* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Adrenergic receptor antagonists
Pharmaceutical industry wikipedia , lookup
Discovery and development of TRPV1 antagonists wikipedia , lookup
Prescription costs wikipedia , lookup
Pharmacogenomics wikipedia , lookup
CCR5 receptor antagonist wikipedia , lookup
Toxicodynamics wikipedia , lookup
5-HT2C receptor agonist wikipedia , lookup
Pharmacognosy wikipedia , lookup
NMDA receptor wikipedia , lookup
Nicotinic agonist wikipedia , lookup
Discovery and development of antiandrogens wikipedia , lookup
Drug interaction wikipedia , lookup
Discovery and development of angiotensin receptor blockers wikipedia , lookup
5-HT3 antagonist wikipedia , lookup
Discovery and development of beta-blockers wikipedia , lookup
Cannabinoid receptor antagonist wikipedia , lookup
Neuropharmacology wikipedia , lookup
Psychopharmacology wikipedia , lookup
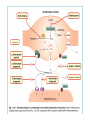
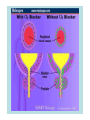
Adrenergic receptor antagonists Dr. Erika Pintér 2013 Alpha receptor antagonists They antagonize the effects of NA and adrenalin on adrenoceptors -non selective: acting on 1 and 2 phentolamine Short acting , reversible Side effects: tachycardia (baroreflex + 2 receptor inhibition), postural hypotension phenoxybenzamine • Mechanism. Binds covalently to alpha-1 and alpha-2 adrenergic receptors. i.e. non-selective, irreversible, alpha blocker. Onset is slow requiring 10-20 minutes for formation of covalent linkages. Offset is even slower with a t1/2 of 24 hours. Terminated by metabolism and new receptor synthesis. Called nonequilibrium or non-competitive blocker. New receptors must be synthesized to overcome the blockade. Several (2-5) days to regenerate. • “Dirty” drug - also blocks histamine, acetylcholine, & serotonin receptors • Medical use: pheocromocytoma Selective 1 receptor blockers: They block 1 receptors in the arterioles and venules prazosin: t1/2: 3-4 h , remarkable first pass effect doxazosin terazosin – longer lasting effect, ones a day dose They act on 1B subtype Inhibit the TPR dilating arterioles and venules. Antihypertensive effect. Unwanted effects :orthostatic hypotension, reflex tachycardia, no effect on 2 receptors 1A selective blocker: tamsulosin, alfuzosin Medical use: prostate hypertrophy (relaxes the urethral sphincter) urapidil • Urapidil is sympatholytic antihypertensive drug. It acts as an α1-adrenoceptor antagonist and as an 5-HT1A receptor agonist Unlike some other α1-adrenoceptor antagonists, urapidil does not elicit reflex tachycardia, and this may be related to its weak β1-adrenoceptor antagonist activity as well as its effect on cardiac vagal drive. Urapidil is currently not approved by the U.S. Food and Drug Administration • but it is available in Europe. • Medical use: hypertensive crisis yohimbine • Yohimbine blocks presynaptic alpha-2 adrenergic receptors. Yohimbine's peripheral autonomic nervous system effect is to increase parasympathetic (cholinergic) and decrease sympathetic (adrenergic) activity. It is to be noted that in male sexual performance, erection is linked to cholinergic activity and to alpha-2 adrenergic blockade which may theoretically result in increased penile inflow, decreased penile outflow or both. It is not used anymore. side effects • Yohimbine readily penetrates the CNS and produces a complex pattern of responses in lower doses than required to produce peripheral (alpha)adrenergic blockage. These include anti-diuresis, a general picture of central excitation including elevated blood pressure and heart rate, increased motor activity, irritability and tremor. Sweating, nausea and vomiting are common after parenteral administration of the drug. Also dizziness, headache, and skin flushing have been reported. -receptor blockers They antagonize the effects of catecholamines on receptors Non-selective propranolol: remarkable first pass metabolism Parcial agonists, with intrinsic sympatomimetic activity oxprenonol pindolol acebutolol penbutolol recommended for elderly people (mild negative inotropic effect, no tolerance) Cardioselective receptor blockers: antagonist effect a 1 receptors advantage: minimal 2 inhibition metoprolol atenolol betaxolol - long lasting effect, ones a day bisoprolol nebivolol Celiprolol + blockers: labetalol medical use: pheocromocytoma, hypertensive crisis, hypertension in pregnancy Clinical uses of β-adrenoceptor antagonists Cardiovascular - angina pectoris - myocardial infarction - dysrhythmias - heart failure - hypertension Other uses: - glaucoma (e.g. timolol eye drops) - thyrotoxicosis, as adjunct to definitive treatment (e.g. preoperatively) - anxiety to control somatic symptoms (e.g. palpitations, tremor) - migraine prophylaxis - benign essential tremor (a familiar disorder) Unwanted effects The main side effects of β-receptor antagonists result from their receptor-blocking action. Bronchoconstriction This is of little importance in the absence of airways disease, but in asthmatic patients the effect can be dramatic and lifethreatening. It is also of clinical importance in patients with other forms of obstructive lung disease (e.g. chronic bronchitis, emphysema). Cardiac depression Cardiac depression can occur, leading to signs of heart failure, particularly in elderly people. Patients suffering from heart failure who are treated with β-receptor antagonists often deteriorate in the first few weeks before the beneficial effect develops. Bradycardia This side effect can lead to life-threatening heart block and can occur in patients with coronary disease, particularly if they are being treated with antiarrhythmic drugs that impair cardiac conduction. Hypoglycaemia Glucose release in response to adrenaline is a safety device that may be important to diabetic patients and to other individuals prone to hypoglycaemic attacks. The sympathetic response to hypoglycaemia produces symptoms (especially tachycardia) that warn patients of the urgent need for carbohydrate (usually in the form of a sugary drink). β-Receptor antagonists reduce these symptoms, so incipient hypoglycaemia is more likely to go unnoticed by the patient. The use of β-receptor antagonists is generally to be avoided in patients with poorly controlled diabetes. There is a theoretical advantage in using β1-selective agents, because glucose release from the liver is controlled by β2 receptors. Fatigue This is probably due to reduced cardiac output and reduced muscle perfusion in exercise. It is a frequent complaint of patients taking β-receptor-blocking drugs. Cold extremities This is due to a loss of β-receptor-mediated vasodilatation in cutaneous vessels, and is a common side effect. Theoretically, β1-selective drugs are less likely to produce this effect, but it is not clear that this is so in practice. Other side effects associated with β-receptor antagonists are not obviously the result of β-receptor blockade. One is the occurrence of bad dreams, which occur mainly with highly lipid-soluble drugs such as propranolol, which enter the brain easily.