* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Lymphatic System Notes
Sociality and disease transmission wikipedia , lookup
Complement system wikipedia , lookup
DNA vaccination wikipedia , lookup
Lymphopoiesis wikipedia , lookup
Sjögren syndrome wikipedia , lookup
Monoclonal antibody wikipedia , lookup
Immune system wikipedia , lookup
Adoptive cell transfer wikipedia , lookup
Hygiene hypothesis wikipedia , lookup
Adaptive immune system wikipedia , lookup
Molecular mimicry wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
Immunosuppressive drug wikipedia , lookup
Psychoneuroimmunology wikipedia , lookup
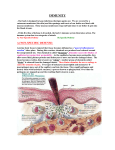
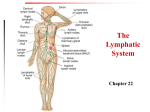
The Lymphatic System http://www.faqs.org/health/Bodyby-Design-V1/The-LymphaticSystem.html The Lymphatic System • The body is constantly in contact with bacteria, fungi, and viruses (all considered pathogens) • The body has two defense systems for foreign materials Types of Defense • Non-Specific Defense – First & Second Line of Defense – Doesn’t care what the pathogen is – your body will be defended! Non-Specific Defense • Non-Specific Defense Mechanisms Include… – Skin: mechanical barrier, acidic skin secretions can also defend – Mucous Membranes: Mucus and nasal hairs trap microorganisms; Cilia move mucus out of body; Gastric juice, saliva, and tears have enzymes that destroy microorganisms – Skin and Mucous Membranes are the first line of defense against pathogens – Cellular & Chemical Defense: Second line of defense; includes… Non-Specific Defense • Phagocytes: • Cell that engulfs a foreign particle, enclosing it in a vacuole; destroyed with enzymatic contents of lysosomes Non-Specific Defense • Examples of phagocytes include macrophages (in body tissues, developed from monocyte WBC), and neutrophils (WBC) Macrophage engulfing E-Coli Non-Specific Defense • Natural Killer Cells: • Defensive cells that can kill cancer cells and virus-infected body cells • Release chemicals to destroy invader’s cell membrane and nucleus Non-Specific Defense • Inflammatory Response: • Non-specific response triggered whenever body tissues are injured Non-Specific Defense • Benefits of inflammatory response include: – Preventing the spread of damaging agents to nearby tissues – Disposes of cell debris and pathogens – Sets the stage for repair Non-Specific Defense • 4 Signs of Inflammatory Response: • Redness – due to dilation of blood vessels in area, bringing more clotting proteins/ oxygen/nutrients to the area • Heat – due to dilation of blood vessels in area, helps increase metabolic rate of cells • Swelling – due to plasma (lymph) leaking from blood stream into tissue spaces • Pain – pain receptors activated by plasma leaking Non-Specific Defense • All of the above symptoms are due to the inflammatory chemicals (including histamine and kinins) that are released when cells are damaged Non-Specific Defense • Fever: response to invading pathogens • Hypothalamus will reset internal temperature based on presence of pyrogens (chemicals secreted by WBC exposed to foreign substances) • Fever inhibits the release of iron and zinc from liver and spleen needed by bacteria • Fever also increases the speed of tissue repair, but if fever gets too high, it can screw up enzymes and proteins Specific Defense • Specific Defense – Third line of defense – AKA immune system – Plans defense based on specific type of pathogen/antigen (The antigen is a marker on the pathogen!) – Must first have an initial exposure before it can protect the body against the pathogen – Involves the Lymph Vessels/Nodes and Lymphoid Organs (Tonsils, Thymus, Spleen, and Peyer’s Patches) Specific Defense • 2 Types of Response: Humoral and CellMediated Specific Defense • 3 important aspects of immune response: • Antigen specific – recognizes and acts against particular foreign substances • Systemic – not restricted to the initial infection site • Has memory – recognizes and mounts a stronger attack on previously encountered pathogens Specific Defense • Antigens: any substance capable of exciting our immune system and provoking an immune response • A foreign signal on the outside of a pathogen! • Examples of common pathogens/antigens – Foreign proteins (ex: blood typing) – Pollen grains – Microorganisms (bacteria, fungi, virus) • Side Note: Our immune cells do not attack our own proteins, but our cells in another person’s body can trigger an immune response because they are foreign (think: organ transplants, blood donation) Immune System Review – Types of cells involved • Lymphocytes (WBC): two types… –B Cells: help with humoral defense, produce antibodies –T Cells: help with cell-mediated defense, do not produce antibodies Specific Defense • Both types of lymphocytes originate from red bone marrow • What determines if it will be a B or T cell is where in the body it becomes immunocompetent (capable of responding to a