* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Cytokines
Complement system wikipedia , lookup
Hygiene hypothesis wikipedia , lookup
DNA vaccination wikipedia , lookup
Lymphopoiesis wikipedia , lookup
Immune system wikipedia , lookup
Molecular mimicry wikipedia , lookup
Monoclonal antibody wikipedia , lookup
Adaptive immune system wikipedia , lookup
Adoptive cell transfer wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
Innate immune system wikipedia , lookup
Psychoneuroimmunology wikipedia , lookup
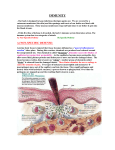
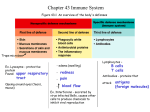
Physiological mechanisms of regulation of the immune system Regulation by antigen Induce immune responses and extinction Affinity maturation of B lymphocytes Maintaining immunological memory Antigenic competition Threshold density of the complex MHC II-gp Ag on APC Regulation by antibodies Antibodies competes with the BCR for antigen (negative regulator of B lymphocyte stimulating) IgG immune complexes bind to the BCR and FcgR on B cells, resulting in blocking activation of B lymphocytes Regulation via idiotypic network Regulation by cytokines and cellular contact Interaction APC - T lymphocyte Interaction TH1 – macrophages Interaction TH2 - B lymphocytes Mutual regulation of activity TH1 versus TH2 Development of leukocyte subpopulations Regulation by cytokines and cellular contact Interaction between APC and T cell T cell: TCR - antigen-specific receptor CD4 or CD8 - coreceptor (MHCgp binding) CD 28 - costimulatory receptor (binds CD 80, CD 86) CTLA-4 - inhibitory receptor (binds CD 80, CD 86) Regulation by cytokines and cellular contact Interaction between TH1 and TH2 cells Negative regulation of effector cells CTLA-4 - T cell inhibitory receptor, binds ligands CD80 and CD86 Self-destruction interaction of the apoptotic receptor Fas with ligand FasL on the surface of activated T lymphocytes Inhibitory receptors of NK cells Suppression mediated by T lymphocytes Mutual negative interaction TH1 and TH2 cytokine-mediated Clonal elimination or anergy of T lymphocytes after contact with antigen on the surface of other cells than APC Regulatory T cells (Treg, Tr1, Th3 - CD 4+) help to maintain tolerance to autoantigens; produce TGFb, IL-10 Factors influencing the outcome of the immune response The same antigen can induce an active immune response or an active state of tolerance, the result of response depends on many factors: State of the immune system Properties of antigen Dose of antigen Route of antigen administration Cytokines (Tissue hormones) Cytokines Regulatory proteins and glycoproteins produced by leukocytes and other cells Essential regulators of the immune system Apply also outside the immune system (angiogenesis, tissue regeneration, carcinogenesis, treatment of many brain functions, embryonic development ...) Cytokines - secreted - membrane (CD 80, CD86, CD40L, FasL ..) Cytokines Pleiotropic effect Operates in a cascade Cytokine network Cytokine system is redundant Effects of cytokines- autocrine - paracrine - endocrine Are known as interleukins (IL-1…IL-38) (except: TNF, lymphotoxin, TGF, interferons, CSF and growth factors) B cells communicate via cytokines with other cells, such as T cells and macrophages Overview of the most important cytokines Cytokine Produced Function IL-1 MF, N T cell costimulation, induction of TNF and IL-8, pyrogen IL-2 Th1 Growth factor for T cells IL-4 Th2, basophils Th2 differentiation, B cell stimulation, isotype switching to IgE and IgG4, Th1 inhibition IL-5 Th2, eosinophils B cell stimulation, growth factor for eosinophils IL-6 Th2, MF, N T and B cell stimulation, stimulation of Ig production, induction of acute phase proteins synthesis, pyrogen IL-8 MF, other cells Granulocyte activation and chemotaxis (primarily neutrophils) IL-10 Th2,M, Treg Th1 and MF inhibition, B cell differentiation to plasma cell IL-12 MF, DC, B Th1 differentiation, NK stimulation TNF M, MF, NK Induction of local inflammation, endothelium activation, induction of apoptosis TGFb T, MF, platelets The anti-inflammatory effect (control of lymphocyte proliferation, control of Ig production, control MF activity), stimulation of fibroblasts and osteoblasts, gain production of extracellular matrix IFNa L, M, MF Inhibition of viral replication IFNb Fibroblasts, epithelial cells Inhibition of viral replication IFNg Th1, NK MF activation, stimulation of MHC gp. expression, Th2 inhibition MF – macrophages; M – monocytes; N – neutrophils; DC – dendritic cells; NK – natural killers; L – lymphocytes; B – B cell; T – T cell Clasification of cytokines by functions Proinflammatory cytokines (IL-1, IL-6,IL- 8,IL- 12,IL- 18, TNF) Antiinflammatory cytokines (IL-4, IL-10, TGFb) Cytokines with the activity of hematopoietic cells growth factor (IL-2, 3, 4, 5, 6, 7, 9, 11, 14, 15, CSF, SCF, LIF, EPO) Cytokines applying in TH2 humoral immunity (IL-4, 5, 9, 13) Cytokines applying in the cell-mediated immunity TH1 (IL-2, 12, IFNg, GM-CSF, lymphotoxin) Cytokines with anti-viral effect (IFN-a, IFN-b , IFN- g) Cytokine receptors Consisting of 2 or 3 subunits One subunit binds cytokine, other are associated with cytoplasmic signaling molecules (protein kinases) Signaling subunit is shared by