* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download lymphatic system
Monoclonal antibody wikipedia , lookup
Immune system wikipedia , lookup
Psychoneuroimmunology wikipedia , lookup
Molecular mimicry wikipedia , lookup
Lymphopoiesis wikipedia , lookup
Polyclonal B cell response wikipedia , lookup
Adaptive immune system wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
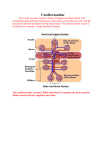
Chapter 22 The Lymphatic System Lecture Outline INTRODUCTION • The ability to ward off the pathogens that produce disease is called resistance. • Lack of resistance is called susceptibility. • Resistance to disease can be grouped into two broad areas. • Nonspecific resistance to disease includes defense mechanisms that provide general protection against invasion by a wide range of pathogens. • Immunity involves activation of specific Chapter 22 The Lymphatic System • Resistance is the ability to ward off disease – lack of resistance is termed susceptibility • Nonspecific resistance to disease – general defensive mechanisms effective on a wide range of pathogens (disease producing microbes) • Specific resistance or immunity is ability to fight a specific pathogen – cell-mediated immunity LYMPHATIC SYSTEM STRUCTURE AND FUNCTION • The lymphatic system consists of a fluid called lymph flowing within lymphatic vessels, several structures and organs that contain lymphatic tissue (specialized reticular tissue containing large numbers of lymphocytes), and bone marrow, which is the site of lymphocyte production (Figure 22.1). • Interstitial fluid and lymph are very similar. • Their major difference is location. Functions of the Lymphatic System • Draining excess interstitial fluid & plasma proteins from tissue spaces • Transporting dietary lipids & vitamins from GI tract to the blood • Facilitating immune responses – recognize microbes or abnormal cells & responding by killing them directly or secreting antibodies that cause their destruction Formation and Flow of Lymph • Interstitial fluid drains into lymph capillaries. • The passage of lymph is from arteries and blood capillaries (blood) to interstitial spaces (interstitial fluid) to lymph capillaries (lymph) to lymphatic vessels to lymph trunks to the thoracic duct or right lymphatic duct to the subclavian veins (blood) (Figure 22.4). • Lymph flows as a result of the milking Lymphatic Organs & Tissues • Widely distributed throughout the body • Primary lymphatic organs – provide environment for stem cells to divide & mature into B and T lymphocytes • red bone marrow gives rise to mature B cells • thymus is site where pre-T cells from red marrow mature • Secondary lymphatic organs & tissues – site where most immune responses occur • lymph nodes, spleen & lymphatic nodules • Large organ in infants (70 g) but atrophied as adult (3 g) • 2 lobed organ located in mediastinum • Capsule & trabeculae divide it into lobules • Each lobule has cortex & medulla • Cortex – tightly packed Thymus Gland Figure 22.5 Lymph Nodes - Overview • Lymph nodes are encapsulated oval structures located along lymphatic vessels (Figures 22.1a and 22.6). • They contain T cells, macrophages, follicular dendritic cells, and B cells. • Lymph enters nodes through afferent lymphatic vessels, is filtered to remove damaged cells and microorganisms, and exits through efferent lymphatic vessels. • Foreign substances filtered by the lymph nodes are trapped by nodal reticular fibers. • Macrophages then destroy some foreign substances by phagocytosis and lymphocytes bring Spleen Figure 22.7 • 5 inch organ between stomach & diaphragm • Hilus contains blood & lymphatic vessels • Stroma consists of capsule, trabeculae, fibers & fibroblasts • Parenchyma consists of white pulp and red pulp – white is lymphatic tissue (lymphocytes & macrophages) around branches of splenic artery – red pulp is venous sinuses filled with blood & splenic tissue • First Line of Defense: Skin and Nonspecific resistanceMembranes refers to a wide variety of Mucous body responses against a wide range of pathogens (disease producing organisms) and their toxins. • Mechanical protection includes the intact epidermis layer of the skin (Figure 5.1), mucous membranes, the lacrimal apparatus, saliva, mucus, cilia, the epiglottis, and the flow of urine. Defecation and vomiting also may be considered mechanical processes that expel microbes. • Chemical protection is localized on the skin, in loose connective tissue, stomach, and vagina. • The skin produces sebum, which has a low pH due to the presence of unsaturated fatty acids and lactic Second Line of Defense: Internal Defenses • The second line of defense involves internal antimicrobial proteins, phagocytic and natural killer cells, inflammation, and fever. Antimicrobial Proteins • Body cells infected with viruses produce proteins called interferons (IFNs). – Once produced and released from virusinfected cells, IFN diffuses to uninfected