* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Immunology 3
Monoclonal antibody wikipedia , lookup
Lymphopoiesis wikipedia , lookup
Sociality and disease transmission wikipedia , lookup
DNA vaccination wikipedia , lookup
Hygiene hypothesis wikipedia , lookup
Molecular mimicry wikipedia , lookup
Adoptive cell transfer wikipedia , lookup
Immune system wikipedia , lookup
Adaptive immune system wikipedia , lookup
Immunosuppressive drug wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
Polyclonal B cell response wikipedia , lookup
Complement system wikipedia , lookup
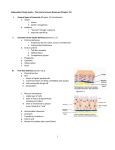
Immunology 3 – the Innate Immune system The innate immune system can be defined as a series of non-specific reactions to invading pathogens which is set off and activated quickly, immediately on the ingestion or intake of pathogen. It is an ancestral process, present in a vast number of cells, it is rarely ever found to malfunction as opposed to the adaptive immune system which regularly malfunctions. The innate immune system is composed of a number of cells but more importantly there are a vast number of diverse, extracellular molecules involved which serve to mediate and set off the innate immune response, involving the cellular components and performing a variety of functions, discussed in the course of this particular lecture. The two most important functions of the innate system are therefore, to provide a quick response to any foreign invasion by the utilization of a number of pre-formed molecules. In essence, the innate immune system bridges the time lag between the invasion of a pathogen and the activation of the adaptive, specific immune response. Additionally, the innate immune system also functions to active the specific, adaptive immune system which can then bring about a targeted and more effective response to any particular pathogen. There are a number of barriers to infection. It is important to consider these when discussing the innate immune system. The skin forms the first barrier to infection; the largest organ of the body. The dense outer layer of keratinocytes right outside the skin may well harbour a number of microorganisms but it can prevent their deeper penetration into deeper tissue. The deeper living keratinocytes form active components of the immune system and contain a number of cytokine releasing cells which secrete interleukins, which help in the co-ordination between different white blood cells. The tumour necrosis factor is also released in tandem with Ils. Skins also contains important Langerhan cells which are sentinel cells of the dendritic cell lineage. They are important following exposure to pathogens because they migrate to the local lymph nodes and play an important part in antigen presentation, which of course, is an integral component of activating the adaptive immune system. The respiratory tract requires continuous protection as well and for the purposes of this topic, it can effectively be divided into upper and lower segments. The upper segments begins at the nose and goes down to the level of the bronchioles. The main protective mechanism is what is often termed as the mucociliatory escalator. This refers to the phenomenon whereby the epithelial cells lining the respiratory tract secrete mucus, this is more specifically done by goblet cells. Mucus contains the glycoprotein mucin, and provides a sticky surface which effectively attracts and holds any incoming pathogenic matter. The cilial projections on these epithelial cells serve to constantly waft up this carpet of dust-laden mucus up the respiratory tract where it can be coughed out, sneezed out, etc. The lower respiratory tract does not contain this mixture of mucus and cilia, the respiratory passageways at this point are too small in diameter. Instead, the role of surfactants comes to the fore. Surfactants are primarily involved with lowering the surface tension in the alveoli and preventing them from collapsing under inspiration and expiration. However, surfactant also has an important role in defense because it contains certain pathogen binding proteins of the collectin family. The distinctive feature of these proteins is that they have a portion which can bind lectin, the carbohydrate portion often present on invading bacteria and a collagen –like domain which can also bind to phagocytes or complement protein, discussed shortly. In essence, they are a kind of pathogen recognition molecule playing a part in the activation of the larger innate immune response. Immunoglobulins are also present in the respiratory tract. The low pH of the stomach provides a highly hostile environment for invading pathogens and this also plays an important defensive role. There are a number of extracellular molecules of the innate immune system, mentioned briefly above. These include the cytokines, the interferons, a type of molecule involved in the inhibition of viral replication in cells and also the activation of NK cells which further secrete what is known as IF gamma. Collectins, complement and C reactive proteins are also constitutively secreted by the liver, and complements in small amounts by the monocytes and macrophages and these are also involved in the innate immune response. Interferons alpha and beta are most important in the inhibition of viral replications in cells whereas IF gamma is important in the activation of adaptive immune response. Type 1 IFNS are secreted by a number of cells in response to encountering double stranded RNA. As you may have imagined, double stranded RNA is specific to invading pathogenic material and is NOT found on host cells. Type 1 interferons hace a number of activities, they inhibit viral replication, activate NK cells, and also activate the TAP proteins, peptide transports and proteosomes, important in the processing of peptide antigenic material and the processes involved in displaying this peptide on MHC Class 1 or 2 molecules. Discussed at length later. There are large number of complement proteins with difficult names. Essentially they form a number of components which are activated through three main pathways and play important