several different cytokine receptors called receptor family Signaling through these receptors may lead to proliferation, differentiation, activation of effector mechanisms or blocking the cell cycle and induction of apoptosis Possibilities of therapeutic affecting of the immune system Causal treatment a) Stem cell transplantation treatment of severe congenital disorders of the immune system and some lymphoproliferative and myeloproliferative disorders complications: infectious complications Graft-versus-host disease obtaining stem cells - from bone marrow - from umbilical cord blood - from peripheral blood Causal treatment b) Gene therapy transduction of the missing gene to hematopoietic stem cells using viral vectors used as a treatment for 2 forms of SCID Substitution treatment autologous stem cell transplantation (following chemotherapy and radiotherapy) treatment with intravenous immunoglobulin (derived from plasma of blood donors) substitution of C1 inhibitor for hereditary angioedema substitution of erythropoietin in patients with chronic renal failure substitution of G-CSF in agranulocytosis Immunomodulation = medical procedure to adjust the disrupted immune function Non-specific immunosuppression nonspecific = affects not only autoreactive and aloreactive lymphocytes, but also other components of immunity (risk of reduction antiinfectious and antitumor immunity) used for treatment of autoimmune diseases, for organ transplantation and severe allergic conditions Non-specific immunosuppression Corticosteroids • anti-inflammatory, immunosuppressive effects • suppress the expression of some genes (IL-2, IL-1, phospholipase A, MHC gp II, adhesion molecules) • inhibition of histamine release from basophils • higher concentrations induce apoptosis of lymfocytes Non-specific immunosuppression Immunosuppressants affecting the metabolism of DNA (cytostatics) • cyclophosphamide (alkylating agent) • methotrexate (antimetabolite) • azathioprine (purine analogue) Non-specific immunosuppression Immunosuppressant selectively inhibiting T cells • immunosuppressive ATB: cyclosporine A, tacrolimus, rapamycin (suppressing the expression of IL-2 and IL-2R in activated T lymphocytes) • anti-CD3 monoclonal antibody (imunosuppression after transplantation, treatment of rejection crises) Non-specific immunosuppression Immunoglobulins in the immunosuppressive indication • polyspecific intravenous immunoglobulins • inhibition of B lymphocytes • antiidiotype activity • inhibition of cytokines • neutralization of toxins • inhibition of complement activation Anti-inflammatory and antiallergic treatment • nonsteroidal anti-inflammatory drugs • antihistamines - blocking H1 receptor - reduce the expression of adhesion molekules - reduce the secretion of histamine ... • inhibitors of inflammatory cytokine - monoclonal antibodies against TNF - thalidomide (TNF inhibitor) • Anti IgE antibodies (omalizumab) - severe allergic astma Non-specific immunostimulant therapy synthetic immunomodulators Methisoprinol (Isoprinosine) - used in viral infections with more severe or relapsing course bacterial extracts and lysates Broncho-Vaxom - prevention of recurrent respiratory tract infections Ribomunyl products of the immune system IL-2 - renal adenocarcinoma IFNa, IFNb - viral hepatitis, some leukemia Erythropoietin – renal failure G-CSF, GM-CSF – neutropenia Transfer factor (blood donors leukocytes undergoing dialysis) Thymus hormones Antigen-specific immunomodulation specific immunomodulation = induce of an immune response or tolerance to a specific antigen • active immunization • passive immunization • specific immunosuppression Antigen-specific immunomodulation Active immunization (vaccination) = the induction of immunity after exposure to an antigen • activates specific cellular and humoral immunity • creates long-term immunity (memory cells) • protect against a pathogen bearing this antigen or similar antigen (prophylaxis) Antigen-specific immunomodulation active immunization (vaccination) • vaccines are made from inactivated or attenuated microorganisms or their antigens (polysaccharide capsule, toxins) • attenuated vaccines cannot be used by immunocompromised individuals • risk of infection or anaphylactic reactions Antigen-specific immunomodulation Passive immunization • natural - transfer of maternal antibodies in fetal blood • therapeutically - the use of animal antibodies against various toxins (snake toxins, tetanus toxin, botulinum toxin) • prophylaxis - the human immunoglobulin from immunized individuals (hepatitis A, rabies, tetanus) - Anti-RhD antibodies – prevent immunization of mother with RhD+ fetus erythrocytes • provides a temporary (3 weeks) specific humoral immunity • the risk anaphylactic reactions Antigen-specific immunomodulation Specific immunosuppression = induction of tolerance to a specific antigen • induction of tolerance by oral administration of antigen (treatment of certain autoimmune diseases) • allergen immunotherapy (pollen, insect poisons) Vaccination against cancer • immunization by dendritic cells Antiinfection immunity Defence against extracellular pathogens bacteria (gram-negative, gram-positive cocci, bacilli), unicellular parasites pathogens induce inflammation