* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download b. Ketogenic amino acids
Survey
Document related concepts
Ribosomally synthesized and post-translationally modified peptides wikipedia , lookup
Artificial gene synthesis wikipedia , lookup
Butyric acid wikipedia , lookup
Catalytic triad wikipedia , lookup
Metalloprotein wikipedia , lookup
Nucleic acid analogue wikipedia , lookup
Point mutation wikipedia , lookup
Glyceroneogenesis wikipedia , lookup
Proteolysis wikipedia , lookup
Fatty acid synthesis wikipedia , lookup
Peptide synthesis wikipedia , lookup
Protein structure prediction wikipedia , lookup
Fatty acid metabolism wikipedia , lookup
Citric acid cycle wikipedia , lookup
Genetic code wikipedia , lookup
Biochemistry wikipedia , lookup
Transcript
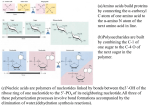
Dr. Walaa AL-Jedda – 2016/2017 Decarboxylation reaction and biogenic amines Decarboxylation is the reaction by which CO2 is removed from the COOH group of an amino acid as a result an amine is formed. The reaction is catalyzed by the enzyme decarboxylase, which requires pyridoxal-P (B6-PO4) as coenzyme. 1 Tissues like liver, kidney, brain possess the enzyme decarboxylase and also by microorganisms of intestinal tract. The enzyme removes CO2 from COOH group and convert the amino acid to corresponding amine. This is mostly a process confined to putrefaction in intestines and produces amines. Biogenic amines formed from various amino acids and their biologic importance are listed in table (27.1). 2 Some of the important biogenic amines: 1-Tyramine: Decarboxylation of tyrosine forms tyramine. This occurs in the gut as a result of bacterial action. Also this reaction takes place in kidney. The reaction is favoured by O2-deficiency. In the presence of sufficient O2, tissue deaminates tyrosine. Tyramine elevated blood pressure. 2-Tryptamine: Mammalian kidney, liver and bacteria of gut can decarboxylate the amino acid, tryptophan to form the amine " tryptamine". Tryptamine also elevate blood pressure. Hydroxylation at 5-position produces 5-OH tryptamine-5-HT (Serotonin). 3- Decarboxylation of amino acids Lysine and Arginine: Lysine and Arginine may undergo decarboxylation to corresponding "diamines" called "cadaverine" and "putrescine" respectively, which are largely excreted in feces, but are essentially non-toxic in amounts ordinarily formed. 4-Histamine: Histamine is formed by decarboxylation of amino acid "Histidine" by the enzyme Histidine decarboxylase or aromatic L-amino acid decarboxylase in presence of (B6-PO4). Site of formation: -Mast cells are the chief source of histamine in the tissues and its about 10% of the weight of mast cell granules. -Also produced by gastric mucosa cells and histaminergic neurones of the central nervous system. 3 -Basophiles are the chief source of histamine in the circulating cells. -Also produced in the gut by bacterial decarboxylation of Histidine. Mechanisms of action and effects: Histamine acts as neurotransmitter, particularly in the hypothalamus. It acts as an anaphylactic and inflammatory agent on being released from mast cells in response to antigens. Histamine markedly depresses blood pressure vascular collapse. and large doses may cause extreme 5-γ- Amino butyric acid (GABA): Formation: Decarboxylation of glutamic acid produces γ- Amino butyric acid (GABA) -glutamate α- decarboxylase is the enzyme which catalyzes the reaction, - it requires(B6-PO4) as coenzyme and Mg++ as cofactor. 4 Function of GABA: -GABA is known to serve as a normal regulator of neuronal activity being active as an inhibitor (pre-synaptic inhibition). - It is released at the axon terminals of neurons in grey matter and acts as inhibitory neurotransmitter by enhancing K+ permeability of postsynaptic membrane. Clinical Aspect: Vit. B6 deficiency in children may be responsible for some of the cases of infantile convulsions. B6 – deficiency causes less formation of GABA leading to neuronal hyper excitability and convulsions. GABA Shunt: GABA by its conversion to succinic acid can form a" by-pass" in TCA cycle. 