neighboring cells and binds to surface receptors, inducing uninfected cells to synthesize antiviral proteins that interfere with or inhibit viral replication. – INFs also enhance the activity of phagocytes and natural killer (NK) cells, inhibit cell growth, and suppress tumor formation; they may hold Antimicrobial Proteins • A group of about 20 proteins present in blood plasma and on cell membranes comprises the complement system – when activated, these proteins “complement” or enhance certain immune, allergic, and inflammatory reactions. Natural Killer Cells & Phagocytes • NK cells kill a variety of microbes & tumor cells – found in blood, spleen, lymph nodes & red marrow – attack cells displaying abnormal MHC antigens • Phagocytes (neutrophils & macrophages) – ingest microbes or particulate matter – macrophages developed from monocytes • fixed macrophages stand guard in specific tissues – histiocytes in the skin, kupffer cells in the liver, alveolar macrophages in the lungs, microglia in the brain & Phagocytosis • Phagocytes are cells specialized to perform phagocytosis and include neutrophils and macrophages. – The four phases of phagocytosis include chemotaxis, adherence, ingestion, digestion and killing. (Figure 22.9). – After phagocytosis has been accomplished, a phagolysosome (Figure 22.9) is formed. – The lysosome in the phagolysosome, along with lethal oxidants produced by the phagocyte, quickly kills many types of Stages of Inflammation • The three basic stages of inflammation are vasodilation and increased permeability of blood vessels, phagocyte migration, and tissue repair (Figure 22.10). • Vasodilation & increased permeability of vessels – caused by histamine from mast cells, kinins from precursors in the blood, prostaglandins from damaged cells, and leukotrienes from basophils & mast cells – occurs within minutes producing heat, redness & edema – pain can result from injury, pressure from edema or irritation by toxic chemicals from organisms – blood-clotting factors leak into tissues trapping microbes • Phagocyte emigration – within an hour, neutrophils and then monocytes arrive and leave blood stream (emigration) SPECIFIC RESISTANCE: IMMUNITY • Immunity is the ability of the body to defend itself against specific invading agents. – bacteria, toxins, viruses, cat dander, etc. • Differs from nonspecific defense mechanisms – specificity----recognize self & non-self – memory----2nd encounter produces even more vigorous response • Antigens are substances recognized as Maturation of T Cells and B Cells • Both T cells and B cells derive from stem cells in bone marrow (Figure 22.11). • B cells complete their development in bone marrow (Figure 22.11). • T cells develop from pre-T cells that migrate to the thymus. • Before T cells leave the thymus or B cells leave bone marrow, they acquire several distinctive surface proteins; some function as antigen receptors, molecules capable Types of Immune Response • Cell-mediated immunity (CMI) refers to destruction of antigens by T cells. – particularly effective against intracellular pathogens, such as fungi, parasites, and viruses; some cancer cells; and foreign tissue transplants. – CMI always involves cells attacking cells. • Antibody-mediated (humoral) immunity (AMI) refers to destruction of antigens by antibodies. Antigens • Molecules or bits of foreign material – entire microbes, parts of microbes, bacterial toxins, pollen, transplanted organs, incompatible blood cells • Required characteristics to be considered an antigen – immunogenicity = ability to provoke immune response – reactivity = ability to react to cells or antibodies it caused to be formed • Get past the bodies nonspecific defenses – enter the bloodstream to be deposited in spleen – penetrate the skin & end up in lymph nodes – penetrate mucous membrane & lodge in associated CELL-MEDIATED IMMUNITY • Begins with activation of T cell by a specific antigen • Result is T cell capable of an immune attack – elimination of the intruder by a direct attack • In a cell-mediated immune response, an antigen is recognized (bound), a small number of specific T cells proliferate and differentiate into a clone of effector cells (a Overview of Mature T Cells 1. Helper T (TH) cells, or T4 cells, display CD4 protein, recognize antigen fragments associated with MHC-II molecules, and secrete several cytokines, most important, interleukin-2, which acts as a costimulator for other helper T cells, cytotoxic T cells, and B cells (Figure 22.14). 2. Cytotoxic T (TC) cells, or T8 cells, develop from T cells that display CD8 protein and Antibody-Mediated Immunity • The body contains not only millions of different T cells but also millions of different B cells, each capable of responding to a specific antigen. • B cells sit still and let antigens be brought to them – stay put in lymph nodes, spleen or peyer’s patches • Once activated, differentiate into plasma cells that secrete antibodies