* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Inborn errors of Metabolism (IEM)
Survey
Document related concepts
Microbial metabolism wikipedia , lookup
Plant nutrition wikipedia , lookup
Point mutation wikipedia , lookup
Metalloprotein wikipedia , lookup
Nucleic acid analogue wikipedia , lookup
Peptide synthesis wikipedia , lookup
Metabolomics wikipedia , lookup
Metabolic network modelling wikipedia , lookup
Butyric acid wikipedia , lookup
Proteolysis wikipedia , lookup
Basal metabolic rate wikipedia , lookup
Pharmacometabolomics wikipedia , lookup
Genetic code wikipedia , lookup
Citric acid cycle wikipedia , lookup
Fatty acid synthesis wikipedia , lookup
Fatty acid metabolism wikipedia , lookup
Biochemistry wikipedia , lookup
Transcript
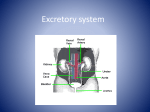
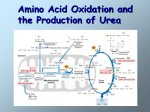
Inborn Errors of Metabolism Dr Mick Henderson Biochemical Genetics Leeds Teaching Hospitals What this seminar will cover • • • • Overview of principles in IEM Neonatal screening Approach to diagnosis Investigating suspected cases – Examples from disorders of intermediary metabolism It won’t and cant be a comprehensive review of all IEM Inborn Errors of Metabolism • Individually rare, collectively a significant health problem • Approx 1:1-2,000 live births • 25-50 in Yorkshire p.a. • Most present in childhood Enzyme Deficiencies z a b c c’ase active d cofactor c’ase inactive IEM are not just enzyme defects, can also be transport proteins, receptors or structural components Mechanisms of Disease • accumulation of a toxin • energy deficiency • deficient production of essential metabolite / structural component Investigation of IEM’s • Population Screening -Neonatal screening programme • Individual Case Investigation - based in clinical presentation Neonatal screening in the UK • Phenylketonuria • Hypothyroidism • Cystic fibrosis • MCAD deficiency • Sickle disease Leeds now involved in pilot for expanded screening, GA1, IVA, LCHADD, Hcys, MSUD www.expandedscreening.org Neonatal screening card Guthrie sample: Good sample Front Back Guthrie sample: repeat needed Front Back Leeds Neonatal Screening Pathway Approach to Diagnosis Investigations likely to be directed by presentation Acute vs Chronic Acute: may be medical emergency, hypoglycaemia, hyperammonaemia, metabolic acidosis Chronic: more difficult, need to decide how many investigations to persue Specific clinical features that immediately suggest a disorder or group e.g. • Dislocated optic lenses • Acute abdominal pain, red urine, hyponatraemia Metabolic Investigations • Most lab’s have a urine “metabolic screen” • Common initial profile: Urine; Organic acids Amino acids Sugar Chromatography Oligosaccharides Mucopolysaccharides Blood; Amino acids Acylcarnitines Further tests Mutation analysis CF mutations Enzyme assays White cells Biopsies Fibroblast studies N.B. Genetic testing is changing fast, increasing use of NGS for arrays and whole exome sequencing Examples from different IEM groups Amino acid metabolism: Urea cycle disorders phenylketonuria (PKU) maple Syrup Urine Disease (MSUD) homocystinuria arginino succinnic aciduria OTC deficiency Organic Acidaemias propionic acidaemia methyl malonic aciduria isovaleric acidaemia Fat Oxidation Defects: MCAD deficiency Carbohydrate Metabolism: glycogen storage disorders galactosaemia Lysosomal storage disorders: gaucher and Fabry diseases mucopolysaccharidoses Transport protein defects: cystic Fibrosis cystinuria cystinosis Mitochondrial