* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Lecture 6
Point mutation wikipedia , lookup
Nitrogen cycle wikipedia , lookup
Basal metabolic rate wikipedia , lookup
Fatty acid synthesis wikipedia , lookup
Metalloprotein wikipedia , lookup
Genetic code wikipedia , lookup
Proteolysis wikipedia , lookup
Biosynthesis wikipedia , lookup
Phosphorylation wikipedia , lookup
Fatty acid metabolism wikipedia , lookup
Amino acid synthesis wikipedia , lookup
Citric acid cycle wikipedia , lookup
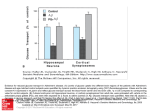
Amino acid metabolism proteins • Only foodstuff that can form structures (tissues and enzymes) • Made up of amino acids • Protein synthesis, enzyme formation • Can serve as fuel during long-term work • 0.8 g/kg recommended for adults; probably too low for athletes Protein structure: Amino acids • Essential vs non-essential – Essential: NOT made by body – Nonessential: made by the body Protein structure • Carboxyl and amino termini come together to from protein structures (peptides) Amino acid Proteins in the diet • Digested in stomach and small intestine – Hydrocholoric acid (stomach) – Trypsin, chymotrypsin, carboxypeptidase (from pancreas) – Polypeptidases and dipeptidases in intestinal cells finish digestion • The amino acid pool – Free amino acids in the liver, skeletal muscle, plasma, interstitial fluid and intracellular water – All interconnected in that metabolism in one affects the others – Continuous excretion of nitrogenous end-products – Necessitates constant input of new amino acids – So, CONSTANT Protein turnover Nitrogen balance • Nitrogen is a component of AAs – Thus, used as a marker of protein metabolism • Protein intake necessary to balance nitrogen turnover (input vs excretion) – 0.8-1.0 g/kg is sufficient for most – 1.2-1.6 g/kg is the highest recommendation for athletes Removal of nitrogen • Before amino acids can be used as fuel, nitrogen group must be removed • Two ways – Deamination – Transamination • Glutamate is a key player in both Removal of Nitrogen • Deamination – Occurs in liver 1) Requires NAD+ as oxidizing agent 2) Produces ammonium ion 3) α-ketoglutarate can be used in Kreb’s cycle • Called anaplerotic (to fill) addition to Kreb’s cycle 1 2 3 Removal of Nitrogen • Transamination – Much more common – Transfers amine group from amino acid to keto acid Keto acid AA • SGPT and SGOT transaminases in liver Keto acid AA Excretion of nitrogenous wastes 2 • Ammonia (small amt) • Most is excreted as urea • Urea cycle 1) Formation of carbamoyl phosphate from ammonia and Co2 2) Addition of aspartate 3) Production of fumarate (Kreb’s cycle intermediate) 4) Produces Urea 1 4 3 Gluconeogenic amino acids 1 • Some amino acids used for gluconeogenesis 1)Pyruvate to OOA 2)OOA to PEP 3)PEP begins “reverse glycolysis” or gluconeogenesis • So, amino acids that give rise to pyruvate and oxaloacetate – Can form phosphoenolpyruvate – Can be converted to glucose 2 Anaplerotic and cataplerotic reactions • Anaplerotic (adding to) • Cataplerotic (emptying) – These Rx add to or deplete the Kreb’s cycle • Glutamate-glutamine • Key intraorgan nitrogen transport vehicle, fuel source for GI tract and immune system and gluconeogenic precursor Branched chain amino acids • Leucine, Isoleucine and valine (LIV) • Catabolized mostly in skeletal muscle • Leucine: – Forms acetyl-CoA, acetoacetate and glutamate • Leucine is thus called ketogenic Transamination AA metabolism • AA can be used in the following ways – Structural (proteins) – Anaplerotic additions to Kreb’s cycle • This keeps the Kreb’s cycle working – Oxidized directly • Branched chain AA – Other contributions to energetics • Ketogenic – Produce ketone bodies when broken down • Glucogenic – Contributes to gluconeogenesis Glucose-alanine cycle • Used during fasting • Alanine can come from glycolysis or AA metabolism – Glycolysis • Kreb’s cycle backs up during starvation – Pyruvate transaminated to alanine – Alanine converted to glucose in liver Glucosealanine II • Other amino acids can also form alanine (glucogenic AA, anything that gives rise to pyruvate or OOA) • So when Pyruvate builds up, converted to Alanine (1) • Alanine shuttled to liver – Converted to glucose 1 Effects of endurance training on AA metab • Greater rates of AA metabolism in trained subjects – Greater oxidation in human subjects during exercise AA metabolism • Note that leucine oxidation increases during exercise – This increases is linear with respect to exercise intensity – Particularly true in fasted state AA metabolism 1 • Note that alanine appearance increases during exercise (1) and this can come from AA leucine (2) • Also, glucose infusion reduces AA oxidation (3) 2 3 AA metabolism • However, exercise training does not appear to increase AA metabolism in human subjects – If anything, it is reduced Ammonia scavenging during high intensity exercise • During high intensity exercise, AMP is formed – Adenylate kinase Rx • ADP + ADP