* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Glomerulonephritis
Herd immunity wikipedia , lookup
Periodontal disease wikipedia , lookup
Atherosclerosis wikipedia , lookup
Adoptive cell transfer wikipedia , lookup
Molecular mimicry wikipedia , lookup
Adaptive immune system wikipedia , lookup
Vaccination wikipedia , lookup
Kawasaki disease wikipedia , lookup
Polyclonal B cell response wikipedia , lookup
Immune system wikipedia , lookup
Complement system wikipedia , lookup
Sociality and disease transmission wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
Pathophysiology of multiple sclerosis wikipedia , lookup
Behçet's disease wikipedia , lookup
Systemic scleroderma wikipedia , lookup
Innate immune system wikipedia , lookup
Ankylosing spondylitis wikipedia , lookup
Neuromyelitis optica wikipedia , lookup
Inflammatory bowel disease wikipedia , lookup
African trypanosomiasis wikipedia , lookup
Germ theory of disease wikipedia , lookup
Globalization and disease wikipedia , lookup
Rheumatoid arthritis wikipedia , lookup
Immunosuppressive drug wikipedia , lookup
Autoimmunity wikipedia , lookup
Multiple sclerosis research wikipedia , lookup
Sjögren syndrome wikipedia , lookup
Hygiene hypothesis wikipedia , lookup
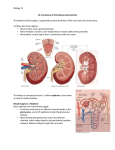
Urinary System Tutorial Glomerulonephritis The renal biopsy • Glomeruli – Glomerulonephritis • Renal tubules and Interstitium – Acute tubular necrosis – Acute interstitial nephritis – Chronic tubulointerstitial nephritis • Vasculature – Nephrosclerosis – Renal artery sclerosis Normal structure of the glomerulus Presentation of glomerular disease • Nephrotic syndrome / Proteinuria – – – – Proteinuria (> 3.5g protein / day) Hypoproteinaemia Oedema Hyperlipidaemia • Nephritic syndrome / Haematuria – Haematuria – Lesser amounts of proteinuria – Hypertension • Progressive renal failure Pathogenesis of glomerular disease • Immune mediated – Immune complex formation/deposition • Intrinsic glomerular antigens (anti-GBM) • Circulating antigens deposited in glomerulus (Membranous) • Circulating immune complexes deposited in glomerulus – – – – Activation of complement Cytokine release Neutrophil / macrophage recruitment and activation Activation of coagulation system Pathogenesis of glomerular disease • Immune mediated – Subepithelial immune complexes • less inflammation • BM alterations +/- podocyte damage • Proteinuria – Subendothelial immune complexes “inflammatory GN” • more inflammation and cellular proliferation • Vessel damage • Haematuria – BM complexes • Either presentation, usually haematuria Pathogenesis of glomerular disease • Non-immune mediated – Activation of complement • “inflammatory GN” like picture but no immune deposits – Epithelial cell injury • • • • Toxins / cytokines / unknown factors Loss of foot processes Detachment from BM Proteinuria Glomerular response to injury • Increased cells (Hypercellularity) – – – – Seen in “inflammatory diseases” Proliferation of mesangial and endothelial cells Inflammatory cells Proliferation of epithelial cells +/- crescent formation • Increased matrix / connective tissue (Hyalinization / Fibrosis) – Hyalinization = accumulation of pink homogenous material – Plasma protein/BM/Mesangial matrix – Eventually leads to Fibrosis • Increased basement membrane – Thickened capillary loops – Increased BM / immune deposits Investigation of glomerular disease • Histopathology / Light microscopy – Glomeruli • Hypercellularity • Increased matrix / Hyalinization / Fibrosis) • Thickened basement membrane – Secondary changes in tubules/interstitium • Amount of tubular atrophy and fibrosis is a sensitive indicator of prognosis – Associated large vessel disease Investigation of glomerular disease • Immunofluorescence – Formation of immune complexes with deposition of antibodies in glomerulus – IgG, IgA, IgM – Basement membrane, mesangium – Linear or granular pattern • Electron microscopy – Changes in podocytes, basement membranes and mesangium – Location and presence of immune deposits (subepithelial, subendothelial, basement membrane) Classification of glomerular disease • How many glomeruli? – Focal = only some glomeruli – Diffuse = all glomeruli affected • How much of a single glomerulus? – Segmental = only part of the glomerulus – Global = the entire glomerulus • Primary vs Secondary – primarily renal disease vs renal complication of systemic disease Glomerular diseases associated with nephrotic syndrome • Primary – Minimal change disease – Membranous GN – Focal segmental glomerulosclerosis (FSGS) • Secondary – Diabetic nephropathy – Amyloidosis Glomerular diseases associated with nephritic syndrome • Primary – – – – Postinfectious / Diffuse proliferative GN Membranoproliferative GN IgA nephropathy (Mesangioproliferative GN) Crescentic GN • Secondary – – – – HSP Systemic vasculitis SLE