removed by phagocytosis - neutrophil granulocytes opsonization (IgG and IgA antibodies, C3b, lectins, CRP...) Defence against extracellular pathogens Opsonisation and phagocytosis Defence against extracellular pathogens Phagocytes are attracted to the site of infection by chemotactic substances (C5a, C3a and chemotactic products of bacteria…) ingested bacteria are destroyed by the microbicidal systems (products of NADP-H oxidase, hydrolytic enzymes and bactericidal substances in lysosomes) phagocytes produce proinflammatory cytokines (IL-1, IL-6, TNF) Defence against extracellular pathogens IgM - complement activation IgG - complement activation, opsonization IgA - opsonization sIgA prevents against infection by intestinal and respiratory bacteria in the defense against bacterial toxins apply neutralizing antibodies (Clostridium tetani and botulinum …) Defence against extracellular pathogens "indirect toxins - bacterial Lipopolysaccharide (LPS) stimulates big number of monocytes to release TNF, which can cause septic shock individuals with immunodeficiency of phagocytes, complement and antibodies production are especially at risk of infections with extracellular bacterial Defense against intracellular pathogens Defense against intracellular pathogens bacteria, fungi and unicellular parasites intracellular parasites are resistant to the microbicidal mechanisms of phagocytes macrophages, which absorbed them, produce IL-12 → TH1 differentiation, production of IFNg and membrane TNF → activation of macrophages and production of NO Defense against intracellular pathogens Defense against intracellular pathogens TC lymphocytes apply in the defense against intracelular parasites, which escape from phagolysosomes individuals with certain disorders of phagocytes and defects of T lymphocytes are at risk of infections with intracellular microorganisms Defense against intracellular pathogens Anti-viral defense Anti-viral defence interferons - production of IFNa and IFNb is induced in infected cells; IFNg activates macrophages (iNOS) IFNa and IFNb - prevents viral replication - induce proliferation of NK cells - increase the expression of HLA-I Anti-viral defence - interferons Anti-viral defence NK cells - ADCC (Antibody-dependent cell-mediated cytotoxicity); NK cell bind with CD16 (Fcg receptor) to IgG which has bound to the surface of infected cell and then NK cell release perforins and granzymes (degranulation) infected macrophages produce IL-12 (a strong activator of NK cells) Anti-viral defence - NK cell activation ADCC Anti-viral defence in the defense against cytopathic viruses applied antibodies: sIgA inhibit mucosal adhesion of viruses (defense against respiratory viruses and enteroviruses) neutralizing IgG and IgM antibodies activate the classical pathway of complement, that is able to lyse certain viruses opsonized viral particles are phagocytosed IgA and IgG have preventive effect in secondary viral infection Anti-viral defence - antibodies Anti-viral defence effector TC lymphocytes destroy infected cells in direct contact (granzym/perforin; FasL) and by produced cytokines (lymfotoxin) some viruses after infection integrate into the host genome, where persist for years (varicella zoster, EBV, papillomavirus) individuals with T lymphocyte immunodeficiency and with combined immune disorders are at risk by viral infections increased susceptibility to herpes infections in individuals with dysfunction of NK cells Anti-viral defence – NK cells and Tc lymphocytes Defense against protozoa parasites Defense against protozoa parasites Toxoplasma gondii, Leishmania, Trypanosoma defense against protozoa parasites is similar to bacteria extracellular parasites - antibodies intracellular parasites - TH1 lymphocytes and activated macrophages Defense against multicellular parasites Defense against multicellular parasites IgE, mast cells, basophils and eosinophils TH2 stimulation under the influence of IL-4 (mast cells and other APC stimulated by parasite) TH2 stimulate B cells with BCR-specific parasite antigens isotype switching under the influence of IL-4 to IgE IgE bind to FceRI on mast cells and basophils Defense against multicellular parasites multicellular parasite binds to IgE on mast cell→ crosslinking of several molecules FceRI initiate mast cell degranulation (release of histamin, tryptase, serotonin…) activation of arachidonic acid metabolism (leukotriene C4, prostaglandin PGD2) - amplification of inflammatory responses cytokine production by mast cell (TNF, TGFb, IL-4, 5, 6) Defense against multicellular parasites Histamine vasodilatation, increase vascular permeability (erythema, edema, itching) bronchoconstriction (cough) increases intestinal peristalsis (diarrhea) increased mucus secretion This helps eliminate the parasite. Mast cell activation Defense against multicellular parasites eosinophils fagocyte complexes of parasitic particles with IgE via their receptors for IgE eosinophils use against parasites extracellular bactericidal substances released from granules (ECP- eosinophil cationic protein, MBP-major basic protein…) Defense against multicellular parasites - eosinophils Thank you for your attention • Phagocytosis https://www.youtube.com/watch?v=7VQU 28itVVw