disorders: Pearson syndrome cytochrome oxidase def Phenylketonuria • • • • • Affects 1: 10,000 Caucasian births Severe mental retardation untreated Excellent prognosis if treated from birth Screening test: bloodspot phenylalanine Confirm diagnosis with plasma phe measurements – no need to meas enzyme or DNA Classical PKU Phenylketones Phenylalanine Pre-block metabolite increases Tetrahydrobiopterin (reduced) X Phenylalanine Hydroxylase Dihydrobiopterin reductase Dihydrobiopterin (Oxidised) Tyrosine Post-block metabolite decreases Treatment • Low phenylalanine diet – requires careful monitoring – risk of tyrosine insufficiency – risk vitamin and trace element deficiencies • ? biopterin supplementation (sapropterin) • Large Neutral Amino Acids (val, leu, ileu) supplements • Diet for life • Management of PKU pregnancies High Phenylalanine Plasma Amino Acid Profile, PKU High phe Low tyrosine Metabolism of homocysteine tetrahydrofolate cobalamin methionine Methyl donor reactions betaine MTHF reductase 5-me tetrahydrofolate homocysteine pyridoxine cystathionine synthase cystathionine homocystine cysteine Molecular Forms COOH Homocysteine CHCH2 CH2SH NH 2 COOH COOH CHCH2 CH2SSCH2CH2 CH NH 2 NH 2 Homocystine Natural History of Clasical Homocystinuria Mudd et al Am J Hum Genet 1985; 31: 1-31 • Lens dislocation: – 82% dislocated by age 10 years • Osteoporosis (x-ray): – 64% with osteoporosis by age 15 yrs • Vascular events: – 27% had an event by age 15 years • Death: – 23% will not survive to age 30 years • Mental Retardation – approx 50% A tragic Case Female, 21 years old Pregnant Normal delivery Died 3 days post partum Saggital vein thrombosis Tests Performed Urine Positive cyanide-nitroprusside test Chromatography: homocystine Plasma total homocysteine: 152 mol/L (ref <18) No comment on haematology report as to significance Follow Up Aunt had similar event some years before Siblings: Total homocysteine (mol/L) F, 20y: F, 18y: M,16y: M, 7y: 3 268 263 4 Urea cycle & Hyperammonaemia Hyperammonaemia variable depends on: - nature of IEM - nutrition, protein intake - renal clearance of metabolites - Lyonisation (for x-linked OTC) Plasma Ammonia • Lithium heparin • Phone lab to request urgently • Transport immediately to lab Delays cause falsely high ammonia • Avoid contamination: smoking The Urea Cycle NH3 + Bicarbonate Converts highly toxic ammonia to less toxic urea Carbamyl phosphate synthetase Carbamyl Phosphate Ornithine Transcarbamylase (OTC) Citrulline Ornithine Urea Argininosuccinate Synthase Arginase Arginine Argininosuccinic acid Argininosuccinate Lyase Disorders of urea cycle Marked hyperammonaemia NH3 Side pathway utilised Carbamyl phosphate synthetase Carbamyl Phosphate Orotic acid Ornithine Transcarbamylase (OTC) OTC deficiency Urea Citrulline Ornithine Impaired urea synthesis Arginase Arginine Argininosuccinic acid Argininosuccinate Lyase Arginino succinic aciduria OTC deficiency NH3 Side pathway utilised Marked hyperammonaemia Carbamyl phosphate synthetase Carbamyl Phosphate Orotic acid Ornithine Transcarbamylase (OTC) Urea X Ornithine Citrulline Impaired urea synthesis Argininosuccinate Synthase Arginase Arginine Argininosuccinic acid Argininosuccinate Lyase OTC deficiency • OTC deficiency is x-linked • Males and female homozygotes are severely affected • Female heterozygotes are variably affected due to random x inactivation (Lyonisation) OTC presentation - infancy – 12- 72 hours of age – Lethargic and poor feeding – Abnormal respirations – vomiting – Seizure – Decreasing conscious level – If untreated die Differential diagnosis is sepsis / meningitis – Initial investigations • Gas – respiratory alkalosis • FBC • U+E, Ca2+, glucose – increase anion gap (anion gap Na – (HCO3+Cl) normally 8 to 11) • Lactate, ammonia • LFT (often abnormal) • Urine and blood cultures and ?LP (also test urine for ketones) – Initial management • commence IV antibiotics... • review management with results of investigations – Interpreting Ammonia • Abnormal • >200 µmol/l premature neonates • >100 µmol/l term neonates • >40 µmol/l in older infants Prognosis depends on duration and degree of hyperammonaemia • <500 = 94% surivival • >1000 = 34% survival Hyperammonaemia Treatment • • • • • • • Protein restriction Antibiotics Benzoate Phenylbutyrate /Phenylacetate Arginine Carbaglu Dialysis Alternative pathway treatment • Benzoate • phenylbutyrate Benzoate Therapy Benzoate + Glycine Hippurate Phenylbutyrate/acetate Therapy Phenylbutyrate Phenylbutyryl CoA Phenylacetate Glutamine Phenylacetylglutamine Urine N-Carbamoyl-L-glutamic acid • • • • • Carbaglu Marketed by Orphan N-acetylglutamate analogue Stimulates Carbamyl phosphate synthetase Particularly useful in NAGS def Arginine supplementation Arginine deficiency common in many urea cycle defects Neonates and young infants have high requirement for arginine Argininosuccinic aciduria NH3 normal, or Why can ammonia be normal ? Carbamyl phosphate synthetase Carbamyl Phosphate Ornithine Transcarbamylase (OTC) Urea Citrulline Ornithine Argininosuccinate Synthase Arginase Argininosuccinic acid Arginine X Argininosuccinate Lyase Arginino succinic aciduria NH3 Carbamyl phosphate synthetase Carbamyl Phosphate Ornithine Transcarbamylase (OTC) Ornithine Citrulline Urea Argininosuccinate Synthase Arginase Arginine Urea cycle effectively becomes a “linear pathway” provided arginine intake is adequate Argininosuccinic acid (ASA) Renal clearance of ASA is much higher than for citrulline. NH3 is excreted as ASA Small MW organic acids are intermediates in most metabolic pathways amino acids drugs, diet cholesterol neurotransmitters Organic acids purines pyrimidines carbohydrates microorganisms fatty acids Clinical indications Acute, intoxication • Unexplained metabolic acidosis • Hyperammonaemia • Hypoglycaemia • Lactic acidaemia • ketonuria Chronic • Developmental delay • Fits or seizures • Liver disease Branched chain amino acid catabolism Leucine 2-Oxoisocaproic Valine Isoleucine 2-Oxoisvaleric 2-Oxo-3-methylvaleric Isovaleryl-CoA 3-Methylcrotonyl-CoA 2-Methylbutyryl 2-Methylmalonic acid semialdehyde Triglyl-CoA 2-Methyl-3OHbutyryl-CoA 3-Methylglutaconyl-CoA 3-OH-3-MethylglutarylCoA Propionyl CoA 2-Methylmalonyl-CoA Succinyl CoA Acetyl-CoA Case history • Male baby • Hx of miscarriages Parents First cousins 3 other children • Admitted Local District Hospital @ 5days • • • • Feeding difficulty Lethargy ?sepsis ?IEM Case cont Na K Urea Creatinine Bicarb Glu Day 7: 156 3.5 24.5 123 12 22 Ammonia 1850mol/L (ref<40) Transferred to Leeds Urine organic acids: Gross inc. in isovalerylglycine and 3OHisovaleric acid Diagnosis Isovaleric acidaemia Day 9 Died in hospital Hyperammonaemia in organic acidaemias propionyl CoA methylmalonyl CoA glutamate ATP + CO2 + NH3 -ve N-acetyl glutamate + acetyl CoA +ve CPS synthetase NAG synthetase Carbamoyl phosphate UREA CYCLE Methyl Malonic Acidaemia • Episodes of metabolic acidosis triggered by intercurrent illness • Hyperammonaemia, ketoacidosis • Vomiting • Poor weight