6- Polyamines: Polyamines are: - Spermidine - Spermine Ornithine in addition to its role in urea cycle, serves as the precursor of ubiquitous mammalian and bacterial polyamines, Spermidine and Spermine. It requires active methionine. Normal human can synthesize about 0.5 nmol of Spermine /day. 5 Clinical significance: 1-Increased polyamines excretion has been claimed to characteristic of malignant disease. Thus excretion has been reported to be increased in leukemia, and in carcinoma of ovaries, lungs, colon, rectum, prostate, GI tract, kidney, bladder and testes. 2-The urinary excretion is increased (5 to 10 times) but the excretion fluctuates with the clinical state and response to treatment. Good correlation has been found between urinary excretion and clinical course. 3-However, not all patients with malignant diseases exhibit increased excretion of polyamines. 4-Spermidine is the best" marker" of tumor cell destruction, whereas putrescine is the best" marker " for cell proliferation. 6 Amino acid synthesis and degradation: Unlike fats and carbohydrates, amino acids are not stored by the body, that is, no protein exist whose sole function it is to maintain a supply of amino acids for future use. Therefore, amino acids must be obtained from the diet, synthesized denovo, or produced from normal protein degradation. - The catabolism of the amino acids found in proteins involves the removal of α-amino groups, followed by the breakdown of the resulting carbon skeletons. -These pathways converge to form seven intermediate products: pyruvate, intermediates of the TCA cycle (oxaloacetate, α-ketoglutarate, fumarate, succinyl CoA), acetyl CoA and acetoacetyl CoA. -These products directly enter the pathway of intermediary metabolism, resulting either in the synthesis of glucose or lipid, or in the production of energy through their oxidation to CO2 and water by the citric acid cycle. -Of the 20 amino acids commonly found in proteins, 11 are not essential in the adult diet, because they can be synthesized in sufficient amounts in the body, from the intermediates of metabolism or, as in the case of cysteine and tyrosine, from essential amino acids. -The essential amino acids cannot be synthesized or produced in sufficient amounts by the body and therefore, must be obtained from the diet in order for normal protein synthesis to occur. -Amino acids also can be classified as Glucogenic or Ketogenic based on which of the seven intermediates are produced during their catabolism. 7 a. Glucogenic amino acids -Amino acids whose catabolism's yield pyruvate or one of the intermediates of the TCA cycle. -These intermediates are substrates for gluconeogenesis, and therefore, can give rise to the net formation of glucose or glycogen in the liver and glycogen in the muscle. b. Ketogenic amino acids -Amino acids whose catabolism's yield either acetoacetate or one of its precursors (Acetyl CoA or acetoacetyl CoA). -Leucine and lysine are the only exclusively ketogenic amino acids. -These cannot give rise to the net formation of glucose or glycogen in the liver or glycogen in the muscle. 8 Synthesis of amino acids 1-Amino acids derived from intermediates of glycolysis -Glycolytic intermediates 3- phosphpglycerate serves as precursor for serine, glycine, cysteine, and alanine. 2-Amino acids derived from TCA cycle a. Oxaloacetate serves as precursor for aspartate and asparagine. b. α-ketoglutarate serves as precursor for glutamate, glutamine, proline and arginine 9 3-Tyrosine: the 11th non-essential amino acid is synthesized from the essential amino acid phenylalanine Degradation of amino acids -When the carbon skeletons of amino acids are degraded, the major products are pyruvate, intermediates of TCA cycle, acetyl-CoA, and acetoacetate. 1.Amino acids that are converted to pyruvate are serine, glycine, cysteine, and alanine. 10 11 2.Amino acids that are converted to intermediates of TCA cycle a- Amino acids that formed α-ketoglutarate are glutamate, glutamine, proline arginine and histidine. b- Amino acids that formed succinyl –CoA are threonine, methionine, valine and isoleucine. 12 c- Amino acids that formed fumarate are phenylalanine, tyrosine and aspartate. d- Amino acids that formed oxaloacetate are aspartate and asparagines 3.Four amino acids (lysine, threonine, isoleucine and tryptophan) can form acetylCoA. Phenylalanine and tyrosine form acetoacetate. Leucine is degraded to form both acetyl-CoA and acetoacetate. 13 14 15