roles in the immune response. They are termed complement proteins because they complement the roles of the immunoglobulins; it has been shown through experiments that antibodies CANNOT functions without certain complement proteins. The main cellular components of the innate immune response include NK cells and Neutrophils. These are the components which are specific only to the innate immune response. However, the innate is intimately connected with the adaptive immune response and the following cellular components are common to both: Macrophages, Monocytes, Dendritic Cells and MAST cells. The cells specific to the adaptive response are the lymphoctyes, the B and the T lymphocytes. Humoural factor involved only in the innate immune response include anti-microbial peptides, known as defensins. The overlap area includes complements and cytokines, and antibodies are specific to the adaptive immune response. Briefly describe the function of the important phagocytic cells, the neutrophils, macrophages and the monocytes, dendritic cells, etc. There is a particular general mode of action of phagocytes. Essentially the idea of phagocytosis involves what is known as ‘celleating’. The specialized phagocytic cells engulfs the invading pathogen by short cytoplasmic processes known as pseudopodia or literally false feet. They engulf the pathogen, the membrane forms a small ring around it, and the membrane then pinches off from the rest of the plasma membrane resulting in the pathogen being enclosed in a vesicle inside the cytoplasm. This is now known as a phagosome. The phagosome can then fuse with a lysosome resulting in the formation of a phagolysosome, the lysosome releases its contents into the phagosome, hydrolytic enzymes, radicals, etc and digests the invading organism. The waste products are then released into the cell cytoplasm or further discarded. The useful digested molecules can be used for metabolic purposes. It is also important to discuss the exact mechanisms by which phagocytes, that is neutrophils as well as macrophages, attack these ingested particules. Proteolytic, hydrolyzing enzymes are hugely important but more important is what is known as the respiratory burst. This produces certain products of metabolism which are very harmful for the pathogens. These toxic metabolites include hydrogen peroxide, singlet oxygen, oxygen superoxide anion and hydroxyl radical. Nitrogen intermediates are also important. Defensins and lactoferrins may also be released into the phagolysosome to aid this process and note that the storage of hydrolytic enzymes in granules is what is responsible for the granulated appearane. Note that the first step in this process, the adherence of the material to the phagocytic plasma membrane is very important and this in effect regulates the whole process. Certain proteins can coat micro-organisms in a process known as opsonization and resultantly, the phagocytes can recognize these opsonins via certain receptors on their plasma membrane resulting in easy phagocytosis. Antibodies and complement proteins function as opsonins because they are recognized by phagocytes and they themselves recognize antigens. Phagocytes are also involved in inflammatory signals. Neutrophils cannot meaningfully be involved in this process due to their short life span; nevertheless they do induce localized inflammation resulting in a pyogenic reaction. Macrophages, however, are important because they also secrete inflammatory mediators known as prostaglandins and leukotrienes. Macrophages can secrete IL1, 6 and TNF aplha following the recognition of pathogen related motifs by their PAMP receptors. As a result, an acute phase response ensues, characterized by an increase in body temperature, release of acute phase proteins from the liver, etc. The increase in body temperature is thought to be detrimental to pathogen reproduction. Phagocytes deficiency can occur due to a number of bacterial and fungal infections such as Staphylococcus Aureus, E-coli, Candida Albicans, etc. This results in deep skin infection and deep wounds with impaired healing. There are two MAIN types of phagocytic cells important for discussion here. The Neutrophils, referred to as the foot soldiers of the immune system are extremely important and very numerous forming up to 60 or 70% of all leukocytes. They are first cells to be recruited to the site of infection; they have a short life span to limit possible damage to normal cells and they can be produced in higher numbers during an immune response. After phagocytosing the material, they often run out of hydrolytic enzymes and die and the pus produced at wounds is essentially a collection of such dead neutrophils. They are also termed as polymorphonuclear granulocytes because they have a particular bi-lobed nucleus with numerous granules in the cytoplasm. To fight infection, neutrophils need to stop circulating, migrate to tissues where they are likely to meet pathogens, bind to the pathogen and kill it. This is done with the help of certain soluble mediators released by macrophages and plenty of other components as a result of which not only increased neutrophil production is stimulated, but the neutrophils are attracted to tissues where the pathogens are. We find that macrophages often release chemotactic cytokines, abbreviated to chemokines which in effect, attract neutrophils. Neutrophils have certain selectin and integrin ligands on their cell surface and the receptors for these are present on endothelial cells. The chemokines change the conformation of these receptors allowing the circulating neutrophils to slow down in circulation, start rolling, bind to particular endothelial cells by means of their activated receptors, stable adhesion and then forge a path through the endothelial cells OUT of the capillaries to the sites of infection. This is known as diapedesis. Note that complement components are also chemotactic for neutrophils. Note also that the neutrophils move along a cytokine gradient to the main site of infection. Macrophages are not present in larger numbers; they can be likened to the generals of this cellular army, and they are