specific antigen) – T Cells: lymphocytes migrating to thymus – B Cells: lymphocytes develop in bone marrow Specific Defense • Our genes determine what specific foreign substances our immune system will be able to recognize and resist – they only become “activated” once exposed to the antigen • FYI: Because of the structure of human DNA (deoxyribonucleic acid; the genetic material determining the makeup of all cells), humans are not subject to certain diseases that dogs and other animals are, and vice-versa. For example, humans cannot contract distemper; however, dogs and cats can. Conversely, humans can suffer from measles; dogs and cats cannot. The genetic makeup of human cells (and of animal and plant cells, also) makes it impossible for certain pathogens to infect and reproduce in those cells. Specific Defense • After becoming immunocompetent, both T and B cells migrate to the lymph nodes and spleen, but can be found throughout lymphatic vessels Specific Defenses • Macrophages: • Arise from monocytes (WBC) formed in the bone marrow • Job is to engulf foreign particles (part of non-specific defense) and present fragments of these antigens on their surface (so T Cells can recognize them and become activated, helping out specific defense!) Humoral Defense • Making the Antibodies – B Cells with specific receptors bind to a specific antigen – …which causes the B Cell to undergo “clonal selection” – a whole bunch of clones are made! Humoral Defense – Most of the clones will become “plasma cells”, which are responsible for producing specific antibodies! – A few of the clones will become “memory cells”, which will be ready to bind with the antigen if it should come around again Humoral Defense • Antibodies – Soluble proteins secreted by B cells (plasma cells) – Carried in blood plasma – Usually has a T or Y shape formed by amino acid chains – Capable of binding specifically to an antigen Humoral Defense • When antibodies attach to antigens, it can have different effects… Humoral Defense – Complement Fixation: antibody will join with a “complement protein” on the invader; which will allow holes on the invader surface; will result in cell lysis (bursting of cell) Humoral Defense – Neutralization: surrounds antigen to mask its effects Humoral Defense – Agglutination: clumping of antigens; will allow macrophages to easily catch and engulf invaders Cell Mediated Defense • Begins with macrophages destroying an antigen • Macrophage will then put fragments of the destroyed antigen on the outside • T Cells will recognize the antigen being presented by the macrophage and bind with the antigen (Antigen Presentation) • After binding, T Cell clones form, but different classes of cells are produced Cell Mediated Defense • Cytotoxic T Cell: “killer” cells, specialize in killing virus-infected, cancer, and foreign cells, often by inserting toxic chemicals, causing the pathogen cell to “blow up” Note: basically does the same thing as a Natural Killer Cell, but does it to a specific pathogen! http://highered.mcgrawhill.com/sites/0072495855/student_view0/chapter24/animation__cytotoxic_tcell_activity_against_target_cells__quiz_2_.html Cell Mediated Defense • Helper T Cell: “regulator/conductor” cells, encourages cloning of B cells, stimulates Cytotoxic T Cells to grow and divide, enhances eating capabilities of macrophages Cell Mediated Defense • Supressor T Cell: helps to stop immune response once an antigen has been inactivated or destroyed • http://highered.mcgrawhill.com/sites/0072495855/student_view0/ chapter24/animation__the_immune_respo nse.html Viruses • Not considered “living” because has no cytoplasm or organelles • Needs a living host cell to survive • Will take over host cell to replicate • Virus infections cannot be treated with antibiotics • Some can be prevented with vaccines Viruses • Common Cold • Varicella - Chicken Pox – rarely fatal • Variola – Smallpox – often fatal – but now eliminated thanks to vaccinations! • Influenza – MANY different strains! • Human Papillomavirus – HPV – can lead to warts, cervical cancer, and some other genital cancers • Rotavirus – leading cause of diarrhea among infants and young children Smallpox Chicken Pox Viruses • Mumps – swelling of salivary glands, and testicular swelling • Measles – can lead to diarrhea, pneumonia, encephalitis, and eye infections • Rubella – rash • Poliomyelitis – in less than 1% of polio cases, virus enters the CNS, destroying motor neurons, leading to muscle weakness and paralysis; highly contagious • Rabies – causes encephalitis; extremely fatal • HIV Measles Mumps Rubella MMR Vaccination protects against all three! Vaccination • Administration of antigenic material to produce immunity to a disease • Can be live but weakened, dead, or inactivated form of pathogen (virus or bacteria) • Pathogens are grown in culture and killed/weakened, but surface proteins are intact enough to be recognized • When