* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Nonspecific host defence factors.med.10 ppt
Survey
Document related concepts
Hygiene hypothesis wikipedia , lookup
Molecular mimicry wikipedia , lookup
Lymphopoiesis wikipedia , lookup
Polyclonal B cell response wikipedia , lookup
Immune system wikipedia , lookup
Complement system wikipedia , lookup
Adaptive immune system wikipedia , lookup
Adoptive cell transfer wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
Psychoneuroimmunology wikipedia , lookup
Transcript
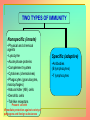
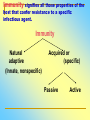
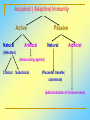
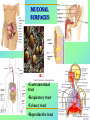
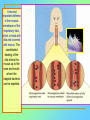
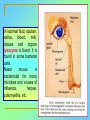
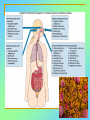
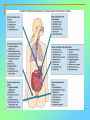
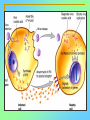
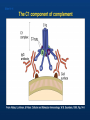
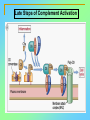
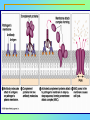
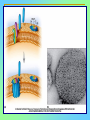
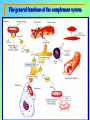
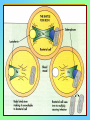
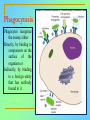
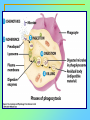
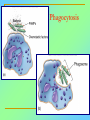
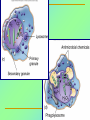
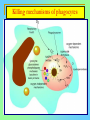
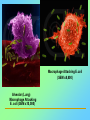
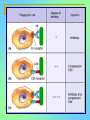
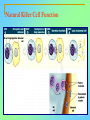
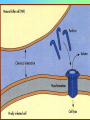
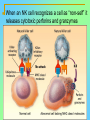
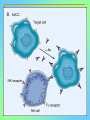
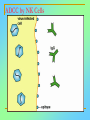
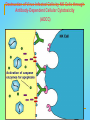
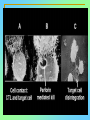
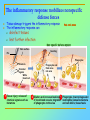
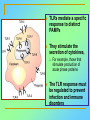
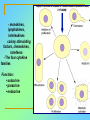
Tvorko M. S. Host defenses are composed of two complementary, frequently interacting systems: (1)innate (nonspecific) defenses, which protect against microorganisms in general, and (2) acquired (specific) immunity, which protects against a particular microorganism. TWO TYPES OF IMMUNITY Nonspecific (innate) •Physical and chemical agents •Lysozyme •Acute phase proteins •Complement system •Cytokines (chemokines) •Phagocytes (granulocytes, macrophages) •Natural killer (NK) cells •Dendritic cells •Toll-like receptors Present at birth Immediate protection against variety of pathogens and foreign substances Specific (adaptive) •Antibodies (B lymphocytes) •T lymphocytes Immunity signifies all those properties of the host that confer resistance to a specific infectious agent. Immunity Natural adaptive (Innate, nonspecific) Acquired or (specific) Passive Active Acquired ( Adaptive) Immunity Active Natural Passive Artificial Natural Artificial (Infection) (Immunizing agents) Clinical Subclinical (Placental transfer, colostrum) (administration of immune sera) First Line of Defense Epidermis Mucous membranes Mucous Cilia Lacrimal apparatus of eyes Saliva Urine flow Vaginal secretions Defecation and vomiting Sebum Perspiration Lysozyme Gastric juice Innate (nonspecific) defenses Skin and Mucous Membranes Intact skin is the first line of defense against many organisms. In addition to the physical barrier presented by skin, the fatty acids secreted by sebaceous glands in the skin have antibacterial and antifungal activity. Mucous membranes protective covering in intestine, lungs, eyes etc., that resists penetration and traps many microbes antimicrobial secretions Lysozyme Lactoferrin: macrophages and PMNs, sequesters iron Lactoperoxidase: produces superoxide radicals mucosal-associated lymphoid tissue (MALT) MUCOSAL SURFACES •Gastrointestinal tract •Respiratory tract •Urinary tract •Reproductive tract Respiratory System - The mucociliary blanket of the respiratory epithelium traps microorganisms less than 10㎛ diameter - The bronchial-Associated Lymphoid Tissue (BALT) Gastrointestinal Tract - In the stomach : lower pH, enzymes ⇒ destory - In the intestine : enzymes microorganisms - In the large intestine : the normal microbiota ⇒ preventing the establishment of pahtogens A second important defense is the mucous membrane of the respiratory tract, which is lined with cilia and covered with mucus. The coordinated beating of the cilia drives the mucus up to the nose and mouth, where the trapped bacteria can be expelled. Genitourinary Tract - Urine kills some bacteria due to its low pH and the presence of urea and other metabolic end products The Eye - Tears contain large amount of lysozyme, lactoferrin and sIgA In lacrimal fluid, sputum, saliva, blood, milk, tissues and organs lysozyme is found. It is found in some bacterial cells. Nasal mucus is bactericidal for many microbes and viruses of influenza, herpes, poliomyelitis, etc. Second Line of Defense 1. Antimicrobial proteins Interferons (IFNs) 2. Complement system 3. Antivirals that prevent replication of virus Enhance immune reactions Transferrins Inhibit bacterial growth by reducing available iron Interferons (IFNs) Interferons (IFNs) are antiviral proteins produced in response to viral