Systemic sclerosis Causes of the nephrotic syndrome (Minimal change disease) Minimal change disease • Commonest cause of nephrotic syndrome in children • Can occur in adults • Characterised by – Lack of glomerular changes on light microscopy – Lack of immune deposits – Good response to steroids • Pathogenesis – Circulating factor causing damage to podocytes (glomerular epithelial cells) Minimal change disease • Light microscopy (LM) – Normal • Immunofluorescence (IF) – Normal (no immune deposits) • Electron microscopy (EM) – Fusion of podocyte foot processes Membranous GN • Commonest cause of nephrotic syndrome in adults • Idiopathic (85%) or secondary (15%) to: – – – – Neoplasms (lung, colon, melanoma) Autoimmune disease (SLE, thyroiditis) Infections (Hep B, syphilis, malaria) Drugs (Penicillamine, gold) • 40% progress to chronic renal failure (CRF) • Pathogenesis – Subepithelial immune deposits – Thickening of BM between deposits – eventually envelopes and covers the deposits Membranous GN • Light microscopy (LM) – Thickened capillary BM – BM spikes on silver stain • Immunofluorescence (IF) – diffuse granular GBM staining • Electron microscopy (EM) – subepithelial deposits FSGS • Idiopathic or secondary to: – Other glomerular disease (IgA) – Other renal disease (chronic reflux / pyelonephritis / interstitial nephritis) – Systemic disorder (HIV) – Drugs (Heroin) • Characterised by: – Sclerosis of portions of some, not all glomeruli – Often progresses to chronic renal failure (CRF) – Recurs in 25-50% renal transplants FSGS • Light microscopy (LM) – Focal segmental sclerosis – Some normal glomeruli • Immunofluorescence (IF) – IgM and C3 deposition in sclerotic areas • Electron microscopy (EM) – Fusion of podocyte foot processes Postinfectious / Diffuse proliferative GN • Characterised by – Onset 1 – 4 weeks after upper respiratory / cutaneous infection with Group A -haemolytic streptococci – Can occur after a number of other bacterial, viral and parasitic infections – Elevated antistreptococcal antibody and decreased C3 – Secondary to anti-strep antibodies binding to glomerular components – Usually resolves within 6 weeks Postinfectious / Diffuse proliferative GN • Light microscopy (LM) – Diffuse glomerular proliferation • Immunofluorescence (IF) – Granular BM IgG, IgM, C3 • Electron microscopy (EM) – Subepithelial deposits Membranoproliferative GN • Type I: – Immune complex disease – Idiopathic or secondary to Neoplasm, Autoimmune disease, Infections, Drugs – Subendothelial immune complexes • Type II: – Complement activation – BM deposits (dense deposit disease) • 50% progress to chronic renal failure (CRF) • High recurrence rate in renal transplants • Characterised by – Thickened capillary loops – Glomerular hypercellularity due to mesangial proliferation – Mesangial interposition – double GBM’s (Type I) Membranoproliferative GN • Light microscopy (LM) – Mesangial proliferation – Thickened capillary BM – Double BM’s on silver stain (Type I) • Immunofluorescence (IF) – Type I: Granular BM and mesangial IgG, IgM, C3 – Type II: Granular BM C3 • Electron microscopy (EM) – Type I: Subendothelial deposits and mesangial interposition – Type II: Dense deposits in GBM IgA Nephropathy Mesangioproliferative GN • Pathogenesis – Increased mucosal IgA secretion in response to inhaled/ingested antigens – Glomerular (mesangial) deposition of IgA • Characterised by episodic haematuria following respiratory tract infections • 50% progress to chronic renal failure (CRF) • Recurs in 20-60% of transplants • Varying histology Mesangioproliferative GN • Light microscopy (LM) – Increased mesangial matrix – Mesangial proliferation – Focal sclerosis (FSGS) • Immunofluorescence (IF) – mesangial IgA • Electron microscopy (EM) – mesangial deposits Crescentic GN Rapidly progressive GN • Characterised by – Glomerular crescents • Accumulation of cells in Bowman’s space • Inflammatory cells, fibrin and epithelial cell proliferation • Compression of glomerulus – Rapidly progressive clinical course • Pathogenesis – Damage to glomerular vessels – Egress of inflammatory cells and fibrin into Bowman’s space – Proliferation of epithelial cells Crescentic GN Rapidly progressive GN • Pathogenesis – Type I – anti-GBM antibodies • linear deposition of IgG • May bind to alveolar BM in lung = Goodpasture’s disease – Type II – immune complexes • Idiopathic or secondary to autoimmune disease or other GN – – – – SLE HSP IgA nephropathy Postinfectious GN – Type III – pauci-immune • Idiopathic or secondary to systemic vasculitis – Wegeners – PAN Crescentic GN • Light microscopy (LM) – Cellular crescents of epithelium and inflammatory cells – Fibrotic crescents • Immunofluorescence (IF) – Type I: linear IgG – Type II: granular IgG – Type III: no deposits • Electron microscopy (EM) – Type II: subendo, mesangial and subepi deposits