injected, immune system will evoke a response Bacteria • Are considered a “living” prokaryotic cell • Does not need a living host cell to survive • Most (99%) are good, but a few are harmful – Good ones help us with digestion, releasing vitamins, eliminating body toxins, preventing fungal growth Bacteria • Harmful bacterial infections can be treated with antibiotics • Some can live harmlessly, but develop into an infection if immune system has had its resistance lowered (ex: AIDS) • A few infections can be prevented with vaccines Bad Bacteria • Tuberculosis – affects lungs • Streptococcus – affects throat (pharynx, larynx, tonsils) • Botulism – weakens muscles, prevents breathing • Bubonic Plague – spread by fleas that live on rats; damages lymph notes • Cholera – affects small intestine, causes diarrhea, vomiting, and rapid dehydration Bad Bacteria • Salmonella – can cause digestive issues • Escherichia Coli – aka E.Coli – some strains are good, but the bad strains can cause lower digestive issues or UTIs • Syphilis – STD that causes lesions; if left untreated, it can cause issues with the heart and brain • Impetigo – skin infection Bad Bacteria • Diphtheria – causes upper respiratory issues • Pertussis – whooping cough • Tetanus – causes muscle spasms • These last three can be quite harmful (even deadly) that we are given the DPT vaccination Antibiotics • A substance or compound that kills or inhibits growth of bacteria • Can either be made synthetically from chemicals or produced by fermenting different fungus molds • Unfortunately, bacteria can mutate to become resistant to antibiotics • EX: penicillin, amoxicillin, tetracycline, sulfa drugs, cefzil Fungus • Are considered a “living” eukaryotic cell • Includes molds and yeasts • Some are good, such as fungi used to make antibiotics (penicillin) or baker’s yeast • Infections can spread very easily! Bad Fungi • • • • Candida – Yeast Infection Tinea Pedis – Athlete’s Foot Tinea Cruris – Jock Itch Tinea Unguium – Nail Fungus Immune System Diseases • Allergies – Abnormally vigorous immune responses – Different types… Immune System Diseases Allergies – Acute hypersensitivity • Pathogen & resulting antibodies cause release of histamine… • Which causes small blood vessels to become dilated and leaky • Symptoms include runny nose, watery eyes, itching, reddened skin (hives), bronchial constriction (asthma) • Antihistamine drugs can reverse effects Immune System Diseases Allergies – Anaphylactic Shock • Allergen directly enters the blood and circulates rapidly throughout the body • Examples: Bee stings, spider bites, drug injections • Dilated & leaky blood vessels throughout body can be life-threatening • The drug Epinephrine can reverse effects Immune System Diseases • Immunodeficiencies – Production or function of immune cells is abnormal – May be congenital or acquired – Examples include… Immune System Diseases Immunodeficiencies • Severe Combined Immunodeficiency Syndrome (SCIDS) – Deficit of both B and T cells – Have no immune response – “Bubble Boy” Disease – Some success with bone marrow transplants For twelve years David Vetter, born with combined immune deficiency, lived inside this plastic bubble at Texas Children's Hospital in Houston, Texas, waiting for a cure to the disease that kept him prisoner. Immune System Diseases Immunodeficiencies • Acquired Immune Deficiency Syndrome (AIDS) – The virus (Human Immunodeficiency Virus, or HIV) destroys Helper T Cells & Macrophages – Cell-mediated immunity is reduced – Virus then begins to multiply in lymph nodes – which takes longer in some than in others Immune System Diseases Immunodeficiencies – A patient is diagnosed with AIDS when the lymph nodes are destroyed & symptoms begin – Symptoms include severe weight loss, night sweats, swollen lymph nodes, and increasingly frequent infections (gastrointestinal, pneumonia) – Some of the drugs that are used to help act by inhibiting the enzymes the HIV virus needs in order to multiply, or helps to boost number of Helper T Cells – THERE IS NO CURE OR VACCINE. Immune System Diseases Immunodeficiencies • Facts: – 33.2 million worldwide have AIDS; 2.5 million are children under age 15 – 1.9 million died of AIDS in 2010; 330,000 were children under age 15 – Sub-Sahara Africa contains 68% of the AIDS population – The median survival time after infection with HIV is estimated to be 9 to 11 years, depending on the HIV subtype Immune System Diseases • Autoimmune Diseases – The immune system does not distinguish between self and non-self – The body produces antibodies and T Cells that attack its own tissues – Examples Include… Immune System Diseases Autoimmune Diseases – Multiple sclerosis: myelin sheaths in the white matter of brain & spinal cord are destroyed – Type 1 diabetes: destroys pancreatic beta cells that produce insulin – Rheumatoid arthritis: destroys joints – Lupus: affects kidney, heart, lung and skin