FOLLOWING CONTINUOUS LOSS OF K+ HYPERKALEMIA Hyperkalemia- Etiology • INCREASED INTAKE • EXIT OF K+ FORM CELLS TO EXTRACELLULAR FLUID • DECREASED URINARY EXCRETION Hyperkalemia– Etiology: Increased Intake • Rare as a cause for hyperkalemia when renal K+ excretion is intact. • Acute K+ load, oral or IV. Can cause transient hyperkalemia. Major causes of hyperkalemia Increase potassium release from cells Pseudohyperkalemia Metabolic acidosis Insulin deficiency, hyperglycemia, hyperosmolality Increased tissue catabolism Beta adrenergic blockade Exercise Hyperkalemic periodic paralysis other Overdose of digitalis or related digitalis glycosides Red cell transfusion Succinylcholine Major causes of hyperkalemia Reduced urinary potassium excretion hypoaldosteronism Acute and chronic kidney disease Effective arterial volume depletion Type IV renal tubular acidosis Selective impairment of potassium excretion (normal renin and aldosterone, no Na wasting, normal antinatriuretic response to exogenous mineralocorticoids) Causes of hypoaldosteronism Aldosterone deficiency Primary Primary adrenal insufficiency Congenital adrenal hyperplasia (21- hydroxylase deficiency) Isolated aldosterone synthase deficiency Heparin and low molecular weight heparin Hyporeninenmic hypoalsdoteronism Renal disease, most often diabetic nephropathy Volume expansion, such in acute glomerulonephritis Angiotensin inhibition (ACEI, ARB, DRI) NSAIDS Cyclosporine HIV infection Some cases of obstructive uropathy Causes of hypoaldosteronism Aldosterone resistance Drugs which close the collecting tubule sodium channel Amiloride Spironolactone Triamterene Trimethoprim (high dose) Pentamidine Tubulointerstitial disease Pseudohypoaldosteronism Distal chloride shunt Drugs affecting K secretion Pseudohypoaldosteronism RESISTANCE TO ALDOSTERONE: HYPERKALEMIA, HYPOTENSION OR HYPERTENSION * ACQUIRED: mostly kidney. in tubulointerstitial diseases of the * CONGENITAL: RARE! 1. TYPE 1: salt wasting, hypotension and hyperkalemia, high levels of renin and aldosterone. Genetics: loss-offunction mutations in MR, or mutations in subunits of ENaC. 2. TYPE 2: Gordon’s syndrome: hypertension, hyperkalemia, metabolic acidosis. genetics: mutation in WNK4 or gain-of-function mutation in WNK1. Hyperkalemia- symptoms • MUSCLE WEAKNESS • CARDIAC ARRHYTHMIAS Hyperkalemia- ECG • PEAKED, NARROWED T WAVES • SHORT QT INTERVAL PRLONGATION OF PR INTERVAL • WIDENING OF QRS COMPLEX • LOSS OF P WAVE • SINE-WAVE PATTERN (QRS COMPLEX MERGES WITH THE T WAVE) ECG CHANGES IN HYPERKALEMIA Hyperkalemia- Diagnosis • ANAMNESIS • PHYSICAL EXAMINATION • CHECK FOR: pH, urea and creatinine, glucose, markers of tissue damage (LDH, CPK), ECG. TTKG- transtubular potassium gradient Hyperkalemia– Treatment • LOOK FOR ECG CHANGES! • IF ANY ECG CHANGES ARE SEEN, ONE SHOULD ACT URGENTLY! • I.V. TREATMENT AND CONTINUOUS ECG MONITORING ARE INDICATED. • BE READY WITH EXTERNAL PACEMACKER Hyperkalemia– Treatment Antagonism of cardiac effects of hyperkalemia: i.v calcium gluconate Increase K+ entry into cells: a. i.v glucose and insulin b. NaHCO3 (esp. if acidotic) c. β2-adrenergic agonists Removal of excess K+ from the body: a. Diuretics b. Cation-exchange resin: kayexalate c. Dialysis