ATP + AMP • AMP then inhibits AK Rx if it builds up • AMP deaminated to IMP • Muscle releases ammonia (NH4+) during contraction – Contains nitrogen • Purine nucleotide cycle Ammonia scavenging • Formation of glutamine (1) helps to transport ammonia in blood – Ammonia is toxic – Transamination • Glutamine goes to kidney (2) • Urea (3) and glucose formed (4) 4 2 3 1 Neuro-endocrine control of blood glucose Hormones • Chemical messengers – Produced and stored in a gland – Secreted into the blood – General and specific effects • Two basic types – Steroid • Produced from cholesterol by adrenal cortex and gonads – Polypeptides • Amino acids Hormones • Powerful effects • Precisely regulated – Feedback control (negative feedback) • Mechanisms of action – Affect cell permeability (insulin) – Activate an enzyme (epinephrine) – Protein synthesis (GH) Blood glucose homeostasis • When fed – Liver glycogenolysis • When fasted – Gluconeogenesis • SNS helps in this – Epi stimulates liver glycogenolysis and gluconeogenesis • Hormones – Released into blood – Epinephrine and nor-epinephrine Hepatic glucose production during exercise • Maintenance of blood glucose levels is paramount – Fuel source – Anaplerotic additions to Kreb’s – Allows fat metabolism – Needed by brain and CNS • Hormones that help maintain blood glucose – glucoregulatory Glucose homeostasis • How difficult is this? • Normal adult – Blood volume = 5L – Blood glucose = 100 mg/dl (1 g/L) – 5g or 20 kcals (4kcal/g) worth of energy – Only enough to support 1 min of maximal activity! • This means – We must get plenty of CHO prior to and even during activity – Liver supplements this Glucose homeostasis • Glucose production increased in 2 ways – Increased absorption from gut and liver output • Liver glycogenlosis • Liver gluconeogenesis Glucose homeostasis • Note how addition of arm exercise increases catecholamine levels – glucoregulatory hormone (raises blood glucose) • Insulin falls – Decreases blood glucose • Thus hormonal changes help maintain blood glucose levels Why increased? Catecholamines and blood glucose • Epinephrine and norepinephrine • Epi binds to β-receptor – Activates adenylate cyclase – Muscle contraction increases intracellular Ca2+ and Pi • Stimulates glycogenolysis – Muscle and liver – Supports liver glucose production – Also increases lipolytic rate Cyclic AMP • Made from ATP (1) • Intracellular messenger • Activates many processes in metabolism • Example – Glycogenolysis • Epinephrine binds to receptor (2) • Adenyl-cyclase creates cAMP (3) • cAMP activates phosphorylase EPI 1 2 3 Insulin and glucagon • Insulin – β cells of the islets of langerhans of pancreas • Glucagon – α cells • Along with epinephrine and nor-epinephrine, main hormones of glucose homeostasis Insulin response to exercise • Falls in response to exercise – Epinephrine suppresses insulin secretion • Thus – Glucose production is increased Why insulin? • Insulin – Helps facilitate glucose transport across sarcolemma during rest – Uses glucose transporters (GLUT) – GLUT-4 • Insulin mobilizes transporters from intracellular pool • Transporters move to sarcolemma Glucose transport: exercise • Muscular contraction – “insulin-like” effect – GLUT-4 can translocate due to insulin or Ca2+ • So, muscular contractions – Cause release of Ca2+ – This causes translocation of Glut4 receptors – Important as epinephrine (released during exercise) inhibits insulin insulin Neuro-endocrine control of hepatic glucose production • Gluconeogenesis – Liver and kidneys • 3 different enzymes than glycolysis – Pyruvate carboxylase – PEP carboxylase – Fructose 1,6 biphosphatase • Glucose 6phosphatase – Liver only • So, muscle resynthesizes glycogen, liver and kidneys, glucose Pyruvate kinase Gluconeogenesis • Those 4 enzymes are either nonexistent or in small supply in skeletal muscle • Found in large amts in liver and kidneys • Pyruvate kinase (last step of glycolysis): – virtually irreversible in skeletal muscle – In liver, can be inhibited by cAMP and phosphorylation (Ca2+-dependent protein kinase) – Reduces glycogenloysis and promotes gluconeogenesis Gluconeogenesis • Pyruvate coverted to oxaloacetate (A) E – High acetyl-CoA, low ADP • Oxaloacetate converted to Phosphoenolpyruvate (B) D – Low ADP • Phosphoenolpyruvate converted to Fructose 1, 6 bisphosphate (C) • F 1,6 bisphosphate converted to F6P (D) – High citrate, low AMP • Converted to glucose (E) C B A Hepatic glucose production The following hormones increase gluconeogenesis • Inhibit pyruvate kinase – Glucagon – Epinephrine – Nor-epinephrine • Insulin – Inhibits gluconeogenesis Can muscle make glucose? • Glycolytic muscle can produce glycogen from lactate – Glyconeogenesis • Likely occurs early in recovery • Muscle lacks G6 phosphatase – So can’t release glucose from cell • However, it is possible that debranching enzyme can release glucose from glycogen – May help explain very rapid inc in blood glucose (fig 9-13)