gain • Progressive loss of renal function • Hypotonia and later learning difficulties • Seizures Methyl Malonic Acidaemia: B12 Treatment • Vitamin B12 is a co-factor Test for B12 responsiveness • Pre-B12, MMA in urine… 4359 3332 5181 • Post-B12, MMA in urine… 279 982 472 (units= umol/mmol creatinine) Methyl Malonic Acidaemia: other treatments • Protein restriction • Carnitine supplements • Antibiotics • Management of CRF MCAD deficiency • A fat oxidation defect • Unable to mobilise full energy from fat during fasting • Prolonged fasting → hypoglycaemia • Impaired ketone production – Hypoketotic response to hypoglycaemia • Incidence 1 in 10,000 MCAD; the biochemical defect ketones mitochondria Acyl carnitines acetyl CoA fatty acids carnitine fatty acid oxidation dicarboxylic acids TCA cycle URINE Ketone production pathways Triglycerides Glucagon, Cortisol Growth hormone, Adrenaline Insulin Free fatty acids + Glycerol Mitochondrial -oxidation Acetyl CoA TCA cycle Ketones (3-hydroxybutyrate, acetoacetate) MCAD deficiency • Before screening 25% of diagnoses were post mortem • Crisis often follows D&V, chest infections, etc i.e. prolonged fasting when present with lethargy and decrease conscious level or seizures • Hypoglycaemia severe (→ zero) and no ketones in urine • Neonatal screening now mandated UK-wide • Untreated ongoing problems liver and brain damage, coma, and sudden death. MCAD deficiency • Treatment in crisis: ABC in A&E • Check BM for all unconsious children if low then bloods hypoglycaemia screen • IV dextrose • Recovery time relatively high • Slow recovery is partly due to accumulation of toxic metabolites • Dieticians: Emergency advice/packs Classical Galactosaemia: Initially • 1 week old, F, term delivery • Milk feeds established, poor feeder and failing to thrive • Vomiting, diarrhoea, jaundice, hepatomegaly • LFT’s: Bilirubin – 371 Conj Bili – 136 (ie around 30%) ALT – 199 Alk Phos – 2293 • Cataracts • Deranged clotting Metabolic Investigations Prolonged jaundice screen - Obstructive jaundice – remember Gal-1-PUTas well as biliary atresia Metabolic investigations • Urine Organic acids: NAD • Urine amino acids: generalised amino aciduria • Urine sugar chromatography: NAD Galactosaemia screen: Absent activity Galactosaemia Diagnosis: Pitfalls • Galactosuria: False Neg & Pos results • False Neg: If no galactose intake • Galactosaemia blood test is red cell enzyme • Invalid if child has been blood transfused Galactosaemia management • Primary source of galactose is lactose therefore: – – – – Stop breast feeding Involve a dietician Lactose free formula (or soy formula) Lactose free diet • Good prognosis but even if well treated there are long term complications – short stature – Female infertility Nephropathic Cystinosis Presents with: Fanconi syndrome: generalised aminoaciduria glycosuria phosphaturia Polyuria, Polydipsia Failure to thrive Renal failure Rickets Fair complexion Photophobia – Cysteine crystals on slit lamp examination Incidence: ~ 1 in 200,000 live births Defective lysosomal membrane transport protein for cystine, cystinosin Cystinosis: Diagnosis Clinical - Opthalmology Corneal cystine crystals on slit-lamp examination of eye Biochemical White cell cystine (definitive) CVS / amniotic fluid prenatal available Lysosomal metabolism Amino acids Specific TP’s Amino acids Hydrolysis Proteins Treatment of cystinosis with cystagon Cystine X cystinosin Cysteamine Cystine Cysteine Cysteamine Cysteamine-cysteine Lysine TP Cysteamine-cysteine