infection. alpha-IFN, beta-IFN, gamma-IFN. The mode of action of -IFN and -IFN is to induce uninfected cells to produce antiviral proteins (AVPs) that prevent viral replication. Interferons are host-cell–specific but not virus-specific. Gamma-interferon activates neutrophils and macrophages to kill bacteria. Complement Complement, or the complement system, refers to a set of more than 20 large regulatory proteins produced by the liver that circulate in plasma in an inactive form. They account for about 10 percent (by weight) of all plasma proteins. The general functions of the complement system are to enhance phagocytosis, produce inflammation, and directly lyse microorganisms. These functions are nonspecific: When the complement system is activated, complement proteins participate in a cascade of reactions that trigger an inflammatory response. IgA and IgE cannot activate complement Late Steps of Complement Activation Cytolysis Caused by Membrane Attack Complex Complement-Mediated Lysis of E. coli Alive Killed The general functions of the complement system Transferrins Transferrins are iron-binding proteins. Inhibit bacterial growth by reducing the amounts of available iron. Lactoferrin is present in tears, semen, breast milk, bile, and nasopharyngeal, bronchial, cervical, and intestinal mucosal secretions. Transferrin is present in serum and the intercellular spaces of many tissues and organs. Transferrin transports iron from the small intestine, where the iron is absorbed, to the tissues, where the iron is used. Transferrin and lactoferrin bind iron, limiting the growth of pathogens in the blood. Second Line of Defense Natural killer (NK) cells Phagocytes Phagocytosis Neutrophils Macrophages Develop from monocytes Wandering Fixed ~ 5 – 10% of lymphocytes In spleen, lymph nodes and red bone marrow Attack body cells displaying abnormal plasma membrane proteins Perforin perforates cell membranes Granzymes destroy cell proteins Phagocytosis Phagocytes recognize the enemy either Directly, by binding to components on the surface of the organism or Indirectly, by binding to a foreign entity that has antibody bound to it. Figure 21.8a Phagocytosis Killing mechanisms of phagocytes SEM of macrophage engulfing E. coli cells on the surface of a blood vessel Macrophage Attacking E.coli (SEM x8,800) Alveolar (Lung) Macrophage Attacking E. coli (SEM x10,000) Natural Killer Cells Recognize and Kill Abnormal Cells NK cells are formed in the bone marrow, and migrate to: tonsils lymph nodes spleen When activated, they produce cytokines that trigger response by macrophages and other cells Then they move into blood and lymph where they kill: cancer cells virus-infected cells Natural Killer Cell Function Figure 22–11 When an NK cell recognizes a cell as “non-self” it releases cytotoxic perforins and granzymes ADCC by NK Cells Destruction of Virus-Infected Cells by NK Cells through Antibody-Dependent Cellular Cytotoxicity (ADCC) The inflammatory response mobilizes nonspecific defense forces Tissue damage triggers the inflammatory response The inflammatory response can Red, swell, warm disinfect tissues limit further infection Non-specific defense system Skin surface Swelling Pin Phagocytes Bacteria Chemical signals White blood cell 1 Tissue injury; release of chemical signals such as histamine Phagocytes and fluid move into area 2 Dilation and increased leakiness3 Phagocytes (macrophages and of local blood vessels; migration neutrophils) consume bacteria of phagocytes to the area and cell debris; tissue heals Innate Immunity Depends on ReceptorRecognition of Common Pathogen-Associated Molecules Pathogen-associated molecular patterns (PAMPs) help the innate immune system recognize pathogens Toll-like receptors (TLRs) are signaling receptors on: macrophages dendritic cells endothelial cells TLRs mediate a specific response to distinct PAMPs They stimulate the secretion of cytokines, For example, those that stimulate production of acute phase proteins The TLR response must be regulated to prevent infection and immune disorders Cytokines •“Cytokines” are soluble protein mediators secreted by immune cells (mostly) that act on other cells to regulate their activity; many are called “interleukins” (IL-1, IL-2, etc.) •Cytokines have many functions, we’ll focus on a few central functions of a few key cytokines •A subfamily of cytokines primarily functions in directing migration of cells, these are called “chemotactic cytokines” or “chemokines” - monokines, lymphokines, interleukines colony stimulating factors, chemokines, interferon - The four cytokine families Function : • autocrine • paracrine • endocrine Cytokine receptor families A summary of innate and acquired immunity INNATE IMMUNITY Rapid responses to a broad range of microbes External defenses Skin Invading microbes (pathogens) ACQUIRED IMMUNITY Slower responses to specific microbes Internal defenses Phagocytic cells Mucous membranes Antimicrobial proteins Secretions Inflammatory response Natural killer cells Humoral response (antibodies) Cell-mediated response (cytotoxic lymphocytes) Break !