much larger than neutrophils with kidney-shaped nuclei. They are also important in phagocytosis, of course; they typically have much longer life spans of months or years, they serve as sentinels guarding certain tissues, they can be stationery in places and often they are named according to their location in a particular tissue. Kuppfer cells in the liver, osteoclasts in the bone, glial cells in the brain. Macrophage function involves the use of a number of receptors all present on the cell membranes of the macrophages. Certain pattern-associated receptors detect particular motifs on invading pathogens as a result of which the macrophages intiate the alarm cytokines. They can also engulf invading pathogens, process and display them on their MHC Class 2 molecules for the activation of the adaptive immune response.Pattern associated receptors include NOD receptors, TOLL like receptors and RIG 1, viral genome. Cytokines are small secreted proteins which play an important part in signalling between the various components of the immune system. They act locally, have biological effects at very small concentration by binding to particular receptors on plasma membranes and neccesarily short lived for efficient down-regulation of the immune response. There are a number of kinds of cytokines, interleukins are involved in communication between leukocytes, interferons are active against viruses, certain cytokines are chemotactic, known as chemokines and certain ones are cytotoxic such as Tumour Necrosis Factor. There are a number of cytokines released by activated macrophages. Cytokine Function IL1 Alarm cytokine plus fever causer TNF alpha Alarm cytokine IL 8 Chemokine IL 6 Release of acute phase proteins IL 12 Activation of adaptive immune response Bacterial septic shock is caused by the release of bacterial endotoxins which bring about a massive release of IL1 and TNF alpha by activated macrophages. This results in a highly increased permeability of the blood vessels, a drop in blood pressure and death in 10% of cases. Note that complement components can also act as anaphylatoxins resulting in the extravasation of capillaries, causing inflammation. The benefit of such a response is to allow for the pooling of blood and the leakiness of capillaries allows for easy diapedesis. The complement proteins play a major role in both the innate and specific immune responses. They form a bunch of about 30 or so proteins and glycoproteins with a serum of concentration of 3-4 mg/ml. They form a triggered enzyme cascade system, with the components being produced by the liver, monocytes and macrophages. Can be activated by three main pathways. Classical pathway is the antigen-antibody complex bringing about the formation of the complement proteins. This happens because C1 is the initiating protein in the triggered enzyme cascade and contains an Fc receptor for immunoglobulin chains. It is only preferential to binding when there is a high concentration of Fc chains around which is only likely to happen if there is some antigen around to bind various immunoglobulin chains together. As a result, the C1 complement protein is activated, and through downstream signalling through a number of intermediary molecules in the cascade, it activates the C3 complement which is the convergence point for the three pathways. The lectin pathway involves the use of Mannan Binding Lectin and C-reactive proteins, produced during the acute phase response but also present as constitutive secretions. The MBL can bind both the antigen using its lectin section and the collagen-like domain can interact with complement components resulting in activation. C3 is once again produced. The alternative pathway occurs through a direct interaction of a particular complement component with a pathogen. However, rather counter-intuitively, the pathogen does not have any particular receptor which makes it amenable for this treatment from the complement but instead, it lacks the complement inhibitory protein present on all body cells to protect them from the complement. The cascade system brings about a large amplification of the initial response which may have only involved considerably fewer molecules. The diagram shows the three modes of complement activation in addition to the three main effector arms of the complement family. Anaphylatoxins. Produces a number of effector molecules, the smaller components due to their low molecular weight, can diffuse away from the site of complement activation and cause the effects such as the increase in vessel permeability, increase in leukocyte adhesion, chemotaxins, stimulation of phagocytosis and degranulation. B cell activation is also aided. Immune complex clearance occurs. Insoluble lattices of antigen bound to antibody can form in the tissues or in the blood, these are periodically removed by components of the complement. Formation of MAC or the Membrane Attack Complex. Can cause lysis. Opsonization Control is achieved by the lability of components, by the formation of inhibitory proteins and by the dilution of components in body fluids. Mast cells can bind to and phagocytose material, they contain histamine and other inflammatory mediators, they degranulate in the presence of the aformentioned anaphylatoxins, they can also caused increased vessel permeability, etc. Acute phase proteins are Serum amyloid A, Mannan Binding Lectin, C-reactive protein, fibrinogen and the complement. Produced from the liver. C-reactive protein activates complement along with MBL which also acts as an opsonin for monocytes. Levels increase 100 flood during an acute phase response. Acute phase response includes release of acute phase proteins from the liver, increased temperature, increased leukocyte production, etc. It is induced by certain cytokines. NK cells. LARGE GRANULATED LYMPHOCYTES: CYTOTOXIC, LYSE TARGET CELLS AND SECRETE INTERFERON- 5-10% PERIPHERAL BLOOD LYMPHOCYTES NO ANTIGEN-SPECIFIC RECEPTOR, BUT EXPRESS BOTH ACTIVATING AND INHIBITORY RECEPTORS: BALANCE OF SIGNALS HAVE RECEPTORS WHICH BIND TO ANTIBODY-COATED CELLS (ADCC) IMPORTANT IN DEFENCE AGAINST TUMOUR CELLS AND VIRAL INFECTIONS (esp. Herpes)